Joint Classification
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-
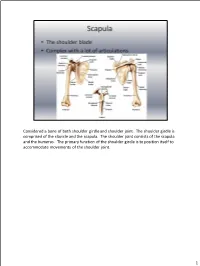
Considered a Bone of Both Shoulder Girdle and Shoulder Joint. the Shoulder Girdle Is Comprised of the Clavicle and the Scapula
Considered a bone of both shoulder girdle and shoulder joint. The shoulder girdle is comprised of the clavicle and the scapula. The shoulder joint consists of the scapula and the humerus. The primary function of the shoulder girdle is to position itself to accommodate movements of the shoulder joint. 1 Superior angle—top point Inferior angle—bottom point Vertebral border—side closest to vertebral column Axillary border—side closest to arm Subscapular fossa—anterior fossa Glenoid fossa, glenoid labrum, glenoid cavity --The glenoid fossa is the shallow cavity where the humeral head goes. The glenoid labrum is the cartilage that goes around the glenoid fossa. So the glenoid fossa and glenoid labrum together comprise the glenoid cavity. Supraspinous fossa—posterior, fossa above the spine Spine of the scapula—the back projection Infraspinous fossa—posterior depression/fossa below spine Coracoid process—anterior projection head Acromion process—posterior projection head above spine 2 Scapulothoracic “joint” = NOT a true joint; there are no ligaments or articular capsule. The scapula just rests on the muscle over top the rib cage, which allows for passive movements. Sternoclavicular joint=where the clavicle (collarbone) and the sternum (breastbone) articulate; movement is slight in all directions and of a gliding, rotational type Acromioclavicular joint = where the clavicle and scapula (acromion process) articulate; AKA: AC Joint; movement is a slight gliding when elevation and depression take place. Glenohumeral joint = the shoulder joint 3 4 All 3 true joints: Sternoclavicular, AC and glenohumeral (GH) all work together to move arm in all directions. The GH allows the arm to go out to the side and be abducted, then the AC and Sternoclavicular joints kick in to allow the arm to go above shoulder level by allowing the shoulderblade to move up to increase the range of motion (ROM). -

The Proximal Interphalangeal Joint: Arthritis and Deformity
4.1800EOR0010.1302/2058-5241.4.180042 research-article2019 EOR | volume 4 | June 2019 DOI: 10.1302/2058-5241.4.180042 Instructional Lecture: Hand & Wrist www.efortopenreviews.org The proximal interphalangeal joint: arthritis and deformity Daniel Herren Finger joints are of the most common site of osteoarthritis Most authors, especially in the rheumatology and arthritis and include the DIP, PIP and the thumb saddle joint. literature, use a modification of the Kellgren and Lawrence 1 Joint arthroplasty provides the best functional outcome scale, initially described for patellofemoral arthritis, for for painful destroyed PIP joints, including the index finger. radiographic classification: Adequate bone stock and functional tendons are required for a successful PIP joint replacement Grade 1: doubtful narrowing of joint space and pos- sible osteophytic lipping Fixed swan-neck and boutonnière deformity are better served with PIP arthrodesis rather than arthroplasty. Grade 2: definite osteophytes, definite narrowing of joint space Silicone implants are the gold standard in terms of implant choice. Newer two-component joints may have potential Grade 3: moderate multiple osteophytes, definite nar- to correct lateral deformities and improve lateral stability. rowing of joint space, some sclerosis and possible deformation of bone contour Different surgical approaches are used for PIP joint implant arthroplasty according to the needs and the experience of Grade 4: large osteophytes, marked narrowing of joint the surgeon. space, severe sclerosis and definite deformation of bone contour Post-operative rehabilitation is as critical as the surgical procedure. Early protected motion is a treatment goal. Revision and exchange PIP arthroplasty may successfully Treatment be used to treat chronic pain, but will not correct defor- mity. -

