TRIAGE in the Emergency Department Using the Emergency Severity Index - (ESI) 5 Levels
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Tracheal Intubation Following Traumatic Injury)
CLINICAL MANAGEMENT UPDATE The Journal of TRAUMA Injury, Infection, and Critical Care Guidelines for Emergency Tracheal Intubation Immediately after Traumatic Injury C. Michael Dunham, MD, Robert D. Barraco, MD, David E. Clark, MD, Brian J. Daley, MD, Frank E. Davis III, MD, Michael A. Gibbs, MD, Thomas Knuth, MD, Peter B. Letarte, MD, Fred A. Luchette, MD, Laurel Omert, MD, Leonard J. Weireter, MD, and Charles E. Wiles III, MD for the EAST Practice Management Guidelines Work Group J Trauma. 2003;55:162–179. REFERRALS TO THE EAST WEB SITE and impaired laryngeal reflexes are nonhypercarbic hypox- Because of the large size of the guidelines, specific emia and aspiration, respectively. Airway obstruction can sections have been deleted from this article, but are available occur with cervical spine injury, severe cognitive impairment on the Eastern Association for the Surgery of Trauma (EAST) (Glasgow Coma Scale [GCS] score Յ 8), severe neck injury, Web site (www.east.org/trauma practice guidelines/Emergency severe maxillofacial injury, or smoke inhalation. Hypoventi- Tracheal Intubation Following Traumatic Injury). lation can be found with airway obstruction, cardiac arrest, severe cognitive impairment, or cervical spinal cord injury. I. STATEMENT OF THE PROBLEM Aspiration is likely to occur with cardiac arrest, severe cog- ypoxia and obstruction of the airway are linked to nitive impairment, or severe maxillofacial injury. A major preventable and potentially preventable acute trauma clinical concern with thoracic injury is the development of Hdeaths.1–4 There is substantial documentation that hyp- nonhypercarbic hypoxemia. Lung injury and nonhypercarbic oxia is common in severe brain injury and worsens neuro- hypoxemia are also potential sequelae of aspiration. -

Emergency Department Resuscitation of the Critically Ill Review by Stephen C
BOOK AND MEDIA REVIEW Emergency Department Resuscitation of the Critically Ill Review by Stephen C. Morris, MD, MPH 0196-0644/$-see front matter Copyright © 2018 by the American College of Emergency Physicians. Emergency Department Resuscitation of the crashing morbidly obese patient reviews some of the nuanced Critically Ill management we should be striving for as more of our patients become obese, such as specific airway and ventilation Winters ME, Bond MC, Marcolini EG, et al management and use of ideal versus total body weight American College of Emergency Physicians calculations for critical-care-specific medications. Consider It was with great pleasure that I agreed to review the another example from the chapter on left ventricular assist second edition of Emergency Department Resuscitation of the devices. Although these patients have long been the domain Critically Ill, by Michael E. Winters. I had read and relied of specialty centers, with complex physiology and on the first edition posttraining. Like most who work in complications, the longevity now offered by the devices will emergency medicine, I practice a great deal of critical care; ultimately make them the domain of the community however, I have not completed a fellowship in critical care, emergency department. Additionally, at the cutting edge of nor do I review critical care literature with the level of our practice, the text contains a chapter on extracorporeal scrutiny that I would like. For those of us who want to membrane oxygenation, with a discussion of the practical ensure that we are up to date to guarantee clinical and clinical aspects of implementation. -

