Shock Waves in the Treatment of Stress Fractures
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Fibular Stress Fractures in Runners
Fibular Stress Fractures in Runners Robert C. Dugan, MS, and Robert D'Ambrosia, MD New Orleans, Louisiana The incidence of stress fractures of the fibula and tibia is in creasing with the growing emphasis on and participation in jog ging and aerobic exercise. The diagnosis requires a high level of suspicion on the part of the clinician. A thorough history and physical examination with appropriate x-ray examination and often technetium 99 methylene diphosphonate scan are re quired for the diagnosis. With the advent of the scan, earlier diagnosis is possible and earlier return to activity is realized. The treatment is complete rest from the precipitating activity and a gradual return only after there is no longer any pain on deep palpation at the fracture site. X-ray findings may persist 4 to 6 months after the initial injury. A stress fracture is best described as a dynamic tigue fracture, spontaneous fracture, pseudofrac clinical syndrome characterized by typical symp ture, and march fracture. The condition was first toms, physical signs, and findings on plain x-ray described in the early 1900s, mostly by military film and bone scan.1 It is a partial or incomplete physicians.5 The first report from the private set fracture resulting from an inability to withstand ting was in 1940, by Weaver and Francisco,6 who nonviolent stress that is applied in a rhythmic, re proposed the term pseudofracture to describe a peated, subthreshold manner.2 The tibiofibular lesion that always occurred in the upper third of joint is the most frequent site.3 Almost invariably one or both tibiae and was characterized on roent the fracture is found in the distal third of the fibula, genograms by a localized area of periosteal thick although isolated cases of proximal fibular frac ening and new bone formation over what appeared tures have also been reported.4 The symptoms are to be an incomplete V-shaped fracture in the cor exacerbated by stress and relieved by inactivity. -

MARCH FRACTURE-PIED FORCE Developed Reactions to These Test Products and to Witte Peptone at Least As Severe As Those Shown by Our by Anaphylactic Case
FEB. 24, 1940 ANAPHYLAXIS AFTER TETANUS TOXOID MERCALTSORHL 95 erythema than similar dilutions of the extracts, and that within a few minutes of injection many persons MARCH FRACTURE-PIED FORCE developed reactions to these test products and to Witte peptone at least as severe as those shown by our BY anaphylactic case. Further investigations are in progress which it is hoped will be the subject of another paper. F. A. R. STAMMERS, Ch.M., F.R.C.S. Our observations throw considerable doubt on the value Major R.A.M.C., Surgical Specialist of scratch and intradermal tests as usually interpreted on the basis of early readings. Nevertheless, our patient Army medical officers everywhere have been asked to see was the only subject who developed mild anaphylactic all sorts of foot troubles precipitated by military training. symptoms-itching of the nose and tongue, slight swelling More often than not these are due to pre-existing con- of the lower lip, smarting of the eyes, and flushing of the ditions such as hallux rigidus, hallux valgus, hammer-toe, face-soon after 1 in 1,000 dilutions of Witte peptone and or pes planus, which, though formerly symptomless, break two other beef fibrin digests had been injected intra- down under the strain of route-marching, physical train- dermally; and she alone showed areas of redness, 50 to ing, and the general extra footwork the soldier- is called 60 mm. in diameter, swelling, and induration (" like upon to do in heavy army boots. Even a seemingly those occurring after staphylococcus toxoid ") about two normal foot may develop trouble under such circum- hours later at the sites of injection of these products. -

Skier Tibia (Leg) Fractures
Skier Tibia (Leg) Fractures In years past, the prototypical ski fracture was sustained at the lower part of the outside of the leg in the region of the ankle. However, in the past 10 years, with the advent of the modern ski boots and improvements in binding, the most commonly seen lower leg skier fracture is the tibia (or shinbone) fracture. 10% of these fractures are associated with a collision. Thus, 90 % are associated with an isolated fall or noncontact type of injury, which is generally the result of binding malfunctions and inappropriate release. The most common mechanism leading to a tibia (leg) fracture is a forward fall. Risk factors for sustaining a skier tibia fracture include: beginners or novice skiers, less than 20 years of age, higher outdoor temperatures, and increased snow depth. Non-risk factors include ski lengths, icy conditions, and male versus female sex. The modern ski boot very closely resembles an extremely well padded short leg cast in the treatment of many orthopaedic lower extremity fractures. It of course goes to a much higher level than the former shorter boot top-level varieties. The binding release and designs have been based on the fracture strength of the adult tibia (shin) bone at the top of the modern ski boot. The treatment of most skier leg fractures includes a closed reduction and cast application for variable periods of time, with or without weight bearing allowed. However, severe misalignments of the bones can lead to later bony prominences that may be incompatible with snug, rigid, high fitting ski boots. -

