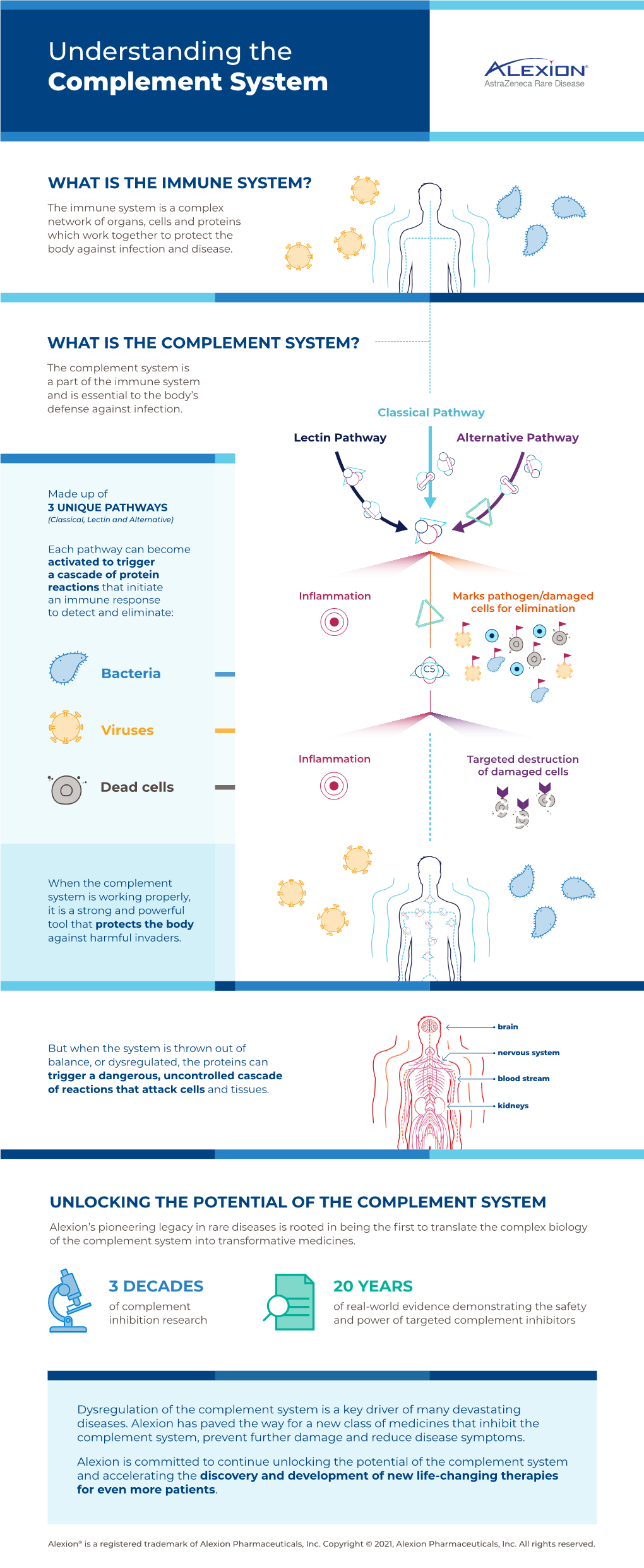
Understanding the Complement System
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Adaptive Tdetect Fact Sheet for Recipient
FACT SHEET FOR RECIPIENTS Coronavirus Adaptive Biotechnologies Corporation September 2, 2021 Disease 2019 T-Detect COVID Test (COVID-19) You are being given this Fact Sheet because your coughing, difficulty breathing, etc.). A full list of sample is being tested or was tested for an adaptive T- symptoms of COVID-19 can be found at the following cell immune response to the virus that causes link: https://www.cdc.gov/coronavirus/2019- Coronavirus Disease 2019 (COVID-19) using the T- ncov/symptoms-testing/symptoms.html. Detect COVID Test. How are people tested for COVID-19? Two main kinds of tests are currently available for You should not interpret the results of this COVID-19: diagnostic tests and adaptive immune response tests. test to indicate the presence or absence of immunity or protection from COVID-19 • A diagnostic test tells you if you have a current infection. infection. • An adaptive immune response test tells you if you may have had a previous infection This Fact Sheet contains information to help you understand the risks and benefits of using this test to What is the T-Detect COVID Test? evaluate your adaptive immune response to SARS-CoV- This test is similar to an antibody test in that it measures 2, the virus that causes COVID-19. After reading this your adaptive immune response to SARS-CoV-2, the Fact Sheet, if you have questions or would like to virus that causes COVID-19. However in this case it discuss the information provided, please talk to your specifically measures your adaptive T-cell immune healthcare provider. -