Management of Acute Liver Failure In
Management of Acute Liver Failure in ICU Philip Berry MRCP, Clinical Research Fellow, Institute of Liver Studies, Kings College Hospital, London, UK Email: [email protected] Self assessment questions Scenario: A twenty-year-old female is brought into the Emergency Department having been found unconscious in her bedsit. There is no other recent history. She did not respond to a bolus of 50% dextrose in the ambulance, despite having an unrecordable blood glucose when tested by the paramedics. While she is being intubated on account of reduced level of consciousness, an arterial blood gas sample reveals profound lactic acidosis (pH 7.05, pCO2 2.5 kPa, base deficit – 10, lactate 13 mg/L). Blood pressure is 95/50 mmHg. 1. What are the possible explanations for her presentation? Laboratory tests demonstrate hepatocellular necrosis (AST 21,000 U/L) and coagulopathy (INR 9.1) with thrombocytopenia (platelet count 26 x 109/L). Acute liver failure appears the most likely diagnosis. 2. What are the most likely causes of acute liver failure (ALF) in this previously well patient? Her mean arterial blood pressure remains low (50mmHg) after 3 litres of colloid and crystalloid. The casualty nurse, who is doing half-hourly neurological observations, reports reduced pupillary response to light. 3. What severe complications of ALF may result in death within hours, and what are the immediate management priorities for this patient? Introduction Successful management of this rare but potentially devastating disorder relies on early recognition. The hallmark of acute liver failure (ALF) is encephalopathy (ranging from a subtle alterations in consciousness level to coma) in the context of an acute, severe liver injury. -

STAB WOUNDS PENETRATING the LEFT ATRIUM by MILROY PAUL from the General Hospital, Colombo, Ceylon
Thorax: first published as 10.1136/thx.16.2.190 on 1 June 1961. Downloaded from Thorax (1961), 16, 190. STAB WOUNDS PENETRATING THE LEFT ATRIUM BY MILROY PAUL From the General Hospital, Colombo, Ceylon (RECEIVED FOR PUBLICATION NOVEMBER 15, 1960) A stab wound penetrating the left atrium followed by 4 pints of dextran throughout the night. (excluding the left auricle) would have to penetrate At 7 a.m. the next day he was still alive, breathing through other chambers of the heart or through quietly, with a pulse of 122 of good volume, blood the great arteries at their origin from the heart to pressure 100/70 mm. Hg, and warm extremities. Although there was still no blood in the bank, an reach the left atrium from the front of the chest. operation was decided on and begun at 8 a.m. Bv Such wounds would be fatal, the patient dying this time the pulse had again become small, although from profuse haemorrhage within a few minutes. the extremities were warm. The left chest was opened A stab wound through the back of the chest could through an intercostal incision in the eighth intercostal reach the left atrium in the narrow sulcus between space. The left pleural cavity contained fluid blood the root of the left lung in front and the oeso- and clots. In the outer surface of the lung under- phagus and descending thoracic aorta behind, but lying the stab wound of the chest wall there was a placing a wound at this site without at the same stab wound of the lung. -

The Nebraska Office of Emergency Health Systems Trauma Program Is Pleased That You Wish to Participate in the Statewide Trauma System
Revised July 2019 INSTRUCTIONS FOR FILLING OUT PRE-REVIEW QUESTIONNAIRE (PRQ) The Nebraska Office of Emergency Health Systems Trauma Program is pleased that you wish to participate in the statewide trauma system. The Nebraska Statewide Trauma System is comprised of hospitals and clinics striving to improve trauma patient care. Through this system all facilities offering trauma care may become centers of excellence. Thank you for participating in this process. In order to prepare for your on-site review, please complete this questionnaire. All answers should directly follow the questions. The entire questionnaire is available on the web in a downloadable format @ http://dhhs.ne.gov/Pages/EHS-Statewide-Trauma-System-of-Care.aspx. The PRQ should be completed electronically if possible otherwise, you may submit a hard copy. Note: If a hard copy is printed a color printer should be used so that information and questions printed in blue appear on the page to the applicant. Return the completed questionnaire to: Sherri Wren EHS Trauma Program Manager Office of Emergency Health Systems P.O. Box 95026 Lincoln, NE 68509-5026 Phone: (402) 471-0539 E-mail: [email protected] If you have questions or concerns while filling out the PRQ, please contact: State of Nebraska Trauma Nurse Specialist OR your Regional Trauma Program Manager (please reference website list of Designated Trauma Centers on the website cited above for names and contact information). I. PURPOSE: A. The purpose of this questionnaire for Consultation Visits is: 1. To provide your institution with an outline of what site visitors will be discussing with you. -

