Abnormal Positions of the Umbilical Cord
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Outcomes of Labour of Nuchal Cord
wjpmr, 2020,6(8), 07-15 SJIF Impact Factor: 5.922 Research Article Ansam et al. WORLD JOURNAL OF PHARMACEUTICAL World Journal of Pharmaceutical and Medical Research AND MEDICAL RESEARCH ISSN 2455-3301 www.wjpmr.com WJPMR OUTCOMES OF LABOUR OF NUCHAL CORD Dr. Ansam Layth Abdulhameed*1 and Dr. Rozhan Yassin Khalil2 1Specialist Obstetrics & Gynaecology, Mosul, Iraq. 2Consultant Obstetrics & Gynaecology, Sulaymania, Iraq. *Corresponding Author: Dr. Ansam Layth Abdulhameed Specialist Obstetrics & Gynaecology, Mosul, Iraq. Article Received on 26/05/2020 Article Revised on 16/06/2020 Article Accepted on 06/07/2020 ABSTRACT Background: The nuchal cord is described as the umbilical cord around the fetal neck. It is classified as simple or multiple, loose or tight with the compression of the fetal neck. The term nuchal cord represents an umbilical cord that passes 360 degrees around the fetal neck. Objective: To find out perinatal outcomes in cases of labour of babies with nuchal cord and compared with other cases without nuchal cord. Patient and Methods: The prospective case-control study was conducted in maternity teaching hospital centre in Sulaimani / Kurdistan Region of Iraq, from June 2018 to April 2019. Cases of study divided into two groups. First group comprised of women in whom nuchal cord was present at the time of delivery they were labelled as cases. Second group was a control group composed of women in whom nuchal cord was absent at the time of delivery. Results: This study included (200) patients, (100) women with nuchal cord in labour. (59%) of the cases of nuchal cord in age group (20-29) years, (40%) of them were primigravida, delivery modes for women with nuchal cord were mainly normal vaginal delivery (76%) and cesarean section (24%). -

Blood Volume in Newborn Piglets: Effects of Time of Natural Cord Rupture, Intra-Uterine Growth Retardation, Asphyxia, and Prostaglandin-Induced Prematurity
Pediatr. Res. 15: 53-57 (1981) asphyxia natural cord rupture blood volume prostaglandin F 2 intra-uterine growth retardation Blood Volume in Newborn Piglets: Effects of Time of Natural Cord Rupture, Intra-Uterine Growth Retardation, Asphyxia, and Prostaglandin-Induced Prematurity 137 OTWIN LINDERKAMP, , KLAUS BETKE, MONIKA GUNTNER, GIOK H. JAP, KLAUS P. RIEGEL, AND KURT WALSER Department of Pediatrics and Department of Veterinary Gynecology, University of Munich, Munich, Federal Republic of Germany Summary (27, 29, 32). Placental transfusion is accelerated by keeping the infant below the placenta (19, 27), by uterine contractions (32), Blood volume (BV), red cell mass (RCM; Cr-51) and plasma 125 and by respiration of the newborn (19). Placental transfusion is volume ( 1-labeled albumin) were measured in lOS piglets from prevented by holding the infant above the placenta (19, 27), by 28 Utters shortly after birth. Spontaneous cord rupture in healthy maternal hypotension ( 17), by tight nuchal cord ( 13), and by acute piglets occurred during delivery (n • 25) or within 190 sec of birth intrapartum asphyxia (5, 12, 13). Intra-uterine asphyxia results in (n • 82). Spontaneous and induced delay of cord rupture resulted prenatal transfusion to the fetus (12, 13, 33). In a time-dependent Increase in BV and RCM. BV (x ± S.D.) at It is to be assumed that blood volume in newborn mammals is birth was 72.5 ± 10.5 ml/kg (RCM, 23.6 ± 4.6 ml/kg) In the 25 similarly influenced by placental transfusion as in the human piglets with prenatal cord rupture and 110.5 ± 12.9 ml/kg (RCM, neonate. -