Synovial Joints Permit Movements of the Skeleton
8 Joints Lecture Presentation by Lori Garrett © 2018 Pearson Education, Inc. Section 1: Joint Structure and Movement Learning Outcomes 8.1 Contrast the major categories of joints, and explain the relationship between structure and function for each category. 8.2 Describe the basic structure of a synovial joint, and describe common accessory structures and their functions. 8.3 Describe how the anatomical and functional properties of synovial joints permit movements of the skeleton. © 2018 Pearson Education, Inc. Section 1: Joint Structure and Movement Learning Outcomes (continued) 8.4 Describe flexion/extension, abduction/ adduction, and circumduction movements of the skeleton. 8.5 Describe rotational and special movements of the skeleton. © 2018 Pearson Education, Inc. Module 8.1: Joints are classified according to structure and movement Joints, or articulations . Locations where two or more bones meet . Only points at which movements of bones can occur • Joints allow mobility while preserving bone strength • Amount of movement allowed is determined by anatomical structure . Categorized • Functionally by amount of motion allowed, or range of motion (ROM) • Structurally by anatomical organization © 2018 Pearson Education, Inc. Module 8.1: Joint classification Functional classification of joints . Synarthrosis (syn-, together + arthrosis, joint) • No movement allowed • Extremely strong . Amphiarthrosis (amphi-, on both sides) • Little movement allowed (more than synarthrosis) • Much stronger than diarthrosis • Articulating bones connected by collagen fibers or cartilage . Diarthrosis (dia-, through) • Freely movable © 2018 Pearson Education, Inc. Module 8.1: Joint classification Structural classification of joints . Fibrous • Suture (sutura, a sewing together) – Synarthrotic joint connected by dense fibrous connective tissue – Located between bones of the skull • Gomphosis (gomphos, bolt) – Synarthrotic joint binding teeth to bony sockets in maxillae and mandible © 2018 Pearson Education, Inc. -

Isaac Newton Academy Revision Booklet- Exam 1
Isaac Newton Academy Revision Booklet- Exam 1 Component 01: Physical factors affecting performance 1.1 Applied anatomy and physiology 1.2 Physical training. Functions of the skeleton Location of Major Bones Bone stores crucial nutrients, minerals, and lipids and produces blood cells that nourish the body and play a vital role in protecting the body against infection. Bones have many functions, including the following: Support: Bones provide a framework for the attachment of muscles and other tissues. Bone Location Arm - humerus, radius and ulna. Hand - Carpals, Metacarpals and Phalanges. Sternum and Ribs. Femur – the thigh bone. Patella – the knee cap. Tibia – the shin bone, the larger of the two leg bones located below the knee cap. Fibula – the smaller of the two leg bones located below the knee cap. The OCR Spec expects us to know the following regarding synovial joints: The definition of a synovial joint, Articulating bones of the knee and elbow hinge joints and also the articulating bones of the shoulder and hip Ball and socket joints Hinge Joint- A hinge joint is found at the knee and the elbow, Synovial Joint- This is a freely moveable joint in thich the bones’ surfaces are covered Articulating bones of the elbow by cartilage and connected by joint are the Humerus radius fibrous connective tissue and Ulna . Articulating bones of capsule lines with synovial the knee are the Femur and fluid Tibia. Ball and socket joint- Allows a wide range of movement, they can be Articulating bones- These found at the hip and shoulder. are bones that move within a joint Articulating bones of the shoulder are Humerus and Scapula. -