Assessment, Management and Decision Making in the Treatment Of
Pediatric Ankle Fractures Anthony I. Riccio, MD Texas Scottish Rite Hospital for Children Update 07/2016 Pediatric Ankle Fractures The Ankle is the 2nd most Common Site of Physeal Injury in Children 10-25% of all Physeal Injuries Occur About the Ankle Pediatric Ankle Fractures Primary Concerns Are: • Anatomic Restoration of Articular Surface • Restoration of Symmetric Ankle Mortise • Preservation of Physeal Growth • Minimize Iatrogenic Physeal Injury • Avoid Fixation Across Physis in Younger Children Salter Harris Classification Prognosis and Treatment of Pediatric Ankle Fractures is Often Dictated by the Salter Harris Classification of Physeal Fractures Type I and II Fractures: Often Amenable to Closed Tx / Lower Risk of Physeal Arrest Type III and IV: More Likely to Require Operative Tx / Higher Risk of Physeal Arrest Herring JA, ed. Tachdjian’s Pediatric Orthopaedics, 5th Ed. 2014. Elsevier. Philadelphia, PA. ISOLATED DISTAL FIBULA FRACTURES Distal Fibula Fractures • The Physis is Weaker than the Lateral Ankle Ligaments – Children Often Fracture the Distal Fibula but…. – …ligamentous Injuries are Not Uncommon • Mechanism of Injury = Inversion of a Supinated Foot • SH I and II Fractures are Most Common – SH I Fractures: Average Age = 10 Years – SH II Fractures: Average Age = 12 Years Distal Fibula Fractures Lateral Ankle Tenderness SH I Distal Fibula Fracture vs. Lateral Ligamentous Injury (Sprain) Distal Fibula Fractures • Sankar et al (JPO 2008) – 37 Children – All with Open Physes, Lateral Ankle Tenderness + Normal Films – 18%: Periosteal -

Overuse Injuries in Sport: a Comprehensive Overview R
Aicale et al. Journal of Orthopaedic Surgery and Research (2018) 13:309 https://doi.org/10.1186/s13018-018-1017-5 REVIEW Open Access Overuse injuries in sport: a comprehensive overview R. Aicale1*, D. Tarantino1 and N. Maffulli1,2 Abstract Background: The absence of a single, identifiable traumatic cause has been traditionally used as a definition for a causative factor of overuse injury. Excessive loading, insufficient recovery, and underpreparedness can increase injury risk by exposing athletes to relatively large changes in load. The musculoskeletal system, if subjected to excessive stress, can suffer from various types of overuse injuries which may affect the bone, muscles, tendons, and ligaments. Methods: We performed a search (up to March 2018) in the PubMed and Scopus electronic databases to identify the available scientific articles about the pathophysiology and the incidence of overuse sport injuries. For the purposes of our review, we used several combinations of the following keywords: overuse, injury, tendon, tendinopathy, stress fracture, stress reaction, and juvenile osteochondritis dissecans. Results: Overuse tendinopathy induces in the tendon pain and swelling with associated decreased tolerance to exercise and various types of tendon degeneration. Poor training technique and a variety of risk factors may predispose athletes to stress reactions that may be interpreted as possible precursors of stress fractures. A frequent cause of pain in adolescents is juvenile osteochondritis dissecans (JOCD), which is characterized by delamination and localized necrosis of the subchondral bone, with or without the involvement of articular cartilage. The purpose of this compressive review is to give an overview of overuse injuries in sport by describing the theoretical foundations of these conditions that may predispose to the development of tendinopathy, stress fractures, stress reactions, and juvenile osteochondritis dissecans and the implication that these pathologies may have in their management. -

