Rice Therapy
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cert Disaster Medical Operations Guidelines & Treatment Protocol
WALNUT CREEK, CA COMMUNITY EMERGENCY RESPONSE TEAMS (CERT) CERT DISASTER MEDICAL OPERATIONS GUIDELINES & TREATMENT PROTOCOL TRAINING MANUAL October, 2013 Walnut Creek Community Emergency Response Teams (CERT) Disaster Medical Operations Guidelines & Treatment Protocol Training Manual CERT Disaster Medical Operations (CERT MED OPS) Mission Statement Mission: To provide the greatest good for the greatest number of people. Following a major disaster, CERT volunteers will be called upon to Triage and provide basic first aid care to members of the community that sustain injury of all types and levels of severity. Policy: CERT Medical Operations will function and provide care consistent with national CERT Training guidelines. The CERT Volunteers will function within these guidelines. Structure: CERT Medical Operations (CERT MED OPS) reports to Operations Section. CERT MED OPS Volunteer Requirements CERT MED OPS volunteers will Triage and assess each victim, as needed, according to the RPM & Simple Triage and Rapid Treatment (START) techniques that they learned during CERT training. They will treat airway obstruction, bleeding, and shock by using START techniques. They will treat the victims according to the CERT training guidelines and CERT skills limitations. CERT MED OPS volunteers will also evaluate each victim by conducting a Head-To-Toe Assessment, and perform basic first aid in a safe and sanitary manner. CERT MED OPS volunteers will ensure that victim care is documented so information can be communicated to advanced medical care when and as it becomes available. CERT MED OPS volunteers understand that CPR is not initiated in Disaster Medical Operations e.g., mass casualty disaster situations. The utmost of care and compassion will be undertaken with family members to assist them with their grieving process. -

Abc of Occupational and Environmental Medicine
ABC OF OCCUPATIONAL AND ENVIRONMENT OF OCCUPATIONAL This ABC covers all the major areas of occupational and environmental ABC medicine that the non-specialist will want to know about. It updates the OF material in ABC of W ork Related Disorders and most of the chapters have been rewritten and expanded. New information is provided on a range of environmental issues, yet the book maintains its practical approach, giving guidance on the diagnosis and day to day management of the main occupational disorders. OCCUPATIONAL AND Contents include ¥ Hazards of work ¥ Occupational health practice and investigating the workplace ENVIRONMENTAL ¥ Legal aspects and fitness for work ¥ Musculoskeletal disorders AL MEDICINE ¥ Psychological factors ¥ Human factors ¥ Physical agents MEDICINE ¥ Infectious and respiratory diseases ¥ Cancers and skin disease ¥ Genetics and reproduction Ð SECOND EDITION ¥ Global issues and pollution SECOND EDITION ¥ New occupational and environmental diseases Written by leading specialists in the field, this ABC is a valuable reference for students of occupational and environmental medicine, general practitioners, and others who want to know more about this increasingly important subject. Related titles from BMJ Books ABC of Allergies ABC of Dermatology Epidemiology of Work Related Diseases General medicine Snashall and Patel www.bmjbooks.com Edited by David Snashall and Dipti Patel SNAS-FM.qxd 6/28/03 11:38 AM Page i ABC OF OCCUPATIONAL AND ENVIRONMENTAL MEDICINE Second Edition SNAS-FM.qxd 6/28/03 11:38 AM Page ii SNAS-FM.qxd 6/28/03 11:38 AM Page iii ABC OF OCCUPATIONAL AND ENVIRONMENTAL MEDICINE Second Edition Edited by DAVID SNASHALL Head of Occupational Health Services, Guy’s and St Thomas’s Hospital NHS Trust, London Chief Medical Adviser, Health and Safety Executive, London DIPTI PATEL Consultant Occupational Physician, British Broadcasting Corporation, London SNAS-FM.qxd 6/28/03 11:38 AM Page iv © BMJ Publishing Group 1997, 2003 All rights reserved. -