Is Nuchal Cord a Cause of Concern?
ISSN: 2638-1575 Madridge Journal of Women’s Health and Emancipation Research Article Open Access Is Nuchal Cord a cause of concern? Surekha Tayade1*, Jaya Kore1, Atul Tayade2, Neha Gangane1, Ketki Thool1 and Jyoti Borkar1 1Department of Obstetrics and Gynecology, Mahatma Gandhi Institute of Medical Sciences, Sewagram, India 2Department of Radiodiagnosis, Mahatma Gandhi Institute of Medical Sciences, Sewagram, India Article Info Abstract *Corresponding author: Context: The controversy about whether nuchal cord is a cause of concern and its Surekha Tayade adverse effect on perinatal outcome still persists. Authors express varying views and Professor Department of Obstetrics and Gynecology hence managing pregnancy with cord around the neck has its own concerns. Thus study Mahatma Gandhi Institute of Medical was carried out to find out the incidence of nuchal cord and its implications. Sciences Sewagram, 442102 Method: This was a prospective, cross sectional, comparative study carried out in the India Kasturba Hospital of MGIMS, Sewagram a rural medical tertiary care institute. All Tel: +917887519832 deliveries over a period of one year, were enrollled and studied for nuchal cord, tight or E-mail: [email protected] loose cord, number of turns, fetal heart rate irregulaties, pregnancy and perinatal Received: May 15, 2018 outcome. Accepted: June 19, 2018 Results: Total women with nuchal cord in labour room were 1116 (2.56%) of which Published: June 23, 2018 85.21 percent had single turn around the babies neck. Most of the babies ( 77.96 %) had Citation: Tayade S, Kore J, Tayade A, Gangane a loose nuchal cord, however 22.04 percent had a tight cord. -

Messages from the Placentae Across Multiple Species a 50 Years
Placenta 84 (2019) 14–27 Contents lists available at ScienceDirect Placenta journal homepage: www.elsevier.com/locate/placenta Messages from the placentae across multiple species: A 50 years exploration T Hiroaki Soma Saitama Medical University, Japan ARTICLE INFO ABSTRACT Keywords: This review explores eight aspects of placentation in multiple mammalian. Gestational trophoblastic disease 1) Specialities of gestational trophoblastic disease. SUA(Single umbilical artery) 2) Clinical significance of single umbilical artery (SUA) syndrome. DIC(Disseminated intravascular coagulation) in 3) Pulmonary trophoblast embolism in pregnant chinchillas and DIC in pregnant giant panda. giant panda 4) Genetics status and placental behaviors during Japanese serow and related antelopes. Placentation in Japanese serow 5) Specific living style and placentation of the Sloth and Proboscis monkey. Hydatidiform mole in chimpanzee Placentation in different living elephant 6) Similarities of placental structures between human and great apes. Manatee and hyrax 7) Similarities of placental forms in elephants, manatees and rock hyrax with different living styles. Specific placental findings of Himalayan people 8) Specialities of placental pathology in Himalayan mountain people. Conclusions: It was taught that every mammalian species held on placental forms applied to different environ- mental life for their infants, even though their gestational lengths were different. 1. Introduction of effective chemotherapeutic agents. In 1959, I was fortunate tore- ceive an invitation from Prof. Kurt Benirschke at the Boston Lying-in Last October, Scientific American published a special issue about a Hospital. Before that, I had written to Prof. Arthur T. Hertig, Chairman baby's first organ, the placenta [1]. It is full of surprises and amazing of Pathology, Harvard Medical School, asking to study human tropho- science. -

FASD Effects of Alcohol on a Fetus
EFFECTS OF ALCOHOL ON A FETUS “Of all the substances of abuse (including cocaine, heroin, and marijuana), alcohol produces by far the most serious neurobehavioral effects in the fetus.” —Institute of Medicine Report to Congress, 19961 Prenatal exposure to alcohol can damage a fetus at any time, causing problems that persist throughout the individual’s life. There is no known safe level of alcohol use in pregnancy. WHAT IS THE SCOPE OF THE PROBLEM? identified in virtually every part of the body, including the brain, face, eyes, ears, heart, kidneys, and bones. No Alcohol is one of the most dangerous teratogens, which single mechanism can account for all the problems that are substances that can damage a developing fetus.1 Every alcohol causes. Rather, alcohol sets in motion many time a pregnant woman has a drink, her unborn child processes at different sites in the developing fetus: has one, too. Alcohol, like carbon monoxide from cigarettes, passes easily through the placenta from the • Alcohol can trigger cell death in a number of ways, mother's bloodstream into her baby's blood (See Figure causing different parts of the fetus to develop abnormally. 1)—and puts her fetus at risk of having a fetal alcohol • Alcohol can disrupt the way nerve cells develop, travel spectrum disorder (FASD). The blood alcohol level to form different parts of the brain, and function. (BAC) of the fetus becomes equal to or greater than the blood alcohol level of the mother. Because the fetus • By constricting the blood vessels, alcohol interferes with cannot break down alcohol the way an adult can, its BAC blood flow in the placenta, which hinders the delivery 2 remains high for a longer period of time. -

