Causes of Hypocalcaemia Hypoparathyroid Nonparathyroid PTH Resistance
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Calciphylaxis with Normal Renal and Parathyroid Function Not As Rare As Previously Believed
OBSERVATION Calciphylaxis With Normal Renal and Parathyroid Function Not as Rare as Previously Believed Andrew H. Kalajian, MD; Paula S. Malhotra, MD; Jeffrey P. Callen, MD; Lynn P. Parker, MD Background: Calciphylaxis is a life-threatening form of previously reported cases of nontraditional calciphylaxis metastatic calcification-induced microvascular occlusion identified the following patient characteristics that high- syndrome. Although traditionally observed in patients with light clinical situations potentially predisposing to calci- end-stage renal disease and/or hyperparathyroidism, the phylaxis: hypoalbuminemia, malignant neoplasm, sys- development of calciphylaxis in “nontraditional” pa- temic corticosteroid use, anticoagulation with warfarin tients having both normal renal and parathyroid func- sodium or phenprocoumon, chemotherapy, systemic in- tion has been reported. However, to date there has been flammation, hepatic cirrhosis, protein C or S deficiency, no collective analysis identifying common patient char- obesity, rapid weight loss, and infection. acteristics potentially predisposing to the development of calciphylaxis in nontraditional patients. Conclusions: Calciphylaxis is becoming increasingly common in patients with normal renal and parathyroid Observations: A 58-year-old woman with endometrial function. The observations from this study may assist der- carcinoma developed extensive calciphylaxis despite the matologists in the rapid diagnosis and prompt initiation presence of normal renal and parathyroid function. -

Soft Tissue Calcification and Ossification
Soft Tissue Calcification and Ossification Soft-tissue Calcification Metastatic Calcification =deposit of calcium salts in previously normal tissue (1) as a result of elevation of Ca x P product above 60-70 (2) with normal Ca x P product after renal transplant Location:lung (alveolar septa, bronchial wall, vessel wall), kidney, gastric mucosa, heart, peripheral vessels Cause: (a)Skeletal deossification 1.1° HPT 2.Ectopic HPT production (lung / kidney tumor) 3.Renal osteodystrophy + 2° HPT 4.Hypoparathyroidism (b)Massive bone destruction 1.Widespread bone metastases 2.Plasma cell myeloma 3.Leukemia Dystrophic Calcification (c)Increased intestinal absorption =in presence of normal serum Ca + P levels secondary to local electrolyte / enzyme alterations in areas of tissue injury 1.Hypervitaminosis D Cause: 2.Milk-alkali syndrome (a)Metabolic disorder without hypercalcemia 3.Excess ingestion / IV administration of calcium salts 1.Renal osteodystrophy with 2° HPT 4.Prolonged immobilization 2.Hypoparathyroidism 5.Sarcoidosis 3.Pseudohypoparathyroidism (d)Idiopathic hypercalcemia 4.Pseudopseudohypoparathyroidism 5.Gout 6.Pseudogout = chondrocalcinosis 7.Ochronosis = alkaptonuria 8.Diabetes mellitus (b) Connective tissue disorder 1.Scleroderma 2.Dermatomyositis 3.Systemic lupus erythematosus (c)Trauma 1.Neuropathic calcifications 2.Frostbite 3.Myositis ossificans progressiva 4.Calcific tendinitis / bursitis (d)Infestation 1.Cysticercosis Generalized Calcinosis 2.Dracunculosis (guinea worm) (a)Collagen vascular disorders 3.Loiasis 1.Scleroderma -

Epileptic Seizure, As the First Symptom of Hypoparathyroidism in Children, Does Not Require Antiepileptic Drugs
