Compressive Myelopathy Caused by Isolated Epidural Myeloid Sarcoma with Systemic Mastocytosis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Updates in Mastocytosis
Updates in Mastocytosis Tryptase PD-L1 Tracy I. George, M.D. Professor of Pathology 1 Disclosure: Tracy George, M.D. Research Support / Grants None Stock/Equity (any amount) None Consulting Blueprint Medicines Novartis Employment ARUP Laboratories Speakers Bureau / Honoraria None Other None Outline • Classification • Advanced mastocytosis • A case report • Clinical trials • Other potential therapies Outline • Classification • Advanced mastocytosis • A case report • Clinical trials • Other potential therapies Mastocytosis symposium and consensus meeting on classification and diagnostic criteria for mastocytosis Boston, October 25-28, 2012 2008 WHO Classification Scheme for Myeloid Neoplasms Acute Myeloid Leukemia Chronic Myelomonocytic Leukemia Atypical Chronic Myeloid Leukemia Juvenile Myelomonocytic Leukemia Myelodysplastic Syndromes MDS/MPN, unclassifiable Chronic Myelogenous Leukemia MDS/MPN Polycythemia Vera Essential Thrombocythemia Primary Myelofibrosis Myeloproliferative Neoplasms Chronic Neutrophilic Leukemia Chronic Eosinophilic Leukemia, NOS Hypereosinophilic Syndrome Mast Cell Disease MPNs, unclassifiable Myeloid or lymphoid neoplasms Myeloid neoplasms associated with PDGFRA rearrangement associated with eosinophilia and Myeloid neoplasms associated with PDGFRB abnormalities of PDGFRA, rearrangement PDGFRB, or FGFR1 Myeloid neoplasms associated with FGFR1 rearrangement (EMS) 2017 WHO Classification Scheme for Myeloid Neoplasms Chronic Myelomonocytic Leukemia Acute Myeloid Leukemia Atypical Chronic Myeloid Leukemia Juvenile Myelomonocytic -

The Association of Bladder Myeloid Sarcoma and Unclassified
90 Case Report The association of bladder myeloid sarcoma and unclassified myelodysplastic/myeloproliferative disease Mesanede myeloid sarkom ve sınıflandırılamayan myeloproliferatif/myelodisplastik hastalık birlikteliği Mehmet Sönmez1, Ümit Çobanoğlu2, Sevdagül Mungan2, Bircan Sönmez3, Rasin Özyavuz4 1Department of Hematology, Karadeniz Technical University, School of Medicine, Trabzon, Turkey 2Department of Pathology, Karadeniz Technical University, School of Medicine, Trabzon, Turkey 3Department of Nuclear Medicine, Karadeniz Technical University, School of Medicine, Trabzon, Turkey 4Department of Urology, Karadeniz Technical University, School of Medicine, Trabzon, Turkey Abstract Myeloid sarcoma of the urinary bladder is a rare disorder. We report a 71-year-old man with hematuria who had a diffuse myeloid sarcoma of the bladder. He was also under follow-up for unclassified myeloproliferative/myelodysplastic disorder, diagnosed two months before. Abdominal ultrasonography and computed tomography findings were normal. Diagnostic cystoscopy revealed patchy areas of mucosal swelling with hyperemia. Histopathological examination of biopsies demon- strated a neoplasm composed of blasts showing myeloperoxidase positivity by immunohistochemistry. To our knowledge, the current case is the first case of myeloid sarcoma in the urinary bladder without evidence of a mass lesion, with a concurrent diagnosis of unclassifiable myelodysplastic/myeloproliferative disease. (Turk J Hematol 2009; 26: 90-2) Key words: Myeloid sarcoma, urinary bladder, unclassified myelodysplastic/myeloproliferative disease Received: April 3, 2008 Accepted: September 10, 2008 Özet Myeloid sarkom mesanede nadir görülen bir hastalıktır. Bu vaka takdiminde hematüri ile başvuran ve 2 ay önce sınıflandırılamayan myeloproliferatif/myelodisplastik hastalık tanısı almış 71 yaşında erkek hastada mesanede diffüz tutulum ile seyreden myeloid sarkom tanımlandı. Hastanın batın ultrasonografisi ve tomografisi normal olup, tanısal amaçlı sistosko- pide hiperemik ve ödemli bir mukoza izlendi. -