The Effect of Nuchal Cord on Perinatal Mortality and Long-Term Offspring Morbidity
Journal of Perinatology https://doi.org/10.1038/s41372-019-0511-x ARTICLE The effect of nuchal cord on perinatal mortality and long-term offspring morbidity 1 1 2 1 Roee Masad ● Gil Gutvirtz ● Tamar Wainstock ● Eyal Sheiner Received: 28 May 2019 / Revised: 11 August 2019 / Accepted: 16 August 2019 © The Author(s), under exclusive licence to Springer Nature America, Inc. 2019 Abstract Objective To evaluate perinatal and long-term cardiovascular and respiratory morbidities of children born with nuchal cord. Study design A large population-based cohort analysis of singleton deliveries was conducted. Maternal and birth char- acteristics, as well as cardiovascular and respiratory morbidity incidence were evaluated. Kaplan–Meier survival curves were used to compare cumulative hospitalization incidence between groups. Cox regression models were used to control for possible confounders and follow-up length. Results 243,682 deliveries were included. Of them, 34,332 (14.1%) were diagnosed with nuchal cord. Perinatal mortality rate was comparable between groups (0.5 vs. 0.6%, p = 0.16). Kaplan–Meier survival curves demonstrated no significant p = p = 1234567890();,: 1234567890();,: differences in cumulative cardiovascular or respiratory morbidity incidence between groups (log rank 0.69 and 0.10, respectively). Cox regression models reaffirmed a comparable risk for hospitalization between groups (aHR = 0.99 (95% CI 0.85–1.14, p = 0.87) and aHR = 0.97 (95% CI 0.92–1.02, p = 0.28). Conclusions Nuchal cord is not associated with higher rate of perinatal mortality nor long-term cardiorespiratory morbidity. Introduction Controversy exists in the literature regarding the sig- nificance of nuchal cord. -

A Guide to Obstetrical Coding Production of This Document Is Made Possible by Financial Contributions from Health Canada and Provincial and Territorial Governments
ICD-10-CA | CCI A Guide to Obstetrical Coding Production of this document is made possible by financial contributions from Health Canada and provincial and territorial governments. The views expressed herein do not necessarily represent the views of Health Canada or any provincial or territorial government. Unless otherwise indicated, this product uses data provided by Canada’s provinces and territories. All rights reserved. The contents of this publication may be reproduced unaltered, in whole or in part and by any means, solely for non-commercial purposes, provided that the Canadian Institute for Health Information is properly and fully acknowledged as the copyright owner. Any reproduction or use of this publication or its contents for any commercial purpose requires the prior written authorization of the Canadian Institute for Health Information. Reproduction or use that suggests endorsement by, or affiliation with, the Canadian Institute for Health Information is prohibited. For permission or information, please contact CIHI: Canadian Institute for Health Information 495 Richmond Road, Suite 600 Ottawa, Ontario K2A 4H6 Phone: 613-241-7860 Fax: 613-241-8120 www.cihi.ca [email protected] © 2018 Canadian Institute for Health Information Cette publication est aussi disponible en français sous le titre Guide de codification des données en obstétrique. Table of contents About CIHI ................................................................................................................................. 6 Chapter 1: Introduction .............................................................................................................. -