Childs Nerv Syst DOI 10.1007/s00381-016-3264-2 ORIGINAL PAPER Epileptic seizure, as the first symptom of hypoparathyroidism in children, does not require antiepileptic drugs Meng-Jia Liu1 & Jiu-Wei Li2 & Xiu-Yu Shi1 & Lin-Yan Hu1 & Li-Ping Zou1,3 Received: 28 May 2016 /Accepted: 3 October 2016 # The Author(s) 2016. This article is published with open access at Springerlink.com Abstract Introduction Objective Patients with hypoparathyroidism exhibit metabol- ic disorders (hypocalcemia) and brain structural abnormalities Epileptic seizure occurs when a burst of electrical impulses in (brain calcifications). Currently, studies have determined the brain exceeds the normal limits. Its manifestation can vary whether antiepileptic drug (AED) treatment is required for from uncontrolled jerking movement (tonic–clonic seizure) to epileptic seizures in children with hypoparathyroidism. momentary loss of awareness (absence seizure). These im- Method This study aims to evaluate the data of two medical pulses spread to adjacent areas in the brain and create an un- centers in Beijing based on the diagnosis of epileptic seizures controlled storm of electrical activity. Brain diseases character- as the first symptom of hypoparathyroidism in children. ized by enduring predisposition to generate epileptic seizures Result A total of 42 patients were included and assigned into are collectively called epilepsy. According to pathogenesis, ep- AED and non-AED treatment groups in a 1:2 matched case– ilepsy can be classified into six categories: metabolic, structural, control study. Results show that the seizure outcome after inherited, immunologic, inflammatory, and idiopathic. 1 year of AED treatment is not significantly different from Hypoparathyroidism is an endocrine disease that results that of the control. -

Electrolyte Disorders in Cancer Patients: a Systematic Review
Berardi et al. J Cancer Metastasis Treat 2019;5:79 Journal of Cancer DOI: 10.20517/2394-4722.2019.008 Metastasis and Treatment Review Open Access Electrolyte disorders in cancer patients: a systematic review Rossana Berardi, Mariangela Torniai, Edoardo Lenci, Federica Pecci, Francesca Morgese, Silvia Rinaldi Clinica Oncologica, Università Politecnica delle Marche, Azienda Ospedaliero-Universitaria Ospedali Riuniti Umberto I - GM Lancisi - G Salesi, Ancona 60126, Italy. Correspondence to: Prof. Rossana Berardi, Clinica Oncologica, Università Politecnica delle Marche, Azienda Ospedaliero- Universitaria Ospedali Riuniti di Ancona, Via Conca 71, Ancona 60126, Italy. E-mail: [email protected] How to cite this article: Berardi R, Torniai M, Lenci E, Pecci F, Morgese F, Rinaldi S. Electrolyte disorders in cancer patients: a systematic review. J Cancer Metastasis Treat 2019;5:79. http://dx.doi.org/10.20517/2394-4722.2019.008 Received: 26 Apr 2019 First Decision: 26 Jul 2019 Revised: 20 Nov 2019 Accepted: 20 Nov 2019 Published: 9 Dec 2019 Science Editor: Stephen J. Ralph Copy Editor: Jing-Wen Zhang Production Editor: Jing Yu Abstract Electrolyte disorders are very common complications in cancer patients. They might be associated to a worsening outcome, influencing quality of life, possibility to receive anticancer drugs, and conditioning survival. In fact, they might provoke important morbidity, with dysfunction of multiple organs and rarely causing life-threatening conditions. Moreover, recent studies showed that they might worsen cancer patients’ outcome, while a prompt correction seems to have a positive impact. Furthermore, there is evidence of a correlation between electrolyte alterations and poorer performance status, delays in therapy commencement and continuation, and negative treatment outcomes. -
Quick Guide to Laboratory Values
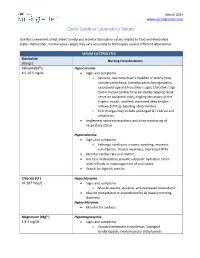
