4 Transcription and Secretion Novel Regulator of Angiopoietin-Like Protein A
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Epha4/Tie2 Crosstalk Regulates Leptomeningeal Collateral Remodeling Following Ischemic Stroke
EphA4/Tie2 crosstalk regulates leptomeningeal collateral remodeling following ischemic stroke Benjamin Okyere, … , John B. Matson, Michelle H. Theus J Clin Invest. 2019. https://doi.org/10.1172/JCI131493. Research In-Press Preview Neuroscience Vascular biology Leptomeningeal anastomoses or pial collateral vessels play a critical role in cerebral blood flow (CBF) restoration following ischemic stroke. The magnitude of this adaptive response is postulated to be controlled by the endothelium, although the underlying molecular mechanisms remain under investigation. Here we demonstrated that endothelial genetic deletion, using EphA4f/f/Tie2-Cre and EphA4f/f/VeCahderin-CreERT2 mice and vessel painting strategies, implicated EphA4 receptor tyrosine kinase as a major suppressor of pial collateral remodeling, CBF and functional recovery following permanent middle cerebral artery occlusion. Pial collateral remodeling is limited by the cross talk between EphA4-Tie2 signaling in vascular endothelial cells, which is mediated through p-Akt regulation. Furthermore, peptide inhibition of EphA4 resulted in acceleration of the pial arteriogenic response. Our findings demonstrate EphA4 is a negative regulator of Tie2 receptor signaling which limits pial collateral arteriogenesis following cerebrovascular occlusion. Therapeutic targeting of EphA4 and/or Tie2 represents an attractive new strategy for improving collateral function, neural tissue health and functional recovery following ischemic stroke. Find the latest version: https://jci.me/131493/pdf 1 EphA4/Tie2 -

The Interplay Between Angiopoietin-Like Proteins and Adipose Tissue: Another Piece of the Relationship Between Adiposopathy and Cardiometabolic Diseases?
International Journal of Molecular Sciences Review The Interplay between Angiopoietin-Like Proteins and Adipose Tissue: Another Piece of the Relationship between Adiposopathy and Cardiometabolic Diseases? Simone Bini *,† , Laura D’Erasmo *,†, Alessia Di Costanzo, Ilenia Minicocci , Valeria Pecce and Marcello Arca Department of Translational and Precision Medicine, Sapienza University of Rome, Viale del Policlinico 155, 00185 Rome, Italy; [email protected] (A.D.C.); [email protected] (I.M.); [email protected] (V.P.); [email protected] (M.A.) * Correspondence: [email protected] (S.B.); [email protected] (L.D.) † These authors contributed equally to this work. Abstract: Angiopoietin-like proteins, namely ANGPTL3-4-8, are known as regulators of lipid metabolism. However, recent evidence points towards their involvement in the regulation of adipose tissue function. Alteration of adipose tissue functions (also called adiposopathy) is considered the main inducer of metabolic syndrome (MS) and its related complications. In this review, we intended to analyze available evidence derived from experimental and human investigations highlighting the contribution of ANGPTLs in the regulation of adipocyte metabolism, as well as their potential role in common cardiometabolic alterations associated with adiposopathy. We finally propose a model of ANGPTLs-based adipose tissue dysfunction, possibly linking abnormalities in the angiopoietins to the induction of adiposopathy and its related disorders. Keywords: adipose tissue; adiposopathy; brown adipose tissue; ANGPTL3; ANGPTL4; ANGPTL8 Citation: Bini, S.; D’Erasmo, L.; Di Costanzo, A.; Minicocci, I.; Pecce, V.; Arca, M. The Interplay between 1. Introduction Angiopoietin-Like Proteins and Adipose tissue (AT) is an important metabolic organ and accounts for up to 25% of Adipose Tissue: Another Piece of the healthy individuals’ weight. -
