Why Does My Patient Have Leukocytosis?
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Updates in Mastocytosis
Updates in Mastocytosis Tryptase PD-L1 Tracy I. George, M.D. Professor of Pathology 1 Disclosure: Tracy George, M.D. Research Support / Grants None Stock/Equity (any amount) None Consulting Blueprint Medicines Novartis Employment ARUP Laboratories Speakers Bureau / Honoraria None Other None Outline • Classification • Advanced mastocytosis • A case report • Clinical trials • Other potential therapies Outline • Classification • Advanced mastocytosis • A case report • Clinical trials • Other potential therapies Mastocytosis symposium and consensus meeting on classification and diagnostic criteria for mastocytosis Boston, October 25-28, 2012 2008 WHO Classification Scheme for Myeloid Neoplasms Acute Myeloid Leukemia Chronic Myelomonocytic Leukemia Atypical Chronic Myeloid Leukemia Juvenile Myelomonocytic Leukemia Myelodysplastic Syndromes MDS/MPN, unclassifiable Chronic Myelogenous Leukemia MDS/MPN Polycythemia Vera Essential Thrombocythemia Primary Myelofibrosis Myeloproliferative Neoplasms Chronic Neutrophilic Leukemia Chronic Eosinophilic Leukemia, NOS Hypereosinophilic Syndrome Mast Cell Disease MPNs, unclassifiable Myeloid or lymphoid neoplasms Myeloid neoplasms associated with PDGFRA rearrangement associated with eosinophilia and Myeloid neoplasms associated with PDGFRB abnormalities of PDGFRA, rearrangement PDGFRB, or FGFR1 Myeloid neoplasms associated with FGFR1 rearrangement (EMS) 2017 WHO Classification Scheme for Myeloid Neoplasms Chronic Myelomonocytic Leukemia Acute Myeloid Leukemia Atypical Chronic Myeloid Leukemia Juvenile Myelomonocytic -

Pathologic Rupture of the Spleen in a Patient with Acute Myelogenous Leukemia and Leukostasis
rev bras hematol hemoter. 2014;36(4):290–292 Revista Brasileira de Hematologia e Hemoterapia Brazilian Journal of Hematology and Hemotherapy www.rbhh.org Case report Pathologic rupture of the spleen in a patient with acute myelogenous leukemia and leukostasis Gil Cunha De Santis ∗, Luciana Correa Oliveira, Aline Fernanda Ramos, Nataly Dantas Fortes da Silva, Roberto Passetto Falcão Universidade de São Paulo (USP), Ribeirão Preto, SP, Brazil article info abstract Article history: Rupture of the spleen can be classified as spontaneous, traumatic, or pathologic. Patho- Received 14 October 2013 logic rupture has been reported in infectious diseases such as infectious mononucleosis, Accepted 14 January 2014 and hematologic malignancies such as acute and chronic leukemias. Splenomegaly is con- Available online 28 May 2014 sidered the most relevant factor that predisposes to splenic rupture. A 66-year-old man with acute myeloid leukemia evolved from an unclassified myeloproliferative neoplasm, Keywords: complaining of fatigue and mild upper left abdominal pain. He was pale and presented Splenomegaly fever and tachypnea. Laboratory analyses showed hemoglobin 8.3 g/dL, white blood cell 9 9 Leukemia count 278 × 10 /L, platelet count 367 × 10 /L, activated partial thromboplastin time (aPTT) Myeloid ratio 2.10, and international normalized ratio (INR) 1.60. A blood smear showed 62% of Acute myeloblasts. The immunophenotype of the blasts was positive for CD117, HLA-DR, CD13, Leukostasis CD56, CD64, CD11c and CD14. Lactate dehydrogenase was 2384 U/L and creatinine 2.4 mg/dL (normal range: 0.7–1.6 mg/dL). Two sessions of leukapheresis were performed. At the end of the second session, the patient presented hemodynamic instability that culminated in cir- culatory shock and death. -

