Hyperemesis Gravidarum with Paraparesis and Tetany
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Association Between Hypocalcemia and Outcome in COVID-19 Patients: a Retrospective Study
The Association Between Hypocalcemia and Outcome in COVID-19 Patients: a Retrospective Study Bhagwan Singh Patidar All India Institute of Medical Sciences Tapasyapreeti Mukhopadhayay All India Institute of Medical Sciences Arulselvi Subramanian ( [email protected] ) All India Institute of Medical Sciences https://orcid.org/0000-0001-7797-6683 Riicha Aggarwal All India Institute of Medical Sciences Kapil Dev Soni All India Institute of Medical Sciences Neeraj Nischal All India Institute of Medical Sciences Debasis Sahoo All India Institute of Medical Sciences Surbhi Surbhi All India Institute of Medical Sciences Ravindra Mohan Pandey All India Institute of Medical Sciences Naveet Wig All India Institute of Medical Sciences Rajesh Malhotra All India Institute of Medical Sciences Anjan Trikha All India Institute of Medical Sciences Research Article Keywords: Calcium, Coronavirus, Laboratory parameters, Mortality, NLR, Pandemic Posted Date: March 16th, 2021 DOI: https://doi.org/10.21203/rs.3.rs-302159/v1 Page 1/14 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 2/14 Abstract Background: Calcium has been shown to have a vital role in the pathophysiology of SARS-CoV and MERS-CoV diseases but less is known about hypocalcemia in COVID-19 patients and its association with the disease severity and the nal outcome. Therefore, this study was conducted with an aim to assess the clinical features in the COVID-19 patients having hypocalcemia and to observe its impact on COVID- 19 disease severity and nal outcome. Method: In this retrospective study, consecutive COVID-19 patients of all age groups were enrolled. -

Epileptic Seizure, As the First Symptom of Hypoparathyroidism in Children, Does Not Require Antiepileptic Drugs
Childs Nerv Syst DOI 10.1007/s00381-016-3264-2 ORIGINAL PAPER Epileptic seizure, as the first symptom of hypoparathyroidism in children, does not require antiepileptic drugs Meng-Jia Liu1 & Jiu-Wei Li2 & Xiu-Yu Shi1 & Lin-Yan Hu1 & Li-Ping Zou1,3 Received: 28 May 2016 /Accepted: 3 October 2016 # The Author(s) 2016. This article is published with open access at Springerlink.com Abstract Introduction Objective Patients with hypoparathyroidism exhibit metabol- ic disorders (hypocalcemia) and brain structural abnormalities Epileptic seizure occurs when a burst of electrical impulses in (brain calcifications). Currently, studies have determined the brain exceeds the normal limits. Its manifestation can vary whether antiepileptic drug (AED) treatment is required for from uncontrolled jerking movement (tonic–clonic seizure) to epileptic seizures in children with hypoparathyroidism. momentary loss of awareness (absence seizure). These im- Method This study aims to evaluate the data of two medical pulses spread to adjacent areas in the brain and create an un- centers in Beijing based on the diagnosis of epileptic seizures controlled storm of electrical activity. Brain diseases character- as the first symptom of hypoparathyroidism in children. ized by enduring predisposition to generate epileptic seizures Result A total of 42 patients were included and assigned into are collectively called epilepsy. According to pathogenesis, ep- AED and non-AED treatment groups in a 1:2 matched case– ilepsy can be classified into six categories: metabolic, structural, control study. Results show that the seizure outcome after inherited, immunologic, inflammatory, and idiopathic. 1 year of AED treatment is not significantly different from Hypoparathyroidism is an endocrine disease that results that of the control. -