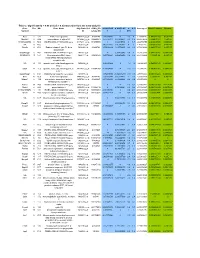
Table 2. Significant
Table 2. Significant (Q < 0.05 and |d | > 0.5) transcripts from the meta-analysis Gene Chr Mb Gene Name Affy ProbeSet cDNA_IDs d HAP/LAP d HAP/LAP d d IS Average d Ztest P values Q-value Symbol ID (study #5) 1 2 STS B2m 2 122 beta-2 microglobulin 1452428_a_at AI848245 1.75334941 4 3.2 4 3.2316485 1.07398E-09 5.69E-08 Man2b1 8 84.4 mannosidase 2, alpha B1 1416340_a_at H4049B01 3.75722111 3.87309653 2.1 1.6 2.84852656 5.32443E-07 1.58E-05 1110032A03Rik 9 50.9 RIKEN cDNA 1110032A03 gene 1417211_a_at H4035E05 4 1.66015788 4 1.7 2.82772795 2.94266E-05 0.000527 NA 9 48.5 --- 1456111_at 3.43701477 1.85785922 4 2 2.8237185 9.97969E-08 3.48E-06 Scn4b 9 45.3 Sodium channel, type IV, beta 1434008_at AI844796 3.79536664 1.63774235 3.3 2.3 2.75319499 1.48057E-08 6.21E-07 polypeptide Gadd45gip1 8 84.1 RIKEN cDNA 2310040G17 gene 1417619_at 4 3.38875643 1.4 2 2.69163229 8.84279E-06 0.0001904 BC056474 15 12.1 Mus musculus cDNA clone 1424117_at H3030A06 3.95752801 2.42838452 1.9 2.2 2.62132809 1.3344E-08 5.66E-07 MGC:67360 IMAGE:6823629, complete cds NA 4 153 guanine nucleotide binding protein, 1454696_at -3.46081884 -4 -1.3 -1.6 -2.6026947 8.58458E-05 0.0012617 beta 1 Gnb1 4 153 guanine nucleotide binding protein, 1417432_a_at H3094D02 -3.13334396 -4 -1.6 -1.7 -2.5946297 1.04542E-05 0.0002202 beta 1 Gadd45gip1 8 84.1 RAD23a homolog (S. -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

Single-Cell RNA Sequencing Demonstrates the Molecular and Cellular Reprogramming of Metastatic Lung Adenocarcinoma
ARTICLE https://doi.org/10.1038/s41467-020-16164-1 OPEN Single-cell RNA sequencing demonstrates the molecular and cellular reprogramming of metastatic lung adenocarcinoma Nayoung Kim 1,2,3,13, Hong Kwan Kim4,13, Kyungjong Lee 5,13, Yourae Hong 1,6, Jong Ho Cho4, Jung Won Choi7, Jung-Il Lee7, Yeon-Lim Suh8,BoMiKu9, Hye Hyeon Eum 1,2,3, Soyean Choi 1, Yoon-La Choi6,10,11, Je-Gun Joung1, Woong-Yang Park 1,2,6, Hyun Ae Jung12, Jong-Mu Sun12, Se-Hoon Lee12, ✉ ✉ Jin Seok Ahn12, Keunchil Park12, Myung-Ju Ahn 12 & Hae-Ock Lee 1,2,3,6 1234567890():,; Advanced metastatic cancer poses utmost clinical challenges and may present molecular and cellular features distinct from an early-stage cancer. Herein, we present single-cell tran- scriptome profiling of metastatic lung adenocarcinoma, the most prevalent histological lung cancer type diagnosed at stage IV in over 40% of all cases. From 208,506 cells populating the normal tissues or early to metastatic stage cancer in 44 patients, we identify a cancer cell subtype deviating from the normal differentiation trajectory and dominating the metastatic stage. In all stages, the stromal and immune cell dynamics reveal ontological and functional changes that create a pro-tumoral and immunosuppressive microenvironment. Normal resident myeloid cell populations are gradually replaced with monocyte-derived macrophages and dendritic cells, along with T-cell exhaustion. This extensive single-cell analysis enhances our understanding of molecular and cellular dynamics in metastatic lung cancer and reveals potential diagnostic and therapeutic targets in cancer-microenvironment interactions. 1 Samsung Genome Institute, Samsung Medical Center, Seoul 06351, Korea. -

Mesenchymal–Epithelial Interactions Involving Epiregulin in Tuberous Sclerosis Complex Hamartomas