Digitalcommons@UNMC Agranulocytosis
University of Nebraska Medical Center DigitalCommons@UNMC MD Theses Special Collections 5-1-1935 Agranulocytosis Gordon A. Gunn University of Nebraska Medical Center This manuscript is historical in nature and may not reflect current medical research and practice. Search PubMed for current research. Follow this and additional works at: https://digitalcommons.unmc.edu/mdtheses Part of the Medical Education Commons Recommended Citation Gunn, Gordon A., "Agranulocytosis" (1935). MD Theses. 386. https://digitalcommons.unmc.edu/mdtheses/386 This Thesis is brought to you for free and open access by the Special Collections at DigitalCommons@UNMC. It has been accepted for inclusion in MD Theses by an authorized administrator of DigitalCommons@UNMC. For more information, please contact [email protected]. AGRANULOOYTOSIS ,- Senior Thesis by GOrdon .M.. Gunn INTRODUCTION Fifteen years ago the medioal profession new nothing of the disease spoken of in this paper as agranulocytosis. Since Schultz, in 1922, gave an accurate description of a fulminat ing case, agranulocytosis has oomettoClOCo.'UPy more and more prominence in the medical field. Today, the literature is fairly teeming with accounts of isolated cases of all descriptions. Added to this a confus ing nomenclature, varied classifications, and heterogeneous forms of treatment; and the large question of whether it is a disease entity, a group of diseases, or only a symptom complex, and some idea may be garnered as to the progress made. Time is a most important factor in diagnosis of this disease, and the prognosis at best is grave. The treatment has gone through the maze of trials as that of any other new disease; there must be a cause and so there must be some specific treatment. -

Follicular Lymphoma
Follicular Lymphoma What is follicular lymphoma? Let us explain it to you. www.anticancerfund.org www.esmo.org ESMO/ACF Patient Guide Series based on the ESMO Clinical Practice Guidelines FOLLICULAR LYMPHOMA: A GUIDE FOR PATIENTS PATIENT INFORMATION BASED ON ESMO CLINICAL PRACTICE GUIDELINES This guide for patients has been prepared by the Anticancer Fund as a service to patients, to help patients and their relatives better understand the nature of follicular lymphoma and appreciate the best treatment choices available according to the subtype of follicular lymphoma. We recommend that patients ask their doctors about what tests or types of treatments are needed for their type and stage of disease. The medical information described in this document is based on the clinical practice guidelines of the European Society for Medical Oncology (ESMO) for the management of newly diagnosed and relapsed follicular lymphoma. This guide for patients has been produced in collaboration with ESMO and is disseminated with the permission of ESMO. It has been written by a medical doctor and reviewed by two oncologists from ESMO including the lead author of the clinical practice guidelines for professionals, as well as two oncology nurses from the European Oncology Nursing Society (EONS). It has also been reviewed by patient representatives from ESMO’s Cancer Patient Working Group. More information about the Anticancer Fund: www.anticancerfund.org More information about the European Society for Medical Oncology: www.esmo.org For words marked with an asterisk, a definition is provided at the end of the document. Follicular Lymphoma: a guide for patients - Information based on ESMO Clinical Practice Guidelines – v.2014.1 Page 1 This document is provided by the Anticancer Fund with the permission of ESMO. -

Childhood Leukemia
Onconurse.com Fact Sheet Childhood Leukemia The word leukemia literally means “white blood.” fungi. WBCs are produced and stored in the bone mar- Leukemia is the term used to describe cancer of the row and are released when needed by the body. If an blood-forming tissues known as bone marrow. This infection is present, the body produces extra WBCs. spongy material fills the long bones in the body and There are two main types of WBCs: produces blood cells. In leukemia, the bone marrow • Lymphocytes. There are two types that interact to factory creates an overabundance of diseased white prevent infection, fight viruses and fungi, and pro- cells that cannot perform their normal function of fight- vide immunity to disease: ing infection. As the bone marrow becomes packed with diseased white cells, production of red cells (which ° T cells attack infected cells, foreign tissue, carry oxygen and nutrients to body tissues) and and cancer cells. platelets (which help form clots to stop bleeding) slows B cells produce antibodies which destroy and stops. This results in a low red blood cell count ° foreign substances. (anemia) and a low platelet count (thrombocytopenia). • Granulocytes. There are four types that are the first Leukemia is a disease of the blood defense against infection: Blood is a vital liquid which supplies oxygen, food, hor- ° Monocytes are cells that contain enzymes that mones, and other necessary chemicals to all of the kill foreign bacteria. body’s cells. It also removes toxins and other waste products from the cells. Blood helps the lymph system ° Neutrophils are the most numerous WBCs to fight infection and carries the cells necessary for and are important in responding to foreign repairing injuries. -