Clinical Physiology Aspects of Chloremia in Fluid Therapy: a Systematic Review David Astapenko1,2* , Pavel Navratil2,3, Jiri Pouska4,5 and Vladimir Cerny1,2,6,7,8,9
Astapenko et al. Perioperative Medicine (2020) 9:40 https://doi.org/10.1186/s13741-020-00171-3 REVIEW Open Access Clinical physiology aspects of chloremia in fluid therapy: a systematic review David Astapenko1,2* , Pavel Navratil2,3, Jiri Pouska4,5 and Vladimir Cerny1,2,6,7,8,9 Abstract Background: This systematic review discusses a clinical physiology aspect of chloride in fluid therapy. Crystalloid solutions are one of the most widely used remedies. While generally used in medicine for almost 190 years, studies focused largely on their safety have only been published since the new millennium. The most widely used solution, normal saline, is most often referred to in this context. Its excessive administration results in hyperchloremic metabolic acidosis with other consequences, including higher mortality rates. Methods: Original papers and review articles eligible for developing the present paper were identified by searching online in the electronic MEDLINE database. The keywords searched for included hyperchloremia, hypochloremia, and compound words containing the word “chloride,” infusion therapy, metabolic acidosis, renal failure, and review. Results: A total of 21,758 papers published before 31 May 2020 were identified; of this number, 630 duplicates were removed from the list. Upon excluding articles based on their title or abstract, 1850 papers were screened, of which 63 full-text articles were assessed. Conclusions: According to the latest medical concepts, dyschloremia (both hyperchloremia and hypochloremia) represents a factor indisputably having a negative effect on selected variables of clinical outcome. As infusion therapy can significantly impact chloride homeostasis of the body, the choice of infusion solutions should always take into account the potentially adverse impact of chloride content on chloremia and organ function. -
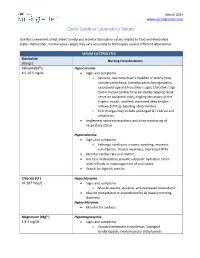
Quick Guide to Laboratory Values
March 2021 www.nursingcenter.com Quick Guide to Laboratory Values Use this convenient cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal value ranges may vary according to techniques used in different laboratories. SERUM ELECTROLYTES Electrolyte Nursing Considerations (Range) Calcium (Ca2+) Hypocalcemia 8.5-10.5 mg/dL • Signs and symptoms o Seizures, neuromuscular irritability or tetany (may include paresthesia, bronchospasm, laryngospasm, carpopedal spasm [Trousseau’s sign], Chvostek’s sign [facial muscle contractions elicited by tapping facial nerve on ipsilateral side], tingling sensations of the fingers, mouth, and feet, increased deep tendon reflexes [DTRs]), bleeding abnormalities o ECG changes may include prolonged QT interval and arrythmias. • Implement seizure precautions and close monitoring of respiratory status. Hypercalcemia • Signs and symptoms o Lethargy, confusion, nausea, vomiting, anorexia, constipation, muscle weakness, depressed DTRs • Monitor cardiac rate and rhythm. • Increase mobilization, provide adequate hydration either with IV fluids or encouragement of oral intake. • Watch for digitalis toxicity. Chloride (Cl-) Hypochloremia 97-107 mEq/L • Signs and symptoms o Muscle spasms, alkalosis, and depressed respirations • May be precipitated or exacerbated by GI losses (vomiting, diarrhea). Hyperchloremia • Monitor for acidosis. Magnesium (Mg2+) Hypomagnesemia 1.8-3 mg/dL • Signs and symptoms o Cardiac/ventricular arrhythmias, laryngeal stridor/spasm, neuromuscular -

Hyponatremia in Hepatic Cirrhosis Following Paracentesis
HYPONATREMIA IN HEPATIC CIRRHOSIS FOLLOWING PARACENTESIS William P. Nelson III, … , Jack D. Rosenbaum, Maurice B. Strauss J Clin Invest. 1951;30(7):738-744. https://doi.org/10.1172/JCI102487. Research Article Find the latest version: https://jci.me/102487/pdf HYPONATREMIA IN HEPATIC CIRRHOSIS FOLLOWING PARACENTESIS 1 By WILLIAM P. NELSON, III, JACK D. ROSENBAUM, AND MAURICE B. STRAUSS (From the Medical Service, Cushing Veterans Administration Hospital, Framingham, Mass.) (Submitted for publication January 15, 1951; accepted April 23, 1951) The retention of water without a physiologically modification of the Folin procedure (14); non-protein equivalent amount of sodium following abdominal nitrogen by micro-Kjeldahl with Nesslerization (15); and sodium and potassium by means of the Barclay internal paracentesis has been studied in two patients with standard flame photometer. Except where otherwise advanced cirrhosis of the liver. In each there de- noted, urine was collected over 24 hour periods and was veloped manifestations considered characteristic analyzed for chloride by the Volhard-Harvey method of sodium deficit, although there was no change in (16), for total nitrogen by the micro-Kjeldahl procedure the total body sodium at the time these appeared. (11), and for creatinine, sodium, and potassium by the methods employed for serum. Change in total body water Such retention of water in excess of salt, regularly (liters) was taken to equal change in weight (kilograms). observed when large external losses of salt and water are replaced with water alone (1-3), has CASE REPORTS AND RESULTS been noted in certain cases of heart failure and chronic renal disease (4-6) as well as in decom- Case I. -