Mesenchymal–epithelial interactions involving epiregulin in tuberous sclerosis complex hamartomas Shaowei Li*, Fumiko Takeuchi*, Ji-an Wang*, Qingyuan Fan*, Toshi Komurasaki†, Eric M. Billings‡, Gustavo Pacheco-Rodriguez‡, Joel Moss‡, and Thomas N. Darling*§ *Department of Dermatology, Uniformed Services University of the Health Sciences, 4301 Jones Bridge Road, Bethesda, MD 20814-4712; †Molecular Biology Laboratory, Molecular and Pharmacology Laboratories, Taisho Pharmaceutical Co., Ltd., 430-1 Yoshino-cho, Saitma-shi, Saitama 331-9530, Japan; and ‡Translational Medicine Branch, National Heart, Lung, and Blood Institute, National Institutes of Health, Building 10, Room 6D05, MSC 1590, Bethesda, MD 20892-1590 Communicated by Martha Vaughan, National Institutes of Health, Bethesda, MD, December 31, 2007 (received for review November 30, 2007) Patients with tuberous sclerosis complex (TSC) develop hamarto- Like other hamartomas, those in TSC skin contain abnormal mas containing biallelic inactivating mutations in either TSC1 or numbers of several types of cells. In the dermis, there are TSC2, resulting in mammalian target of rapamycin (mTOR) activa- increased numbers of large stellate fibroblasts, capillaries, and tion. Hamartomas overgrow epithelial and mesenchymal cells in dermal dendritic cells (6–9). The epidermis is acanthotic (i.e., TSC skin. The pathogenetic mechanisms for these changes had not thickened from increased numbers of keratinocytes in the spi- been investigated, and the existence or location of cells with nous layer). Acanthosis is pronounced in PFs and variable in AFs biallelic mutations (‘‘two-hit’’ cells) was unclear. We compared TSC (7, 8). The epidermis of treated AFs, several months after argon skin hamartomas (angiofibromas and periungual fibromas) with or CO2 laser surgery, no longer appears acanthotic (10, 11). -

Angiocrine Endothelium: from Physiology to Cancer Jennifer Pasquier1,2*, Pegah Ghiabi2, Lotf Chouchane3,4,5, Kais Razzouk1, Shahin Rafi3 and Arash Rafi1,2,3
Pasquier et al. J Transl Med (2020) 18:52 https://doi.org/10.1186/s12967-020-02244-9 Journal of Translational Medicine REVIEW Open Access Angiocrine endothelium: from physiology to cancer Jennifer Pasquier1,2*, Pegah Ghiabi2, Lotf Chouchane3,4,5, Kais Razzouk1, Shahin Rafi3 and Arash Rafi1,2,3 Abstract The concept of cancer as a cell-autonomous disease has been challenged by the wealth of knowledge gathered in the past decades on the importance of tumor microenvironment (TM) in cancer progression and metastasis. The sig- nifcance of endothelial cells (ECs) in this scenario was initially attributed to their role in vasculogenesis and angiogen- esis that is critical for tumor initiation and growth. Nevertheless, the identifcation of endothelial-derived angiocrine factors illustrated an alternative non-angiogenic function of ECs contributing to both physiological and pathological tissue development. Gene expression profling studies have demonstrated distinctive expression patterns in tumor- associated endothelial cells that imply a bilateral crosstalk between tumor and its endothelium. Recently, some of the molecular determinants of this reciprocal interaction have been identifed which are considered as potential targets for developing novel anti-angiocrine therapeutic strategies. Keywords: Angiocrine, Endothelium, Cancer, Cancer microenvironment, Angiogenesis Introduction of blood vessels in initiation of tumor growth and stated Metastatic disease accounts for about 90% of patient that in the absence of such angiogenesis, tumors can- mortality. Te difculty in controlling and eradicating not expand their mass or display a metastatic phenotype metastasis might be related to the heterotypic interaction [7]. Based on this theory, many investigators assumed of tumor and its microenvironment [1]. -