Treatment Outcomes of Pediatric Acute Myeloid Leukemia In
children Article Treatment Outcomes of Pediatric Acute Myeloid Leukemia in the Yeungnam Region: A Multicenter Retrospective Study of the Study Alliance of Yeungnam Pediatric Hematology–Oncology (SAYPH) Jae Min Lee 1 , Eu Jeen Yang 2 , Kyung Mi Park 2 , Young-Ho Lee 3, Heewon Chueh 4, Jeong Ok Hah 5, Ji Kyoung Park 6, Jae Young Lim 7, Eun Sil Park 7, Sang Kyu Park 8, Heung Sik Kim 9, Ye Jee Shim 10 , Jeong A. Park 11,12, Eun Jin Choi 13, Kun Soo Lee 14, Ji Yoon Kim 14 and Young Tak Lim 2,* 1 Department of Pediatrics, College of Medicine, Yeungnam University, Daegu 42415, Korea; [email protected] 2 Department of Pediatrics, Pusan National University Children’s Hospital, Pusan National University, School of Medicine, Yangsan 50612, Korea; [email protected] (E.J.Y.); [email protected] (K.M.P.) 3 Department of Pediatrics, Hanyang University College of Medicine, Hanyang University Medical Center, Seoul 04763, Korea; [email protected] 4 Department of Pediatrics, Dong-A University College of Medicine, Busan 49201, Korea; [email protected] 5 Department of Pediatrics, Daegu Fatima Hospital, Daegu 41199, Korea; [email protected] 6 Department of Pediatrics, Inje University College of Medicine, Busan Paik Hospital, Busan 47392, Korea; [email protected] 7 Department of Pediatrics, Gyeongsang National University College of Medicine, Jinju 52727, Korea; [email protected] (J.Y.L.); [email protected] (E.S.P.) Citation: Lee, J.M.; Yang, E.J.; Park, 8 Department of Pediatrics, Ulsan University Hospital, Ulsan 44033, Korea; [email protected] K.M.; Lee, Y.-H.; Chueh, H.; Hah, J.O.; 9 Department of Pediatrics, Keimyung University School of Medicine, Keimyung University Daegu Dongsan Park, J.K.; Lim, J.Y.; Park, E.S.; Park, Hospital, Daegu 41931, Korea; [email protected] S.K.; et al. -
Myeloid Sarcoma
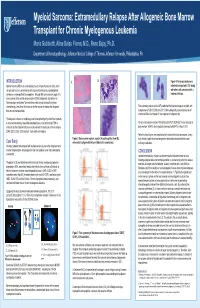
Myeloid Sarcoma: Extramedullary Relapse After Allogeneic Bone Marrow Transplant for Chronic Myelogenous Leukemia Maria Gubbiotti, Alina Dulau Florea, M.D., Renu Bajaj, Ph.D. Department of Hematopathology, Jefferson Medical College of Thomas Jefferson University, Philadelphia, PA INTRODUCTION A. B. Figure 4: Numerous blasts were Myeloid sarcoma (MS) is an extramedullary tumor of myeloid precursor cells, which detected in the patient’s CSF along can precede or occur concomitantly with acute myeloid leukemia, myelodysplastic with other cells consistent with a syndrome, or myeloproliferative neoplasms. Although MS can involve any organ, it is leukemic infiltrate. more common in the central nervous system (CNS) and gonads, sites known as “pharmacologic sanctuaries” where leukemic cells can survive despite systemic chemotherapy. Less often, this tumor can be the manner of relapse after allogeneic Flow cytometry analysis of the CSF established the blast phenotype as myeloid, with bone marrow transplantation. coexpression of CD13, CD33 and CD117. She subsequently received two cycles of intrathecal ARA-C and repeat LP was negative for malignant cells. The diagnosis is based on morphology and immunophenotype by either flow cytometry or immunohistochemistry of paraffin-embedded tissue, and confirmed by FISH or Reverse transcription real-time PCR detected the P210 BCR-ABL1 fusion transcript in molecular studies. Myeloid sarcomas usually express the leukocyte common antigens bone marrow : 0.064%, which gradually increased to 98.947% in March 2013. CD45, CD13, CD33, CD43 and lack T-cell and B-cell antigens. Patient’s clinical course was complicated with multiple infections (pneumonia, urinary Figure 2: Bone marrow aspirate, regular (A) and magnified view (B), tract infection) septic shock and progressive deterioration despite antibiotics and Case Study demonstrating hypercellularity and blast crisis respectively. -