Fluid & Electrolytes Fluid Balance Sodium 135-145 Meq/L
11/24/2009 Fluid & Electrolytes The Basics Fluid Balance Sodium 135‐145 meq/L • Imbalances typically associated with parallel changes in osmolality • Plays a major role in – ECF volume and concenttitration – Generation and transmission of nerve impulses – Acid–base balance 1 11/24/2009 Hypernatremia • Elevated serum sodium occurring with water loss or sodium gain • Causes hyperosmolality leading to cellular dehydration • Primary protection is thirst from hypothalamus Differential Assessment of ECF Volume Hypernatremia • Manifestations – Thirst, lethargy, agitation, seizures, and coma • Impaired LOC • Produced by clinical states – Central or nephrogenic diabetes insipidus – Serum sodium levels must be reduced gradually to avoid cerebral edema 2 11/24/2009 Nursing Management Nursing Diagnoses • Potential complication: seizures and coma leading to irreversible brain damage • Management • Treat undliderlying cause • If oral fluids cannot be ingested, IV solution of 5% dextrose in water or hypotonic saline • Diuretics Hyponatremia • Results from loss of sodium‐containing fluids or from water excess • Manifestations – CfiConfusion, nausea, vomiting, seizures, and coma Nursing Management Nursing Diagnoses • Risk for injury • Potential complication: severe neurologic changes • Management • Abnormal fluid loss – Fluid replacement with sodium‐containing solution • Caused by water excess – Fluid restriction is needed • Severe symptoms (seizures) – Give small amount of IV hypertonic saline solution (3% NaCl) 3 11/24/2009 Potassium 3.5‐5.5 meq/L • -

The Prognostic Effects of Hyponatremia and Hyperchloremia on Postoperative NSCLC Patients
Current Problems in Cancer 43 (2019) 402–410 Contents lists available at ScienceDirect Current Problems in Cancer journal homepage: www.elsevier.com/locate/cpcancer The prognostic effects of hyponatremia and hyperchloremia on postoperative NSCLC patients Wei Li a,b,1, Xiaowei Chen a,1, Liguang Wang a,c, Yu Wang a, ∗ Cuicui Huang a, Guanghui Wang a,d, Jiajun Du a,d, a Institute of Oncology, Shandong Provincial Hospital Affiliated to Shandong University, Jinan, PR China b Department of Thoracic Surgery, Shandong Juxian People’s Hospital, Rizhao, PR China c Department of Oncology, Shandong Provincial Hospital Affiliated to Shandong University, Jinan, PR China d Department of Thoracic Surgery, Shandong Provincial Hospital Affiliated to Shandong University, Jinan, PR China a b s t r a c t Electrolytic disorders are common in lung cancer patients. But the association between serum electrolytes levels and survival in patients undergoing lung cancer resections for non–small-cell lung cancer (NSCLC) has been poorly inves- tigated. A retrospective study was conducted on consecutive postoperative NSCLC patients. Pearson’s test was used to determine the association between serum sodium and chlorine levels and clinical characteristics, and cox regression and Kaplan-Meier model were applied to analyze risk factors on overall survival. We found that hyponatremia was an independent prognostic factor associated with poor prognosis in NSCLC patients undergoing complete resection (log-rank test, P = 0.004). In addition, we found that hyperchloremia predicted a poor clinical outcome in patients with non-anion-gap (log-rank test, P = 0.011), whereas it predicted a favorable clinical outcome in patients with high- anion-gap (log-rank test, P = 0.002). -