Adaptive Immune Systems
Immunology 101 (for the Non-Immunologist) Abhinav Deol, MD Assistant Professor of Oncology Wayne State University/ Karmanos Cancer Institute, Detroit MI Presentation originally prepared and presented by Stephen Shiao MD, PhD Department of Radiation Oncology Cedars-Sinai Medical Center Disclosures Bristol-Myers Squibb – Contracted Research What is the immune system? A network of proteins, cells, tissues and organs all coordinated for one purpose: to defend one organism from another It is an infinitely adaptable system to combat the complex and endless variety of pathogens it must address Outline Structure of the immune system Anatomy of an immune response Role of the immune system in disease: infection, cancer and autoimmunity Organs of the Immune System Major organs of the immune system 1. Bone marrow – production of immune cells 2. Thymus – education of immune cells 3. Lymph Nodes – where an immune response is produced 4. Spleen – dual role for immune responses (especially antibody production) and cell recycling Origins of the Immune System B-Cell B-Cell Self-Renewing Common Progenitor Natural Killer Lymphoid Cell Progenitor Thymic T-Cell Selection Hematopoetic T-Cell Stem Cell Progenitor Dendritic Cell Myeloid Progenitor Granulocyte/M Macrophage onocyte Progenitor The Immune Response: The Art of War “Know your enemy and know yourself and you can fight a hundred battles without disaster.” -Sun Tzu, The Art of War Immunity: Two Systems and Their Key Players Adaptive Immunity Innate Immunity Dendritic cells (DC) B cells Phagocytes (Macrophages, Neutrophils) Natural Killer (NK) Cells T cells Dendritic Cells: “Commanders-in-Chief” • Function: Serve as the gateway between the innate and adaptive immune systems. -

Stress and the Immune System Tracy B
4 World Health • 47th Yeor, No. 2, Morch-Aprill994 Stress and the immune system Tracy B. Herbert any people have the effects of factors as diverse as experienced the examinations, bereavement, divorce, Mconnection between stress unemployment, mental arithmetic, and getting sick. Colds, influenza, and looking after a relative with herpes and allergies seem worse Alzheimer's di sease. In general, when we are severely stressed at these studies find that stress is work or in the home. Others are related to changes in both the never sick until they go on vacation numbers of white blood cells in (that is, after the stress is over), and circulation and the quantity of then they spend the whole time antibody in the blood. Moreover, fighting the virus. Because of stress is associated with changes in intrinsic connections like these, the functioning of immune cells. many researchers are today That is, there is a relatively large exploring whether (and how) stress decrease in both lymphocyte and illness are actually linked. One proliferation and natural killer cell specific focus of this research is to activity in individuals who have study the effects of stress on the experienced stress. There seems to immune systems; after all, if stress A lymphocyte: stress may weaken the capacity be some connection between the affects immunity, that would be one of lymphocytes to combat infection. duration of the stress and the amount way in which stress could contribute of immune change. For example, the to illness. longer the stress, the greater the The function of the immune proliferation"- by incubating these decrease in the number of specific system is to protect us from cells for several days with types of white blood cells. -

Rapid Induction of Antigen-Specific CD4+ T Cells Guides Coordinated Humoral and Cellular Immune Responses to SARS-Cov-2 Mrna Vaccination
bioRxiv preprint doi: https://doi.org/10.1101/2021.04.21.440862; this version posted April 22, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. Rapid induction of antigen-specific CD4+ T cells guides coordinated humoral and cellular immune responses to SARS-CoV-2 mRNA vaccination Authors: Mark M. Painter1,2, †, Divij Mathew1,2, †, Rishi R. Goel1,2, †, Sokratis A. Apostolidis1,2,3, †, Ajinkya Pattekar2, Oliva Kuthuru1, Amy E. Baxter1, Ramin S. Herati4, Derek A. Oldridge1,5, Sigrid Gouma6, Philip Hicks6, Sarah Dysinger6, Kendall A. Lundgreen6, Leticia Kuri-Cervantes1,6, Sharon Adamski2, Amanda Hicks2, Scott Korte2, Josephine R. Giles1,7,8, Madison E. Weirick6, Christopher M. McAllister6, Jeanette Dougherty1, Sherea Long1, Kurt D’Andrea1, Jacob T. Hamilton2,6, Michael R. Betts1,6, Paul Bates6, Scott E. Hensley6, Alba Grifoni9, Daniela Weiskopf9, Alessandro Sette9, Allison R. Greenplate1,2, E. John Wherry1,2,7,8,* Affiliations 1 Institute for Immunology, University of Pennsylvania Perelman School of Medicine, Philadelphia, PA, USA 2 Immune Health™, University of Pennsylvania Perelman School of Medicine, Philadelphia, PA, USA 3 Division of Rheumatology, University of Pennsylvania Perelman School of Medicine, Philadelphia, PA, USA 4 NYU Langone Vaccine Center, Department of Medicine, New York University School of Medicine, New York, NY 5 Department -

