Upper Airway Innervation
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Superior Laryngeal Nerve Identification and Preservation in Thyroidectomy
ORIGINAL ARTICLE Superior Laryngeal Nerve Identification and Preservation in Thyroidectomy Michael Friedman, MD; Phillip LoSavio, BS; Hani Ibrahim, MD Background: Injury to the external branch of the su- recorded and compared on an annual basis for both be- perior laryngeal nerve (EBSLN) can result in detrimen- nign and malignant disease. Overall results were also com- tal voice changes, the severity of which varies according pared with those found in previous series identified to the voice demands of the patient. Variations in its ana- through a 50-year literature review. tomic patterns and in the rates of identification re- ported in the literature have discouraged thyroid sur- Results: The 3 anatomic variations of the distal aspect geons from routine exploration and identification of this of the EBSLN as it enters the cricothyroid were encoun- nerve. Inconsistent with the surgical principle of pres- tered and are described. The total identification rate over ervation of critical structures through identification, mod- the 20-year period was 900 (85.1%) of 1057 nerves. Op- ern-day thyroidectomy surgeons still avoid the EBSLN erations performed for benign disease were associated rather than identifying and preserving it. with higher identification rates (599 [86.1%] of 696) as opposed to those performed for malignant disease Objectives: To describe the anatomic variations of the (301 [83.4%] of 361). Operations performed in recent EBSLN, particularly at the junction of the inferior con- years have a higher identification rate (over 90%). strictor and cricothyroid muscles; to propose a system- atic approach to identification and preservation of this Conclusions: Understanding the 3 anatomic variations nerve; and to define the identification rate of this nerve of the distal portion of the EBSLN and its relation to the during thyroidectomy. -
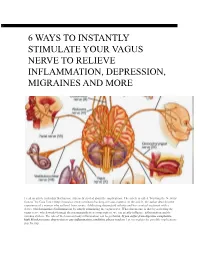
6 Ways to Instantly Stimulate Your Vagus Nerve to Relieve Inflammation, Depression, Migraines and More
O 6 WAYS TO INSTANTLY STIMULATE YOUR VAGUS NERVE TO RELIEVE INFLAMMATION, DEPRESSION, MIGRAINES AND MORE I read an article yesterday that has me extremely excited about the implications. The article is called “Hacking the Nervous System” by Gaia Vince (http://mosaicscience.com/story/hacking-nervous-system). In the article, the author describes the experience of a woman who suffered from severe, debilitating rheumatoid arthritis and her eventual treatment with a device which minimized inflammation by simply stimulating the vagus nerve. What this means, is that by activating the vagus nerve which works through the parasympathetic nervous system, we can greatly influence inflammation and the immune system. The role of the brain on body inflammation can be profound. If you suffer from digestive complaints, high blood pressure, depression or any inflammatory condition, please read on. Let me explain the possible implications step by step. What is the vagus nerve? First of all, the vagus nerve is the longest nerve in the body which originates in the brain as cranial nerve ten, travels down the from go the neck and then passes around the digestive system, liver, spleen, pancreas, heart and lungs. This nerve is a major player in the parasympathetic nervous system, which is the ‘rest and digest’ part (opposite to the sympathetic nervous system which is ‘fight of flight’). Vagal tone The tone of the vagus nerve is key to activating the parasympathetic nervous system. Vagal tone is measured by tracking your heart-rate alongside your breathing rate. Your heart-rate speeds up a little when your breathe in, and slows down a little when you breathe out. -

Neuroanatomy Crash Course