Effects of Delayed Versus Early Cord Clamping on Healthy Term Infants
Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 893 Effects of Delayed versus Early Cord Clamping on Healthy Term Infants OLA ANDERSSON ACTA UNIVERSITATIS UPSALIENSIS ISSN 1651-6206 ISBN 978-91-554-8647-1 UPPSALA urn:nbn:se:uu:diva-198167 2013 Dissertation presented at Uppsala University to be publicly examined in Rosénsalen, Ingång 95/96, Akademiska Barnsjukhuset, Uppsala, Thursday, May 23, 2013 at 09:30 for the degree of Doctor of Philosophy. The examination will be conducted in English. Abstract Andersson, O. 2013. Effects of Delayed versus Early Cord Clamping on Healthy Term Infants. Acta Universitatis Upsaliensis. Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 893. 66 pp. Uppsala. ISBN 978-91-554-8647-1. The aim of this thesis was to study maternal and infant effects of delayed cord clamping (≥180 seconds, DCC) compared to early (≤10 seconds, ECC) in a randomised controlled trial. Practice and guidelines regarding when to clamp the cord vary globally, and different meta- analyses have shown contradictory conclusions on benefits and disadvantages of DCC and ECC. The study population consisted of 382 term infants born after normal pregnancies and ran- domised to DCC or ECC after birth. The primary objective was iron stores and iron defi- ciency at 4 months of age, but the thesis was designed to investigate a wide range of sug- gested effects associated with cord clamping. Paper I showed that DCC was associated with improved iron stores at 4 months (45% higher ferritin) and that the incidence of iron deficiency was reduced from 5.7% to 0.6%. -
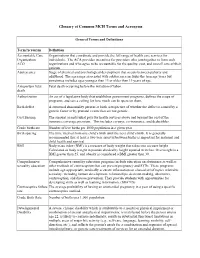
Glossary of Common MCH Terms and Acronyms
Glossary of Common MCH Terms and Acronyms General Terms and Definitions Term/Acronym Definition Accountable Care Organizations that coordinate and provide the full range of health care services for Organization individuals. The ACA provides incentives for providers who join together to form such ACO organizations and who agree to be accountable for the quality, cost, and overall care of their patients. Adolescence Stage of physical and psychological development that occurs between puberty and adulthood. The age range associated with adolescence includes the teen age years but sometimes includes ages younger than 13 or older than 19 years of age. Antepartum fetal Fetal death occurring before the initiation of labor. death Authorization An act of a legislative body that establishes government programs, defines the scope of programs, and sets a ceiling for how much can be spent on them. Birth defect A structural abnormality present at birth, irrespective of whether the defect is caused by a genetic factor or by prenatal events that are not genetic. Cost Sharing The amount an individual pays for health services above and beyond the cost of the insurance coverage premium. This includes co-pays, co-insurance, and deductibles. Crude birth rate Number of live births per 1000 population in a given year. Birth spacing The time interval from one child’s birth until the next child’s birth. It is generally recommended that at least a two-year interval between births is important for maternal and child health and survival. BMI Body mass index (BMI) is a measure of body weight that takes into account height. -

Potentially Asphyxiating Conditions and Spastic Cerebral Palsy in Infants of Normal Birth Weight
Fetus-Placenta-N ewborn Potentially asphyxiating conditions and spastic cerebral palsy in infants of normal birth weight Karin B. Nelson, MD, and Judith K. Grether, PhD Bethesda, Maryland, and Emeryville, California OBJECTIVE: Our purpose was to examine the association of cerebral palsy with conditions that can inter rupt oxygen supply to the fetus as a primary pathogenetic event. STUDY DESIGN: A population-based case-control study was performed in four California counties, 1983 through 1985, comparing birth records of 46 children with disabling spastic cerebral palsy without recognized prenatal brain lesions and 378 randomly selected control children weighing 2:2500 g at birth and surviving to age 3 years. RESULTS: Eight of 46 children with otherwise unexplained spastic cerebral palsy, all eight with quadriplegic cerebral palsy, and 15 of 378 controls had births complicated by tight nuchal cord (odds ratio for quadriplegia 18, 95% confidence interval 6.2 to 48). Other potentially asphyxiating conditions were uncommon and none was associated with spastic diplegia or hemiplegia. Level of care, oxytocin for augmentation of labor, and surgical delivery did not alter the association of potentially asphyxiating conditions with spastic quadriplegia. Intrapartum indicators of fetal stress, including meconium in amniotic fluid and fetal monitoring abnormalities, were common and did not distinguish children with quadriplegia who had potentially asphyxiating conditions from controls with such conditions. CONCLUSION: Potentially asphyxiating conditions, chiefly tight nuchal cord, were associated with an appre ciable proportion of unexplained spastic quadriplegia but not with diplegia or hemi-plegia. Intrapartum abnor malities were common both in children with cerebral palsy and controls and did not distinguish between them. -

