Bilateral Orbital Myeloid Sarcoma As Initial Sign of Acute Myeloid Leukemia
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Association of Bladder Myeloid Sarcoma and Unclassified
90 Case Report The association of bladder myeloid sarcoma and unclassified myelodysplastic/myeloproliferative disease Mesanede myeloid sarkom ve sınıflandırılamayan myeloproliferatif/myelodisplastik hastalık birlikteliği Mehmet Sönmez1, Ümit Çobanoğlu2, Sevdagül Mungan2, Bircan Sönmez3, Rasin Özyavuz4 1Department of Hematology, Karadeniz Technical University, School of Medicine, Trabzon, Turkey 2Department of Pathology, Karadeniz Technical University, School of Medicine, Trabzon, Turkey 3Department of Nuclear Medicine, Karadeniz Technical University, School of Medicine, Trabzon, Turkey 4Department of Urology, Karadeniz Technical University, School of Medicine, Trabzon, Turkey Abstract Myeloid sarcoma of the urinary bladder is a rare disorder. We report a 71-year-old man with hematuria who had a diffuse myeloid sarcoma of the bladder. He was also under follow-up for unclassified myeloproliferative/myelodysplastic disorder, diagnosed two months before. Abdominal ultrasonography and computed tomography findings were normal. Diagnostic cystoscopy revealed patchy areas of mucosal swelling with hyperemia. Histopathological examination of biopsies demon- strated a neoplasm composed of blasts showing myeloperoxidase positivity by immunohistochemistry. To our knowledge, the current case is the first case of myeloid sarcoma in the urinary bladder without evidence of a mass lesion, with a concurrent diagnosis of unclassifiable myelodysplastic/myeloproliferative disease. (Turk J Hematol 2009; 26: 90-2) Key words: Myeloid sarcoma, urinary bladder, unclassified myelodysplastic/myeloproliferative disease Received: April 3, 2008 Accepted: September 10, 2008 Özet Myeloid sarkom mesanede nadir görülen bir hastalıktır. Bu vaka takdiminde hematüri ile başvuran ve 2 ay önce sınıflandırılamayan myeloproliferatif/myelodisplastik hastalık tanısı almış 71 yaşında erkek hastada mesanede diffüz tutulum ile seyreden myeloid sarkom tanımlandı. Hastanın batın ultrasonografisi ve tomografisi normal olup, tanısal amaçlı sistosko- pide hiperemik ve ödemli bir mukoza izlendi. -

Treatment Outcomes of Pediatric Acute Myeloid Leukemia In
children Article Treatment Outcomes of Pediatric Acute Myeloid Leukemia in the Yeungnam Region: A Multicenter Retrospective Study of the Study Alliance of Yeungnam Pediatric Hematology–Oncology (SAYPH) Jae Min Lee 1 , Eu Jeen Yang 2 , Kyung Mi Park 2 , Young-Ho Lee 3, Heewon Chueh 4, Jeong Ok Hah 5, Ji Kyoung Park 6, Jae Young Lim 7, Eun Sil Park 7, Sang Kyu Park 8, Heung Sik Kim 9, Ye Jee Shim 10 , Jeong A. Park 11,12, Eun Jin Choi 13, Kun Soo Lee 14, Ji Yoon Kim 14 and Young Tak Lim 2,* 1 Department of Pediatrics, College of Medicine, Yeungnam University, Daegu 42415, Korea; [email protected] 2 Department of Pediatrics, Pusan National University Children’s Hospital, Pusan National University, School of Medicine, Yangsan 50612, Korea; [email protected] (E.J.Y.); [email protected] (K.M.P.) 3 Department of Pediatrics, Hanyang University College of Medicine, Hanyang University Medical Center, Seoul 04763, Korea; [email protected] 4 Department of Pediatrics, Dong-A University College of Medicine, Busan 49201, Korea; [email protected] 5 Department of Pediatrics, Daegu Fatima Hospital, Daegu 41199, Korea; [email protected] 6 Department of Pediatrics, Inje University College of Medicine, Busan Paik Hospital, Busan 47392, Korea; [email protected] 7 Department of Pediatrics, Gyeongsang National University College of Medicine, Jinju 52727, Korea; [email protected] (J.Y.L.); [email protected] (E.S.P.) Citation: Lee, J.M.; Yang, E.J.; Park, 8 Department of Pediatrics, Ulsan University Hospital, Ulsan 44033, Korea; [email protected] K.M.; Lee, Y.-H.; Chueh, H.; Hah, J.O.; 9 Department of Pediatrics, Keimyung University School of Medicine, Keimyung University Daegu Dongsan Park, J.K.; Lim, J.Y.; Park, E.S.; Park, Hospital, Daegu 41931, Korea; [email protected] S.K.; et al. -