March 2021 www.nursingcenter.com Quick Guide to Laboratory Values Use this convenient cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal value ranges may vary according to techniques used in different laboratories. SERUM ELECTROLYTES Electrolyte Nursing Considerations (Range) Calcium (Ca2+) Hypocalcemia 8.5-10.5 mg/dL • Signs and symptoms o Seizures, neuromuscular irritability or tetany (may include paresthesia, bronchospasm, laryngospasm, carpopedal spasm [Trousseau’s sign], Chvostek’s sign [facial muscle contractions elicited by tapping facial nerve on ipsilateral side], tingling sensations of the fingers, mouth, and feet, increased deep tendon reflexes [DTRs]), bleeding abnormalities o ECG changes may include prolonged QT interval and arrythmias. • Implement seizure precautions and close monitoring of respiratory status. Hypercalcemia • Signs and symptoms o Lethargy, confusion, nausea, vomiting, anorexia, constipation, muscle weakness, depressed DTRs • Monitor cardiac rate and rhythm. • Increase mobilization, provide adequate hydration either with IV fluids or encouragement of oral intake. • Watch for digitalis toxicity. Chloride (Cl-) Hypochloremia 97-107 mEq/L • Signs and symptoms o Muscle spasms, alkalosis, and depressed respirations • May be precipitated or exacerbated by GI losses (vomiting, diarrhea). Hyperchloremia • Monitor for acidosis. Magnesium (Mg2+) Hypomagnesemia 1.8-3 mg/dL • Signs and symptoms o Cardiac/ventricular arrhythmias, laryngeal stridor/spasm, neuromuscular -
Fluid and Electrolyte Balance
Fluid and Electrolyte Balance Done By: Faisal S. AlGhamdi Abdullah Almousa Total Body Fluids and fluids compartment: 60% in male of Total body weight 55% in female 2/3 (65%) of TBW is intracellular (ICF) 1/3 (35%) extracellular water – 25 % interstitial fluid (ISF) – 5 - 7 % in plasma (IVF intravascular fluid) – 1- 2 % in transcellular fluids – CSF, intraocular fluids, serous membranes, and in GI, respiratory and urinary tracts (third space) • Fluid compartments are separated by membranes that are freely permeable to water. • Movement of fluids due to: – Hydrostatic pressure (Fluid) – Osmotic/Oncotic pressure (tissue) In Hydrostatic pressure: As the pressure increase as the movement of fluid outside increase In Osmotic pressure: As the pressure increase as the absorption of fluid increase. Fluid balance: • Neutral balance: input = output • Positive balance: input > output • Negative balance: input < output (+ve lead to edema, and -ve lead to dehydration) Daily input should = Daily output Most of water intake in Beverages Most of water output in Urine Electrolytes: Cations – positively charged ions . Na+, K+ , Ca++, H+ Anions – negatively charged ions - - 3- . Cl , HCO3 , PO4 Intracellular fluid space: • 40% of body weight • Largest proportion is in skeletal muscle • Larger percentage of water is Intracellular in males (large muscle mass) • Cations = Potassium & Magnesium • Anions = Phosphates and Proteins Extracellular fluid space: • 20% of body weight • Interstitial 15%, Plasma 5% • Cations = Sodium • Anions = Chloride and Bicarbonate Homeostasis: • Maintained by Ion transport, Water movement and Kidney function. • Tonicity Isotonic, Hypertonic and Hypotonic (the difference btw tonicity and osmolarity that tonicity is concentration of solutions in relation to adjacent compartments *like concentration of plasma compared to interstitial space*, but osmolarity take the compartment on it’s own) Movement of body fluids: “ Where Na goes, H2O follows” Diffusion – movement of particles down a concentration gradient. -

Fluid & Electrolytes Fluid Balance Sodium 135-145 Meq/L