HAC 2016 ABSTRACT for Oral Presentations
HAC 2016 ABSTRACT for Oral Presentations Presentation no.: F1.6 Presenting Author: M T SOO Dr, KWH ACON(PAD) Project title Delayed Umbilical Cord Clamping in Premature Neonates Author(s) SING C(1), LAM YY (2) , LAU WL(1), SOO M T(2), PAU B(2), TAI S M (1), LEUNG Y N(1),NG D (2), LEUNG W C (1) Department of Obstetrics & Gynaecology, Kwong Wah Hospital (1) Department of Paediatrics, Kwong Wah Hospital (2) Keyword(s) delayed umbilical cord clamping premature neonates neonatal jaundice intraventricular hemorrhage necrotizing enterocolitis Approval by Ethics Committee: N ****************************************************************************** Introduction Early umbilical cord clamping (<20 seconds after birth) has been a routine for decades. Recent evidence reveals delayed cord clamping (30 seconds or more after birth) allows blood flow between the placenta and neonate. The return of placental blood volume to the neonate leads to a higher neonatal blood volume, whichy ma cause a higher incidence of severe neonatal jaundice (NNJ) related to polycythaemia. However, the higher neonatal blood volume has also been linked to many benefits, including decreases in the number of blood transfusions, intraventricular hemorrhage (IVH) and necrotising enterocolitis (NEC) in preterm neonates. In light of these beneficial effects, our Obstetric and Paediatrics service leads the change of delayed umbilical cord clamping (DCC) after thorough evidence review. Objectives (1)‐ To provide evidence‐based recommendation on time of cord clamping in premature neonates; and (2) to assess the effects of DCC for neonates from 30 to 35 weeks 6 days of gestation age. Methodology A working group including paediatricians, obstetricians and midwives, has been set up since July 2013 to study the feasibility and refinement of a safe and effective practice for DCC Singleton vaginal births from 30 to 35 + 6 weeks of gestation age are assessed for DCC. -

What Is the Role of the Placenta—Does It Protect Against Or Is It a Target for Insult?
Teratology Primer, 3rd Edition www.teratology.org/primer What Is the Role of the Placenta—Does It Protect Against or Is It a Target for Insult? Richard K. Miller University of Rochester School of Medicine & Dentistry Rochester, New York The placenta is not just a barrier but has many functions that are vital to the health of the embryo/fetus. The placenta is the anchor, the conduit, and the controller of pregnancy—and it can also be a target for toxicant action. The placenta encompasses not only the chorioallantoic placenta but all of its extraembryonic membranes (chorion/amnion) and the yolk sac. (Figure 1). The placenta and its membranes secure the embryo and fetus to the decidua (uterine lining) and release a variety of steroid and protein hormones that characterize the physiology of the pregnant female. Figure 1. Placental Structure in the Mouse. Figures depict early development of the mouse conceptus at embryonic days (E3.5, E7.5, E12.5). In the fetus, the visceral yolk sac (vYS) inverts and remains active throughout the entire gestation providing for transfer of selective large molecules, e.g., immunoglobulins IgG and vitamin B12. Abbreviations: Al, allantois; Am, amnion; Ch, chorion; Dec, decidua; Emb, embryo; Epc, ectoplacental cone; ICM, inner cell mass; Lab, Labyrinth; pYS, parietal yolk sac; SpT, spongiotrophoblast; TCG, trophoblast giant cell; Umb Cord, umbilical cord; vYS, visceral yolk sac; C-TGC, maternal blood canal trophoblast giant cell; P-TGC, parietal trophoblast giant cell; S-TGC, sinusoidal trophoblast giant cell; SpA-TGC, Spiral artery-associated trophoblast giant cell; Cyan-trophectoderm and trophoblast lineage, Black- inner cell mass and embryonic ectoderm; Gray -endoderm, Red-maternal vasculature, Purple-mesoderm, Yellow- decidua, Pink-fetal blood vessels in labyrinth.