Leukocyte Adhesion Deficiency-I
Clinical Communications Leukocyte adhesion deficiency-I: A this article’s Online Repository at www.jaci-inpractice.org for a comprehensive review of all published comprehensive listing of publications and patient numbers by cases country and Table E2 for a comprehensive listing of references). Elena Almarza Novoa, PhDa,b,*, Per investigator assessment, 113 patients were considered to have severe LAD-I, 63 moderate, and 147 not classified. Sanchali Kasbekar, PharmDc,*, d e Neutrophil CD18 expression was reported for 265 cases and was Adrian J. Thrasher, MD, PhD , Donald B. Kohn, MD , less than 2% in 135 patients (51%) and 2% or more in 130 Julian Sevilla, MD, PhDf, Tony Nguyen, MBAg, patients (49%). Four patients with CD18 greater than or equal Jonathan D. Schwartz, MDc,z, and to 2% were considered to have severe LAD-I (CD18% range, Juan A. Bueren, PhDa,b,z 2.4-17.3). Sex information was available for 282 patients, of which 148 (52%) were males. Clinical Implications Age at presentation was reported for 146 cases. For 63 patients with CD18 less than 2%, median presentation was at age 1 Leukocyte adhesion deficiency-I (LAD-I) is a rare, serious month (range, 0.03-18 months); for 62 patients with CD18 of disorder with severity determined by defective CD18 2% or more, median presentation was at age 6 months (range, expression. LAD-I is characterized by umbilical 0.03-192 months). HSCT was performed for 125 patients; 198 complications, granulocytosis, and diverse infections. patients did not undergo HSCT. Severe LAD-I is frequently fatal before the age of 2 years Infections were described for 248 (77%) of the 323 cases; fi without allogeneic transplant. -

Late Effects Among Long-Term Survivors of Childhood Acute Leukemia in the Netherlands: a Dutch Childhood Leukemia Study Group Report
0031-3998/95/3805-0802$03.00/0 PEDIATRIC RESEARCH Vol. 38, No.5, 1995 Copyright © 1995 International Pediatric Research Foundation, Inc. Printed in U.S.A. Late Effects among Long-Term Survivors of Childhood Acute Leukemia in The Netherlands: A Dutch Childhood Leukemia Study Group Report A. VAN DER DOES-VAN DEN BERG, G. A. M. DE VAAN, J. F. VAN WEERDEN, K. HAHLEN, M. VAN WEEL-SIPMAN, AND A. J. P. VEERMAN Dutch Childhood Leukemia Study Group,' The Hague, The Netherlands A.8STRAC ' Late events and side effects are reported in 392 children cured urogenital, or gastrointestinal tract diseases or an increased vul of leukemia. They originated from 1193 consecutively newly nerability of the musculoskeletal system was found. However, diagnosed children between 1972 and 1982, in first continuous prolonged follow-up is necessary to study the full-scale late complete remission for at least 6 y after diagnosis, and were effects of cytostatic treatment and radiotherapy administered treated according to Dutch Childhood Leukemia Study Group during childhood. (Pediatr Res 38: 802-807, 1995) protocols (70%) or institutional protocols (30%), all including cranial irradiation for CNS prophylaxis. Data on late events (relapses, death in complete remission, and second malignancies) Abbreviations were collected prospectively after treatment; late side effects ALL, acute lymphocytic leukemia were retrospectively collected by a questionnaire, completed by ANLL, acute nonlymphocytic leukemia the responsible pediatrician. The event-free survival of the 6-y CCR, continuous first complete remission survivors at 15 y after diagnosis was 92% (±2%). Eight late DCLSG, Dutch Childhood Leukemia Study Group relapses and nine second malignancies were diagnosed, two EFS, event free survival children died in first complete remission of late toxicity of HR, high risk treatment, and one child died in a car accident. -