Objectives Complement (C') Complement Proteins Functions Of
Complement Objectives Foundations of Public Health Identify functions of complement Immunology Recognize the similarities and differences of the three complement pathways Complement Identify important complement components & their functions Identify deleterious effects of complement activation and deficiency 1 2 Complement (C’) Complement Proteins Synthesized in the liver and by several Series of approximately 30 heat-labile proteins cells types (splenic macrophages) Normally inactive in the serum Plays an essential role in Inactive complement proteins known as zymogens inflammation and in facilitating Can be sequentially activated in a antibody effectiveness controlled sequence Amplification of the reaction occurs at each step Severe infections or autoimmune Production of biologically active fragments diseases can result from complement for lysis or killing of the target deficiencies (rare in the population) 3 4 Functions of Complement Functions of Complement Essential role in inflammation Assists antibodies in effector functions (Antibody Dependent Cell- mediated Cytotoxicity- ADCC) Assist in clearing immune complexes Opsonization and facilitation of phagocytosis No antigen specificity 5 6 1 Complement 3 Pathways of Activation Complement Activators Classical Triggered when IgM or certain IgG subclasses bind antigens Alternative (Properdin) Triggered by the deposition of complement protein, C3b, onto microbial surfaces No antibodies required for activation Lectin Triggered by the attachment of plasma mannose-binding lectin (MBL) to microbes No antibodies required for Activators start the domino effect… activation 7 8 Early Steps Late Steps The initial steps vary between pathways Dependent on activating substance C3 convertase quickly forms in all paths to cleave C3 Watch this well-done animation on the activation of complement, the Late steps (after C5 convertase) are same in all pathways steps in the complement pathways, Lead to formation of MAC & the functions of complement. -

Hormones and the Immune Response
Ann Rheum Dis: first published as 10.1136/ard.48.1.1 on 1 January 1989. Downloaded from Annals of the Rheumatic Diseases, 1989; 48, 1-6 Review Hormones and the immune response Recent advances suggest that the immune system cells, are present on mouse spleen cells3 and human does not function in isolation but is influenced by peripheral blood mononuclear cells.4 Receptors, other physiological systems such as the endocrine identical to those in the central nervous system, for and neuroendocrine systems. This review discusses methionine enkephalin are present on splenocytes aspects of immune function altered by neuroendo- and T lymphocytes.3 In contrast, leucine enkephalin crine peptides, sex hormones, and vitamin D and j3-endorphin receptors on T lymphocyte differ metabolites. from those in the central nervous system as binding cannot be inhibited by opiate antagonists.5 6 In the Neuroendocrine effects case of ,3-endorphin the bindings occur through its carboxy terminal, whereas opiates bind their A system of bidirectional communication between receptor through the amino terminus. This raises the immune and neuroendocrine system exists, in an interesting possibility that a peptide such as which the two systems share a common set of f6-endorphin could form a bridge between two hormones and receptors.'2 Not only do immune lymphocyte subtypes by binding to one through its for peptides, to the and cells possess receptors neuroendocrine amino terminus opiate receptor through copyright. they are also capable of synthesising them and of its carboxy terminus to the non-opiate receptor on responding to them. Products of immune cells affect another lymphocyte.4 the central nervous system, which possesses recep- Other neuroendocrine peptide receptors present tors for cytokines and can also synthesise them on leucocztes include those for neurotensin,7 sub- (Fig. -

