Lipid Mediators Regulate Pulmonary Fibrosis: Potential Mechanisms and Signaling Pathways
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Retinamide Increases Dihydroceramide and Synergizes with Dimethylsphingosine to Enhance Cancer Cell Killing
2967 N-(4-Hydroxyphenyl)retinamide increases dihydroceramide and synergizes with dimethylsphingosine to enhance cancer cell killing Hongtao Wang,1 Barry J. Maurer,1 Yong-Yu Liu,2 elevations in dihydroceramides (N-acylsphinganines), Elaine Wang,3 Jeremy C. Allegood,3 Samuel Kelly,3 but not desaturated ceramides, and large increases in Holly Symolon,3 Ying Liu,3 Alfred H. Merrill, Jr.,3 complex dihydrosphingolipids (dihydrosphingomyelins, Vale´rie Gouaze´-Andersson,4 Jing Yuan Yu,4 monohexosyldihydroceramides), sphinganine, and sphin- Armando E. Giuliano,4 and Myles C. Cabot4 ganine 1-phosphate. To test the hypothesis that elevation of sphinganine participates in the cytotoxicity of 4-HPR, 1Childrens Hospital Los Angeles, Keck School of Medicine, cells were treated with the sphingosine kinase inhibitor University of Southern California, Los Angeles, California; D-erythro-N,N-dimethylsphingosine (DMS), with and 2 College of Pharmacy, University of Louisiana at Monroe, without 4-HPR. After 24 h, the 4-HPR/DMS combination Monroe, Louisiana; 3School of Biology and Petit Institute of Bioengineering and Bioscience, Georgia Institute of Technology, caused a 9-fold increase in sphinganine that was sustained Atlanta, Georgia; and 4Gonda (Goldschmied) Research through +48 hours, decreased sphinganine 1-phosphate, Laboratories at the John Wayne Cancer Institute, and increased cytotoxicity. Increased dihydrosphingolipids Saint John’s Health Center, Santa Monica, California and sphinganine were also found in HL-60 leukemia cells and HT-29 colon cancer cells treated with 4-HPR. The Abstract 4-HPR/DMS combination elicited increased apoptosis in all three cell lines. We propose that a mechanism of N Fenretinide [ -(4-hydroxyphenyl)retinamide (4-HPR)] is 4-HPR–induced cytotoxicity involves increases in dihy- cytotoxic in many cancer cell types. -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

A Benchmarking Study on Virtual Ligand Screening Against Homology Models of Human Gpcrs
bioRxiv preprint doi: https://doi.org/10.1101/284075; this version posted March 19, 2018. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. A benchmarking study on virtual ligand screening against homology models of human GPCRs Victor Jun Yu Lima,b, Weina Dua, Yu Zong Chenc, Hao Fana,d aBioinformatics Institute (BII), Agency for Science, Technology and Research (A*STAR), 30 Biopolis Street, Matrix No. 07-01, 138671, Singapore; bSaw Swee Hock School of Public Health, National University of Singapore, 12 Science Drive 2, 117549, Singapore; cDepartment of Pharmacy, National University of Singapore, 18 Science Drive 4, 117543, Singapore; dDepartment of Biological Sciences, National University of Singapore, 16 Science Drive 4, Singapore 117558 To whom correspondence should be addressed: Dr. Hao Fan, Bioinformatics Institute (BII), Agency for Science, Technology and Research (A*STAR), 30 Biopolis Street, Matrix No. 07-01, 138671, Singapore; Telephone: +65 64788500; Email: [email protected] Keywords: G-protein-coupled receptor, GPCR, X-ray crystallography, virtual screening, homology modelling, consensus enrichment 1 bioRxiv preprint doi: https://doi.org/10.1101/284075; this version posted March 19, 2018. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Abstract G-protein-coupled receptor (GPCR) is an important target class of proteins for drug discovery, with over 27% of FDA-approved drugs targeting GPCRs. However, being a membrane protein, it is difficult to obtain the 3D crystal structures of GPCRs for virtual screening of ligands by molecular docking. -