A Review of Natural Joint Systems and Numerical Investigation of Bio-Inspired GFRP-To-Steel Joints
materials Article A Review of Natural Joint Systems and Numerical Investigation of Bio-Inspired GFRP-to-Steel Joints Evangelos I. Avgoulas and Michael P. F. Sutcliffe * Department of Engineering, University of Cambridge, Trumpington Street, Cambridge CB2 1PZ, UK; [email protected] * Correspondence: [email protected]; Tel.: +44-1223-332-996 Academic Editor: Frank Müller Received: 25 April 2016; Accepted: 1 July 2016; Published: 12 July 2016 Abstract: There are a great variety of joint types used in nature which can inspire engineering joints. In order to design such biomimetic joints, it is at first important to understand how biological joints work. A comprehensive literature review, considering natural joints from a mechanical point of view, was undertaken. This was used to develop a taxonomy based on the different methods/functions that nature successfully uses to attach dissimilar tissues. One of the key methods that nature uses to join dissimilar materials is a transitional zone of stiffness at the insertion site. This method was used to propose bio-inspired solutions with a transitional zone of stiffness at the joint site for several glass fibre reinforced plastic (GFRP) to steel adhesively bonded joint configurations. The transition zone was used to reduce the material stiffness mismatch of the joint parts. A numerical finite element model was used to identify the optimum variation in material stiffness that minimises potential failure of the joint. The best bio-inspired joints showed a 118% increase of joint strength compared to the standard joints. Keywords: natural joints; adhesive joints; biomimetics; bio-inspiration; composites 1. Introduction In recent years, the use of composite materials in automotive and aerospace industries has shown an upward trend due to their good stiffness-to-weight (E/r) and strength-to-weight (s/r) ratios. -

Lecture Notes on Human Anatomy. Part One, Fourth Edition. PUB DATE Sep 89 NOTE 79P.; for Related Documents, See SE 051 219-221
DOCUMENT RESUME ED 315 320 SE 051 218 AUTHOR Conrey, Kathleen TITLE Lecture Notes on Human Anatomy. Part One, Fourth Edition. PUB DATE Sep 89 NOTE 79p.; For related documents, see SE 051 219-221. Black and white illustrations will not reproduce clearly. AVAILABLE FROM Aramaki Design and Publications, 12077 Jefferson Blvd., Culver City, CA 90506 ($7.75). PUB TYPE Guides - Classroom Use - Materials (For Learner) (051) EDRS PRICE MF01 Plus Postage. PC Not Available from EDRS. DESCRIPTORS *Anatomy; *Biological Sciences; *College Science; Higher Education; *Human Body; *Lecture Method; Science Education; Secondary Education; Secondary School Science; Teaching Guides; Teaching Methods ABSTRACT During the process of studying the specific course content of human anatomy, students are being educated to expand their vocabulary, deal successfully with complex tasks, anduse a specific way of thinking. This is the first volume in a set of notes which are designed to accompany a lecture series in human anatomy. This volume Includes discussions of anatomical planes and positions, body cavities, and architecture; studies of the skeleton including bones and joints; studies of the musculature of the body; and studiesof the nervous system including the central, autonomic, motor and sensory systems. (CW) *****1.**k07********Y*******t1.****+***********,****A*******r****** % Reproductions supplied by EDRS are the best that can be made from the original document. **************************************************************A**t***** "PERMISSION TO REPRODUCE -

Ossified Brodie's Ligament
International Journal of Anatomy and Research, Int J Anat Res 2015, Vol 3(2):1084-86. ISSN 2321- 4287 Case Report DOI: http://dx.doi.org/10.16965/ijar.2015.169 OSSIFIED BRODIE’S LIGAMENT R. Siva Chidambaram *1, Neelee Jayasree 2, Soorya Sridhar 3. *1,3 Post Graduate, 2 Professor and Head. Department of Anatomy, Narayana Medical College, Nellore, Andhra Pradesh, India. ABSTRACT The transverse humeral ligament (THL) or Brodie’s ligament is a narrow sheet of connective tissue fibers that runs between the lesser and the greater tubercles of the humerus. Together with the intertubercular groove of the humerus, the ligament creates a canal through which the long head of the biceps tendon and its synovial sheath passes. The ossification of transverse humeral ligament is a rare interesting anatomical variation, which has been identified as one of the predisposing factor for biceps tendonitis and tenosynovitis. In the present study of 100 humerus bones, we found a right side humerus with completely ossified transverse humeral ligament which extended from the lateral margin of lesser tubercle to the medial margin of greater tubercle of the humerus. The Length and breadth of the ossified ligament were 8 mm and 6 mm respectively. Such an ossified ligament may damage the biceps tendon and its synovial sheath during biomechanical movement of the arm leading to anterior shoulder pain. It may also complicate the use of bicipital groove as a landmark for orientation of the humeral prosthesis in complex proximal humeral fractures. Hence, the anatomical knowledge of ossified transverse humeral ligament is important for the radiologist and orthopedic surgeon in diagnosis and planning the treatment for patient with anterior shoulder pain. -

