Neurotization from Two Medial Pectoral Nerves to Musculocutaneous Nerve in a Pediatric Brachial Plexus Injury
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Anatomical Variants of the Musculocutaneous Nerve- Report of Two Cases
Open Access CRIMSON PUBLISHERS C Wings to the Research Research in Anatomy ISSN: 2577-1922 Case Report Anatomical Variants of the Musculocutaneous Nerve- Report of Two Cases Fernando Martinez1,2 and Guzmán Ripoll1* 1Anatomy Department, Facultad de Medicina Universidad Claeh, Uruguay 2Neurosurgery Department, Universidad de la República, Uruguay *Corresponding author: Guzmán Ripoll, AnatomyDepartment, Facultad de Medicina Universidad Claeh, Maldonado, Uruguay, Email: Submission: February 22, 2018; Published: April 19, 2018 Abstract Introduction: The muscle-cutaneous nerve (MCN) is a mixed nerve, which is mainly responsible for shoulder flexion, elbow flexion and supinationMaterial of theand hand. method: The anatomical variations in this nerve are relatively frequent, fact with clinical and surgical implications. Results: Two variants were A retrospective found in the review 20 cases of 20studied patients (10% operated of the cases): on with anastomosis the Oberlin betweentechnique MCN was and made. median nerve, and absence of the MCN.Discussion: MCN variants are frequently described by the different authors. This has an embryological and phylogenetic explanation: the lateralConclusion: and medial cords form the flexor plane of the muscles of the upper limb. We present 2 cases: an unusual one of median nerve-MCN, and another absence of it. We emphasize that the knowledge of these variants have clinical, surgical and neuro-physiological applications. Introduction The musclecutaneous nerve (MCN) is a mixed nerve, which from basically the use of fascicles of the median nerve to reinforce the ulnar nerve (Figure 1). The modifications of this technique are the motor point of view is mainly responsible for shoulder flexion, brachial plexus injuries with involvement of the upper trunk (C5- the muscles that innervate: coracobrachial, biceps brachialis and anterior brachial muscle (Figure 2). -

Anatomical Variations of the Brachial Plexus Terminal Branches in Ethiopian Cadavers
ORIGINAL COMMUNICATION Anatomy Journal of Africa. 2017. Vol 6 (1): 896 – 905. ANATOMICAL VARIATIONS OF THE BRACHIAL PLEXUS TERMINAL BRANCHES IN ETHIOPIAN CADAVERS Edengenet Guday Demis*, Asegedeche Bekele* Corresponding Author: Edengenet Guday Demis, 196, University of Gondar, Gondar, Ethiopia. Email: [email protected] ABSTRACT Anatomical variations are clinically significant, but many are inadequately described or quantified. Variations in anatomy of the brachial plexus are important to surgeons and anesthesiologists performing surgical procedures in the neck, axilla and upper limb regions. It is also important for radiologists who interpret plain and computerized imaging and anatomists to teach anatomy. This study aimed to describe the anatomical variations of the terminal branches of brachial plexus on 20 Ethiopian cadavers. The cadavers were examined bilaterally for the terminal branches of brachial plexus. From the 40 sides studied for the terminal branches of the brachial plexus; 28 sides were found without variation, 10 sides were found with median nerve variation, 2 sides were found with musculocutaneous nerve variation and 2 sides were found with axillary nerve variation. We conclude that variation in the median nerve was more common than variations in other terminal branches. Key words: INTRODUCTION The brachial plexus is usually formed by the may occur (Moore and Dalley, 1992, Standring fusion of the anterior primary rami of the C5-8 et al., 2005). and T1 spinal nerves. It supplies the muscles of the back and the upper limb. The C5 and C6 fuse Most nerves in the upper limb arise from the to form the upper trunk, the C7 continues as the brachial plexus; it begins in the neck and extends middle trunk and the C8 and T1 join to form the into the axilla. -