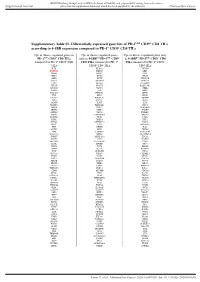
Supplementary Table S5. Differentially Expressed Gene Lists of PD-1High CD39+ CD8 Tils According to 4-1BB Expression Compared to PD-1+ CD39- CD8 Tils
BMJ Publishing Group Limited (BMJ) disclaims all liability and responsibility arising from any reliance Supplemental material placed on this supplemental material which has been supplied by the author(s) J Immunother Cancer Supplementary Table S5. Differentially expressed gene lists of PD-1high CD39+ CD8 TILs according to 4-1BB expression compared to PD-1+ CD39- CD8 TILs Up- or down- regulated genes in Up- or down- regulated genes Up- or down- regulated genes only PD-1high CD39+ CD8 TILs only in 4-1BBneg PD-1high CD39+ in 4-1BBpos PD-1high CD39+ CD8 compared to PD-1+ CD39- CD8 CD8 TILs compared to PD-1+ TILs compared to PD-1+ CD39- TILs CD39- CD8 TILs CD8 TILs IL7R KLRG1 TNFSF4 ENTPD1 DHRS3 LEF1 ITGA5 MKI67 PZP KLF3 RYR2 SIK1B ANK3 LYST PPP1R3B ETV1 ADAM28 H2AC13 CCR7 GFOD1 RASGRP2 ITGAX MAST4 RAD51AP1 MYO1E CLCF1 NEBL S1PR5 VCL MPP7 MS4A6A PHLDB1 GFPT2 TNF RPL3 SPRY4 VCAM1 B4GALT5 TIPARP TNS3 PDCD1 POLQ AKAP5 IL6ST LY9 PLXND1 PLEKHA1 NEU1 DGKH SPRY2 PLEKHG3 IKZF4 MTX3 PARK7 ATP8B4 SYT11 PTGER4 SORL1 RAB11FIP5 BRCA1 MAP4K3 NCR1 CCR4 S1PR1 PDE8A IFIT2 EPHA4 ARHGEF12 PAICS PELI2 LAT2 GPRASP1 TTN RPLP0 IL4I1 AUTS2 RPS3 CDCA3 NHS LONRF2 CDC42EP3 SLCO3A1 RRM2 ADAMTSL4 INPP5F ARHGAP31 ESCO2 ADRB2 CSF1 WDHD1 GOLIM4 CDK5RAP1 CD69 GLUL HJURP SHC4 GNLY TTC9 HELLS DPP4 IL23A PITPNC1 TOX ARHGEF9 EXO1 SLC4A4 CKAP4 CARMIL3 NHSL2 DZIP3 GINS1 FUT8 UBASH3B CDCA5 PDE7B SOGA1 CDC45 NR3C2 TRIB1 KIF14 TRAF5 LIMS1 PPP1R2C TNFRSF9 KLRC2 POLA1 CD80 ATP10D CDCA8 SETD7 IER2 PATL2 CCDC141 CD84 HSPA6 CYB561 MPHOSPH9 CLSPN KLRC1 PTMS SCML4 ZBTB10 CCL3 CA5B PIP5K1B WNT9A CCNH GEM IL18RAP GGH SARDH B3GNT7 C13orf46 SBF2 IKZF3 ZMAT1 TCF7 NECTIN1 H3C7 FOS PAG1 HECA SLC4A10 SLC35G2 PER1 P2RY1 NFKBIA WDR76 PLAUR KDM1A H1-5 TSHZ2 FAM102B HMMR GPR132 CCRL2 PARP8 A2M ST8SIA1 NUF2 IL5RA RBPMS UBE2T USP53 EEF1A1 PLAC8 LGR6 TMEM123 NEK2 SNAP47 PTGIS SH2B3 P2RY8 S100PBP PLEKHA7 CLNK CRIM1 MGAT5 YBX3 TP53INP1 DTL CFH FEZ1 MYB FRMD4B TSPAN5 STIL ITGA2 GOLGA6L10 MYBL2 AHI1 CAND2 GZMB RBPJ PELI1 HSPA1B KCNK5 GOLGA6L9 TICRR TPRG1 UBE2C AURKA Leem G, et al. -

Neurological S1P Signaling As an Emerging Mechanism of Action of Oral FTY720 (Fingolimod) in Multiple Sclerosis
Arch Pharm Res Vol 33, No 10, 1567-1574, 2010 DOI 10.1007/s12272-010-1008-5 REVIEW Neurological S1P Signaling as an Emerging Mechanism of Action of Oral FTY720 (Fingolimod) in Multiple Sclerosis Chang Wook Lee1, Ji Woong Choi2, and Jerold Chun1 1Department of Molecular Biology, Dorris Neuroscience Center, The Scripps Research Institute, La Jolla, California 92037, USA and 2Department of Pharmacology, Division of Basic Medicine and Science, Gachon University of Medi- cine and Science, Incheon 406-799, Korea (Received August 15, 2010/Revised August 23, 2010/Accepted August 24, 2010) FTY720 (fingolimod, Novartis) is a promising investigational drug for relapsing forms of multi- ple sclerosis (MS), an autoimmune and neurodegenerative disorder of the central nervous sys- tem. It is currently under FDA review in the United States, and could represent the first approved oral treatment for MS. Extensive, ongoing clinical trials in Phase II/III have sup- ported both the efficacy and safety of FTY720. FTY720 