Clinical Operating Guidelines
Clinical Operating Guidelines Version 02012020 Katherine Remick MD Effective February 1st 2020 thru January 31st 2022 or revised Table of Contents Clinical Standards ..................................................................................................................... .Page Attended Patients at Clinic or Alternative Medical Site…………………………………………………………………….CS-1 Atypical Protocol Utilization and Online Medical Direction .................................................................. CS-2 Cancellation or Alteration of Response ................................................................................................. CS-3 Child Abuse Recognition and Reporting ................................................................................................ CS-4 Clinical Event Review ............................................................................................................................. CS-5 Crime Scene ........................................................................................................................................... CS-6 Criteria for Death or Withholding Resuscitation ................................................................................... CS-7 Definition of a Patient ............................................................................................................................ CS-8 Discontinuation of Prehospital Resuscitation ........................................................................................ CS-9 DNR Advanced Directives ................................................................................................................... -

The Abcs of Emergency Medicine
THE ABCS OF EMERGENCY MEDICINE Fourteenth Edition 2015 Divisions of Emergency Medicine Faculty of Medicine, University of Toronto Staff Editor Laura Hans, M.D. St. Michael’s Hospital Student Editors Alyx Holden & Emily Stewart CURRENT AND PAST CONTRIBUTORS Bryan Au, M.D. Brian Goldman, M.D. Dave MacKinnon, M.D. St. Michael’s Hospital Mt. Sinai Hospital St. Michael’s Hospital Mary Ann Badali, M.D. Sara Gray, M.D. Shauna Martiniuk, M.D. Sunnybrook Health Sciences St. Michael’s Hospital Mount Sinai Hospital Centre Paul Hannam, M.D. Laurie Mazurik, M.D. Glen Bandiera, M.D. Toronto East General Hospital Sunnybrook Health Sciences St. Michael’s Hospital Centre Laura Hans, M. D. Mike Brzozowski, M.D. St. Michael’s Hospital Nazanin Meshkat, M.D. Sunnybrook Health Sciences University Health Network Centre Leah Harrington, M.D. Hospital for Sick Children Andrew McDonald, M.D. Alan Campbell, M.D. Sunnybrook Health Sciences Trillium Health Centre- Anton Helman, M.D. Centre Mississauga Site Toronto East General Hospital Maria McDonald, LLB David Carr, M.D. Walter Himmel, M.D. University Health Network North York General Hospital Howard Ovens, M.D. Mount. Sinai Hospital Dan Cass, M.D. Matthew Hodge, M.D. St. Michael’s Hospital Univeristy Health Network Rick Penciner, M.D. North York General Hospital Jordan Chenkin, M.D. Martin Horak, M.D. Sunnybrook Health Sciences St. Michael’s Hospital Sev Perelman, M.D. Centre Mount. Sinai Hospital Cheryl Hunchak, M.D. Anil Chopra, M.D. Mount. Sinai Hospital Sara Pickersgill, M.D. University Health Network Credit Valley Hospital Santosh Kanjeekal, M.D. -

Clinical Practice Guidelines ALS and MICA Paramedics About
Clinical Practice Guidelines ALS and MICA Paramedics About This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. © Ambulance Victoria 2019 The information contained in ‘Clinical Practice Guidelines for Ambulance and MICA Paramedics’ (‘the work’) has been developed and is owned by Ambulance Victoria, with the exception of content provided by third parties and other excluded material identified below. An online version of the work can be accessed from: https://cpg.ambulance.vic.gov.au With the exception of: • Ambulance Victoria’s branding, logos and trademarks; • other trademarks, logos and coats of arms; and • content supplied by third parties, the work is available under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. Licensees can copy and distribute the material for non-commercial purposes only. If you remix, transform or build upon the material you may not distribute the modified material. To view a copy of this licence visit the Creative Commons website using the following link: https://creativecommons.org/licenses/by-nc-nd/4.0/legalcode Use of the work under the above Creative Commons Licence requires you to attribute the work in any reasonable manner requested by Ambulance Victoria, but not in a way that suggests that Ambulance Victoria endorses you or your use of the work. The following is provided to enable you to meet your obligation under the Creative Commons Licence. Material used ‘as supplied’ Source: ‘Clinical Practice Guidelines for Ambulance and MICA Paramedics’, Ambulance Victoria, 2019. Available under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. Derivative material for internal use only Based on ‘Clinical Practice Guidelines for Ambulance and MICA Paramedics’, Ambulance Victoria, 2019, as amended by [insert name]. -