Calcium and Phosphorous Metabolism
CALCIUM AND PHOSPHOROUS METABOLISM -DR. SUHASINI. G P Lecturer Dept. of Oral Pathology & Microbiology Dr. Suhasini GP, Subharti Dental College, SVSU INTRODUCTION • Metabolism (Greek, Metabote= change) • Sum of the chemical and physical changes in tissue consisting of anabolism (reactions that convert small molecules into large) & catabolism (reactions that convert large molecules into small) Dr. Suhasini GP, Subharti Dental College, SVSU Functions of Calcium • Most abundant mineral • Most important inorganic cation in mineralised tissue- structural role • [Ca10(PO4)6(OH)2] in bone, dentin, cementum & enamel Dr. Suhasini GP, Subharti Dental College, SVSU Functions Formation of bone and teeth Controls secretion of glandular cells Muscle contraction Clotting of blood Neuromuscular excitability Cell-cell adhesion, cell integrity Intracellular second messenger in harmonal actions Dr. Suhasini GP, Subharti Dental College, SVSU Dietary requirements • Adults- 0.8 gms/day • Children & pregnant and lactating women- additional 1gm of Ca supplements/day • Postmenopausal women Dr. Suhasini GP, Subharti Dental College, SVSU Sources • Milk & its products • Green leafy veg (oxalic acid and phytic acid- reduces absorption) • Raagi • Egg yolk • Legumes • Nuts • Dried fish • Pan chewing with slacked lime • Drinking water Dr. Suhasini GP, Subharti Dental College, SVSU Distribution of Ca++` • Essentially distributed extracellularly • 1.2-1.4 kg in 70kg adult • 99%-skeleton • 1%- soft tissue+ body fluids Dr. Suhasini GP, Subharti Dental College, SVSU Bone Ca++ Exists in 2 forms- • Readily exchangeable form- simple exchange b/n newly deposited bone & exctracellular Ca++ • Stable form- constant formation & resorption of bone- – Controlled by PTH, calcitonin & vit.D Dr. Suhasini GP, Subharti Dental College, SVSU Blood Ca++ • Plasma, little in RBC • 9-11mg/dl- constant • In plasma- 1. -

Calcinosis Cutis,Calcinosis Circumscripta,And “Mille Feuille
Calcinosis Cutis, Calcinosis Circumscripta, and “Mille Feuille” Lesions James Yi-Chien Lin, DVM MS; Han-Ju Tsai, DVM MS; Kau-Shen Hsu, DVM; Fun-In Wang, DVM PhD Skin and subcutaneous lesions of 2 cases with natural occurring Cushing’s disease and 1 case with calcinosis circumscripta were compared. Case 1 was typical of osteoma cutis, containing somewhat regularly arranged discrete ossification foci in the mid and deep dermis. Case 2 had layers of “mille feuille”, yellowish to white gritty chalky substances diffusely scattered in the sub- cutis, seen histologically as disseminatedly scattered light purple crystalloid and blue granular mineral salts. Lesions stained orange red with Alizarin Red S indicated the presence of calcium ions. Discrete ossification foci in the deep dermis and early multifocal collagenolysis with mine- ralization were also noted. Case 3 was typical of calcinosis circumscripta, seen grossly as yel- lowish chalky substance in both dermis and subcutis, and histologically as lakes of well- circumscribed light purple crystals and granular deep blue mineral salts. Case 2 had features of calcinosis cutis such as ossification foci and early multifocal collagenolysis. Case 2 also had “mille feuille” that was histologically similar to those mineral salts in case 3, but was not circum- scribed, and was not exactly calcinosis universalis. The component in case 1 was most likely hydroxyapatite Ca10(PO4)6(OH)2; the “mille feuille” of case 2 was most likely “calcium soap” after panniculitis and fat necrosis; and that in case 3 was most likely calcium phosphate CaPO4. Lo- cal factors, such as fluid exudation reflecting how well the inflammation was controlled clinically, may influence the wound healing, and thus the outcome of lesions. -

Sex Differences in Electrolyte Imbalances Caused by SARS-Cov-2
Sex differences in electrolyte imbalances caused by SARS-CoV-2: a case-control study Arianna Pani1, Elvira Inglese2, Massimo Puoti2, Valeria Cento1, Claudia Alteri1, Alessandra Romandini1, Federica Di Ruscio2, Michele Senatore1, Mauro Moreno2, Paolo Tarsia2, Fabrizio Colombo2, Oscar Epis2, Valentina Panetta3, Chiara Vismara2, Andrea Bellone2, and Francesco Scaglione1 1Universit`adegli Studi di Milano 2Niguarda Hospital 3L’altrastatistica srl - Consultancy & Training March 27, 2021 Abstract Background - Since SARS-CoV-2 spread, evidences regarding sex differences in progression and prognosis of COVID-19 have emerged. Besides this, studies on patients’ clinical characteristics have described electrolyte imbalances as one of the recurrent features of COVID-19. Methods - We performed a case-control study on all patients admitted to the emergency department (ED) from 1st March to 31st May 2020 who had undergone a blood gas analysis and a nasopharyngeal swab test for SARS- CoV-2 by rtPCR. We defined positive patients as cases and negatives as controls. The study was approved by the local ethics committee Area 3 Milan. Data were automatically extracted from the hospital laboratory SQL-based repository in anonymized form. We considered as outcomes potassium (K+), sodium (Na+), chlorine (Cl-) and calcium (Ca++) as continuous and as categorical variables, in their relation with age, sex and SARS-CoV-2 infection status. Results - We observed a higher prevalence of hypokalemia among patients positive for SARS-CoV-2 (13.7% vs 6% of negative subjects). Positive patients had a higher probability to be admitted to the ED with hypokalemia (OR 2.75, 95% CI 1.8-4.1 p<0.0001) and women were twice as likely to be affected than men (OR 2.43, 95% CI 1.67-3.54 p<0.001). -

