Neurologic Complications of Electrolyte Disturbances and Acid–Base Balance
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Hyponatremia and Hypernatremia MICHAEL M
This is a corrected version of the article that appeared in print. Diagnosis and Management of Sodium Disorders: Hyponatremia and Hypernatremia MICHAEL M. BRAUN, DO, Madigan Army Medical Center, Tacoma, Washington CRAIG H. BARSTOW, MD, Womack Army Medical Center, Fort Bragg, North Carolina NATASHA J. PYZOCHA, DO, Madigan Army Medical Center, Tacoma, Washington Hyponatremia and hypernatremia are common findings in the inpatient and outpatient settings. Sodium disorders are associated with an increased risk of morbidity and mortality. Plasma osmolality plays a critical role in the patho- physiology and treatment of sodium disorders. Hyponatremia and hypernatremia are classified based on volume status (hypovolemia, euvolemia, and hypervolemia). Sodium disorders are diagnosed by findings from the history, physical examination, laboratory studies, and evaluation of volume status. Treatment is based on symptoms and underlying causes. In general, hyponatremia is treated with fluid restriction (in the setting of euvolemia), isotonic saline (in hypovolemia), and diuresis (in hypervolemia). A combination of these therapies may be needed based on the presentation. Hypertonic saline is used to treat severe symptomatic hyponatremia. Medications such as vaptans may have a role in the treatment of euvolemic and hypervolemic hyponatremia. The treatment of hypernatremia involves correcting the underlying cause and correcting the free water deficit. Am( Fam Physician. 2015;91(5):299-307. Copy- right © 2015 American Academy of Family Physicians.) More online yponatremia is a common elec- a worse prognosis in patients with liver cir- at http://www. trolyte disorder defined as a rhosis, pulmonary hypertension, myocardial aafp.org/afp. serum sodium level of less than infarction, chronic kidney disease, hip frac- CME This clinical content 135 mEq per L.1-3 A Dutch sys- tures, and pulmonary embolism.1,8-10 conforms to AAFP criteria Htematic review of 53 studies showed that the for continuing medical Etiology and Pathophysiology education (CME). -

Epileptic Seizure, As the First Symptom of Hypoparathyroidism in Children, Does Not Require Antiepileptic Drugs
Childs Nerv Syst DOI 10.1007/s00381-016-3264-2 ORIGINAL PAPER Epileptic seizure, as the first symptom of hypoparathyroidism in children, does not require antiepileptic drugs Meng-Jia Liu1 & Jiu-Wei Li2 & Xiu-Yu Shi1 & Lin-Yan Hu1 & Li-Ping Zou1,3 Received: 28 May 2016 /Accepted: 3 October 2016 # The Author(s) 2016. This article is published with open access at Springerlink.com Abstract Introduction Objective Patients with hypoparathyroidism exhibit metabol- ic disorders (hypocalcemia) and brain structural abnormalities Epileptic seizure occurs when a burst of electrical impulses in (brain calcifications). Currently, studies have determined the brain exceeds the normal limits. Its manifestation can vary whether antiepileptic drug (AED) treatment is required for from uncontrolled jerking movement (tonic–clonic seizure) to epileptic seizures in children with hypoparathyroidism. momentary loss of awareness (absence seizure). These im- Method This study aims to evaluate the data of two medical pulses spread to adjacent areas in the brain and create an un- centers in Beijing based on the diagnosis of epileptic seizures controlled storm of electrical activity. Brain diseases character- as the first symptom of hypoparathyroidism in children. ized by enduring predisposition to generate epileptic seizures Result A total of 42 patients were included and assigned into are collectively called epilepsy. According to pathogenesis, ep- AED and non-AED treatment groups in a 1:2 matched case– ilepsy can be classified into six categories: metabolic, structural, control study. Results show that the seizure outcome after inherited, immunologic, inflammatory, and idiopathic. 1 year of AED treatment is not significantly different from Hypoparathyroidism is an endocrine disease that results that of the control. -
CURRENT Essentials of Nephrology & Hypertension
a LANGE medical book CURRENT ESSENTIALS: NEPHROLOGY & HYPERTENSION Edited by Edgar V. Lerma, MD Clinical Associate Professor of Medicine Section of Nephrology Department of Internal Medicine University of Illinois at Chicago College of Medicine Associates in Nephrology, SC Chicago, Illinois Jeffrey S. Berns, MD Professor of Medicine and Pediatrics Associate Dean for Graduate Medical Education The Perelman School of Medicine at the University of Pennsylvania Philadelphia, Pennsylvania Allen R. Nissenson, MD Emeritus Professor of Medicine David Geffen School of Medicine at UCLA Los Angeles, California Chief Medical Offi cer DaVita Inc. El Segundo, California New York Chicago San Francisco Lisbon London Madrid Mexico City Milan New Delhi San Juan Seoul Singapore Sydney Toronto Lerma_FM_p00i-xvi.indd i 4/27/12 10:33 AM Copyright © 2012 by The McGraw-Hill Companies, Inc. All rights reserved. Except as permitted under the United States Copyright Act of 1976, no part of this publication may be reproduced or distributed in any form or by any means, or stored in a database or retrieval system, without the prior written permission of the publisher. ISBN: 978-0-07-180858-3 MHID: 0-07-180858-2 The material in this eBook also appears in the print version of this title: ISBN: 978-0-07-144903-8, MHID: 0-07-144903-5. All trademarks are trademarks of their respective owners. Rather than put a trademark symbol after every occurrence of a trademarked name, we use names in an editorial fashion only, and to the benefi t of the trademark owner, with no intention of infringement of the trademark. -