Module 6 : Anatomy of the Joints
Module 6 : Anatomy of the Joints In this module you will learn: About the classification of joints What synovial joints are and how they work Where the hinge joints are located and their functions Examples of gliding joints and how they work About the saddle joint and its function 6.1 Introduction The body has a need for strength and movement, which is why we are rigid. If our bodies were not made this way, then movement would be impossible. We are designed to grow with bones, tendons, ligaments, and joints that all play a part in natural movements known as articulations – these strong connections join up bones, teeth, and cartilage. Each joint in our body makes these links possible and each joint performs a specific job – many of them differ in shape and structure, but all control a range of motion between the body parts that they connect. 6.2 Classifying Joints Joints that do not allow movement are known as synarthrosis joints. Examples of synarthroses are sutures of the skull, and the gomphoses which connect our teeth to the skull. Amphiarthrosis joints allow a small range of movement, an example of this is your intervertebral discs attached to the spine. Another example is the pubic symphysis in your hip region. The freely moving joints are classified as diarthrosis joints. These have a higher range of motion than any other type of joint, they include knees, elbows, shoulders, and wrists. Joints can also be classified depending on the kind of material each one is structurally made up of. A fibrous joint is made up of tough collagen fiber, examples of this are previously mentioned sutures of the skull or the syndesmosis joint, which holds the ulna and radius of your forearm in place. -

Femur Pelvis HIP JOINT Femoral Head in Acetabulum Acetabular
Anatomy of the Hip Joint Overview The hip joint is one of the largest weight-bearing HIP JOINT joints in the body. This ball-and-socket joint allows the leg to move and rotate while keeping the body Femoral head in stable and balanced. Let's take a closer look at the acetabulum main parts of the hip joint's anatomy. Pelvis Bones Two bones meet at the hip joint, the femur and the pelvis. The femur, commonly called the "thighbone," is the longest and heaviest bone of the body. At the top of the femur, positioned on the femoral neck, is the femoral head. This is the "ball" of the hip joint. The other part of the joint – the Femur "socket" – is found in the pelvis. The pelvis is a bone made of three sections: the ilium, the ischium and the pubis. The socket is located where these three sections fuse. The proper name of the socket is the "acetabulum." The head of the femur fits tightly into this cup-shaped cavity. Articular Cartilage The femoral head and the acetabulum are covered Acetabular with a layer of articular cartilage. This tough, smooth tissue protects the bones. It allows them to labrum glide smoothly against each other as the ball moves in the socket. Soft Tissues Several soft tissue structures work together to hold the femoral head securely in place. The acetabulum is surrounded by a ring of cartilage called the "acetabular labrum." This deepens the socket and helps keep the ball from slipping out of alignment. It also acts as a shock absorber. -