Listen to the Associated Podcast Episodes: MSK: Fractures for the ABR Core Exam Parts 1-3, Available at Theradiologyreview.Com O
MSK: Fractures for Radiology Board Study, Matt Covington, MD Listen to the associated podcast episodes: MSK: Fractures for the ABR Core Exam Parts 1-3, available Listen to associated Podcast episodes: ABR Core Exam, Multisystemic Diseases Parts 1-3, available at at theradiologyreview.com or on your favorite podcast directory. Copyrighted. theradiologyreview.com or on your favorite podcast direcry. Fracture resulting From abnormal stress on normal bone = stress Fracture Fracture From normal stress on abnormal bone = insuFFiciency Fracture Scaphoid Fracture site with highest risk for avascular necrosis (proximal or distal)? Proximal pole scaphoid Fractures are at highest risk For AVN Comminuted Fracture at the base oF the First metacarpal = Rolando Fracture Non-comminuted Fracture at base oF the First metacarpal = Bennett Fracture The pull oF which tendon causes the dorsolateral dislocation in a Bennett fracture? The abductor pollicus longus tendon. Avulsion Fracture at the base oF the proximal phalanx with ulnar collateral ligament disruption = Gamekeeper’s thumb. Same Fracture but adductor tendon becomes caught in torn edge oF the ulnar collateral ligament? Stener’s lesion. IF Stener’s lesion is present this won’t heal on its own so you need surgery. You shouldn’t image a Gamekeeper’s thumb with stress views because you can convert it to a Stener’s lesion. Image with MRI instead. Distal radial Fracture with dorsal angulation = Colle’s Fracture (C to D= Colle’s is Dorsal) Distal radial Fracture with volar angulation = Smith’s Fracture (S -

Long Term Treatment of Recurring Pathological Fractures Due to Mccune Albright Syndrome: Case Report and Literature Review
Vol.2, No.9, 562-567 (2013) Case Reports in Clinical Medicine http://dx.doi.org/10.4236/crcm.2013.29142 Long term treatment of recurring pathological fractures due to Mccune Albright Syndrome: Case report and literature review Yoshvin Sunnassee, Yuhui Shen, Rong Wan, Jianqiang Xu, Weibin Zhang* Department of Orthopedics, Shanghai Ruijin Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai Institute of Traumatology and Orthopedics, Shanghai, China; *Corresponding Author: [email protected] Received 17 June 2013; revised 15 July 2013; accepted 10 August 2013 Copyright © 2013 Yoshvin Sunnassee et al. This is an open access article distributed under the Creative Commons Attribution Li- cense, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. In accordance of the Creative Commons Attribution License all Copyrights © 2013 are reserved for SCIRP and the owner of the intel- lectual property Yoshvin Sunnassee et al. All Copyright © 2013 are guarded by law and by SCIRP as a guardian. ABSTRACT mentation, precocious puberty and polyostotic fibrous dysplasia (PFD) [1,2]. Patients with PFD have poor bone McCune Albright syndrome is a rare genetic quality and are liable to pathological fractures. We here- disorder which is characterized by café au lait by report the case of a male patient who is treated for 7 skin pigmentation, precocious puberty and poly- years in our center for recurring pathological fractures of ostotic fibrous dysplasia. Treating recurring pa- the femur due to MAS. When the patient was first seen, thological fractures due to Albright syndrome is he presented with a shepherd’s crook deformity of the a very challenging endeavor, and more so when proximal femur. -