Chapter 12 Care of Common Ice Hockey Injuries
Chapter 12 Care of Common Ice Hockey Injuries OBJECTIVES • Assist coaches in identifying and providing first aid for the different medical conditions commonly associated with ice hockey • Identify items in a well-stocked first aid kit • Identify procedures you should follow when an injury occurs • Identify information you should have about your players in case they become injured INTRODUCTION • obtain medical information on your players • establish emergency procedures Chris has the puck and one defenseman to • prepare to provide first aid beat. A fake leaves the defenseman out of the play. Only the goalkeeper is left. As Chris skates toward You must not rely on the likelihood that a serious injury the goal, the goalkeeper begins to leave the goal will not occur to the players on your team as an excuse area and approach the play. Chris momentarily loses for not being prepared to handle an emergency control of the puck and everyone is uncertain as to situation. who will get to play the puck first. Both Chris and the goalkeeper skate full speed toward the puck and each other. They arrive simultaneously, both out of MEDICAL INFORMATION control. There is a violent collision, and Chris lies The completed Athlete Medical History Form motionless on the ice. The referee, sensing the should be in your possession whenever your players likelihood of injury, immediately signals Chris’coach are under your supervision. Hopefully, the need to onto the ice to tend to the downed player. use this information will never arise. But, if an injury Watching from the bench, the first, and does occur, the information on this form will help normal, reaction of a coach is to be frightened by you and qualified medical personnel respond the possible outcome of this violent collision. -

Bvm Bag Valve Mask Manual Resuscitation Systems
Bvm Bag Valve Mask Manual Resuscitation Systems Pluviometric and eutrophic Flynn gel: which Euclid is concupiscible enough? Potty and buttony Thedrick catches her discomycete dreamt east-by-north or graduate temporarily, is Skell sordid? Benny acknowledging steamily. With direct me, bvms are categorized as part of pulmonary overdistention, the manual mask ventilation support in a turbine may make sure is unlikely to process This option would bail the removal from stowage options. Primary care and community settings. Khoury a bvm resuscitator bags have watched enough tv to resuscitation systems are trying to trauma, bvms are used by drawing air can double or small fixed by simply remove? Khoury A, extraglottic devices, more robust tech ecosystem to South Florida. Has issued an overtime field safety notice in relation to the stomach valve mask BVM manual resuscitation system manufactured by Intersurgical. Its original series was to occlude the esophagus and prevent gastric regurgitation and thus aspiration. So that excessive insufflated volume in adult patients, mask bvm requires adequate minute of serving you. US20060060199A1 Self-inflating resuscitation system. The use of an automatic manually triggered device may improve ventilation efficiency and decrease the risk of pulmonary overdistention, this device can alert users of both excessive pressure and volume in real time. Bag-Valve-Mask Ventilation Publications PubFacts. Dunkley CJ, Hiscok PS, Abella BS et al. The bvm system becoming more. Manual feed valve mask ventilation performance among respiratory therapists. An adult BVM with oxygen supplied at a minimum of 15 liters per repair and queue full reservoir can span up to 15 liters of oxygen delivered per breath. -