Elbow Checklist
Workbook Musculoskeletal Ultrasound September 26, 2013 Shoulder Checklist Long biceps tendon Patient position: Facing the examiner Shoulder in slight medial rotation; elbow in flexion and supination Plane/ region: Transverse (axial): from a) intraarticular portion to b) myotendinous junction (at level of the pectoralis major tendon). What you will see: Long head of the biceps tendon Supraspinatus tendon Transverse humeral ligament Subscapularis tendon Lesser tuberosity Greater tuberosity Short head of the biceps Long head of the biceps (musculotendinous junction) Humeral shaft Pectoralis major tendon Plane/ region: Logitudinal (sagittal): What you will see: Long head of biceps; fibrillar structure Lesser tuberosity Long head of the biceps tendon Notes: Subscapularis muscle and tendon Patient position: Facing the examiner Shoulder in lateral rotation; elbow in flexion/ supination Plane/ region: longitudinal (axial): full vertical width of tendon. What you will see: Subscapularis muscle, tendon, and insertion Supraspinatus tendon Coracoid process Deltoid Greater tuberosity Lesser tuberosity Notes: Do passive medial/ lateral rotation while examining Plane/ region: Transverse (sagittal): What you will see: Lesser tuberosity Fascicles of subscapularis tendon Supraspinatus tendon Patient position: Lateral to examiner Shoulder in extension and medial rotation Hand on ipsilateral buttock Plane/ region: Longitudinal (oblique sagittal) Identify the intra-articular portion of biceps LH in the transverse plane; then -

Mobilization for the Neurologically Involved Child
MOBILIZATION FOR THE NEUROLOGICALLY INVOLVED CHILD Assessment and Application Strategies For Pediatric PTs and OTs Sandy Brooks-Scott M.S., PPT, PCS www.clinicians-view.com Chapter I Pathology and Resultant Immobility Mobility is a worthy goal. However, before it can be achieved in a child with neurological dysfunction, certain prerequisites must be in place: normal bony alignment; normal muscle strength, flexibility and endurance; a coordinating nervous system; an efficient cardiorespi ratory system; and normal connective tissue flexibility. Immobility after initial neurological insult affects all these systems, making assessment and treatment of all systems interfering with efficient mobility a paramount goal of the therapist. Neurological Damage-Original Insult The motor result of the neurological insult is dependent upon the age, the location, and the extent of the insult (Brann 1988; Costello et al. 1988; Nelson 1988; Pape and Wigglesworth 1979). The most widely discussed reason for brain damage in the pre-, peri- or initial postnatal stages is a change in blood pressure, causing the vessels in the developing organ to hemorrhage or become ischemic (Pape and Wigglesworth 1979). Nelson (1988) notes that most infants who live through severe asphyxia at birth do not develop cerebral palsy or mental retardation. Brann (1988), in his discussion of the effects of acute total and prolonged partial asphyxia, clearly demonstrates that the neurological changes and motor outcomes vary depending on the acuteness, duration, and severity of the asphyxia. Because a child will not have autoregulatory mechanisms to control blood pressure until 3 months of age, excessive heat loss, abnormal partial pressures of oxygen and carbon dioxide, or fluid imbalances can affect a newborn's blood pressure, producing ischemic hypoxia and neural damage. -

Degenerative Joint Disease
DEGENERATIVE JOINT DISEASE As our pets age, the tissues lining the bones and joints may deteriorate and degenerate. Degenerative Joint Disease (DJD) describes chronic arthritis (osteoarthritis) which is a gradual deterioration of articular cartilage within the joints. What is DJD? Joints consist of a tough fibrous joint capsule joining the bones. The joint capsule is lined by a thin membrane which produces joint fluid. This acts as a lubricant and also carries nourishment to the spongy articular cartilage which covers the ends of the bones. The articular cartilage does not have any blood supply of its own to provide nourishment and oxygen. The articular cartilage receives nourishment from small vessels in the underlying bone and through absorption from the joint fluid. DJD can follow a number of joint diseases including infection and surgery. It also occurs from excessive weight and obesity. This smooth resilient cartilage degenerates and becomes brittle and may actually split from the bone and become detached within the joint. Although DJD is said to be non-inflammatory, mild inflammation plays a part in causing clinical signs. The damaged cells of the cartilage release substances which result in inflammation, pain and further damage to the cartilage. Thus, once DJD begins it can become a vicious cycle. Can the condition be cured? Most of the damage caused by DJD is irreversible. Fortunately, new products are available that can slow the progress of the disease and promote cartilage healing. In addition, modern analgesics can effectively control pain without few side effects. We will discuss treatment options to allow your pet to enjoy a happy, pain free life.