Complement Herbert L
Host Defense 2011 Complement Herbert L. Mathews, Ph.D. COMPLEMENT Date: 4/11/11 Reading Assignment: Janeway’s Immunobiology, 7th Edition, pp. 54-55, 61-82, 406- 409, 514-515. Figures: (Unless otherwise noted) Janeway’s Immunobiology, 7th Edition, Murphy et al., Garland Publishing. KEY CONCEPTS AND LEARNING OBJECTIVES You will be able to describe the mechanism and consequences of the activation of the complement system. To attain the goals for these lectures you will be able to: a. List the components of the complement system. b. Describe the three activation pathways for complement. c. Explain the consequences of complement activation. d. Describe the consequence of complement deficiency. Page 1 Host Defense 2011 Complement Herbert L. Mathews, Ph.D. CONTENT SUMMARY Introduction Nomenclature Activation of Complement The classical pathway The mannan-binding lectin pathway The alternative pathway Biological Consequence of Complement Activation Cell lysis and viral neutralization Opsonization Clearance of Immune Complexes Inflammation Regulation of Complement Activation Human Complement Component Deficiencies Page 2 Host Defense 2011 Complement Herbert L. Mathews, Ph.D. Introduction The complement system is a group of more than 30 plasma and membrane proteins that play a critical role in host defense. When activated, complement components interact in a highly regulated fashion to generate products that: Recruit inflammatory cells (promoting inflammation). Opsonize microbial pathogens and immune complexes (facilitating antigen clearance). Kill microbial pathogens (via a lytic mechanism known as the membrane attack complex). Generate an inflammatory response. Complement activation takes place on antigenic surfaces. However, the activation of complement generates several soluble fragments that have important biologic activity. -

Understanding the Immune System: How It Works
Understanding the Immune System How It Works U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES NATIONAL INSTITUTES OF HEALTH National Institute of Allergy and Infectious Diseases National Cancer Institute Understanding the Immune System How It Works U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES NATIONAL INSTITUTES OF HEALTH National Institute of Allergy and Infectious Diseases National Cancer Institute NIH Publication No. 03-5423 September 2003 www.niaid.nih.gov www.nci.nih.gov Contents 1 Introduction 2 Self and Nonself 3 The Structure of the Immune System 7 Immune Cells and Their Products 19 Mounting an Immune Response 24 Immunity: Natural and Acquired 28 Disorders of the Immune System 34 Immunology and Transplants 36 Immunity and Cancer 39 The Immune System and the Nervous System 40 Frontiers in Immunology 45 Summary 47 Glossary Introduction he immune system is a network of Tcells, tissues*, and organs that work together to defend the body against attacks by “foreign” invaders. These are primarily microbes (germs)—tiny, infection-causing Bacteria: organisms such as bacteria, viruses, streptococci parasites, and fungi. Because the human body provides an ideal environment for many microbes, they try to break in. It is the immune system’s job to keep them out or, failing that, to seek out and destroy them. Virus: When the immune system hits the wrong herpes virus target or is crippled, however, it can unleash a torrent of diseases, including allergy, arthritis, or AIDS. The immune system is amazingly complex. It can recognize and remember millions of Parasite: different enemies, and it can produce schistosome secretions and cells to match up with and wipe out each one of them. -

Immunology 101
Immunology 101 Justin Kline, M.D. Assistant Professor of Medicine Section of Hematology/Oncology Committee on Immunology University of Chicago Medicine Disclosures • I served as a consultant on Advisory Boards for Merck and Seattle Genetics. • I will discuss non-FDA-approved therapies for cancer 2 Outline • Innate and adaptive immune systems – brief intro • How immune responses against cancer are generated • Cancer antigens in the era of cancer exome sequencing • Dendritic cells • T cells • Cancer immune evasion • Cancer immunotherapies – brief intro 3 The immune system • Evolved to provide protection against invasive pathogens • Consists of a variety of cells and proteins whose purpose is to generate immune responses against micro-organisms • The immune system is “educated” to attack foreign invaders, but at the same time, leave healthy, self-tissues unharmed • The immune system can sometimes recognize and kill cancer cells • 2 main branches • Innate immune system – Initial responders • Adaptive immune system – Tailored attack 4 The immune system – a division of labor Innate immune system • Initial recognition of non-self (i.e. infection, cancer) • Comprised of cells (granulocytes, monocytes, dendritic cells and NK cells) and proteins (complement) • Recognizes non-self via receptors that “see” microbial structures (cell wall components, DNA, RNA) • Pattern recognition receptors (PRRs) • Necessary for priming adaptive immune responses 5 The immune system – a division of labor Adaptive immune system • Provides nearly unlimited diversity of receptors to protect the host from infection • B cells and T cells • Have unique receptors generated during development • B cells produce antibodies which help fight infection • T cells patrol for infected or cancerous cells • Recognize “foreign” or abnormal proteins on the cell surface • 100,000,000 unique T cells are present in all of us • Retains “memory” against infections and in some cases, cancer. -