Death from Mast Cell Leukemia: a Young Patient with Longstanding Cutaneous Mastocytosis Evolving Into Fatal Mast Cell Leukemia
CASE REPORTS Pediatric Dermatology Vol. 29 No. 5 605–609, 2012 Death from Mast Cell Leukemia: A Young Patient with Longstanding Cutaneous Mastocytosis Evolving into Fatal Mast Cell Leukemia Rattanavalai Chantorn, M.D.,*, and Tor Shwayder, M.D. *Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand, Department of Pediatric Dermatology, Henry Ford Hospital, Detroit, Michigan Abstract: Mastocytosis is a broad term used for a group of disorders characterized by accumulation of mast cells in the skin with or without extracutaneous involvement. The clinical spectrum of the disease varies from only cutaneous lesions to highly aggressive systemic involvement such as mast cell leukemia. Mastocytosis can present from birth to adult- hood. In children, mastocytosis is usually benign, and there is a good chance of spontaneous regression at puberty, unlike adult-onset disease, which is generally systemic and more severe. Moreover, individuals with systemic mastocytosis may be at risk of developing hematologic malignancies. We describe a girl who presented to us with a solitary mastocytoma at age 5 and later developed maculopapular cutaneous mastocytosis. At age 23, after an episode of anaphylactic shock, a bone marrow examination revealed mast cell leukemia. She ultimately died despite aggressive chemotherapy and bone marrow transplantation. Mastocytosis is characterized by the abnormal common forms of CM in childhood. The excoriation growth and infiltration of mast cells (MC) in various of lesions causes hives and perilesional erythema, tissues and is classified into two broad categories: which characterizes Darier’s sign (Fig. 3). SM is cutaneous mastocytosis (CM) and systemic mastocy- characterized by multifocal MC infiltrates with or tosis (SM) (1). -

Molecular Profiling of Myeloid Progenitor Cells in Multi-Mutated Advanced Systemic Mastocytosis Identifies KIT D816V As a Distin
Leukemia (2015) 29, 1115–1122 © 2015 Macmillan Publishers Limited All rights reserved 0887-6924/15 www.nature.com/leu ORIGINAL ARTICLE Molecular profiling of myeloid progenitor cells in multi-mutated advanced systemic mastocytosis identifies KIT D816V as a distinct and late event M Jawhar1,8, J Schwaab1,8, S Schnittger2, K Sotlar3, H-P Horny3, G Metzgeroth1, N Müller1, S Schneider4, N Naumann1, C Walz3, T Haferlach2, P Valent5, W-K Hofmann1, NCP Cross6,7, A Fabarius1 and A Reiter1 To explore the molecular profile and its prognostic implication in systemic mastocytosis (SM), we analyzed the mutation status of granulocyte–macrophage colony-forming progenitor cells (CFU-GM) in patients with KIT D816V+ indolent SM (ISM, n = 4), smoldering SM (SSM, n = 2), aggressive SM (ASM, n = 1), SM with associated clonal hematologic non-mast cell lineage disorder (SM-AHNMD, n = 5) and ASM-AHNMD (n = 7). All patients with (A)SM-AHNMD (n = 12) carried 1–4 (median 3) additional mutations in 11 genes tested, most frequently TET2, SRSF2, ASXL1, CBL and EZH2. In multi-mutated (A)SM-AHNMD, KIT D816V+ single-cell-derived CFU-GM colonies were identified in 8/12 patients (median 60%, range 0–95). Additional mutations were identified in CFU-GM colonies in all patients, and logical hierarchy analysis indicated that mutations in TET2, SRSF2 and ASXL1 preceded KIT D816V. In ISM/SSM, no additional mutations were detected and CFU-GM colonies were exclusively KIT D816V−. These data indicate that (a) (A)SM-AHNMD is a multi-mutated neoplasm, (b) mutations in TET2, SRSF2 or ASXL1 precede KIT D816V in ASM-AHNMD, (c) KIT D816V is thus a phenotype modifier toward SM and (d) KIT D816V or other mutations are rare in CFU-GM colonies of ISM/SSM patients, which might explain at least in part their better prognosis. -