Myeloid Sarcoma
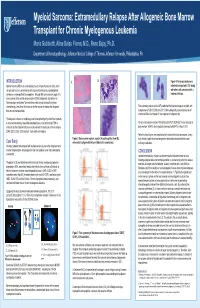
Myeloid Sarcoma: Extramedullary Relapse After Allogeneic Bone Marrow Transplant for Chronic Myelogenous Leukemia Maria Gubbiotti, Alina Dulau Florea, M.D., Renu Bajaj, Ph.D. Department of Hematopathology, Jefferson Medical College of Thomas Jefferson University, Philadelphia, PA INTRODUCTION A. B. Figure 4: Numerous blasts were Myeloid sarcoma (MS) is an extramedullary tumor of myeloid precursor cells, which detected in the patient’s CSF along can precede or occur concomitantly with acute myeloid leukemia, myelodysplastic with other cells consistent with a syndrome, or myeloproliferative neoplasms. Although MS can involve any organ, it is leukemic infiltrate. more common in the central nervous system (CNS) and gonads, sites known as “pharmacologic sanctuaries” where leukemic cells can survive despite systemic chemotherapy. Less often, this tumor can be the manner of relapse after allogeneic Flow cytometry analysis of the CSF established the blast phenotype as myeloid, with bone marrow transplantation. coexpression of CD13, CD33 and CD117. She subsequently received two cycles of intrathecal ARA-C and repeat LP was negative for malignant cells. The diagnosis is based on morphology and immunophenotype by either flow cytometry or immunohistochemistry of paraffin-embedded tissue, and confirmed by FISH or Reverse transcription real-time PCR detected the P210 BCR-ABL1 fusion transcript in molecular studies. Myeloid sarcomas usually express the leukocyte common antigens bone marrow : 0.064%, which gradually increased to 98.947% in March 2013. CD45, CD13, CD33, CD43 and lack T-cell and B-cell antigens. Patient’s clinical course was complicated with multiple infections (pneumonia, urinary Figure 2: Bone marrow aspirate, regular (A) and magnified view (B), tract infection) septic shock and progressive deterioration despite antibiotics and Case Study demonstrating hypercellularity and blast crisis respectively. -

Compressive Myelopathy Caused by Isolated Epidural Myeloid Sarcoma with Systemic Mastocytosis
Clinical Notes Compressive myelopathy caused by isolated epidural myeloid sarcoma with systemic mastocytosis. Rare presentation of a hematological malignancy Cyril J. Kurian, MBBS, Indira Madhavan, MBBS, MD, Prabhalakshmi K. Krishnankutty, MBBS, MD, Mekkattukunnel A. Andrews, MD, DM. eurological manifestations of acute leukemia are Ndue to direct involvement by meningeal infiltration and myeloid sarcoma; and indirect involvement by immunosuppression and treatment related side effects. It is rare for myeloid sarcoma to present without bone marrow involvement (isolated myeloid sarcoma or primary granulocytic sarcoma).1 It is even rarer for an isolated myeloid sarcoma to present in the epidural space. We evaluated a case of paraplegia admitted to our department. He had several atypical features that we would like to present in this report. A 39-year-old gentleman with a body weight of Figure 1 - Magnetic resonance imaging of thoracic spine T1W sagittal 58 kg presented with paresthesia and heaviness of view, arrow showing extradural mass at T6 level. both lower limbs of 4 days duration. He was found to have spastic paraplegia with bladder involvement and sensory level at T6. The clinical diagnosis of acute peripheral blood picture showed dimorphic anemia, transverse myelitis was made. Table 1 summarizes the occasional large cells with granular cytoplasm and nucleus with condensed chromatin, and no blast cells. laboratory investigations. The MRI study of the dorsal Ultrasound of the abdomen showed mild splenomegaly. spine (Figure 1) shows that a moderate sized enhancing Urine Bence Jones protein was absent. No M band was posterior epidural component was compressing the seen on serum protein electrophoresis. Bone marrow thecal sac and spinal cord. -