Anastomotic Branch from the Median Nerve to the Musculocutaneous Nerve: a Case Report
Case Report www.anatomy.org.tr Recieved: February 10, 2008; Accepted: April 22, 2008; Published online: October 31, 2008 doi:10.2399/ana.08.063 Anastomotic branch from the median nerve to the musculocutaneous nerve: a case report Feray Güleç Uyaro¤lu1, Gülgün Kayal›o¤lu2, Mete Ertürk2 1Department of Neurology, Ege University Faculty of Medicine, Izmir, Turkey 2Department of Anatomy, Ege University Faculty of Medicine, Izmir, Turkey Abstract Anomalies of the brachial plexus and its terminal branches are not uncommon. Communicating branch arising from the mus- culocutaneous nerve to the median nerve is a frequent variation, whereas the presence of an anastomotic branch arising from the median nerve and joining the musculocutaneous nerve is very rare. During routine dissection of cadaver upper limbs, we observed an anastomotic branch arising from the median nerve running distally to join with the branches of the musculocutaneous nerve in a left upper extremity. The anastomotic branch originated from the median nerve 11.23 cm prox- imal to the interepicondylar line. After running distally and coursing between the biceps brachii and the brachialis muscles, this anastomotic branch communicated with two branches of the musculocutaneous nerve separately. The presence of the communicating branches between these nerves should be considered during surgical interventions and clinical investigations of the arm. Key words: anatomy; brachial plexus; communicating branch; upper limb; variation Anatomy 2008; 2: 63-66, © 2008 TSACA Introduction neous nerve (C5, C6, and C7) connects with the median nerve in the arm.2,3 The musculocutaneous nerve is the Variations of the brachial plexus and its terminal continuation of the lateral cord of the brachial plexus. -
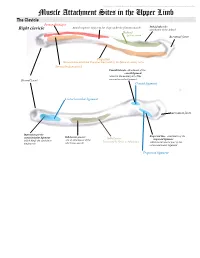
Muscle Attachment Sites in the Upper Limb
This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. Muscle Attachment Sites in the Upper Limb The Clavicle Pectoralis major Smooth superior surface of the shaft, under the platysma muscle Deltoid tubercle: Right clavicle attachment of the deltoid Deltoid Axillary nerve Acromial facet Trapezius Sternocleidomastoid and Trapezius innervated by the Spinal Accessory nerve Sternocleidomastoid Conoid tubercle, attachment of the conoid ligament which is the medial part of the Sternal facet coracoclavicular ligament Conoid ligament Costoclavicular ligament Acromial facet Impression for the Trapezoid line, attachment of the costoclavicular ligament Subclavian groove: Subclavius trapezoid ligament which binds the clavicle to site of attachment of the Innervated by Nerve to Subclavius which is the lateral part of the the first rib subclavius muscle coracoclavicular ligament Trapezoid ligament This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. The Scapula Trapezius Right scapula: posterior Levator scapulae Supraspinatus Deltoid Deltoid and Teres Minor are innervated by the Axillary nerve Rhomboid minor Levator Scapulae, Rhomboid minor and Rhomboid Major are innervated by the Dorsal Scapular Nerve Supraspinatus and Infraspinatus innervated by the Suprascapular nerve Infraspinatus Long head of triceps Rhomboid major Teres Minor Teres Major Teres Major -
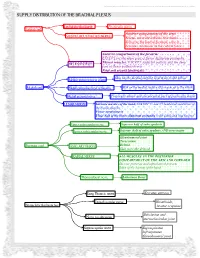
Supply Distribution of the Brachial Plexus
This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. SUPPLY DISTRIBUTION OF THE BRACHIAL PLEXUS Lateral pectoral nerve Pectoralis major Lateral cord Anterior compartment of the arm: MUSCULOCUTANEOUS NERVE Biceps, coracobrachialis, brachialis Skin over the lateral forearm, once it becomes cutaneous in the cubital fossa Anterior compartment of the forearm: EXCEPT for the ulnar part of flexor digitorum profundis MEDIAN NERVE Thenar muscles: EXCEPT adductor pollicis and the deep part of flexor pollicis brevis First and second lumbricals Skin on the medial surface of arm up to the elbow MedialLateral cutaneous cord: nerve of arm lateral pectoral nerve Medial cord Skin on the medial surface of forearm up to the elbow Medial cutaneous MUSCULOCUTANEOUS nerve of forearm NERVE lateral root of MEDIAN NERVE Medial pectoral nerve Pectoralis minor and sternocostal part of pectoralis major o Medial cord forms ULNAR NERVE Intrinsic muscles of the hand, EXCEPT 1st and 2nd lumbricals and three of the thenar muscles Flexor carpi ulnaris Ulnar half of the flexor digitorum profundis to the pinky and ring fingers Upper subscapular nerve Superior half of subscapularis medial root of MEDIAN NERVE Lower subscapular nerve Inferior half of subscapularis AND teres major medial pectoral nerve medial cutaneous nerveGlenohumeral of arm joint Teres minor medial cutaneous nerve of forearm Posterior cord AXILLARY NERVE Deltoid ULNAR NERVE Skin over the deltoid RADIAL NERVE ALL MUSCLES IN THE POSTERIOR COMPARTMENT OF THE ARM AND FOREARM Ski over posterior and inferolateral forearm Some of the dorsum of the hand o o Thoracodorsal nerve Latissimus Dorsi o o Posterior cord forms: Long Thoracic nerve Serratus anterior Dorsal scapular nerve Rhomboids; Supraclavicular branches levator scapulae Subclavius and Nerve to subclavius sternoclavicular joint Suprascapular nerve Supraspinatus Infraspinatus Glenohumeral joint. -