11/24/2009 Fluid & Electrolytes The Basics Fluid Balance Sodium 135‐145 meq/L • Imbalances typically associated with parallel changes in osmolality • Plays a major role in – ECF volume and concenttitration – Generation and transmission of nerve impulses – Acid–base balance 1 11/24/2009 Hypernatremia • Elevated serum sodium occurring with water loss or sodium gain • Causes hyperosmolality leading to cellular dehydration • Primary protection is thirst from hypothalamus Differential Assessment of ECF Volume Hypernatremia • Manifestations – Thirst, lethargy, agitation, seizures, and coma • Impaired LOC • Produced by clinical states – Central or nephrogenic diabetes insipidus – Serum sodium levels must be reduced gradually to avoid cerebral edema 2 11/24/2009 Nursing Management Nursing Diagnoses • Potential complication: seizures and coma leading to irreversible brain damage • Management • Treat undliderlying cause • If oral fluids cannot be ingested, IV solution of 5% dextrose in water or hypotonic saline • Diuretics Hyponatremia • Results from loss of sodium‐containing fluids or from water excess • Manifestations – CfiConfusion, nausea, vomiting, seizures, and coma Nursing Management Nursing Diagnoses • Risk for injury • Potential complication: severe neurologic changes • Management • Abnormal fluid loss – Fluid replacement with sodium‐containing solution • Caused by water excess – Fluid restriction is needed • Severe symptoms (seizures) – Give small amount of IV hypertonic saline solution (3% NaCl) 3 11/24/2009 Potassium 3.5‐5.5 meq/L • -

T PATHOLOGIC CALCIFICATION Deposition of Calcium Salts In
t PATHOLOGIC CALCIFICATION Deposition of calcium salts in tissues other than osteoid or enamel is called pathologic or heterotopic calcification. Two distinct types of pathologic calcification are recognised: Dystrophic calcification, which is characterised by deposition of calcium salts in dead or degenerated tissues with normal calcium metabolism and normal serum calcium levels. Dystrophic calcification may occur due to 2 types of causes: ● Calcification in dead tissue ● Calcification of degenerated tissue Metastatic calcification, on the other hand, occurs in apparently normal tissues and is associated with deranged calcium metabolism and hypercalcaemia. Since metastatic calcification occurs in normal tissues due to hypercalcaemia, its causes would include one of the following two conditions: ● Excessive mobilisation of calcium from the bone. ● Excessive absorption of calcium from the gut. Pathogenesis of Dystrophic Calcification The process of dystrophic calcification has been likened to the formation of normal hydroxyapatite in the bone involving 2 phases: ● Initiation and propagation: Initiation is the phase in which precipitates of calcium phosphate begin to accumulate intracellularly in the mitochondria, or extracellularly in membrane-bound vesicles. Propagation is the phase in which minerals deposited in the initiation phase are propagated to form mineral crystals. Pathogenesis of metastatic calcification Metastatic calcification occurs due to excessive binding of inorganic phosphate ions with calcium ions, which are elevated due to underlying metabolic derangement. This leads to formation of precipitates of calcium phosphate at the preferential sites. Metastatic calcification is reversible upon correction of underlying metabolic disorder. GANGRENE Gangrene is a form of necrosis of tissue with superadded putrefaction. The type of necrosis is usually coagulative due to ischaemia (e.g. -

Parenteral Nutrition Primer: Balance Acid-Base, Fluid and Electrolytes