Neurofibromatosis with Pancreatic Duct Obstruction and Steatorrhoea
Postgrad Med J: first published as 10.1136/pgmj.43.500.432 on 1 June 1967. Downloaded from 432 Case reports References KORST, D.R., CLATANOFF, D.V. & SCHILLING, R.F. (1956) APPLEBY, A., BATSON, G.A., LASSMAN, L.P. & SIMPSON, On myelofibrosis. Arch. intern. Med. 97, 169. C.A. (1964) Spinal cord compression by extramedullary LEIBERMAN, P.H., ROSVOLL, R.V. & LEY, A.B. (1965) Extra- haematopoiesis in myelosclerosis. J. Neurol. Neurosurg. medullary myeloid tumors in primary myelofibrosis. Psychiat. 27, 313. Cancer, 18, 727. ASK-UPMARK, E. (1945) Tumour-simulating intra-thoracic LEIGH, T.F., CORLEY, C.C., Jr, HUGULEY, C.M. & ROGERS, heterotopia of bone marrow, Acta radiol. (Stockh.), 26, J.V., Jr (1959) Myelofibrosis. The general and radiologic 425. in 25 cases. Amer. J. 82, 183. BRANNAN, D. (1927) Extramedullary hematopoiesis in findings proved Roentgenol. anaemias. Bull. Johns Hopk. Hosp. 41 104. LOWMAN, R.M., BLOOR, C.M. & NEWCOMB, A.W. (1963) CLOSE, A.S., TAIRA, Y. & CLEVELAND, D.A. (1958) Spinal Thoracic extramedullary hematopoiesis. Dis. Chest. 44, cord compression due to extramedullary hematopoiesis. 154. Ann. intern. Med. 48, 421. MALAMOS, B., PAPAVASILIOU, C. & AVRAMIS, A. (1962) CRAVEN, J.D. (1964) Renal glomerular osteodystrophy. Tumor-simulating intrathoracic extramedullary hemo- Clin. Radiol. 15, 210. poiesis. Report of a case. Acta radiol. (Stockh.), 57, 227. DENT, C.E. (1955) Clinical section. Proc. roy. Soc. Med. 48, 530. PITCOCK, J.A., REINHARD, E.H., JUSTUS, B.W. & MENDEL- DODGE, O.G. & EVANS, D. (1956) Haemopoiesis in a pre- SOHN, R.S. (1962) A clinical and pathological study of 70 sacral tumor (myelolipoma). -

WHO Manual of Diagnostic Imaging Radiographic Anatomy and Interpretation of the Musculoskeletal System
The WHO manual of diagnostic imaging Radiographic Anatomy and Interpretation of the Musculoskeletal System Editors Harald Ostensen M.D. Holger Pettersson M.D. Authors A. Mark Davies M.D. Holger Pettersson M.D. In collaboration with F. Arredondo M.D., M.R. El Meligi M.D., R. Guenther M.D., G.K. Ikundu M.D., L. Leong M.D., P. Palmer M.D., P. Scally M.D. Published by the World Health Organization in collaboration with the International Society of Radiology WHO Library Cataloguing-in-Publication Data Davies, A. Mark Radiography of the musculoskeletal system / authors : A. Mark Davies, Holger Pettersson; in collaboration with F. Arredondo . [et al.] WHO manuals of diagnostic imaging / editors : Harald Ostensen, Holger Pettersson; vol. 2 Published by the World Health Organization in collaboration with the International Society of Radiology 1.Musculoskeletal system – radiography 2.Musculoskeletal diseases – radiography 3.Musculoskeletal abnormalities – radiography 4.Manuals I.Pettersson, Holger II.Arredondo, F. III.Series editor: Ostensen, Harald ISBN 92 4 154555 0 (NLM Classification: WE 141) The World Health Organization welcomes requests for permission to reproduce or translate its publications, in part or in full. Applications and enquiries should be addressed to the Office of Publications, World Health Organization, CH-1211 Geneva 27, Switzerland, which will be glad to provide the latest information on any changes made to the text, plans for new editions, and reprints and translations already available. © World Health Organization 2002 Publications of the World Health Organization enjoy copyright protection in accordance with the provisions of Protocol 2 of the Universal Copyright Convention. All rights reserved. -
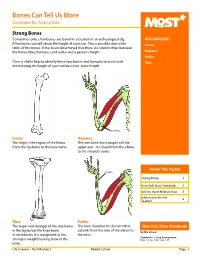
Bones Can Tell Us More Compiled By: Nancy Volk
Bones Can Tell Us More Compiled By: Nancy Volk Strong Bones Sometimes only a few bones are found in a location in an archeological dig. VOCABULARY A few bones can tell about the height of a person. This is possible due to the Femur ratios of the bones. It has been determined that there are relationships between the femur, tibia, humerus, and radius and a person’s height. Humerus Radius Here is a little help to identify these four bones and formulas to assist with Tibia determining the height of a person based on bone length. Humerus Femur: Humerus: The thigh is the region of the femur. The arm bone most people call the From the hip bone to the knee bone. upper arm. It is found from the elbow to the shoulder joints. Inside This Packet Radius Strong Bones 1 New York State Standards 1 Activity: Bone Relationships 2 Information for the Teacher 4 Tibia: Radius: The larger and stronger of the two bones The bone found in the forearm that New York State Standards in the leg below the knee bone. extends from the side of the elbow to Middle School In vertebrates It is recognized as the the wrist. Standard 4: Living Environment strongest weight bearing bone in the Idea 1: 1.2a, 1.2b, 1.2e, 1.2f body. Life Sciences - Post Module 3 Middle School Page 1 Activity: Bone Relationships MATERIALS NEEDED Skeleton Formulas: Tape Measure Bone relationship is represented by the following formulas: Directions and formulas P represents the person’s height. The last letter of each formula stands for the Calculator known length of the bone (femur, tibia, humerus, or radius) through measurement. -