Isolated Myeloid Sarcoma of Femur in an Aleukemic Child: Case Report
Case Report Clinics in Surgery Published: 21 Apr, 2021 Isolated Myeloid Sarcoma of Femur in an Aleukemic Child: Case Report Celik ZE1*, Ugras S1, Aydin BK2 and Ozturk M3 1Department of Pathology, Selcuk University, Turkey 2Department of Orthopedics and Traumatology, Selcuk University, Turkey 3Department of Pediatric Radiology, Selcuk University, Turkey Abstract Myeloid Sarcoma (MS) is a tumour mass consisting of myeloid blasts, with or without maturation, occurring at an anatomical site other than the bone marrow. It can develop de novo, as well as occurs following a hematologic disorder such as acute myeloid leukemia, myeloproliferative disorder or myelodysplastic syndrome. In this report, we present the radiologic and pathologic findings of a case diagnosed as isolated MS of femur. According to our literature research, this is the first case of isolated MS of femur in an aleukemic patient. MS is a rare neoplasm with diagnostic difficulty owing to its similarity to many other tumors and by the lack of clinical suspicion in patients without any hematological disorder. Histopathological and a detailed immunohistochemical work-up is mandatory for accurate diagnosis of MS to avoid delay in treatment. Keywords: Myeloid sarcoma; Aleukemic; Femur; Child Introduction Myeloid Sarcoma (MS) is a rare neoplasm composed of proliferation of myeloid precursors at extramedullary sites such as skin, lymph node, bone and soft tissue, although it can arise at every site of the body [1-3]. It may develop spontaneously or can be seen simultaneously with hematopoietic disorders such as Acute Myeloid Leukemia (AML), Myeloproliferative Disorder (MPD) or Myelodysplastic Syndrome (MDS). MS can also be the first evidence of AML or progress to AML over months to years. -

The 2016 Revision to the World Health Organization Classification of Myeloid Neoplasms and Acute Leukemia
From www.bloodjournal.org by guest on January 9, 2019. For personal use only. Review Series THE UPDATED WHO CLASSIFICATION OF HEMATOLOGICAL MALIGNANCIES The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia Daniel A. Arber,1 Attilio Orazi,2 Robert Hasserjian,3 J¨urgen Thiele,4 Michael J. Borowitz,5 Michelle M. Le Beau,6 Clara D. Bloomfield,7 Mario Cazzola,8 and James W. Vardiman9 1Department of Pathology, Stanford University, Stanford, CA; 2Department of Pathology, Weill Cornell Medical College, New York, NY; 3Department of Pathology, Massachusetts General Hospital, Boston, MA; 4Institute of Pathology, University of Cologne, Cologne, Germany; 5Department of Pathology, Johns Hopkins Medical Institutions, Baltimore, MD; 6Section of Hematology/Oncology, University of Chicago, Chicago, IL; 7Comprehensive Cancer Center, James Cancer Hospital and Solove Research Institute, The Ohio State University, Columbus, OH; 8Department of Molecular Medicine, University of Pavia, and Department of Hematology Oncology, Fondazione IRCCS Policlinico San Matteo, Pavia, Italy; and 9Department of Pathology, University of Chicago, Chicago, IL The World Health Organization (WHO) the prognostic relevance of entities cur- The 2016 edition represents a revision classification of tumors of the hemato- rently included in the WHO classification of the prior classification rather than poietic and lymphoid tissues was last and that also suggest new entities that an entirely new classification and at- updated in 2008. Since then, there have should be added. Therefore, there is a tempts to incorporate new clinical, prog- been numerous advances in the identifi- clear need for a revision to the current nostic, morphologic, immunophenotypic, cation of unique biomarkers associated classification. -