Pectoral Region and Axilla Doctors Notes Notes/Extra Explanation Editing File Objectives
Color Code Important Pectoral Region and Axilla Doctors Notes Notes/Extra explanation Editing File Objectives By the end of the lecture the students should be able to : Identify and describe the muscles of the pectoral region. I. Pectoralis major. II. Pectoralis minor. III. Subclavius. IV. Serratus anterior. Describe and demonstrate the boundaries and contents of the axilla. Describe the formation of the brachial plexus and its branches. The movements of the upper limb Note: differentiate between the different regions Flexion & extension of Flexion & extension of Flexion & extension of wrist = hand elbow = forearm shoulder = arm = humerus I. Pectoralis Major Origin 2 heads Clavicular head: From Medial ½ of the front of the clavicle. Sternocostal head: From; Sternum. Upper 6 costal cartilages. Aponeurosis of the external oblique muscle. Insertion Lateral lip of bicipital groove (humerus)* Costal cartilage (hyaline Nerve Supply Medial & lateral pectoral nerves. cartilage that connects the ribs to the sternum) Action Adduction and medial rotation of the arm. Recall what we took in foundation: Only the clavicular head helps in flexion of arm Muscles are attached to bones / (shoulder). ligaments / cartilage by 1) tendons * 3 muscles are attached at the bicipital groove: 2) aponeurosis Latissimus dorsi, pectoral major, teres major 3) raphe Extra Extra picture for understanding II. Pectoralis Minor Origin From 3rd ,4th, & 5th ribs close to their costal cartilages. Insertion Coracoid process (scapula)* 3 Nerve Supply Medial pectoral nerve. 4 Action 1. Depression of the shoulder. 5 2. Draw the ribs upward and outwards during deep inspiration. *Don’t confuse the coracoid process on the scapula with the coronoid process on the ulna Extra III. -

A Comprehensive Review of Anatomy and Regional Anesthesia Techniques of Clavicle Surgeries
vv ISSN: 2641-3116 DOI: https://dx.doi.org/10.17352/ojor CLINICAL GROUP Received: 31 March, 2021 Research Article Accepted: 07 April, 2021 Published: 10 April, 2021 *Corresponding author: Dr. Kartik Sonawane, Uncovering secrets of the Junior Consultant, Department of Anesthesiol- ogy, Ganga Medical Centre & Hospitals, Pvt. Ltd. Coimbatore, Tamil Nadu, India, E-mail: beauty bone: A comprehensive Keywords: Clavicle fractures; Floating shoulder sur- gery; Clavicle surgery; Clavicle anesthesia; Procedure review of anatomy and specific anesthesia; Clavicular block regional anesthesia techniques https://www.peertechzpublications.com of clavicle surgeries Kartik Sonawane1*, Hrudini Dixit2, J.Balavenkatasubramanian3 and Palanichamy Gurumoorthi4 1Junior Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 2Fellow in Regional Anesthesia, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 3Senior Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 4Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India Abstract The clavicle is the most frequently fractured bone in humans. General anesthesia with or without Regional Anesthesia (RA) is most frequently used for clavicle surgeries due to its complex innervation. Many RA techniques, alone or in combination, have been used for clavicle surgeries. These include interscalene block, cervical plexus (superficial and deep) blocks, SCUT (supraclavicular nerve + selective upper trunk) block, and pectoral nerve blocks (PEC I and PEC II). The clavipectoral fascial plane block is also a safe and simple option and replaces most other RA techniques due to its lack of side effects like phrenic nerve palsy or motor block of the upper limb. -