(ACIP) General Best Guidance for Immunization
8. Altered Immunocompetence Updates This section incorporates general content from the Infectious Diseases Society of America policy statement, 2013 IDSA Clinical Practice Guideline for Vaccination of the Immunocompromised Host (1), to which CDC provided input in November 2011. The evidence supporting this guidance is based on expert opinion and arrived at by consensus. General Principles Altered immunocompetence, a term often used synonymously with immunosuppression, immunodeficiency, and immunocompromise, can be classified as primary or secondary. Primary immunodeficiencies generally are inherited and include conditions defined by an inherent absence or quantitative deficiency of cellular, humoral, or both components that provide immunity. Examples include congenital immunodeficiency diseases such as X- linked agammaglobulinemia, SCID, and chronic granulomatous disease. Secondary immunodeficiency is acquired and is defined by loss or qualitative deficiency in cellular or humoral immune components that occurs as a result of a disease process or its therapy. Examples of secondary immunodeficiency include HIV infection, hematopoietic malignancies, treatment with radiation, and treatment with immunosuppressive drugs. The degree to which immunosuppressive drugs cause clinically significant immunodeficiency generally is dose related and varies by drug. Primary and secondary immunodeficiencies might include a combination of deficits in both cellular and humoral immunity. Certain conditions like asplenia and chronic renal disease also can cause altered immunocompetence. Determination of altered immunocompetence is important to the vaccine provider because incidence or severity of some vaccine-preventable diseases is higher in persons with altered immunocompetence; therefore, certain vaccines (e.g., inactivated influenza vaccine, pneumococcal vaccines) are recommended specifically for persons with these diseases (2,3). Administration of live vaccines might need to be deferred until immune function has improved. -

Follicular Lymphoma with Leukemic Phase at Diagnosis: a Series Of
Leukemia Research 37 (2013) 1116–1119 Contents lists available at SciVerse ScienceDirect Leukemia Research journa l homepage: www.elsevier.com/locate/leukres Follicular lymphoma with leukemic phase at diagnosis: A series of seven cases and review of the literature a c c c c Brady E. Beltran , Pilar Quinones˜ , Domingo Morales , Jose C. Alva , Roberto N. Miranda , d e e b,∗ Gary Lu , Bijal D. Shah , Eduardo M. Sotomayor , Jorge J. Castillo a Department of Oncology and Radiotherapy, Edgardo Rebagliati Martins Hospital, Lima, Peru b Division of Hematology and Oncology, Rhode Island Hospital, Brown University Alpert Medical School, Providence, RI, USA c Department of Pathology, Edgardo Rebaglati Martins Hospital, Lima, Peru d Department of Hematopathology, MD Anderson Cancer Center, Houston, TX, USA e Department of Malignant Hematology, H. Lee Moffitt Cancer Center & Research Institute, Tampa, FL, USA a r t i c l e i n f o a b s t r a c t Article history: Follicular lymphoma (FL) is a prevalent type of non-Hodgkin lymphoma in the United States and Europe. Received 23 April 2013 Although, FL typically presents with nodal involvement, extranodal sites are less common, and leukemic Received in revised form 25 May 2013 phase at diagnosis is rare. There is mounting evidence that leukemic presentation portends a worse Accepted 26 May 2013 prognosis in patients with FL. We describe 7 patients with a pathological diagnosis of FL who presented Available online 20 June 2013 with a leukemic phase. We compared our cases with 24 additional cases reported in the literature. Based on our results, patients who present with leukemic FL tend to have higher risk disease. -