Neuroanatomy Crash Course Jens Vikse ∙ Bendik Myhre ∙ Danielle Mellis Nilsson ∙ Karoline Hanevik Illustrated by: Peder Olai Skjeflo Holman Second edition October 2015 The autonomic nervous system ● Division of the autonomic nervous system …………....……………………………..………….…………... 2 ● Effects of parasympathetic and sympathetic stimulation…………………………...……...……………….. 2 ● Parasympathetic ganglia ……………………………………………………………...…………....………….. 4 Cranial nerves ● Cranial nerve reflexes ………………………………………………………………….…………..…………... 7 ● Olfactory nerve (CN I) ………………………………………………………………….…………..…………... 7 ● Optic nerve (CN II) ……………………………………………………………………..…………...………….. 7 ● Pupillary light reflex …………………………………………………………………….…………...………….. 7 ● Visual field defects ……………………………………………...................................…………..………….. 8 ● Eye dynamics …………………………………………………………………………...…………...………….. 8 ● Oculomotor nerve (CN III) ……………………………………………………………...…………..………….. 9 ● Trochlear nerve (CN IV) ………………………………………………………………..…………..………….. 9 ● Trigeminal nerve (CN V) ……………………………………………………................…………..………….. 9 ● Abducens nerve (CN VI) ………………………………………………………………..…………..………….. 9 ● Facial nerve (CN VII) …………………………………………………………………...…………..………….. 10 ● Vestibulocochlear nerve (CN VIII) …………………………………………………….…………...…………. 10 ● Glossopharyngeal nerve (CN IX) …………………………………………….……….…………...………….. 10 ● Vagus nerve (CN X) …………………………………………………………..………..…………...………….. 10 ● Accessory nerve (CN XI) ……………………………………………………...………..…………..………….. 11 ● Hypoglossal nerve (CN XII) …………………………………………………..………..…………...…………. -

Cranial Nerve Palsy
Cranial Nerve Palsy What is a cranial nerve? Cranial nerves are nerves that lead directly from the brain to parts of our head, face, and trunk. There are 12 pairs of cranial nerves and some are involved in special senses (sight, smell, hearing, taste, feeling) while others control muscles and glands. Which cranial nerves pertain to the eyes? The second cranial nerve is called the optic nerve. It sends visual information from the eye to the brain. The third cranial nerve is called the oculomotor nerve. It is involved with eye movement, eyelid movement, and the function of the pupil and lens inside the eye. The fourth cranial nerve is called the trochlear nerve and the sixth cranial nerve is called the abducens nerve. They each innervate an eye muscle involved in eye movement. The fifth cranial nerve is called the trigeminal nerve. It provides facial touch sensation (including sensation on the eye). What is a cranial nerve palsy? A palsy is a lack of function of a nerve. A cranial nerve palsy may cause a complete or partial weakness or paralysis of the areas served by the affected nerve. In the case of a cranial nerve that has multiple functions (such as the oculomotor nerve), it is possible for a palsy to affect all of the various functions or only some of the functions of that nerve. What are some causes of a cranial nerve palsy? A cranial nerve palsy can occur due to a variety of causes. It can be congenital (present at birth), traumatic, or due to blood vessel disease (hypertension, diabetes, strokes, aneurysms, etc). -

Questions and Answers About Vagus Nerve Stimulation by Jerry Shih, M.D. 1. WHAT IS VAGUS NERVE STIMULATION? Therapeutic Vagus Ne
Questions and Answers About Vagus Nerve Stimulation By Jerry Shih, M.D. 1. WHAT IS VAGUS NERVE STIMULATION? Therapeutic vagus nerve stimulation (VNS) is chronic, intermittent electrical stimulation of the mid-cervical segment of the left vagus nerve. The stimulation occurs automatically at set intervals, during waking and sleep. The electrical pulses are generated by a pacemaker-like device that is implanted below the clavicle and are delivered by a lead wire that is coiled around the vagus nerve. 2. WHAT IS THE EVIDENCE THAT VAGUS NERVE STIMULATION IS EFFECTIVE IN EPILEPSY? The empirical evidence of antiepileptic efficacy arose sequentially from l) experiments in animal models of epilepsy; 2) anecdotal reports and small case series ofearly human trials, and 3) two prospec-tive, double-blind, controlled studies in large groups of patients with complex partial and secondarily generalized seizures. 3. HOW DOES VAGUS NERVE STIMULATION CONTROL SEIZURES? The mechanisms by which therapeutic VNS reduces seizure activity in humans and in experimental models of epilepsy are unknown. 4. WHEN SHOULD ONE CONSIDER VAGUS NERVE STIMULATION? Medically refractory complex partial and secondarily generalized seizures have been efficaciously treated with adjunctive VNS in the large, randomized studies. Children may benefit considerably from VNS, but large-scale, randomized, controlled studies have not been completed in young children. Thus, any adolescent or adult whose complex partial or secondarily generalized seizures have not been controlled with the appropriate first- and second -line antiepileptic drugs may be a good candidate for VNS. The FDA has specifically approved VNS with the Cyberonics device for adjunctive therapy of refractory partial-onset seizures in persons l2 years of age. -