Myeloid Sarcoma in a Child with Acute Myeloblastic Leukaemia Jamal Ahmad1, Lubna Zafar1, Gul Hussain2 and Sajida Kausar3
CASE REPORT Myeloid Sarcoma in a Child with Acute Myeloblastic Leukaemia Jamal Ahmad1, Lubna Zafar1, Gul Hussain2 and Sajida Kausar3 ABSTRACT We report a rare occurrence of myeloid sarcoma in a 7 years old child with acute myeloblastic leukaemia (AML - FAB type M2). He presented with fever, generalized weakness, bilateral proptosis and left parotid swelling. CT scan revealed a mass in paranasal sinuses extending into brain and retro-orbital region. Diagnosis of AML M2 was made on bone marrow aspiration and special stains. Induction therapy for AML was given according to standard protocol. The extramedullary lesion as well as the acute leukaemia went into complete remission. Key words: Myeloid sarcoma. Chloroma. Acute myeloblastic leukaemia. Paranasal sinus. INTRODUCTION palpable. Fundoscopy showed established Myeloid (granulocytic) sarcoma or chloroma is an extra papilloedema. Ear examination showed left conductive medullary tumour composed of immature malignant deafness due to collapse of left external auditory canal white blood cells or myeloblasts with or without (pressure effect of tumour). CT scan of brain and neck maturation.1 It affects older adults more frequently. showed locally infiltrative mass in nasopharyngeal Simple infiltration by myeloid blasts in any part of the region with intraorbital and intracranial extension body to form tumour mass is not labelled as myeloid (Figure 2). A differential diagnoses of rhabdomyo- sarcoma unless the tissue architecture of the part is lost. sarcoma, lymphoma and meningioma were suggested This tumour may precede or occur concurrently with by the radiologist. Fine needle aspiration cytology of acute or chronic myeloid leukaemia. It can also occur parotid region swelling showed benign epithelial lesion. -

Mast Cell Sarcoma: a Rare and Potentially Under
Modern Pathology (2013) 26, 533–543 & 2013 USCAP, Inc. All rights reserved 0893-3952/13 $32.00 533 Mast cell sarcoma: a rare and potentially under-recognized diagnostic entity with specific therapeutic implications Russell JH Ryan1, Cem Akin2,3, Mariana Castells2,3, Marcia Wills4, Martin K Selig1, G Petur Nielsen1, Judith A Ferry1 and Jason L Hornick2,5 1Pathology Service, Massachusetts General Hospital, and Harvard Medical School, Boston, MA, USA; 2Mastocytosis Center, Harvard Medical School, Boston, MA, USA; 3Department of Medicine, Harvard Medical School, Boston, MA, USA; 4Seacoast Pathology / Aurora Diagnostics, Exeter, NH and 5Department of Pathology, Brigham and Women’s Hospital, and Harvard Medical School, Boston, MA, USA Mast cell sarcoma is a rare, aggressive neoplasm composed of cytologically malignant mast cells presenting as a solitary mass. Previous descriptions of mast cell sarcoma have been limited to single case reports, and the pathologic features of this entity are not well known. Here, we report three new cases of mast cell sarcoma and review previously reported cases. Mast cell sarcoma has a characteristic morphology of medium-sized to large epithelioid cells, including bizarre multinucleated cells, and does not closely resemble either normal mast cells or the spindle cells of systemic mastocytosis. One of our three cases arose in a patient with a remote history of infantile cutaneous mastocytosis, an association also noted in one previous case report. None of our three cases were correctly diagnosed as mast cell neoplasms on initial pathological evaluation, suggesting that this entity may be under-recognized. Molecular testing of mast cell sarcoma has not thus far detected the imatinib- resistant KIT D816V mutation, suggesting that recognition of these cases may facilitate specific targeted therapy. -