Electrodiagnosis of Brachial Plexopathies and Proximal Upper Extremity Neuropathies
Electrodiagnosis of Brachial Plexopathies and Proximal Upper Extremity Neuropathies Zachary Simmons, MD* KEYWORDS Brachial plexus Brachial plexopathy Axillary nerve Musculocutaneous nerve Suprascapular nerve Nerve conduction studies Electromyography KEY POINTS The brachial plexus provides all motor and sensory innervation of the upper extremity. The plexus is usually derived from the C5 through T1 anterior primary rami, which divide in various ways to form the upper, middle, and lower trunks; the lateral, posterior, and medial cords; and multiple terminal branches. Traction is the most common cause of brachial plexopathy, although compression, lacer- ations, ischemia, neoplasms, radiation, thoracic outlet syndrome, and neuralgic amyotro- phy may all produce brachial plexus lesions. Upper extremity mononeuropathies affecting the musculocutaneous, axillary, and supra- scapular motor nerves and the medial and lateral antebrachial cutaneous sensory nerves often occur in the context of more widespread brachial plexus damage, often from trauma or neuralgic amyotrophy but may occur in isolation. Extensive electrodiagnostic testing often is needed to properly localize lesions of the brachial plexus, frequently requiring testing of sensory nerves, which are not commonly used in the assessment of other types of lesions. INTRODUCTION Few anatomic structures are as daunting to medical students, residents, and prac- ticing physicians as the brachial plexus. Yet, detailed understanding of brachial plexus anatomy is central to electrodiagnosis because of the plexus’ role in supplying all motor and sensory innervation of the upper extremity and shoulder girdle. There also are several proximal upper extremity nerves, derived from the brachial plexus, Conflicts of Interest: None. Neuromuscular Program and ALS Center, Penn State Hershey Medical Center, Penn State College of Medicine, PA, USA * Department of Neurology, Penn State Hershey Medical Center, EC 037 30 Hope Drive, PO Box 859, Hershey, PA 17033. -

Neuroanatomy for Nerve Conduction Studies
Neuroanatomy for Nerve Conduction Studies Kimberley Butler, R.NCS.T, CNIM, R. EP T. Jerry Morris, BS, MS, R.NCS.T. Kevin R. Scott, MD, MA Zach Simmons, MD AANEM 57th Annual Meeting Québec City, Québec, Canada Copyright © October 2010 American Association of Neuromuscular & Electrodiagnostic Medicine 2621 Superior Drive NW Rochester, MN 55901 Printed by Johnson Printing Company, Inc. AANEM Course Neuroanatomy for Nerve Conduction Studies iii Neuroanatomy for Nerve Conduction Studies Contents CME Information iv Faculty v The Spinal Accessory Nerve and the Less Commonly Studied Nerves of the Limbs 1 Zachary Simmons, MD Ulnar and Radial Nerves 13 Kevin R. Scott, MD The Tibial and the Common Peroneal Nerves 21 Kimberley B. Butler, R.NCS.T., R. EP T., CNIM Median Nerves and Nerves of the Face 27 Jerry Morris, MS, R.NCS.T. iv Course Description This course is designed to provide an introduction to anatomy of the major nerves used for nerve conduction studies, with emphasis on the surface land- marks used for the performance of such studies. Location and pathophysiology of common lesions of these nerves are reviewed, and electrodiagnostic methods for localization are discussed. This course is designed to be useful for technologists, but also useful and informative for physicians who perform their own nerve conduction studies, or who supervise technologists in the performance of such studies and who perform needle EMG examinations.. Intended Audience This course is intended for Neurologists, Physiatrists, and others who practice neuromuscular, musculoskeletal, and electrodiagnostic medicine with the intent to improve the quality of medical care to patients with muscle and nerve disorders. -