Current Neurosurgical Management of Glossopharyngeal Neuralgia and Technical Nuances for Microvascular Decompression Surgery
Neurosurg Focus 34 (3):E8, 2013 ©AANS, 2013 Current neurosurgical management of glossopharyngeal neuralgia and technical nuances for microvascular decompression surgery ROBERTO REY-DIOS, M.D.,1 AND AARON A. COHEN-GADOL, M.D., M.SC.2 1Department of Neurosurgery, University of Mississippi Medical Center, Jackson, Mississippi; 2Goodman Campbell Brain and Spine, Indiana University Department of Neurological Surgery, Indianapolis, Indiana Glossopharyngeal neuralgia (GPN) is an uncommon facial pain syndrome often misdiagnosed as trigeminal neuralgia. The rarity of this condition and its overlap with other cranial nerve hyperactivity syndromes often leads to a significant delay in diagnosis. The surgical procedures with the highest rates of pain relief for GPN are rhizotomy and microvascular decompression (MVD) of cranial nerves IX and X. Neurovascular conflict at the level of the root exit zone of these cranial nerves is believed to be the cause of this pain syndrome in most cases. Vagus nerve rhizotomy is usually reserved for cases in which vascular conflict is not evident. A review of the literature reveals that although the addition of cranial nerve X rhizotomy may improve the chances of long-term pain control, this maneuver also increases the risk of permanent dysphagia and vocal cord paralysis. The risks of this procedure have to be carefully weighed against its benefits. Based on the authors’ experience, careful patient selection with a thorough exploratory operation most often leads to identification of the site of vascular conflict, obviating the need for cranial nerve X rhizotomy. (http://thejns.org/doi/abs/10.3171/2012.12.FOCUS12391) KEY WORDS • glossopharyngeal neuralgia • microvascular decompression • vagus nerve • rhizotomy • cranial nerve LOSSOPHARYNGEAL neuralgia, or vagoglossopharyn impairment can be found in the distribution of the above geal neuralgia, is a cranial nerve hyperactivity nerves due to structural lesions.20 This classification does pain syndrome leading to severe, transient, sharp not take into consideration associated syncopal events. -

Neurophysiological Aspects of the Trigeminal Sensory System: an Update
Rev. Neurosci. 2018; 29(2): 115–123 Frederic Van der Cruyssen* and Constantinus Politis Neurophysiological aspects of the trigeminal sensory system: an update https://doi.org/10.1515/revneuro-2017-0044 Keywords: infraorbital; mandibular; neurophysiology; Received June 21, 2017; accepted July 20, 2017; previously published ophthalmic nerve; oral somatosensory functioning; online November 8, 2017 trigeminal sensory system. Abstract: The trigeminal system is one of the most complex cranial nerve systems of the human body. Research on it has vastly grown in recent years and concentrated more and more on molecular mechanisms and pathophysiology, Introduction but thorough reviews on this topic are lacking, certainly Knowledge about physiological aspects of the trigeminal on the normal physiology of the trigeminal sensory system. system today is largely based on animal models (Akerman Here we review the current literature on neurophysiology and Goadsby, 2015; Herta et al., 2017), cadaver studies of the trigeminal nerve from peripheral receptors up to its (Ezure et al., 2001; Williams et al., 2003) or extrapola- central projections toward the somatosensory cortex. We tions from peripheral nerve functioning. Human studies focus on the most recent scientific discoveries and describe are frequently limited to pathophysiology and lack proper historical relevant research to substantiate further. One study designs (Tanaka and Zhao, 2016; Goadsby et al., chapter on new insights of the pathophysiology of pain 2017). Neurophysiological research in this area is difficult at the level of the trigeminal system is added. A database due to the invasive character of most neurophysiological search of Medline, Embase and Cochrane was conducted tests, the small caliber of fibers, high density of receptors, with the search terms ‘animal study’, ‘neurophysiology’, cross-connections between different cranial nerves, dif- ‘trigeminal’, ‘oral’ and ‘sensory’. -
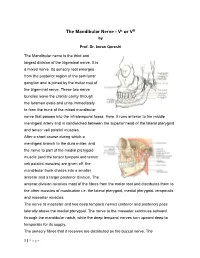
The Mandibular Nerve - Vc Or VIII by Prof