Isolated Myeloid Sarcoma of Femur in an Aleukemic Child: Case Report
Case Report Clinics in Surgery Published: 21 Apr, 2021 Isolated Myeloid Sarcoma of Femur in an Aleukemic Child: Case Report Celik ZE1*, Ugras S1, Aydin BK2 and Ozturk M3 1Department of Pathology, Selcuk University, Turkey 2Department of Orthopedics and Traumatology, Selcuk University, Turkey 3Department of Pediatric Radiology, Selcuk University, Turkey Abstract Myeloid Sarcoma (MS) is a tumour mass consisting of myeloid blasts, with or without maturation, occurring at an anatomical site other than the bone marrow. It can develop de novo, as well as occurs following a hematologic disorder such as acute myeloid leukemia, myeloproliferative disorder or myelodysplastic syndrome. In this report, we present the radiologic and pathologic findings of a case diagnosed as isolated MS of femur. According to our literature research, this is the first case of isolated MS of femur in an aleukemic patient. MS is a rare neoplasm with diagnostic difficulty owing to its similarity to many other tumors and by the lack of clinical suspicion in patients without any hematological disorder. Histopathological and a detailed immunohistochemical work-up is mandatory for accurate diagnosis of MS to avoid delay in treatment. Keywords: Myeloid sarcoma; Aleukemic; Femur; Child Introduction Myeloid Sarcoma (MS) is a rare neoplasm composed of proliferation of myeloid precursors at extramedullary sites such as skin, lymph node, bone and soft tissue, although it can arise at every site of the body [1-3]. It may develop spontaneously or can be seen simultaneously with hematopoietic disorders such as Acute Myeloid Leukemia (AML), Myeloproliferative Disorder (MPD) or Myelodysplastic Syndrome (MDS). MS can also be the first evidence of AML or progress to AML over months to years. -

The 2016 Revision to the World Health Organization Classification of Myeloid Neoplasms and Acute Leukemia
From www.bloodjournal.org by guest on January 9, 2019. For personal use only. Review Series THE UPDATED WHO CLASSIFICATION OF HEMATOLOGICAL MALIGNANCIES The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia Daniel A. Arber,1 Attilio Orazi,2 Robert Hasserjian,3 J¨urgen Thiele,4 Michael J. Borowitz,5 Michelle M. Le Beau,6 Clara D. Bloomfield,7 Mario Cazzola,8 and James W. Vardiman9 1Department of Pathology, Stanford University, Stanford, CA; 2Department of Pathology, Weill Cornell Medical College, New York, NY; 3Department of Pathology, Massachusetts General Hospital, Boston, MA; 4Institute of Pathology, University of Cologne, Cologne, Germany; 5Department of Pathology, Johns Hopkins Medical Institutions, Baltimore, MD; 6Section of Hematology/Oncology, University of Chicago, Chicago, IL; 7Comprehensive Cancer Center, James Cancer Hospital and Solove Research Institute, The Ohio State University, Columbus, OH; 8Department of Molecular Medicine, University of Pavia, and Department of Hematology Oncology, Fondazione IRCCS Policlinico San Matteo, Pavia, Italy; and 9Department of Pathology, University of Chicago, Chicago, IL The World Health Organization (WHO) the prognostic relevance of entities cur- The 2016 edition represents a revision classification of tumors of the hemato- rently included in the WHO classification of the prior classification rather than poietic and lymphoid tissues was last and that also suggest new entities that an entirely new classification and at- updated in 2008. Since then, there have should be added. Therefore, there is a tempts to incorporate new clinical, prog- been numerous advances in the identifi- clear need for a revision to the current nostic, morphologic, immunophenotypic, cation of unique biomarkers associated classification. -