Normative Values for Femoral Length, Tibial Length, Andthe Femorotibial
Article Normative Values for Femoral Length, Tibial Length, and the Femorotibial Ratio in Adults Using Standing Full-Length Radiography Stuart A Aitken MaineGeneral Medical Center, 35 Medical Center Parkway, Augusta, ME 04330, USA; [email protected] Abstract: Knowledge of the normal length and skeletal proportions of the lower limb is required as part of the evaluation of limb length discrepancy. When measuring limb length, modern standing full-length digital radiographs confer a level of clinical accuracy interchangeable with that of CT imaging. This study reports a set of normative values for lower limb length using the standing full-length radiographs of 753 patients (61% male). Lower limb length, femoral length, tibial length, and the femorotibial ratio were measured in 1077 limbs. The reliability of the measurement method was tested using the intra-class correlation (ICC) of agreement between three observers. The mean length of 1077 lower limbs was 89.0 cm (range 70.2 to 103.9 cm). Mean femoral length was 50.0 cm (39.3 to 58.4 cm) and tibial length was 39.0 cm (30.8 to 46.5 cm). The median side-to-side difference was 0.4 cm (0.2 to 0.7, max 1.8 cm) between 324 paired limbs. The mean ratio of femoral length to tibial length for the study population was 1.28:1 (range 1.16 to 1.39). A moderately strong inverse linear relationship (r = −0.35, p < 0.001, Pearson’s) was identified between tibial length and the Citation: Aitken, S.A. Normative corresponding femorotibial ratio. -

Tibial De-Rotational Osteotomies for Tibial Torsion
Tibial De-Rotational Osteotomies for Tibial Torsion Why does my child need tibial torsion surgery? What happens during the surgery? A lot of young children walk with their toes pointing in or First, the surgeon cracks the tibia and the smaller fibula bone out instead of straight ahead. The most common reason is next to it, usually just above the ankle. Surgically cracking a tibial torsion, a twist in the tibia bone of the lower leg. This bone is also known as an osteotomy. It is similar to breaking twist brings the knee and ankle out of alignment. The feet a bone, except that it is done on purpose. The surgeon respond by turning in (internal tibia torsion) or out (external weakens the tibia bone first by drilling holes through a small tibia torsion). Most of the time, tibial torsion gets better as a surgical opening. The next step is to rotate, or turn, the bone child exercises the leg muscles by walking and running. into correct alignment. The surgeon then places a pin in the bone just below the knee. The pin will be removed once the But when a child has spasticity, a condition in which muscle bone heals. In the meantime, your child will wear a cast that tone is very strong, tibial torsion can get worse instead starts at the pin and covers the leg and foot. The cast keeps of better as the child grows. Surgery helps children with the leg from moving while new bone grows. spasticity who can stand, but cannot walk or run normally because of tibial torsion.