Parenteral Nutrition Primer: Balancing Acid-Base, Fluids and Electrolytes Phil Ayers, PharmD, BCNSP, FASHP Todd W. Canada, PharmD, BCNSP, FASHP, FTSHP Michael Kraft, PharmD, BCNSP Gordon S. Sacks, Pharm.D., BCNSP, FCCP Disclosure . The program chair and presenters for this continuing education activity have reported no relevant financial relationships, except: . Phil Ayers - ASPEN: Board Member/Advisory Panel; B Braun: Consultant; Baxter: Consultant; Fresenius Kabi: Consultant; Janssen: Consultant; Mallinckrodt: Consultant . Todd Canada - Fresenius Kabi: Board Member/Advisory Panel, Consultant, Speaker's Bureau • Michael Kraft - Rockwell Medical: Consultant; Fresenius Kabi: Advisory Board; B. Braun: Advisory Board; Takeda Pharmaceuticals: Speaker’s Bureau (spouse) . Gordon Sacks - Grant Support: Fresenius Kabi Sodium Disorders and Fluid Balance Gordon S. Sacks, Pharm.D., BCNSP Professor and Department Head Department of Pharmacy Practice Harrison School of Pharmacy Auburn University Learning Objectives Upon completion of this session, the learner will be able to: 1. Differentiate between hypovolemic, euvolemic, and hypervolemic hyponatremia 2. Recommend appropriate changes in nutrition support formulations when hyponatremia occurs 3. Identify drug-induced causes of hypo- and hypernatremia No sodium for you! Presentation Outline . Overview of sodium and water . Dehydration vs. Volume Depletion . Water requirements & Equations . Hyponatremia • Hypotonic o Hypovolemic o Euvolemic o Hypervolemic . Hypernatremia • Hypovolemic • Euvolemic • Hypervolemic Sodium and Fluid Balance . Helpful hint: total body sodium determines volume status, not sodium status . Examples of this concept • Hypervolemic – too much volume • Hypovolemic – too little volume • Euvolemic – normal volume Water Distribution . Total body water content varies from 50-70% of body weight • Dependent on lean body mass: fat ratio o Fat water content is ~10% compared to ~75% for muscle mass . -

Hyperemesis Gravidarum with Paraparesis and Tetany
Open Access Case Report DOI: 10.7759/cureus.17014 Hyperemesis Gravidarum With Paraparesis and Tetany Jyotsnaa Muralitharan 1 , Vijayakumar Nagarajan 1 , Umarani Ravichandran 1 1. Internal Medicine, Rajah Muthiah Medical College & Hospital, Chidambaram, IND Corresponding author: Jyotsnaa Muralitharan, [email protected] Abstract Subacute-onset muscle weakness can result from channelopathies, inflammatory myopathies, thyroid dysfunction, hypoparathyroidism, vitamin D deficiency, and dyselectrolytemias like hypokalemia, hypocalcemia, and hypomagnesemia. We report a curious and extremely rare case of a 29-year-old woman with hyperemesis gravidarum presenting with disabling muscle weakness involving her lower limbs and trunk, and concurrent features of tetany. Following voluminous vomiting over the last two months, she presented with history of weakness of her lower limbs of 14 days duration, resulting in difficulty in her getting out of bed or walking unassisted. On examination, she was hypotensive (80/60 mmHg) and tachycardic (110 bpm), with flaccid weakness of her lower limbs (proximal weakness more than distal weakness - power of 1/5 at the hips bilaterally, and 3/5 at the knees and ankles bilaterally) and diminished deep tendon reflexes. She also had positive Trousseau’s sign and Chvostek’s sign. Interestingly, she also had thinned-out bluish sclerae, a high-arched palate, short stature, and bilateral conductive hearing loss. Laboratory evaluation revealed anemia, hyponatremia, hypokalemia, hypomagnesemia, hypochloremia, hypophosphatemia, and low vitamin D levels. Electrocardiogram showed prolonged QT interval. Her thyroid function test and parathyroid levels were normal. With parenteral replenishment of the electrolytes and vitamin D, her power improved and she was discharged on oral supplements. Thus, this case report demonstrates the importance of aggressive, early, and adequate management of hyperemesis gravidarum to prevent dyselectrolytemia-associated paraparesis. -

Calcium and Phosphorous Metabolism