The Mandibular Nerve - Vc or VIII by Prof. Dr. Imran Qureshi The Mandibular nerve is the third and largest division of the trigeminal nerve. It is a mixed nerve. Its sensory root emerges from the posterior region of the semilunar ganglion and is joined by the motor root of the trigeminal nerve. These two nerve bundles leave the cranial cavity through the foramen ovale and unite immediately to form the trunk of the mixed mandibular nerve that passes into the infratemporal fossa. Here, it runs anterior to the middle meningeal artery and is sandwiched between the superior head of the lateral pterygoid and tensor veli palatini muscles. After a short course during which a meningeal branch to the dura mater, and the nerve to part of the medial pterygoid muscle (and the tensor tympani and tensor veli palatini muscles) are given off, the mandibular trunk divides into a smaller anterior and a larger posterior division. The anterior division receives most of the fibres from the motor root and distributes them to the other muscles of mastication i.e. the lateral pterygoid, medial pterygoid, temporalis and masseter muscles. The nerve to masseter and two deep temporal nerves (anterior and posterior) pass laterally above the medial pterygoid. The nerve to the masseter continues outward through the mandibular notch, while the deep temporal nerves turn upward deep to temporalis for its supply. The sensory fibres that it receives are distributed as the buccal nerve. The 1 | P a g e buccal nerve passes between the medial and lateral pterygoids and passes downward and forward to emerge from under cover of the masseter with the buccal artery. -

Morphometry and Morphology of Foramen Petrosum in Indian Population
Basic Sciences of Medicine 2020, 9(1): 8-9 DOI: 10.5923/j.medicine.20200901.02 Morphometry and Morphology of Foramen Petrosum in Indian Population Rajani Singh1,*, Nand Kishore Gupta1, Raj Kumar2 1Department of Anatomy, Uttar Pradesh University of Medical Sciences Saifai 206130 Etawah UP India 2Department of Neurosugery Uttar Pradesh University of Medical Sciences Saifai 206130 Etawah UP India Abstract Greater wing of sphenoid contains three constant foramina, Foramen ovale, foramen rotundum and foramen spinosum. The presence of foramen Vesalius and foramen petrosum are inconsistent. Normally foramen ovale transmits mandibular nerve, accessory meningeal artery, lesser petrosal nerve and emissary vein. When foramen petrosum is present, lesser petrosal nerve passes through petrosal foramen instead of foramen ovale. Lesser petrosal nerve distribute postganglionic fibers from otic ganglion to parotid gland. In absence of knowledge of petrosal foramen transmitting lesser petrosal nerve, the clinician may damage the nerve during skull base surgery creating complications like hyperemia of face and profuse salivation from the parotid gland (following atropine administration), lacrimation (crocodile tears syndrome) and mucus nasal secretion. Considering clinical implications associated with petrosal foramen, the study was carried out. The aim of the study is to determine the prevalence of petrosal foramen in Indian Population and to bring out associated clinical significance. The study was conducted in the department of Anatomy UPUMS Saifai Etawah Indian. 30 half skulls were observed for the presence of petrosal foramina and morphometry was also done. Literature search was carried out, our findings were compared with previous work and associated clinical implications were bought out. Keywords Petrosal foramen, Lesser petrosal nerve, Foramen ovale patients. -

Cranial Nerves - Iii (Cn Ix, X, Xi & Xii)
CRANIAL NERVES - III (CN IX, X, XI & XII) DR. SANGEETA KOTRANNAVAR ASSISTANT PROFESSOR DEPT. OF ANATOMY USM KLE IMP BELAGAVI OBJECTIVES • Describe the functional component, nuclei of origin, course, distribution and functional significance of cranial nerves IX, X, XI and XII • Describe the applied anatomy of cranial nerves IX, X, XI and XII overview Relationship of the last four cranial nerves at the base of the skull The last four cranial nerves arise from medulla & leave the skull close together, the glossopharyngeal, vagus & accessory through jugular foramen, and the hypoglossal nerve through the hypoglossal canal Functional components OF CN Afferent Efferent General General somatic afferent fibers General somatic efferent fibers Somatic (GSA): transmit exteroceptive & (GSE): innervate skeletal muscles proprioceptive impulses from skin of somatic origin & muscles to somatic sensory nuclei