Cells, Tissues and Organs of the Immune System
Immune Cells and Organs Bonnie Hylander, Ph.D. Aug 29, 2014 Dept of Immunology [email protected] Immune system Purpose/function? • First line of defense= epithelial integrity= skin, mucosal surfaces • Defense against pathogens – Inside cells= kill the infected cell (Viruses) – Systemic= kill- Bacteria, Fungi, Parasites • Two phases of response – Handle the acute infection, keep it from spreading – Prevent future infections We didn’t know…. • What triggers innate immunity- • What mediates communication between innate and adaptive immunity- Bruce A. Beutler Jules A. Hoffmann Ralph M. Steinman Jules A. Hoffmann Bruce A. Beutler Ralph M. Steinman 1996 (fruit flies) 1998 (mice) 1973 Discovered receptor proteins that can Discovered dendritic recognize bacteria and other microorganisms cells “the conductors of as they enter the body, and activate the first the immune system”. line of defense in the immune system, known DC’s activate T-cells as innate immunity. The Immune System “Although the lymphoid system consists of various separate tissues and organs, it functions as a single entity. This is mainly because its principal cellular constituents, lymphocytes, are intrinsically mobile and continuously recirculate in large number between the blood and the lymph by way of the secondary lymphoid tissues… where antigens and antigen-presenting cells are selectively localized.” -Masayuki, Nat Rev Immuno. May 2004 Not all who wander are lost….. Tolkien Lord of the Rings …..some are searching Overview of the Immune System Immune System • Cells – Innate response- several cell types – Adaptive (specific) response- lymphocytes • Organs – Primary where lymphocytes develop/mature – Secondary where mature lymphocytes and antigen presenting cells interact to initiate a specific immune response • Circulatory system- blood • Lymphatic system- lymph Cells= Leukocytes= white blood cells Plasma- with anticoagulant Granulocytes Serum- after coagulation 1. -
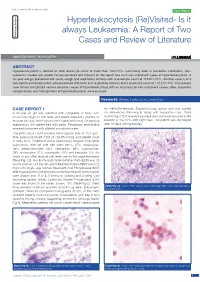
Hyperleukocytosis (Re)Visited- Is It Case Series Always Leukaemia: a Report of Two Pathology Section Cases and Review of Literature Short Communication
Review Article Clinician’s corner Original Article Images in Medicine Experimental Research Miscellaneous Letter to Editor DOI: 10.7860/JCDR/2020/40556.13409 Case Report Postgraduate Education Hyperleukocytosis (Re)Visited- Is it Case Series always Leukaemia: A Report of Two Pathology Section Cases and Review of Literature Short Communication ASHUTOSH RATH1, RICHA GUPTA2 ABSTRACT Hyperleukocytosis is defined as total leukocyte count of more than 100×109/L. Commonly seen in leukaemic conditions, non- leukaemic causes are usually not encountered and thought of. We report two such non-malignant cases of hyperleukocytosis. A six-year old girl presented with fever, cough and respiratory distress with a leukocyte count of 125.97×109/L. Another case is of a two-month old female infant, who presented with fever and respiratory distress and a leukocyte count of 112.27×109/L. The present case thrives to highlight various possible causes of hyperleukocytosis with an emphasis on non-malignant causes. Also, important complications and management of hyperleukocytosis are discussed. Keywords: Benign, Leukocytosis, Leukostasis CASE REPORT 1 for methicillin-resistant Staphylococcus aureus and was started A six-year-old girl was admitted with complaints of fever, non- on intravenous Vancomycin along with supportive care. Serial productive cough for one week and severe respiratory distress for monitoring of TLC revealed a gradual reduction and it returned to the the past one day. There was no other significant history. On physical baseline of 15×109/L after eight days. The patient was discharged examination, the patient had mild pallor. Respiratory examination after 10 days of hospital stay. -

Leukemoid Reaction in a Patient with Acute Lymphoblastic Leukemia Following the Second Chemotherapy
262JCEI / Yokuş et al. Leukemoid reaction in ALL 2013; 4 (2): 262-263 Journal of Clinical and Experimental Investigations doi: 10.5799/ahinjs.01.2013.02.0280 LETTER TO EDITOR Leukemoid reaction in a patient with acute lymphoblastic leukemia following the second chemotherapy Akut lenfoblastik lösemili hastada ikinci kemoterapi sonrası gelişen lökomoid reaksiyon Osman Yokuş1, Murat Albayrak2, Aynur Albayrak3, Habip Gedik4 To the Editor, to 50.000 cells/µL. The examined peripheral blood smear appeared as similar to the chronic phase of The occurrence of persistent neutrophilic leukocy- CML (fig.2). A cytogenetic examination of Philadel- tosis above 50,000 cells/µL for reasons other than phia chromosome [t(9:22] was found to be nega- leukemia is defined as leukemoid reaction. Chronic tive, therefore, CML was excluded in the patient. myelogenous leukemia (CML) and chronic neutro- Hydroxurea was initiated once a day. Leukocytosis philic leukemia (CNL) should be excluded, and un- recovered to normal range after one week (fig.3) derlying diseases or causes should be examined, and bone marrow examination revealed remission. in differential diagnosis. The most commonly ob- Cytogenetic analysis was normal and this leukocy- served causes of leukemoid reactions are severe tosis was determined as reactive leukemoid reac- infections, intoxications, malignancies, severe hem- tion. We aimed to report this case owing to the fact orrhage, or acute hemolysis [1]. J Clin Exp Invest that leukocytosis associated with G-CSF, which is 2013; 4 (2): 262-263 used to increase the leukocyte count during neutro- Rarely, leukemoid reaction can be seen in pa- penia, has been reported previously but it occurred tients with acute leukemia subsequent to chemo- after second chemotherapy without G-CSF [4].