Cerebral Salt Wasting Syndrome and Systemic Lupus Erythematosus: Case Report
Elmer ress Case Report J Med Cases. 2016;7(9):399-402 Cerebral Salt Wasting Syndrome and Systemic Lupus Erythematosus: Case Report Filipe Martinsa, c, Carolina Ouriquea, Jose Faria da Costaa, Joao Nuakb, Vitor Braza, Edite Pereiraa, Antonio Sarmentob, Jorge Almeidaa Abstract disorders, that results in hyponatremia and a decrease in ex- tracellular fluid volume. It is characterized by a hypotonic hy- Cerebral salt wasting (CSW) is a rare cause of hypoosmolar hypona- ponatremia with inappropriately elevated urine sodium con- tremia usually associated with acute intracranial disease character- centration in the setting of a normal kidney function [1-3]. ized by extracellular volume depletion due to inappropriate sodium The onset of this disorder is typically seen within the first wasting in the urine. We report a case of a 46-year-old male with 10 days following a neurological insult and usually lasts no recently diagnosed systemic lupus erythematosus (SLE) initially pre- more than 1 week [1, 2]. Pathophysiology is not completely senting with neurological involvement and an antiphospholipid syn- understood but the major mechanism might be the inappropri- drome (APS) who was admitted because of chronic asymptomatic ate and excessive release of natriuretic peptides which would hyponatremia previously assumed as secondary to syndrome of inap- result in natriuresis and volume depletion. A secondary neu- propriate antidiuretic hormone secretion (SIADH). Initial evaluation rohormonal response would result in an increase in the renin- revealed a hypoosmolar hyponatremia with high urine osmolality angiotensin system and consequently in antidiuretic hormone and elevated urinary sodium concentration. Clinically, the patient’s (ADH) production. Since the volume stimulus is more potent extracellular volume status was difficult to define accurately. -