itself is not bioactive, but when phospho- rylated (FTY720-P) by sphingosine kinase 2, it becomes active through modulation of 4 of the 5 known G protein-coupled sphingosine 1-phosphate (S1P) receptors. The mechanism of action (MOA) is thought to be immunological, where FTY720 alters lymphocyte trafficking via S1P1. However, MOA for FTY720 in MS may also involve a direct, neurological action within the cen- tral nervous system in view of documented S1P receptor-mediated signaling influences in the brain, and this review considers observations that support an emerging neurological MOA. Key words: FTY720, Fingolimod, Sphingosine 1-phosphate receptors, Multiple sclerosis, Cen- tral nervous system INTRODUCTION factors that initiate MS are still unknown. -

Cancer Stem Cells—Key Players in Tumor Relapse
cancers Review Cancer Stem Cells—Key Players in Tumor Relapse Monica Marzagalli *, Fabrizio Fontana, Michela Raimondi and Patrizia Limonta Department of Pharmacological and Biomolecular Sciences, University of Milan, via Balzaretti 9, 20133 Milano, Italy; [email protected] (F.F.); [email protected] (M.R.); [email protected] (P.L.) * Correspondence: [email protected]; Tel.: +39-02-503-18427 Simple Summary: Cancer is one of the hardest pathologies to fight, being one of the main causes of death worldwide despite the constant development of novel therapeutic strategies. Therapeutic failure, followed by tumor relapse, might be explained by the existence of a subpopulation of cancer cells called cancer stem cells (CSCs). The survival advantage of CSCs relies on their ability to shape their phenotype against harmful conditions. This Review will summarize the molecular mechanisms exploited by CSCs in order to escape from different kind of therapies, shedding light on the potential novel CSC-specific targets for the development of innovative therapeutic approaches. Abstract: Tumor relapse and treatment failure are unfortunately common events for cancer patients, thus often rendering cancer an uncurable disease. Cancer stem cells (CSCs) are a subset of cancer cells endowed with tumor-initiating and self-renewal capacity, as well as with high adaptive abilities. Altogether, these features contribute to CSC survival after one or multiple therapeutic approaches, thus leading to treatment failure and tumor progression/relapse. Thus, elucidating the molecular mechanisms associated with stemness-driven resistance is crucial for the development of more effective drugs and durable responses. This review will highlight the mechanisms exploited by CSCs to overcome different therapeutic strategies, from chemo- and radiotherapies to targeted therapies Citation: Marzagalli, M.; Fontana, F.; and immunotherapies, shedding light on their plasticity as an insidious trait responsible for their Raimondi, M.; Limonta, P. -

Unveiling Role of Sphingosine-1-Phosphate Receptor 2 As a Brake of Epithelial Stem Cell Proliferation and a Tumor Suppressor in Colorectal Cancer
Unveiling role of Sphingosine-1-phosphate receptor 2 as a brake of epithelial stem cell proliferation and a tumor suppressor in colorectal cancer Luciana Petti Humanitas Clinical and Research Center-IRCCS Giulia Rizzo Humanitas University Federica Rubbino Humanitas University Sudharshan Elangovan Humanitas University Piergiuseppe Colombo Humanitas Clinical and Research Center-IRRCS Restelli Silvia Humanitas University Andrea Piontini Humanitas University Vincenzo Arena Policlinico Universitario Agostino Gemelli Michele Carvello Humanitas Clinical and Research Center-IRCCS Barbara Romano Universita degli