General General visceral afferent General visceral efferent(GVE): transmit visceral fibers (GVA): transmit motor impulses from general visceral interoceptive impulses motor nuclei &relayed in parasympathetic from the viscera to the ganglions. Postganglionic fibers supply visceral sensory nuclei glands, smooth muscles, vessels & viscera Special Special somatic afferent fibers (SSA): ------------ Somatic transmit sensory impulses from special sense organs eye , nose & ear to brain Special Special visceral afferent fibers Special visceral efferent fibers (SVE): visceral (SVA): transmit sensory transmit motor impulses from the impulses from special sense brain to skeletal muscles derived from taste (tounge) to the brain pharyngeal arches : include muscles of mastication, face, pharynx & larynx Cranial Nerve Nuclei in Brainstem: Schematic picture Functional components OF CN GLOSSOPHARYNGEAL NERVE • Glossopharyngeal nerve is the 9th cranial nerve. • It is a mixed nerve, i.e., composed of both the motor and sensory fibres, but predominantly it is sensory. -

ANATOMY of EAR Basic Ear Anatomy
ANATOMY OF EAR Basic Ear Anatomy • Expected outcomes • To understand the hearing mechanism • To be able to identify the structures of the ear Development of Ear 1. Pinna develops from 1st & 2nd Branchial arch (Hillocks of His). Starts at 6 Weeks & is complete by 20 weeks. 2. E.A.M. develops from dorsal end of 1st branchial arch starting at 6-8 weeks and is complete by 28 weeks. 3. Middle Ear development —Malleus & Incus develop between 6-8 weeks from 1st & 2nd branchial arch. Branchial arches & Development of Ear Dev. contd---- • T.M at 28 weeks from all 3 germinal layers . • Foot plate of stapes develops from otic capsule b/w 6- 8 weeks. • Inner ear develops from otic capsule starting at 5 weeks & is complete by 25 weeks. • Development of external/middle/inner ear is independent of each other. Development of ear External Ear • It consists of - Pinna and External auditory meatus. Pinna • It is made up of fibro elastic cartilage covered by skin and connected to the surrounding parts by ligaments and muscles. • Various landmarks on the pinna are helix, antihelix, lobule, tragus, concha, scaphoid fossa and triangular fossa • Pinna has two surfaces i.e. medial or cranial surface and a lateral surface . • Cymba concha lies between crus helix and crus antihelix. It is an important landmark for mastoid antrum. Anatomy of external ear • Landmarks of pinna Anatomy of external ear • Bat-Ear is the most common congenital anomaly of pinna in which antihelix has not developed and excessive conchal cartilage is present. • Corrections of Pinna defects are done at 6 years of age. -
Cranial Nerve VIII
Cranial Nerve VIII Color Code Important (The Vestibulo-Cochlear Nerve) Doctors Notes Notes/Extra explanation Please view our Editing File before studying this lecture to check for any changes. Objectives At the end of the lecture, the students should be able to: ✓ List the nuclei related to vestibular and cochlear nerves in the brain stem. ✓ Describe the type and site of each nucleus. ✓ Describe the vestibular pathways and its main connections. ✓ Describe the auditory pathway and its main connections. Due to the difference of arrangement of the lecture between the girls and boys slides we will stick to the girls slides then summarize the pathway according to the boys slides. Ponto-medullary Sulcus (cerebello- pontine angle) Recall: both cranial nerves 8 and 7 emerge from the ventral surface of the brainstem at the ponto- medullary sulcus (cerebello-pontine angle) Brain – Ventral Surface Vestibulo-Cochlear (VIII) 8th Cranial Nerve o Type: Special sensory (SSA) o Conveys impulses from inner ear to nervous system. o Components: • Vestibular part: conveys impulses associated with body posture ,balance and coordination of head & eye movements. • Cochlear part: conveys impulses associated with hearing. o Vestibular & cochlear parts leave the ventral surface* of brain stem through the pontomedullary sulcus ‘at cerebellopontine angle*’ (lateral to facial nerve), run laterally in posterior cranial fossa and enter the internal acoustic meatus along with 7th (facial) nerve. *see the previous slide Auditory Pathway Only on the girls’ slides 04:14 Characteristics: o It is a multisynaptic pathway o There are several locations between medulla and the thalamus where axons may synapse and not all the fibers behave in the same manner.