Electrolyte and Acid-Base
Special Feature American Society of Nephrology Quiz and Questionnaire 2013: Electrolyte and Acid-Base Biff F. Palmer,* Mark A. Perazella,† and Michael J. Choi‡ Abstract The Nephrology Quiz and Questionnaire (NQ&Q) remains an extremely popular session for attendees of the annual meeting of the American Society of Nephrology. As in past years, the conference hall was overflowing with interested audience members. Topics covered by expert discussants included electrolyte and acid-base disorders, *Department of Internal Medicine, glomerular disease, ESRD/dialysis, and transplantation. Complex cases representing each of these categories University of Texas along with single-best-answer questions were prepared by a panel of experts. Prior to the meeting, program Southwestern Medical directors of United States nephrology training programs answered questions through an Internet-based ques- Center, Dallas, Texas; † tionnaire. A new addition to the NQ&Q was participation in the questionnaire by nephrology fellows. To review Department of Internal Medicine, the process, members of the audience test their knowledge and judgment on a series of case-oriented questions Yale University School prepared and discussed by experts. Their answers are compared in real time using audience response devices with of Medicine, New the answers of nephrology fellows and training program directors. The correct and incorrect answers are then Haven, Connecticut; ‡ briefly discussed after the audience responses, and the results of the questionnaire are displayed. This article and Division of recapitulates the session and reproduces its educational value for the readers of CJASN. Enjoy the clinical cases Nephrology, Department of and expert discussions. Medicine, Johns Clin J Am Soc Nephrol 9: 1132–1137, 2014. -
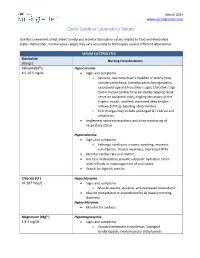
Quick Guide to Laboratory Values
March 2021 www.nursingcenter.com Quick Guide to Laboratory Values Use this convenient cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal value ranges may vary according to techniques used in different laboratories. SERUM ELECTROLYTES Electrolyte Nursing Considerations (Range) Calcium (Ca2+) Hypocalcemia 8.5-10.5 mg/dL • Signs and symptoms o Seizures, neuromuscular irritability or tetany (may include paresthesia, bronchospasm, laryngospasm, carpopedal spasm [Trousseau’s sign], Chvostek’s sign [facial muscle contractions elicited by tapping facial nerve on ipsilateral side], tingling sensations of the fingers, mouth, and feet, increased deep tendon reflexes [DTRs]), bleeding abnormalities o ECG changes may include prolonged QT interval and arrythmias. • Implement seizure precautions and close monitoring of respiratory status. Hypercalcemia • Signs and symptoms o Lethargy, confusion, nausea, vomiting, anorexia, constipation, muscle weakness, depressed DTRs • Monitor cardiac rate and rhythm. • Increase mobilization, provide adequate hydration either with IV fluids or encouragement of oral intake. • Watch for digitalis toxicity. Chloride (Cl-) Hypochloremia 97-107 mEq/L • Signs and symptoms o Muscle spasms, alkalosis, and depressed respirations • May be precipitated or exacerbated by GI losses (vomiting, diarrhea). Hyperchloremia • Monitor for acidosis. Magnesium (Mg2+) Hypomagnesemia 1.8-3 mg/dL • Signs and symptoms o Cardiac/ventricular arrhythmias, laryngeal stridor/spasm, neuromuscular -

Fluid & Electrolytes Fluid Balance Sodium 135-145 Meq/L
11/24/2009 Fluid & Electrolytes The Basics Fluid Balance Sodium 135‐145 meq/L • Imbalances typically associated with parallel changes in osmolality • Plays a major role in – ECF volume and concenttitration – Generation and transmission of nerve impulses – Acid–base balance 1 11/24/2009 Hypernatremia • Elevated serum sodium occurring with water loss or sodium gain • Causes hyperosmolality leading to cellular dehydration • Primary protection is thirst from hypothalamus Differential Assessment of ECF Volume Hypernatremia • Manifestations – Thirst, lethargy, agitation, seizures, and coma • Impaired LOC • Produced by clinical states – Central or nephrogenic diabetes insipidus – Serum sodium levels must be reduced gradually to avoid cerebral edema 2 11/24/2009 Nursing Management Nursing Diagnoses • Potential complication: seizures and coma leading to irreversible brain damage • Management • Treat undliderlying cause • If oral fluids cannot be ingested, IV solution of 5% dextrose in water or hypotonic saline • Diuretics Hyponatremia • Results from loss of sodium‐containing fluids or from water excess • Manifestations – CfiConfusion, nausea, vomiting, seizures, and coma Nursing Management Nursing Diagnoses • Risk for injury • Potential complication: severe neurologic changes • Management • Abnormal fluid loss – Fluid replacement with sodium‐containing solution • Caused by water excess – Fluid restriction is needed • Severe symptoms (seizures) – Give small amount of IV hypertonic saline solution (3% NaCl) 3 11/24/2009 Potassium 3.5‐5.5 meq/L • -

Hyperchloremia – Why and How
Document downloaded from http://www.elsevier.es, day 23/05/2017. This copy is for personal use. Any transmission of this document by any media or format is strictly prohibited. n e f r o l o g i a 2 0 1 6;3 6(4):347–353 Revista de la Sociedad Española de Nefrología www.revistanefrologia.com Brief review Hyperchloremia – Why and how Glenn T. Nagami Nephrology Section, Department of Medicine, VA Greater Los Angeles Healthcare System and David Geffen School of Medicine at UCLA, United States a r t i c l e i n f o a b s t r a c t Article history: Hyperchloremia is a common electrolyte disorder that is associated with a diverse group of Received 5 April 2016 clinical conditions. The kidney plays an important role in the regulation of chloride concen- Accepted 11 April 2016 tration through a variety of transporters that are present along the nephron. Nevertheless, Available online 3 June 2016 hyperchloremia can occur when water losses exceed sodium and chloride losses, when the capacity to handle excessive chloride is overwhelmed, or when the serum bicarbonate is low Keywords: with a concomitant rise in chloride as occurs with a normal anion gap metabolic acidosis Hyperchloremia or respiratory alkalosis. The varied nature of the underlying causes of the hyperchloremia Electrolyte disorder will, to a large extent, determine how to treat this electrolyte disturbance. Serum bicarbonate Published by Elsevier Espana,˜ S.L.U. on behalf of Sociedad Espanola˜ de Nefrologıa.´ This is an open access article under the CC BY-NC-ND license (http://creativecommons.org/ licenses/by-nc-nd/4.0/). -