Mass/Multiple Casualty Triage
9.1 MASS/MULTIPLE CASUALTY TRIAGE PURPOSE · The goal of the mass/multiple Casualty Triage protocol is to prepare for a unified, coordinated, and immediate EMS mutual aid response by prehospital and hospital agencies to effectively expedite the emergency management of the victims of any type of Mass Casualty Incident (MCI). · Successful management of any MCI depends upon the effective cooperation, organization, and planning among health care professionals, hospital administrators and out-of-hospital EMS agencies, state and local government representatives, and individuals and/or organizations associated with disaster-related support agencies. · Adoption of Model Uniform Core Criteria (MUCC). DEFINITIONS Multiple Casualty Situations · The number of patients and the severity of the injuries do not exceed the ability of the provider to render care. Patients with life-threatening injuries are treated first. Mass Casualty Incidents · The number of patients and the severity of the injuries exceed the capability of the provider, and patients sustaining major injuries who have the greatest chance of survival with the least expenditure of time, equipment, supplies, and personnel are managed first. H a z GENERAL CONSIDERATIONS m Initial assessment to include the following: a t · Location of incident. & · Type of incident. M · Any hazards. C · Approximate number of victims. I · Type of assistance required. 9 . 1 COMMUNICATION · Within the scope of a Mass Casualty Incident, the EMS provider may, within the limits of their scope of practice, perform necessary ALS procedures, that under normal circumstances would require a direct physician’s order. · These procedures shall be the minimum necessary to prevent the loss of life or the critical deterioration of a patient’s condition. -
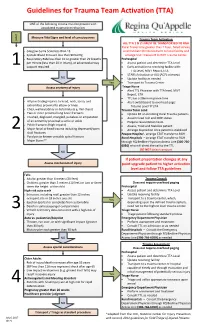
Guidelines for Trauma Team Activation (TTA)
Guidelines for Trauma Team Activation (TTA) ONE of the following criteria must be present with associated traumatic mechanism L e v e Measure Vital Signs and level of consciousness l Trauma Team Activation ALL TTA 1 & 2's MUST BE TRANSPORTED TO RGH Rural Travel time greater than 1 hour, failed airway · Glasgow Coma Scale less than 13 or immediate life threat divert to local facility and · Systolic Blood Pressure less than 90mmHg arrange STAT transport to RGH Trauma Center · Respiratory Rate less than 10 or greater then 29 breaths Prehospital per minute (less than 20 in infant), or advanced airway · Assess patient and determine TTA Level 1 support required · Early activation to receiving facility with: TTA Level, MIVT Report, ETA · STARS Activation or ALS (ACP) intercept NO · Update facility as needed Yes · Transport to Trauma Center Assess anatomy of injury Triage Nurse · Alert TTL Physician with TTA level, MIVT Report, ETA · TTL has a 20min response time · All penetrating injuries to head, neck, torso, and · Alert switchboard to overhead page: extremities proximal to elbow or knee Trauma Level ‘#’ ETA · Chest wall instability or deformity (e.g. flail chest) Trauma Team Lead · Two or more proximal long-bone fractures · Update ER on incoming Rural Trauma patients · Crushed, degloved, mangled, pulseless or amputation · Assume lead role and MRP status of an extremity proximal to wrist or ankle · Prepare resuscitation team · Pelvic fractures (high impact) · Assess, Treat and Stabilize patient 2 · Major facial or head trauma including depressed/open -