Extramedullary Relapse of Acute Myeloid Leukemia After Allogeneic Hematopoietic Stem Cell Transplantation: an Easily Overlooked but Significant Pattern of Relapse
Extramedullary Relapse of Acute Myeloid Leukemia after Allogeneic Hematopoietic Stem Cell Transplantation: An Easily Overlooked but Significant Pattern of Relapse Satoshi Yoshihara,1 Toshihiko Ando,2 Hiroyasu Ogawa1 Acute myeloid leukemia may manifest as myeloid sarcoma in a variety of extramedullary (EM) tissues at diagnosis or at relapse. Although EM relapse after allogeneic hematopoietic stem cell transplantation (alloSCT) has been considered to be rare, recent studies have suggested that it occurs in 5% to 12% of pa- tients who receive alloSCT, accounting for 7% to 46% of total relapses. The incidence of EM relapse after immunomodulation (eg, donor lymphocyte infusion) or a second SCT is even higher. Moreover, patients with EM relapse are more likely to have had preceding acute graft-versus-host disease or chronic graft- versus-host disease relative to those with bone marrow relapse. Collectively, these observations suggest that the preferential occurrence of the graft-versus-leukemia effect underlies the pathogenesis of EM relapse. Establishing an early diagnosis of EM relapse has been challenging because of the immense diversity in the relapse sites; however, recent studies have suggested the usefulness of 18F-fluorodeoxyglucose positron emission tomography scans in the detection of EM relapse. As a treatment for EM relapse, a combination of local and systemic therapy should be considered, because local therapy alone often results in subsequent systemic relapse. The prognosis for patients who develop EM relapse after SCTremains poor but is slightly better than that after bone marrow relapse. In addition to an early diagnosis with new modalities, clinical studies using new agents that may offer systemic activity while preserving the graft-versus-leukemia effect are warranted as part of an effort to improve the clinical outcome. -

Cutaneous Myeloid Sarcoma
Case Report Journal of Hematology & Multiple Myeloma Published: 13 Sep, 2018 Cutaneous Myeloid Sarcoma Wronska M*, Golbari NM, D’Abreo N and Sticco K Department of Medicine and Population Health, NYU School of Medicine, New York Abstract Introduction: Myeloid Sarcomas (MS) are rare neoplasm’s occurring at extramedullary sites. They are typically found in the setting of Acute Myeloid Leukemia (AML) either concurrently or at relapse. Less often, they may be associated with other hematologic disorders such Myelodysplastic Syndromes (MDS) or Myeloproliferative Neoplasms (MPN). Rarely MS can present as an isolated leukemic tumor, without bone marrow involvement. The presentation of these isolated cases is greatly variable and can make diagnosis particularly challenging. Case Presentation: A case report of a 79-year old patient with rare and rapidly evolving cutaneous presentation of isolated MS, without bone marrow involvement. Discussion: This case identifies the potential for isolated MS to present as a cutaneous skin infiltration in the absence of AML, MDS or MPN. Given the rarity of this neoplasm and the wide variation in symptomology, it is prudent to be aware of aberrant presentations of isolated MS. This case highlights the need for physicians to consider MS in the differential diagnosis, even in the context of negative bone marrow, as early diagnosis and treatment with chemotherapy has been demonstrated to improve survival outcomes. Keywords: Isolated myeloid sarcoma; Cutaneous infiltration; Skin infiltration Introduction Myeloid Sarcoma (MS), also known as granulocytic sarcoma, chloroma, or myeloblastoma, is a rare extramedullary proliferation of myeloblasts thought to be a variant of Acute Myeloid Leukemia (AML) [1]. The initial manifestation of the disease is highly variable and can present at different stages, such as preceding or coinciding with AML, arising from plastic transformation of a Myelodys plastic Syndrome (MDS), or developing from a chronic Myeloproliferative Neoplasm (MPN) [2]. -