Studi di Napoli Federico II Dipartimento di Medicina Clinica e Chirurgia Tommaso Cavalleri Humanitas Clinical and Research Center-IRCCS Achille Anselmo Humanitas Clinical and Research Center-IRCCS Federica Ungaro Humanitas University Silvia D’Alessio Humanitas University Antonino Spinelli Humanitas University Sanja Stifter Page 1/28 University of Rijeka Fabio Grizzi Humanitas Clinical and Research Center-IRCCS Alessandro Sgambato Istituto di Ricovero e Cura a Carattere Scientico Centro di Riferimento Oncologico della Basilicata Silvio Danese Humanitas University Luigi Laghi Universita degli Studi di Parma Alberto Malesci Humanitas University STEFANIA VETRANO ( [email protected] ) Humanitas University Research Keywords: colorectal cancer, Lgr5, S1PR2, PTEN, epithelial proliferation Posted Date: October 13th, 2020 DOI: https://doi.org/10.21203/rs.3.rs-56319/v2 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Version of Record: A version of this preprint was published on November 23rd, 2020. See the published version at https://doi.org/10.1186/s13046-020-01740-6. Page 2/28 Abstract Background. Sphingosine-1-phosphate receptor 2 (S1PR2) mediates pleiotropic functions encompassing cell proliferation, survival, and migration, which become collectively de-regulated in cancer. -

Fingolimod (FTY720): Discovery and Development of an Oral Drug to Treat Multiple Sclerosis
REVIEWS CASE HISTORY Fingolimod (FTY720): discovery and development of an oral drug to treat multiple sclerosis Volker Brinkmann*, Andreas Billich*, Thomas Baumruker*, Peter Heining‡, Robert Schmouder§, Gordon Francis||, Shreeram Aradhye¶ and Pascale Burtin# Abstract | The discovery of fingolimod (FTY720/Gilenya; Novartis), an orally active immunomodulatory drug, has opened up new approaches to the treatment of multiple sclerosis, the most common inflammatory disorder of the central nervous system. Elucidation of the effects of fingolimod — mediated by the modulation of sphingosine 1‑phosphate (S1P) receptors — has indicated that its therapeutic activity could be due to regulation of the migration of selected lymphocyte subsets into the central nervous system and direct effects on neural cells, particularly astrocytes. An improved understanding of the biology of S1P receptors has also been gained. This article describes the discovery and development of fingolimod, which was approved by the US Food and Drug Administration in September 2010 as a first‑line treatment for relapsing forms of multiple sclerosis, thereby becoming the first oral disease‑modifying therapy to be approved for multiple sclerosis in the United States. Demyelination Multiple sclerosis (MS) is a chronic autoimmune disorder Treatment strategies for MS usually involve the man- Damage of the myelin sheath of the central nervous system (CNS) that is characterized agement of symptoms and the use of disease-modifying of axons. A demyelinating by inflammation leading to astrogliosis, demyelination, drugs to reduce the frequency of relapses and to slow disease is any disease of and loss of oligodendrocytes and neurons1. MS is the the progression of disability. Established first-line the nervous system in which the myelin sheath is damaged. -

Inflammatory Modulation of Hematopoietic Stem Cells by Magnetic Resonance Imaging