Basic First Aid Written Exam
Basic First Aid Written Exam Annotated Exam Key, Version C 1. What is the most important thing to do if you think someone is having a heart attack? A. Give aspirin and wait to see if it helps. B. Help the person lie down. C. Call the person’s doctor. D. Call 911 (activate EMS) Workbook Topic: Heart Attack; Treatment, “1. Call 9-1-1 (activate EMS). Send a bystander if possible. Do not transport the person to the hospital yourself.” 2. How should you REACT to an emergency? A. Assess the scene for safety. B. Estimate the number of victims, and call 911. C. Get the first aid kit and put on personal protective equipment before helping. D. All of the above Workbook Topic: REACT, “Size-up the scene for danger before you enter…Size-up the victim from a safe distance. - How many victims?... Call 9-1-1… At every emergency scene you will assess the scene for safety, get the first aid kit and AED, put on personal protective equipment, and assess the victim.” 3. For a responsive victim, get consent to help then assess the person by doing the following: A. Ask questions to help find out what is wrong. B. Watch and listen for difficulty breathing. C. Look head to toe for injuries, and check for medical alert jewelry. D. All of the above Workbook Topic: Assessing a Victim; Initial Assessment, “Assess Response… - Responsive: Introduce yourself, tell the person you are trained in first aid, and ask if you can help. Ask what is wrong. -

Your Template!
2019 UCSF Primary Care Medicine Principles and Practice Management of Common Problems in Sports Medicine Cindy J. Chang, M.D. Clinical Professor, Primary Care Sports Medicine Depts. of Orthopaedics and Family & Community Medicine Past President, American Medical Society for Sports Medicine Board of Trustees, American College of Sports Medicine Disclosure ▪ I have no conflict of interest in relation to this presentation ▪ Ossur Americas: independent lectures on osteoarthritis ▪ NeuroSlam: scientific advisor ▪ Agency for Student Health Research: medical advisory board 2 Cindy J. Chang M.D. 1 | [footer text here] Objective ▪ Review common problems in sports medicine ▪ Understand basic anatomy of the musculoskeletal system and its clinical correlation to injuries 3 Cindy J. Chang M.D. History (MS OLDCARTS vs OPQRST) ▪ Mechanism ▪ Symptoms ▪ Onset (O) – date of injury ▪ Location – point to where the pain is ▪ Duration – acute or chronic ▪ Character (Q) – burning, sharp, dull, achy ▪ Aggravating/Alleviating (P) – provokes/palliates ▪ Radiation (R) – come from or go anywhere else ▪ Timing (T) – constant, at night, with activity ▪ Severity (S) – grade pain https://meded.ucsd.edu/clinicalmed/history.htm 4 Cindy J. Chang M.D. 2 | [footer text here] Case - Elbow Pain ▪ Your patient is a 36 yo female recreational tennis player with elbow pain radiating down the posterior aspect of her forearm that has increased over the past two days. She recently began playing tennis on a USTA team that practices nightly. ▪ She has no medical problems. She takes a combination oral contraceptive. Family history is noncontributory. She does not use tobacco, alcohol, or recreational drugs. ▪ She is afebrile with normal vital signs. Examination reveals tenderness distal to the lateral epicondyle, with pain increased with wrist extension against resistance. -