How Are White Blood Cells Classified?
How are white blood cells classified? Copyright 2017 by the Rector and Visitors of the University of Virginia How are white blood cells classified? Types of White Blood Cells: Neutrophil Eosinophil Basophil Lymphocyte Monocyte . The types of white blood cells are shown above. The next page will describe lymphocytes in further detail. A healthy individual has all of these white blood cells types, but within specific ranges. Deviation from these ranges can indicate acute illness or a chronic disease. A mnemonic that is often used to remember the relative amount of each white blood cell that should be present is “Never Let Monkeys Eat Bananas.” Never Neutrophil Highest amounts Let Lymphocyte Monkeys Monocyte Eat Eosinophil Bananas Basophil Lowest amounts . In other words, neutrophils should always be present in higher amounts compared to the other cell types. This will be described further in “A first step in diagnosing LGL leukemia: The blood smear.” Copyright 2017 by the Rector and Visitors of the University of Virginia How are white blood cells classified? Introduction: White blood cells are blood cells that fight infection and disease. Lymphocytes are a type of white blood cell. They can identify antigens (substances foreign to the body) and cause an immune response. There are three types of lymphocytes: T-cell, NK-cell, and B-cell. In healthy adults, 10-15% of the lymphocytes are large granular lymphocytes (LGLs). To learn more about LGL cells, see “A first step in diagnosing LGL leukemia: The blood smear.” A person is diagnosed with LGL leukemia if there is a clonal (copied) population of T-cells or NK-cells present. -

Activation of the Complement System on Human Endothelial Cells by Urban Particulate Matter Triggers Inflammation-Related Protein Production
International Journal of Molecular Sciences Article Activation of the Complement System on Human Endothelial Cells by Urban Particulate Matter Triggers Inflammation-Related Protein Production Myoung Su Choi 1,† , Hyungtaek Jeon 2,†, Seung-Min Yoo 2 and Myung-Shin Lee 2,* 1 Department of Otorhinolaryngology, Eulji University Medical Center, Eulji University School of Medicine, Daejeon 35233, Korea; [email protected] 2 Department of Microbiology and Immunology, Eulji University School of Medicine, Daejeon 34824, Korea; [email protected] (H.J.); [email protected] (S.-M.Y.) * Correspondence: [email protected]; Tel.: +82-42-259-1662 † These authors have contributed equally to this work. Abstract: Exposure to particulate matter (PM) is becoming a major global health issue. The amount and time of exposure to PM are known to be closely associated with cardiovascular diseases. However, the mechanism through which PM affects the vascular system is still not clear. Endothelial cells line the interior surface of blood vessels and actively interact with plasma proteins, including the complement system. Unregulated complement activation caused by invaders, such as pollutants, may promote endothelial inflammation. In the present study, we sought to investigate whether urban PM (UPM) acts on the endothelial environment via the complement system. UPM-treated human endothelial cells with normal human serum showed the deposition of membrane attack complexes Citation: Choi, M.S.; Jeon, H.; Yoo, (MACs) on the cell surface via the alternative pathway of the complement system. Despite the forma- S.-M.; Lee, M.-S. Activation of the tion of MACs, cell death was not observed, and cell proliferation was increased in UPM-mediated Complement System on Human complement activation. -

Vaccine Immunology Claire-Anne Siegrist
2 Vaccine Immunology Claire-Anne Siegrist To generate vaccine-mediated protection is a complex chal- non–antigen-specifc responses possibly leading to allergy, lenge. Currently available vaccines have largely been devel- autoimmunity, or even premature death—are being raised. oped empirically, with little or no understanding of how they Certain “off-targets effects” of vaccines have also been recog- activate the immune system. Their early protective effcacy is nized and call for studies to quantify their impact and identify primarily conferred by the induction of antigen-specifc anti- the mechanisms at play. The objective of this chapter is to bodies (Box 2.1). However, there is more to antibody- extract from the complex and rapidly evolving feld of immu- mediated protection than the peak of vaccine-induced nology the main concepts that are useful to better address antibody titers. The quality of such antibodies (e.g., their these important questions. avidity, specifcity, or neutralizing capacity) has been identi- fed as a determining factor in effcacy. Long-term protection HOW DO VACCINES MEDIATE PROTECTION? requires the persistence of vaccine antibodies above protective thresholds and/or the maintenance of immune memory cells Vaccines protect by inducing effector mechanisms (cells or capable of rapid and effective reactivation with subsequent molecules) capable of rapidly controlling replicating patho- microbial exposure. The determinants of immune memory gens or inactivating their toxic components. Vaccine-induced induction, as well as the relative contribution of persisting immune effectors (Table 2.1) are essentially antibodies— antibodies and of immune memory to protection against spe- produced by B lymphocytes—capable of binding specifcally cifc diseases, are essential parameters of long-term vaccine to a toxin or a pathogen.2 Other potential effectors are cyto- effcacy.