MASS CASUALTY TRAUMA TRIAGE PARADIGMS and PITFALLS July 2019
1 Mass Casualty Trauma Triage - Paradigms and Pitfalls EXECUTIVE SUMMARY Emergency medical services (EMS) providers arrive on the scene of a mass casualty incident (MCI) and implement triage, moving green patients to a single area and grouping red and yellow patients using triage tape or tags. Patients are then transported to local hospitals according to their priority group. Tagged patients arrive at the hospital and are assessed and treated according to their priority. Though this triage process may not exactly describe your agency’s system, this traditional approach to MCIs is the model that has been used to train American EMS As a nation, we’ve got a lot providers for decades. Unfortunately—especially in of trailers with backboards mass violence incidents involving patients with time- and colored tape out there critical injuries and ongoing threats to responders and patients—this model may not be feasible and may result and that’s not what the focus in mis-triage and avoidable, outcome-altering delays of mass casualty response is in care. Further, many hospitals have not trained or about anymore. exercised triage or re-triage of exceedingly large numbers of patients, nor practiced a formalized secondary triage Dr. Edward Racht process that prioritizes patients for operative intervention American Medical Response or transfer to other facilities. The focus of this paper is to alert EMS medical directors and EMS systems planners and hospital emergency planners to key differences between “conventional” MCIs and mass violence events when: • the scene is dynamic, • the number of patients far exceeds usual resources; and • usual triage and treatment paradigms may fail. -

THE BUSINESS of EMERGENCY MEDICINE … MADE EASY! Sponsored by AAEM Services, the Management Education Division of AAEM
THE BUSINESS OF EMERGENCY MEDICINE … MADE EASY! Sponsored by AAEM Services, the management education division of AAEM UDisclaimer The views presented in this course and syllabus represent those of the lecturers. The information is presented in a generalized manner and may not be applicable to your specific situation. Also, in many cases, one method of tackling a problem is demonstrated when many others (perhaps better alternatives for your situation) exist. Thus, it is important to consult your attorney, accountant or practice management service before implementing the concepts relayed in this course. UGoal This course is designed to introduce emergency physicians with no formal business education to running the business of emergency medicine. The title “The Business of Emergency Medicine Made Easy” is not meant to be demeaning. Instead, the course will convince anyone with the aptitude to become an emergency physician that, by comparison, running the business of emergency medicine is relatively simple. With off- the-shelf software and a little help from key business associates, we can run an emergency medicine business and create a win-win-win situation for the hospital, patients, and EPs. By eliminating an unnecessary profit stream as exists with CMGs, we can attract and retain better, brighter EPs. AAEM’s Certificate of Compliance on “Fairness in the Workplace” defines the boundaries within which independent groups should practice in order to be considered truly fair. Attesting to the following eight principles allows a group the privilege -

Validation of Lactate Clearance at 6 H for Mortality Prediction in Critically Ill Children
570 Research Article Validation of lactate clearance at 6 h for mortality prediction in critically ill children Rajeev Kumar, Nirmal Kumar Background and Aims: To validate the lactate clearance (LC) at 6 h for mortality Access this article online prediction in Pediatric Intensive Care Unit (PICU)-admitted patients and its comparison Website: www.ijccm.org with a pediatric index of mortality 2 (PIM 2) score. Design: A prospective, observational DOI: 10.4103/0972-5229.192040 study in a tertiary care center. Materials and Methods: Children <13 years of age, Quick Response Code: Abstract admitted to PICU were included in the study. Lactate levels were measured at 0 and 6 h of admission for clearance. LC and delayed or nonclearance group compared for in-hospital mortality and compared with PIM 2 score for mortality prediction. Results: Of the 140 children (mean age 33.42 months) who were admitted to PICU, 23 (16.42%) patients died. For LC cut-off (16.435%) at 6 h, 92 patients qualified for clearance and 48 for delayed or non-LC group. High mortality was observed (39.6%) in delayed or non-LC group as compared to clearance group (4.3%) (P = 0.000). LC cut-off of 16.435% at 6 h (sensitivity 82.6%, specificity 75.2%, positive predictive value 39.6%, and negative predictive value 95.7%) correlates with mortality. Area under receiver operating characteristic (ROC) for LC at 6 h for mortality prediction was 0.823 (P = 0.000). The area under ROC curve for expected mortality prediction by PIM 2 score at admission was 0.906 and at 12.3% cut-off of PIM 2 Score was related with mortality. -