Myeloid Sarcoma in a Child with Acute Myeloblastic Leukaemia Jamal Ahmad1, Lubna Zafar1, Gul Hussain2 and Sajida Kausar3
CASE REPORT Myeloid Sarcoma in a Child with Acute Myeloblastic Leukaemia Jamal Ahmad1, Lubna Zafar1, Gul Hussain2 and Sajida Kausar3 ABSTRACT We report a rare occurrence of myeloid sarcoma in a 7 years old child with acute myeloblastic leukaemia (AML - FAB type M2). He presented with fever, generalized weakness, bilateral proptosis and left parotid swelling. CT scan revealed a mass in paranasal sinuses extending into brain and retro-orbital region. Diagnosis of AML M2 was made on bone marrow aspiration and special stains. Induction therapy for AML was given according to standard protocol. The extramedullary lesion as well as the acute leukaemia went into complete remission. Key words: Myeloid sarcoma. Chloroma. Acute myeloblastic leukaemia. Paranasal sinus. INTRODUCTION palpable. Fundoscopy showed established Myeloid (granulocytic) sarcoma or chloroma is an extra papilloedema. Ear examination showed left conductive medullary tumour composed of immature malignant deafness due to collapse of left external auditory canal white blood cells or myeloblasts with or without (pressure effect of tumour). CT scan of brain and neck maturation.1 It affects older adults more frequently. showed locally infiltrative mass in nasopharyngeal Simple infiltration by myeloid blasts in any part of the region with intraorbital and intracranial extension body to form tumour mass is not labelled as myeloid (Figure 2). A differential diagnoses of rhabdomyo- sarcoma unless the tissue architecture of the part is lost. sarcoma, lymphoma and meningioma were suggested This tumour may precede or occur concurrently with by the radiologist. Fine needle aspiration cytology of acute or chronic myeloid leukaemia. It can also occur parotid region swelling showed benign epithelial lesion. -

©Ferrata Storti Foundation
ORIGINAL ARTICLES Synergistic growth-inhibitory effects of two tyrosine kinase inhibitors, dasatinib and PKC412, on neoplastic mast cells expressing the D816V-mutated oncogenic variant of KIT Karoline V. Gleixner, Matthias Mayerhofer, Karoline Sonneck, Alexander Gruze, Puchit Samorapoompichit, Christian Baumgartner, Francis Y. Lee, Karl J. Aichberger, Paul W. Manley, Doriano Fabbro, Winfried F. Pickl, Christian Sillaber, Peter Valent ABSTRACT From the Department of Internal Background and Objectives Medicine I, Division of Hematology & Hemostaseology (KVG, KS, CB, In a majority of all patients with systemic mastocytosis (SM) including those with KJA, CS, PV); Institute of Immunology mast cell leukemia (MCL), neoplastic mast cells (MC) display the D816V-mutated vari- (AG, WFP), Clinical Institute of ant of KIT. The respective oncoprotein, KIT D816V, exhibits constitutive tyrosine Medical and Chemical Laboratory kinase (TK) activity and has been implicated in malignant cell growth. Therefore, sev- Diagnostics (MM); Center of Anatomy eral attempts have been made to identify KIT D816V-targeting drugs. and Cell Biology, Medical University of Vienna, Austria (PS); Oncology Design and Methods Drug Discovery, Bristol-Myers Squibb, We examined the effects of the novel TK-inhibitor dasatinib alone and in combination Princeton, NJ, USA (FYL); Novartis Pharma AG, Basel, Switzerland with other targeted drugs on growth of neoplastic MC. (PWM, DF). Results Funding: this study was supported by Confirming previous studies, dasatinib was found to inhibit the TK activity of wild type the Fonds zur Förderung der (wt) KIT and KIT-D816V as well as growth and survival of neoplastic MC and of the Wissenschaftlichen Forschung in MCL cell line, HMC-1. The growth-inhibitory effects of dasatinib in HMC-1 cells were Österreich (FWF) grant #P-17205- found to be associated with a decrease in expression of CD2 and CD63. -