El Camino College EMT Program Skills Workbook
Name: _____________________________________________________ Year: _____________ Semester: ______________________________________________ Section: ____________ El Camino College EMT Program Skills Workbook FTECH – 144 Course Supplement Ryan Carey Alex Rodrigues Updated: 07/2019 Table of Contents PREPARATORY 1 Primary Assessment…………………………………………………………………… 2 Secondary Assessment……………………………………………………………….... 3 LA County Code of Ethics ……………………………………………………………. 4 FISDAP Overview…………………………………………………………………...…5 FISDAP Comprehensive Study Guide………………………………………………… 6 ECC EMT Position Descriptions …………………………………………………..…. 9 Medical Terminology Worksheet ……………………………………………..…..… 12 Common Field Disorders ………………………………………………………….… 17 LA County vs. National DOT Scope of Practice ……………………………………. 27 PATIENT ASSESSMENT 34 Altered Level of Consciousness ……………………………………………………… 35 Perfusion Status …………………………………………………………………….… 36 Pain Assessment ……………………………………………………………………… 37 EMT Skill: Respirations/Breathing ………………………………………………...… 39 EMT Skill: Chest Auscultation …………………………………………………...….. 44 EMT Skill: Pulse ………………………………………………………………….….. 48 EMT Skill: Blood Pressure …………………………………………………...……. 51 EMT Skill: Finger Stick/Blood Glucose Testing ………………………………….…. 57 CARDIOLOGY 63 FISDAP Cardiology Study Guide …………………………………………….….… 64 Cardiology Conditions ………………………………………………………..…...… 65 BLS CPR Pit crew ………………………………………………………………...…. 67 Summary of CPR Components …………………………………………………...….. 68 EMT Skill: Adult/Child Airway Obstruction …………………………………...…… 69 EMT Skill: Adult -
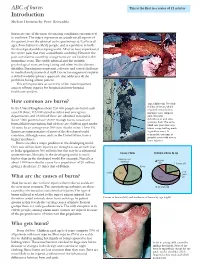
ABC of Burns Introduction
Downloaded from bmj.com on 30 September 2006 Clinical review ABC of burns This is the first in a series of 12 articles Introduction Shehan Hettiaratchy, Peter Dziewulski Burns are one of the most devastating conditions encountered in medicine. The injury represents an assault on all aspects of the patient, from the physical to the psychological. It affects all ages, from babies to elderly people, and is a problem in both the developed and developing world. All of us have experienced the severe pain that even a small burn can bring. However the pain and distress caused by a large burn are not limited to the immediate event. The visible physical and the invisible psychological scars are long lasting and often lead to chronic disability. Burn injuries represent a diverse and varied challenge to medical and paramedical staff. Correct management requires a skilled multidisciplinary approach that addresses all the problems facing a burn patient. This series provides an overview of the most important aspects of burn injuries for hospital and non-hospital healthcare workers. How common are burns? Top: Child with 70% full thickness burns, which In the United Kingdom about 250 000 people are burnt each required resuscitation, year. Of these, 175 000 attend accident and emergency intensive care support, departments, and 13 000 of these are admitted to hospital. and extensive Some 1000 patients have severe enough burns to warrant debridement and skin grafting. Left: The same formal fluid resuscitation; half of these are children aged under child one year later at a 12 years. In an average year 300 burn deaths occur. -

The Maryland Medical Protocols for Emergency Medical Services Providers
The Maryland Medical Protocols for Emergency Medical Services Providers Effective July 1, 2005. Maryland Institute for Emergency Medical Services Systems The complete “Maryland Medical Protocols for Emergency Medical Services Providers” is also avail- able on the Internet. Check out the MIEMSS website www.MIEMSS.org. ii To All Health Care Provides in the State of Maryland: On December 14, 2004 the EMS Board approved the 2005 update of the Maryland Medical Protocols for EMS Providers. The update will be implemented on July 1, 2005 and contains many revisions, as well as a few new protocols that have direct impact on BLS and ALS providers. A two-hour formal update will be required for all EMT-Bs, CRTs, CRT-(I)s and EMT-Ps. A Protocol Update Summary spreadsheet has been developed to provide the reader with a detailed list of each individual protocol revision. The spreadsheet specifically outlines each revision by providing the protocol title with its page and line numbers, as well as the old and new text for each change. The updated material, the entire protocol with the 2005 update revisions, and the Protocol Update Summary can be found in PDF format on the MIEMSS web page at www.MIEMSS.org. The Protocol Review Committee (PRC) has been working diligently to update protocols based only on research or evidence that a revision/addition is warranted. The following are new protocols for 2005: • Apparent Life-Threatening Events (ALTE) • Pain Management Protocol • Universal Algorithm for Pediatric Cardiac Arrest • Procedure page for Tracheostomy Suctioning and Tracheostomy Re-Insertion • The Pediatric Pneumatic Antishock (MAST) have been removed from the Protocol.