Package for Emergency Resuscitation and Intensive Care Unit
Package for Emergency Resuscitation and Intensive Care Unit Extracted from WHO manual Surgical Care at the District Hospital and WHO Integrated Management for Emergency & Essential Surgical Care toolkit For further details and anaesthetic resources please refer to full text at: http://www.who.int/surgery/publications/imeesc/en/index.html 1 1. Anaesthesia and Oxygen XYGEN KEY POINTS: • A reliable oxygen supply is essential for anaesthesia and for any seriously ill patients • In many places, oxygen concentrators are the most suitable and economical way of providing oxygen, with a few backup cylinders in case of electricity failure • Whatever your source of oxygen, you need an effective system for maintenance and spares • Clinical staff need to be trained how to use oxygen safely, effectively and economically. • A high concentration of oxygen is needed during and after anaesthesia: • If the patient is very young, old, sick, or anaemic • If agents that cause cardio-respiratory depression, such as halothane, are used. Air already contains 20.9% oxygen, so oxygen enrichment with a draw-over system is a very economical method of providing oxygen. Adding only 1 litre per minute may increase the oxygen concentration in the inspired gas to 35–40%. With oxygen enrichment at 5 litres per minute, a concentration of 80% may be achieved. Industrial-grade oxygen, such as that used for welding, is perfectly acceptable for the enrichment of a draw-over system and has been widely used for this purpose. Oxygen Sources In practice, there are two possible sources of oxygen for medical purposes: • Cylinders: derived from liquid oxygen • Concentrators: which separate oxygen from air. -

Western Trauma Association Critical Decisions in Trauma: Penetrating Chest Trauma
WTA 2014 ALGORITHM Western Trauma Association Critical Decisions in Trauma: Penetrating chest trauma Riyad Karmy-Jones, MD, Nicholas Namias, MD, Raul Coimbra, MD, Ernest E. Moore, MD, 09/30/2020 on BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3Ypodx1mzGi19a2VIGqBjfv9YfiJtaGCC1/kUAcqLCxGtGta0WPrKjA== by http://journals.lww.com/jtrauma from Downloaded Martin Schreiber, MD, Robert McIntyre, Jr., MD, Martin Croce, MD, David H. Livingston, MD, Jason L. Sperry, MD, Ajai K. Malhotra, MD, and Walter L. Biffl, MD, Portland, Oregon Downloaded from http://journals.lww.com/jtrauma his is a recommended algorithm of the Western Trauma Historical Perspective TAssociation for the acute management of penetrating chest The precise incidence of penetrating chest injury, varies injury. Because of the paucity of recent prospective randomized depending on the urban environment and the nature of the trials on the evaluation and management of penetrating chest review. Overall, penetrating chest injuries account for 1% to injury, the current algorithms and recommendations are based 13% of trauma admissions, and acute exploration is required in by on available published cohort, observational and retrospective BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3Ypodx1mzGi19a2VIGqBjfv9YfiJtaGCC1/kUAcqLCxGtGta0WPrKjA== 5% to 15% of cases; exploration is required in 15% to 30% of studies, and the expert opinion of the Western Trauma Asso- patients who are unstable or in whom active hemorrhage is ciation members. The two algorithms should be reviewed in the suspected. Among patients managed by tube thoracostomy following sequence: Figure 1 for the management and damage- alone, complications including retained hemothorax, empy- control strategies in the unstable patient and Figure 2 for the ema, persistent air leak, and/or occult diaphragmatic injuries management and definitive repair strategies in the stable patient.