Mast Cell Sarcoma: a Rare and Potentially Under
Modern Pathology (2013) 26, 533–543 & 2013 USCAP, Inc. All rights reserved 0893-3952/13 $32.00 533 Mast cell sarcoma: a rare and potentially under-recognized diagnostic entity with specific therapeutic implications Russell JH Ryan1, Cem Akin2,3, Mariana Castells2,3, Marcia Wills4, Martin K Selig1, G Petur Nielsen1, Judith A Ferry1 and Jason L Hornick2,5 1Pathology Service, Massachusetts General Hospital, and Harvard Medical School, Boston, MA, USA; 2Mastocytosis Center, Harvard Medical School, Boston, MA, USA; 3Department of Medicine, Harvard Medical School, Boston, MA, USA; 4Seacoast Pathology / Aurora Diagnostics, Exeter, NH and 5Department of Pathology, Brigham and Women’s Hospital, and Harvard Medical School, Boston, MA, USA Mast cell sarcoma is a rare, aggressive neoplasm composed of cytologically malignant mast cells presenting as a solitary mass. Previous descriptions of mast cell sarcoma have been limited to single case reports, and the pathologic features of this entity are not well known. Here, we report three new cases of mast cell sarcoma and review previously reported cases. Mast cell sarcoma has a characteristic morphology of medium-sized to large epithelioid cells, including bizarre multinucleated cells, and does not closely resemble either normal mast cells or the spindle cells of systemic mastocytosis. One of our three cases arose in a patient with a remote history of infantile cutaneous mastocytosis, an association also noted in one previous case report. None of our three cases were correctly diagnosed as mast cell neoplasms on initial pathological evaluation, suggesting that this entity may be under-recognized. Molecular testing of mast cell sarcoma has not thus far detected the imatinib- resistant KIT D816V mutation, suggesting that recognition of these cases may facilitate specific targeted therapy. -

Mast Cell Differentiation from Human Peripheral Blood Mononuclear Cells
Mast Cell and Myeloid Marker Expression During Early In Vitro Mast Cell Differentiation from Human Peripheral Blood Mononuclear Cells Pia Welker, JuÈrgen Grabbe,* Torsten Zuberbier, Sven Guhl, and Beate M. Henz Departments of Dermatology, Humboldt-University, Berlin, Germany; *Medical University, LuÈbeck, Germany In order to characterize the phenotype of human after 2 wk of culture showed that FceRIa-positive mast cell precursors in the peripheral blood mono- cells were mostly CD14+ (90%),CD64+ (82%),and nuclear fraction and its alterations during in vivo mast CD68+ (52%) on ¯ow cytometry. Intracellular tryp- cell differentiation,cells were studied before and tase activity was ®rst detectable after 1 wk of culture, during culture with stem cell factor or stem cell fac- increased FceRIa expression was only detectable by tor-containing cell supernatants. Prior to culture, week 2. Cultured cells acquired the ability to release 86% of cells were immunoreactive for the monocytic histamine during IgE-dependent stimulation,and marker CD14,slightly fewer for CD11b and CD64, culture with the c-Kit antibody YB5.B8 resulted in a <10% expressed FceRIa,rare cells were CD34+ downregulation of tryptase and FceRIa,but not of (<0,1%), and none stained for CD1, CD33, c-Kit, c-Kit. These data show that human mast cells and tryptase. After 2 wk of culture,there was de novo develop from c-Kit- and tryptase-negative precursors expression of c-Kit (14%±43% positive cells),tryptase in the myelomonocytic fraction of peripheral blood (26%±79%),CD33 (57%),and CD64 (64%),an upre- and that they upregulate,maintain,and share many gulation of FceRIa (23%±52%),CD11b (93%),and phenotypic characteristics of cells from the mono- CD68 (95%),but no expression of CD34.