Electronic Supplementary Material (ESI) for RSC Advances. This journal is © The Royal Society of Chemistry 2014 Inflammatory modulation of hematopoietic stem cells by Magnetic Resonance Imaging (MRI)-detectable nanoparticles Sezin Aday1,2*, Jose Paiva1,2*, Susana Sousa2, Renata S.M. Gomes3, Susana Pedreiro4, Po-Wah So5, Carolyn Ann Carr6, Lowri Cochlin7, Ana Catarina Gomes2, Artur Paiva4, Lino Ferreira1,2 1CNC-Center for Neurosciences and Cell Biology, University of Coimbra, Coimbra, Portugal, 2Biocant, Biotechnology Innovation Center, Cantanhede, Portugal, 3King’s BHF Centre of Excellence, Cardiovascular Proteomics, King’s College London, London, UK, 4Centro de Histocompatibilidade do Centro, Coimbra, Portugal, 5Department of Neuroimaging, Institute of Psychiatry, King's College London, London, UK, 6Cardiac Metabolism Research Group, Department of Physiology, Anatomy & Genetics, University of Oxford, UK, 7PulseTeq Limited, Chobham, Surrey, UK. *These authors contributed equally to this work. #Correspondence to Lino Ferreira ([email protected]). Experimental Section Preparation and characterization of NP210-PFCE. PLGA (Resomers 502 H; 50:50 lactic acid: glycolic acid) (Boehringer Ingelheim) was covalently conjugated to fluoresceinamine (Sigma- Aldrich) according to a protocol reported elsewhere1. NPs were prepared by dissolving PLGA (100 mg) in a solution of propylene carbonate (5 mL, Sigma). PLGA solution was mixed with perfluoro- 15-crown-5-ether (PFCE) (178 mg) (Fluorochem, UK) dissolved in trifluoroethanol (1 mL, Sigma). This solution was then added to a PVA solution (10 mL, 1% w/v in water) dropwise and stirred for 3 h. The NPs were then transferred to a dialysis membrane and dialysed (MWCO of 50 kDa, Spectrum Labs) against distilled water before freeze-drying. Then, NPs were coated with protamine sulfate (PS). -

G Protein‐Coupled Receptors
S.P.H. Alexander et al. The Concise Guide to PHARMACOLOGY 2019/20: G protein-coupled receptors. British Journal of Pharmacology (2019) 176, S21–S141 THE CONCISE GUIDE TO PHARMACOLOGY 2019/20: G protein-coupled receptors Stephen PH Alexander1 , Arthur Christopoulos2 , Anthony P Davenport3 , Eamonn Kelly4, Alistair Mathie5 , John A Peters6 , Emma L Veale5 ,JaneFArmstrong7 , Elena Faccenda7 ,SimonDHarding7 ,AdamJPawson7 , Joanna L Sharman7 , Christopher Southan7 , Jamie A Davies7 and CGTP Collaborators 1School of Life Sciences, University of Nottingham Medical School, Nottingham, NG7 2UH, UK 2Monash Institute of Pharmaceutical Sciences and Department of Pharmacology, Monash University, Parkville, Victoria 3052, Australia 3Clinical Pharmacology Unit, University of Cambridge, Cambridge, CB2 0QQ, UK 4School of Physiology, Pharmacology and Neuroscience, University of Bristol, Bristol, BS8 1TD, UK 5Medway School of Pharmacy, The Universities of Greenwich and Kent at Medway, Anson Building, Central Avenue, Chatham Maritime, Chatham, Kent, ME4 4TB, UK 6Neuroscience Division, Medical Education Institute, Ninewells Hospital and Medical School, University of Dundee, Dundee, DD1 9SY, UK 7Centre for Discovery Brain Sciences, University of Edinburgh, Edinburgh, EH8 9XD, UK Abstract The Concise Guide to PHARMACOLOGY 2019/20 is the fourth in this series of biennial publications. The Concise Guide provides concise overviews of the key properties of nearly 1800 human drug targets with an emphasis on selective pharmacology (where available), plus links to the open access knowledgebase source of drug targets and their ligands (www.guidetopharmacology.org), which provides more detailed views of target and ligand properties. Although the Concise Guide represents approximately 400 pages, the material presented is substantially reduced compared to information and links presented on the website. -

Targeting the Sphingosine Kinase/Sphingosine-1-Phosphate Signaling Axis in Drug Discovery for Cancer Therapy