NAME:ETINOSA-OGBAHON OSASENAGA PHARMACOLOGY 18/MHS07/019 BCH 204 Question 1
NAME:ETINOSA-OGBAHON OSASENAGA PHARMACOLOGY 18/MHS07/019 BCH 204 Question 1. Outline the toxicity values and deficiency manifestation of the following minerals: ● Potassium ● Calcium ● Magnesium ● Chloride ● Iron ◆POTASSIUM DEFICIENCY MANIFESTATION A. Hyperkalemia Hyperkalemia is a clinical condition associated with elevated plasma potassium above the normal range (3.5–5 mEq/L). Causes of hyperkalemia •Renal failure: The kidney may not be able to excrete a potassium load when GFR is very low. •Mineralocorticoid deficiency: For example, in Addison’s disease. •Cell damage: For example, in trauma and malignancy. Symptoms of hyperkalemia First manifestation is cardiac arrest, changes in electro- cardiogram, cardiac arrhythmia, muscle weakness which may be preceded by parasthesia (abnormal tingling sensation). Treatment for Hyperkalemia Treatment may include: •Going on a low-potassium diet •Stopping or changing meds that are contributing to the hyperkalemia •Taking medicine to lower the potassium in your body. Water pills (diuretics) remove potassium via the urinary tract. •Treating your kidney disease, which may include dialysis, which filters potassium from your blood B.Hypokalemia (low plasma concentration) In hypokalemia, the level of potassium in blood is too low. Causes of hypokalemia •Gastrointestinal losses: Potassium may be lost from the intestine due to vomiting, diarrhea. •Renal losses: Due to renal disease, administration of diuretics. •Drinking too much alcohol •Sweating a lot •Folic acid deficiency •Certain antibiotics •Diabetic ketoacidosis (high levels of acids called ketones in your blood) •Laxatives taken over a long period of time •Certain types of tobacco •Some asthma medications •Low magnesium Several syndromes can be associated with low potassium, such as: •Cushing's syndrome •Gitelman syndrome •Liddle syndrome •Bartter syndrome •Fanconi syndrome Symptoms of hypokalemia Muscular weakness, tachycardia, electrocardiographic (ECG) changes (flattering of ECG waves), lethargy, and confusion. -

Bartter Syndrome Precision Panel Overview Indications Clinical Utility
Bartter Syndrome Precision Panel Overview Bartter Syndrome is an autosomal recessive renal tubular disorder caused by a defective salt reabsorption in the thick ascending loop of Henle resulting in hypokalemia, hypochloremia, metabolic alkalosis, high renin and aldosterone with normal blood pressure. In neonatal cases, it can be suspected before birth and diagnosed soon after birth whereas in classic cases the presentation can begin at 2 years of age or younger. The genetic heterogeneity of this disease comes from genetic mutations in either the sodium chloride/potassium chloride cotransporter or the potassium channel transporter in the thick ascending loop of Henle. The Igenomix Bartter Syndrome Precision Panel can be used to make a directed and accurate diagnosis ultimately leading to a better management and prognosis of the disease. It provides a comprehensive analysis of the genes involved in this disease using next-generation sequencing (NGS) to fully understand the spectrum of relevant genes involved. Indications The Igenomix Bartter Syndrome Precision Panel is indicated for those patients with a clinical suspicion or diagnosis of Bartter Syndrome presenting with: - Family history of Bartter Syndrome - Maternal polyhydramnios - Fetal fluid loss and volume depletion - Failure to thrive - Polyuria - Polydipsia - Vomiting - Constipation - Salt craving Clinical Utility The clinical utility of this panel is: - The genetic and molecular confirmation for an accurate clinical diagnosis of a symptomatic patient. 1 - Early initiation of treatment with a multidisciplinary team in the form of medical care with potassium sparing diuretics, ion supplements and counselling regarding pregnancy- related considerations. - Risk assessment of asymptomatic family members according to the mode of inheritance.