CALCIUM AND PHOSPHOROUS METABOLISM -DR. SUHASINI. G P Lecturer Dept. of Oral Pathology & Microbiology Dr. Suhasini GP, Subharti Dental College, SVSU INTRODUCTION • Metabolism (Greek, Metabote= change) • Sum of the chemical and physical changes in tissue consisting of anabolism (reactions that convert small molecules into large) & catabolism (reactions that convert large molecules into small) Dr. Suhasini GP, Subharti Dental College, SVSU Functions of Calcium • Most abundant mineral • Most important inorganic cation in mineralised tissue- structural role • [Ca10(PO4)6(OH)2] in bone, dentin, cementum & enamel Dr. Suhasini GP, Subharti Dental College, SVSU Functions Formation of bone and teeth Controls secretion of glandular cells Muscle contraction Clotting of blood Neuromuscular excitability Cell-cell adhesion, cell integrity Intracellular second messenger in harmonal actions Dr. Suhasini GP, Subharti Dental College, SVSU Dietary requirements • Adults- 0.8 gms/day • Children & pregnant and lactating women- additional 1gm of Ca supplements/day • Postmenopausal women Dr. Suhasini GP, Subharti Dental College, SVSU Sources • Milk & its products • Green leafy veg (oxalic acid and phytic acid- reduces absorption) • Raagi • Egg yolk • Legumes • Nuts • Dried fish • Pan chewing with slacked lime • Drinking water Dr. Suhasini GP, Subharti Dental College, SVSU Distribution of Ca++` • Essentially distributed extracellularly • 1.2-1.4 kg in 70kg adult • 99%-skeleton • 1%- soft tissue+ body fluids Dr. Suhasini GP, Subharti Dental College, SVSU Bone Ca++ Exists in 2 forms- • Readily exchangeable form- simple exchange b/n newly deposited bone & exctracellular Ca++ • Stable form- constant formation & resorption of bone- – Controlled by PTH, calcitonin & vit.D Dr. Suhasini GP, Subharti Dental College, SVSU Blood Ca++ • Plasma, little in RBC • 9-11mg/dl- constant • In plasma- 1. -
Sir, Metastatic Calcification in the Eye Is Often Seen in the Cornea and the Interpalpebral Conjunctiva. in Hypercalcaemic Subje
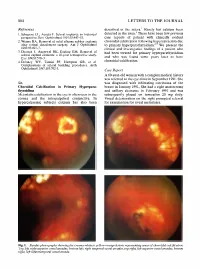
804 LETTERS TO THE JOURNAL References described in the sclera.1 Rarely has calcium been 1 1. Schepens CL, Acosta F. Scleral implants: an historical detected in the uvea. There have been few previous perspective. Surv OphthalmoI1991;35:447-53. case reports of patient with clinically evident 2. Wizina RA. Removal of solid silicone rubber explants choroidal calcification following hypercalcaemia due after retinal detachment surgery. Am J Ophthalmol to primary hyperparathyroidism 2. We present the 1983;95:495-7. clinical and investigative findings of a patient who 3. Deutsch J, Aggarwal RK, Eagling EM. Removal of had been treated for primary hyperparathyroidism · scleral explant elements: a 10-year retrospective study. and who was found some years later to have Eye 1992;6:570-3. choroidal calcification. 4. Delaney WV, Tomisi PF, Hampton GR, et al. Complications of scleral buckling procedures. Arch OphthalmoI1987;105:702-3. Case Report A 60-year-old woman with a complex medical history was referred to the eye clinic in September 1991. She Sir, was diagnosed with infiltrating carcinoma of the Choroidal Calcification in Primary Hyperpara breast in January 1991. She had a right mastectomy thyroidism and axillary clearance in February 1991 and was Metastatic calcificationin the eye is often seen in the subsequently placed on tamoxifen 20 mg daily. cornea and the interpalpebral conjunctiva. In Visual deterioration on the right prompted referral hypercalcaemic subjects calcium has also been for examination for uveal metastases. Fig. 1. Fundus photographs showing the creamy-white to yellow-orange lesions representing areas of choroidal calcification: Top left, right superior vessel arcades; bottom left, right temporal vessel arcades; top right, left superior vessel arcades; bottom right, left inferotemporal vessel arcade.