cancers Review Targeting the Sphingosine Kinase/Sphingosine-1-Phosphate Signaling Axis in Drug Discovery for Cancer Therapy Preeti Gupta 1, Aaliya Taiyab 1 , Afzal Hussain 2, Mohamed F. Alajmi 2, Asimul Islam 1 and Md. Imtaiyaz Hassan 1,* 1 Centre for Interdisciplinary Research in Basic Sciences, Jamia Millia Islamia, Jamia Nagar, New Delhi 110025, India; [email protected] (P.G.); [email protected] (A.T.); [email protected] (A.I.) 2 Department of Pharmacognosy, College of Pharmacy, King Saud University, Riyadh 11451, Saudi Arabia; afi[email protected] (A.H.); [email protected] (M.F.A.) * Correspondence: [email protected] Simple Summary: Cancer is the prime cause of death globally. The altered stimulation of signaling pathways controlled by human kinases has often been observed in various human malignancies. The over-expression of SphK1 (a lipid kinase) and its metabolite S1P have been observed in various types of cancer and metabolic disorders, making it a potential therapeutic target. Here, we discuss the sphingolipid metabolism along with the critical enzymes involved in the pathway. The review provides comprehensive details of SphK isoforms, including their functional role, activation, and involvement in various human malignancies. An overview of different SphK inhibitors at different phases of clinical trials and can potentially be utilized as cancer therapeutics has also been reviewed. Citation: Gupta, P.; Taiyab, A.; Hussain, A.; Alajmi, M.F.; Islam, A.; Abstract: Sphingolipid metabolites have emerged as critical players in the regulation of various Hassan, M..I. Targeting the Sphingosine Kinase/Sphingosine- physiological processes. Ceramide and sphingosine induce cell growth arrest and apoptosis, whereas 1-Phosphate Signaling Axis in Drug sphingosine-1-phosphate (S1P) promotes cell proliferation and survival. -

Gilenya; FTY720
STRADER, CHERILYN R., M.S. Fingolimod (Gilenya; FTY720): A Recently Approved Multiple Sclerosis Drug Based on a Fungal Secondary Metabolite and the Creation of a Natural Products Pure Compound Database and Organized Storage System. (2012) Directed by Dr. Nicholas H. Oberlies, 78 pp. Fingolimod (Gilenya; FTY720), a synthetic compound based on the fungal secondary metabolite, myriocin (ISP-I), is a potent immunosuppressant that was approved in September 2010 by the U.S. FDA as a new treatment for multiple sclerosis (MS). Fingolimod was synthesized by the research group of Tetsuro Fujita at Kyoto University in 1992 while investigating structure-activity relationships of derivatives of the fungal metabolite, ISP-I, isolated from Isaria sinclairii. Fingolimod becomes active in vivo following phosphorylation by sphingosine kinase 2 to form fingolimod-phosphate, which binds to specific G protein-coupled receptors (GPCRs) and prevents the release of lymphocytes from lymphoid tissue. Fingolimod is orally active, which is unique among current first-line MS therapies, and it has the potential to be used in the treatment of organ transplants and cancer. The first chapter reviews the discovery and development of fingolimod, from an isolated lead natural product, through synthetic analogues, to an approved drug. Natural products play an important role in the pharmaceutical industry, accounting for approximately half of all drugs approved in the U.S. between 1981 and 2006. Given the importance of natural product research and the vast amount of data that is generated in the process, it is imperative that the pure compounds and data are stored in a manner that will allow researchers to derive as much value as possible.