Tricks and Techniques to Maximize Success with Nerve Transfers
IC12-L: Tricks and Techniques to Maximize Success with Nerve Transfers Moderator(s): Susan E. Mackinnon, MD Faculty: Christine B. Novak, PT, PhD and J. Megan Patterson, MD Session Handouts Friday, October 02, 2020 75TH VIRTUAL ANNUAL MEETING OF THE ASSH OCTOBER 1-3, 2020 822 West Washington Blvd Chicago, IL 60607 Phone: (312) 880-1900 Web: www.assh.org Email: [email protected] All property rights in the material presented, including common-law copyright, are expressly reserved to the speaker or the ASSH. No statement or presentation made is to be regarded as dedicated to the public domain. IC12 – Tricks and Techniques to Maximize Success with Nerve Transfers American Society for Surgery of the Hand Annual Meeting, October 2, 2020 Susan E. Mackinnon, MD, St. Louis, Missouri J. Megan M. Patterson, Chapel Hill, North Carolina Christine B. Novak, PT, PhD, Toronto, Ontario Andrew Yee, BS, St. Louis, Missouri Overview: Following complex nerve injury, motor and sensory recovery can be less than optimal. For high median, ulnar and radial nerve injuries, nerve transfers can provide a distal source of motor and/or sensory innervation closer to the target end organ allowing for faster recovery and improved outcome. This course will focus on techniques to maximize success with upper extremity motor and sensory nerve transfers. Classification of Nerve Injury: Degree of Injury Tinel’s Sign Recovery Rate of Surgical Procedure Present Recovery I Neurapraxia No Complete Up to 12 weeks None II Axonotmesis Yes Complete 1” per month None III Yes Varies * -

Case Report Isolated Musculocutaneous Nerve Palsy in A
Spinal Cord (1998) 36, 591 ± 592 1998 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/98 $12.00 http://www.stockton-press.co.uk/sc Case Report Isolated musculocutaneous nerve palsy in a spinal cord injury C Fattal1, J Weber2 and F Beuret-Blanquart1,2 1CRF Les Herbiers, BP 24-76231, Bois-Guillaume Cedex; 2Groupe de Recherche sur le Handicap de l'Appareil Locomoteur, CHU de Rouen 76, France Isolated musculocutaneous nerve palsy is rare. We report one case of a bilateral palsy of this nerve following a road accident which led to a complete thoracic level paraplegia. Keywords: musculocutaneous nerve palsy; spinal cord injury Introduction Musculocutaneous nerve injuries usually go together brachii was graded 0/5 on the right-hand side and 4/5 with other nervous injuries of the brachial plexus and on the left-hand side. The biceps tendon re¯exes were thus are rarely isolated. The lesions are frequently due absent. There was a decreased sensation to touch and to a direct trauma: surgical wound, bullet or knife pinprick on the radial side of both forearms. The rest wound, direct and violent impact while practising a of the neurological examination of the upper limbs was contact sport or crushing injury during working normal. activities.1 Several reports also mention indirect Forty-®ve days later, needle electromyographic trauma involving a violent extension of the forearm,2 sampling revealed a complete denervation in the right or involving strenuous exercises.3 A postural mechan- biceps brachii and partial denervation in the left biceps ism is also evoked in one case of isolated musculocu- brachii associated with a rich spontaneous activity taneous nerve injury following abdominal surgery.4 In such as ®brillations. -

SŁOWNIK ANATOMICZNY (ANGIELSKO–Łacinsłownik Anatomiczny (Angielsko-Łacińsko-Polski)´ SKO–POLSKI)
ANATOMY WORDS (ENGLISH–LATIN–POLISH) SŁOWNIK ANATOMICZNY (ANGIELSKO–ŁACINSłownik anatomiczny (angielsko-łacińsko-polski)´ SKO–POLSKI) English – Je˛zyk angielski Latin – Łacina Polish – Je˛zyk polski Arteries – Te˛tnice accessory obturator artery arteria obturatoria accessoria tętnica zasłonowa dodatkowa acetabular branch ramus acetabularis gałąź panewkowa anterior basal segmental artery arteria segmentalis basalis anterior pulmonis tętnica segmentowa podstawna przednia (dextri et sinistri) płuca (prawego i lewego) anterior cecal artery arteria caecalis anterior tętnica kątnicza przednia anterior cerebral artery arteria cerebri anterior tętnica przednia mózgu anterior choroidal artery arteria choroidea anterior tętnica naczyniówkowa przednia anterior ciliary arteries arteriae ciliares anteriores tętnice rzęskowe przednie anterior circumflex humeral artery arteria circumflexa humeri anterior tętnica okalająca ramię przednia anterior communicating artery arteria communicans anterior tętnica łącząca przednia anterior conjunctival artery arteria conjunctivalis anterior tętnica spojówkowa przednia anterior ethmoidal artery arteria ethmoidalis anterior tętnica sitowa przednia anterior inferior cerebellar artery arteria anterior inferior cerebelli tętnica dolna przednia móżdżku anterior interosseous artery arteria interossea anterior tętnica międzykostna przednia anterior labial branches of deep external rami labiales anteriores arteriae pudendae gałęzie wargowe przednie tętnicy sromowej pudendal artery externae profundae zewnętrznej głębokiej