An Infant with Chronic Hypernatremia
European Journal of Endocrinology (2006) 155 S141–S144 ISSN 0804-4643 An infant with chronic hypernatremia M L Marcovecchio Department of Paediatrics, University of Chieti, Via dei Vestini 5, 66100 Chieti, Italy (Correspondence should be addressed to M L Marcovecchio; Email: [email protected]) Abstract A 4-month-old boy was presented with failure to thrive, refusal to feed, delayed motor development, truncal hypotonia, and head lag. His plasma osmolality and sodium were significantly high, while his urine osmolality was inappropriately low and did not increase after desmopressin administration. Despite his hyperosmolality, he presented with a lack of thirst and became clearly polyuric and polydipsic only at the age of 2 years. Initial treatment with indomethacin was ineffective, while the combination of hydrochlorothiazide and amiloride was effective and well tolerated. European Journal of Endocrinology 155 S141–S144 Introduction (61 ml/kg) respectively. Other investigations including thyroid and adrenal function were normal. He was Chronic hypernatremia in young patients is generally refusing oral fluids despite being hypernatremic. the result of alterations in the mechanisms controlling A cranial magnetic resonance imaging scan excluded fluid balance (1). Excessive water loss, as in diabetes structural abnormalities in the hypophysis, hypo- insipidus, or an inadequate fluid intake, as in adipsic thalamus and surrounding area. There was no response hypernatremia, may be the underlying cause. The to 0.3 mg 1-desamino-8-D-arginine-vasopressin (DDAVP) differential diagnosis between these conditions is given intravenously (osmolality pre- 374 mosmol/kg; important in order to choose the appropriate treatment. post- 371 mosmol/kg). This suggested a tubular defect However, pitfalls in the diagnosis are often related to an causing nephrogenic diabetes insipidus (NDI). -

Electrolyte and Acid-Base Disorders Triggered by Aminoglycoside Or Colistin Therapy: a Systematic Review
antibiotics Review Electrolyte and Acid-Base Disorders Triggered by Aminoglycoside or Colistin Therapy: A Systematic Review Martin Scoglio 1,* , Gabriel Bronz 1, Pietro O. Rinoldi 1,2, Pietro B. Faré 3,Céline Betti 1,2, Mario G. Bianchetti 1, Giacomo D. Simonetti 1,2, Viola Gennaro 1, Samuele Renzi 4, Sebastiano A. G. Lava 5 and Gregorio P. Milani 2,6,7 1 Faculty of Biomedicine, Università della Svizzera Italiana, 6900 Lugano, Switzerland; [email protected] (G.B.); [email protected] (P.O.R.); [email protected] (C.B.); [email protected] (M.G.B.); [email protected] (G.D.S.); [email protected] (V.G.) 2 Department of Pediatrics, Pediatric Institute of Southern Switzerland, Ospedale San Giovanni, Ente Ospedaliero Cantonale, 6500 Bellinzona, Switzerland; [email protected] 3 Department of Internal Medicine, Ospedale La Carità, Ente Ospedaliero Cantonale, 6600 Locarno, Switzerland; [email protected] 4 Division of Hematology and Oncology, The Hospital for Sick Children, Toronto, ON M5G 1X8, Canada; [email protected] 5 Pediatric Cardiology Unit, Department of Pediatrics, Centre Hospitalier Universitaire Vaudois, and University of Lausanne, 1011 Lausanne, Switzerland; [email protected] 6 Pediatric Unit, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, 20122 Milan, Italy 7 Department of Clinical Sciences and Community Health, Università degli Studi di Milano, 20122 Milan, Italy * Correspondence: [email protected] Citation: Scoglio, M.; Bronz, G.; Abstract: Aminoglycoside or colistin therapy may alter the renal tubular function without decreasing Rinoldi, P.O.; Faré, P.B.; Betti, C.; the glomerular filtration rate. This association has never been extensively investigated. -