011 Monoblastic Sarcoma Myeloid Sarcoma.Cdr
Gujarat Cancer Society Research Journal Monoblastic Sarcoma / Myeloid Sarcoma of Paraspinal Region Presenting as Acute Paraparesis in Aleukemic Patient- A Rare Case Report from Western India Kikani Alpeshkumar1, Modi Mitul1*, Panchal Harsha2, Trivedi Priti2*, Lakum Nirmal1#, Parikh Sonia2, Makadia Gautam1: Resident1, Professor2 Department of Medical and Pediatric Oncology *Department of Pathology #Department of Radiology Summary spine screening. Ultrasonography of pelvis suggested Myeloid sarcoma (MS), also known as extramedullary large well defined hypoechoic lesion measuring 45 acute myeloid leukemia, extramedullary myeloid tumor, and granulocytic sarcoma, myeloblastoma or chloroma, is a rare mm×30 mm in subcutaneous tissue and musculature manifestation which is characterized by the occurrence of 1 or in anterior abdominal wall, possibility of metastatic more tumor myeloid masses occurring at an extramedullary site. deposit , biopsy of which was suggestive of malignant We are reporting a rare case of monoblastic sarcoma in a 50 year round cell tumor. MRI of spine revealed altered signal male patient without history of acute myeloid leukemia with involvement of paraspinal region, abdominal wall and tongue, intensity lesion in intraduralextramedullary who presented with acute paraparesis. The patient was treated compartment extending from D3 to D7 level in post with decompression laminectomy followed by Radiotherapy. contrast T1 weighted SAG images (Figure 1) and in After confirming diagnosis of monoblastic sarcoma, patient was T2 weighted -

Treatment of Extramedullary Myeloid Sarcoma with Radiotherapy
Open Access Case Report DOI: 10.7759/cureus.15676 Treatment of Extramedullary Myeloid Sarcoma With Radiotherapy Suzanne R. Graham 1 1. Radiation Oncology, Genesis Care, Bundaberg, AUS Corresponding author: Suzanne R. Graham, [email protected] Abstract Myeloid sarcoma is a rare pathology with important clinical implications. In this paper, we report the case of a 95-year-old gentleman with an orbital mass, which was later confirmed to be a myeloid sarcoma. We also discuss the role of radiotherapy in regard to this diagnosis in patients. Categories: Ophthalmology, Radiation Oncology, Hematology Keywords: acute myeloid sarcoma, orbital swelling, acute myeloid leukemia (aml), radiotherapy (rt), palliative radiation therapy Introduction Myeloid sarcoma (also known as chloroma, granulocytic sarcoma, or myeloblastoma) is a rare extramedullary manifestation of acute myeloid leukaemia (AML) with an estimated incidence throughout the literature of under 1% [1]. This rare neoplastic condition, which consists of immature myeloid cells, most often occurs in areas such as bone and skin; however, almost any area of the body can be affected. It can sometimes be the first manifestation of AML in a patient, precede a diagnosis of AML, or even be the initial finding in a patient who has relapsed from previously treated AML [2,3]. Case Presentation Our patient was a 95-year-old gentleman from a nursing home background who presented with a large, fixed, non-tender mass around his left orbit, which progressed quickly over the two-week period prior to presentation. His vision was intact, but the pressure of the mass was causing discomfort to the patient. He had obvious proptosis of the left eye and associated diplopia as the mass progressed in size.