Is There a Relationship Between COVID-19 and Hyponatremia?
medicina Review Is There a Relationship between COVID-19 and Hyponatremia? Gina Gheorghe 1,2,†, Madalina Ilie 1,2, Simona Bungau 3,† , Anca Mihaela Pantea Stoian 4 , Nicolae Bacalbasa 5 and Camelia Cristina Diaconu 6,7,* 1 Department of Gastroenterology, “Carol Davila” University of Medicine and Pharmacy, 050474 Bucharest, Romania; [email protected] (G.G.); [email protected] (M.I.) 2 Department of Gastroenterology, Clinical Emergency Hospital of Bucharest, 105402 Bucharest, Romania 3 Department of Pharmacy, Faculty of Medicine and Pharmacy, University of Oradea, 410028 Oradea, Romania; [email protected] 4 Department of Diabetes, Nutrition and Metabolic Diseases, “Carol Davila” University of Medicine and Pharmacy, 020475 Bucharest, Romania; [email protected] 5 Department of Visceral Surgery, Center of Excellence in Translational Medicine, Fundeni Clinical Institute, 022328 Bucharest, Romania; [email protected] 6 Department of Internal Medicine, “Carol Davila” University of Medicine and Pharmacy, 050474 Bucharest, Romania 7 Department of Internal Medicine, Clinical Emergency Hospital of Bucharest, 105402 Bucharest, Romania * Correspondence: [email protected]; Tel.: +40-0726-377-300 † This author has equal contribution to the paper as the first author. Abstract: Nowadays, humanity faces one of the most serious health crises, the severe acute respi- ratory syndrome coronavirus 2 (SARS-CoV-2) pandemic. The severity of coronavirus disease 2019 (COVID-19) pandemic is related to the high rate of interhuman transmission of the virus, variability of clinical presentation, and the absence of specific therapeutic methods. COVID-19 can manifest with non-specific symptoms and signs, especially among the elderly. In some cases, the clinical manifestations of hyponatremia may be the first to appear. -

Parenteral Nutrition Primer: Balance Acid-Base, Fluid and Electrolytes
Parenteral Nutrition Primer: Balancing Acid-Base, Fluids and Electrolytes Phil Ayers, PharmD, BCNSP, FASHP Todd W. Canada, PharmD, BCNSP, FASHP, FTSHP Michael Kraft, PharmD, BCNSP Gordon S. Sacks, Pharm.D., BCNSP, FCCP Disclosure . The program chair and presenters for this continuing education activity have reported no relevant financial relationships, except: . Phil Ayers - ASPEN: Board Member/Advisory Panel; B Braun: Consultant; Baxter: Consultant; Fresenius Kabi: Consultant; Janssen: Consultant; Mallinckrodt: Consultant . Todd Canada - Fresenius Kabi: Board Member/Advisory Panel, Consultant, Speaker's Bureau • Michael Kraft - Rockwell Medical: Consultant; Fresenius Kabi: Advisory Board; B. Braun: Advisory Board; Takeda Pharmaceuticals: Speaker’s Bureau (spouse) . Gordon Sacks - Grant Support: Fresenius Kabi Sodium Disorders and Fluid Balance Gordon S. Sacks, Pharm.D., BCNSP Professor and Department Head Department of Pharmacy Practice Harrison School of Pharmacy Auburn University Learning Objectives Upon completion of this session, the learner will be able to: 1. Differentiate between hypovolemic, euvolemic, and hypervolemic hyponatremia 2. Recommend appropriate changes in nutrition support formulations when hyponatremia occurs 3. Identify drug-induced causes of hypo- and hypernatremia No sodium for you! Presentation Outline . Overview of sodium and water . Dehydration vs. Volume Depletion . Water requirements & Equations . Hyponatremia • Hypotonic o Hypovolemic o Euvolemic o Hypervolemic . Hypernatremia • Hypovolemic • Euvolemic • Hypervolemic Sodium and Fluid Balance . Helpful hint: total body sodium determines volume status, not sodium status . Examples of this concept • Hypervolemic – too much volume • Hypovolemic – too little volume • Euvolemic – normal volume Water Distribution . Total body water content varies from 50-70% of body weight • Dependent on lean body mass: fat ratio o Fat water content is ~10% compared to ~75% for muscle mass .