Cross-Talk Between ANGPTL4 Gene SNP Rs1044250 and Weight
Tong et al. J Transl Med (2021) 19:72 https://doi.org/10.1186/s12967-021-02739-z Journal of Translational Medicine RESEARCH Open Access Cross-talk between ANGPTL4 gene SNP Rs1044250 and weight management is a risk factor of metabolic syndrome Zhoujie Tong1†, Jie Peng2†, Hongtao Lan2, Wenwen Sai1, Yulin Li1, Jiaying Xie1, Yanmin Tan1, Wei Zhang1, Ming Zhong1 and Zhihao Wang2* Abstract Background: The prevalence of metabolic syndrome (Mets) is closely related to an increased incidence of cardiovas- cular events. Angiopoietin-like protein 4 (ANGPTL4) is contributory to the regulation of lipid metabolism, herein, may provide a target for gene-aimed therapy of Mets. This observational case control study was designed to elucidate the relationship between ANGPTL4 gene single nucleotide polymorphism (SNP) rs1044250 and the onset of Mets, and to explore the interaction between SNP rs1044250 and weight management on Mets. Methods: We have recruited 1018 Mets cases and 1029 controls in this study. The SNP rs1044250 was genotyped with blood samples, base-line information and Mets-related indicators were collected. A 5-year follow-up survey was carried out to track the lifestyle interventions and changes in Mets-related indicators. Results: ANGPTL4 gene SNP rs1044250 is an independent risk factor for increased waist circumference (OR 1.618, 95% CI [1.119–2.340]; p 0.011), elevated blood pressure (OR 1.323, 95% CI [1.002–1.747]; p 0.048), and Mets (OR 1.875, 95% CI [1.363–2.580];= p < 0.001). The follow-up survey shows that rs1044250 CC genotype= patients with weight gain have an increased number of Mets components (M [Q1, Q3]: CC 1 (0, 1), CT TT 0 [ 1, 1]; p 0.021); The interaction between SNP rs1044250 and weight management is a risk factor for increased+ systolic− blood= pressure (β 0.075, p < 0.001) and increased diastolic blood pressure (β 0.097, p < 0.001), the synergistic efect of weight management= and SNP rs1044250 is negative (S < 1). -

Functional Analysis of Somatic Mutations Affecting Receptor Tyrosine Kinase Family in Metastatic Colorectal Cancer
Author Manuscript Published OnlineFirst on March 29, 2019; DOI: 10.1158/1535-7163.MCT-18-0582 Author manuscripts have been peer reviewed and accepted for publication but have not yet been edited. Functional analysis of somatic mutations affecting receptor tyrosine kinase family in metastatic colorectal cancer Leslie Duplaquet1, Martin Figeac2, Frédéric Leprêtre2, Charline Frandemiche3,4, Céline Villenet2, Shéhérazade Sebda2, Nasrin Sarafan-Vasseur5, Mélanie Bénozène1, Audrey Vinchent1, Gautier Goormachtigh1, Laurence Wicquart6, Nathalie Rousseau3, Ludivine Beaussire5, Stéphanie Truant7, Pierre Michel8, Jean-Christophe Sabourin9, Françoise Galateau-Sallé10, Marie-Christine Copin1,6, Gérard Zalcman11, Yvan De Launoit1, Véronique Fafeur1 and David Tulasne1 1 Univ. Lille, CNRS, Institut Pasteur de Lille, UMR 8161 - M3T – Mechanisms of Tumorigenesis and Target Therapies, F-59000 Lille, France. 2 Univ. Lille, Plateau de génomique fonctionnelle et structurale, CHU Lille, F-59000 Lille, France 3 TCBN - Tumorothèque Caen Basse-Normandie, F-14000 Caen, France. 4 Réseau Régional de Cancérologie – OncoBasseNormandie – F14000 Caen – France. 5 Normandie Univ, UNIROUEN, Inserm U1245, IRON group, Rouen University Hospital, Normandy Centre for Genomic and Personalized Medicine, F-76000 Rouen, France. 6 Tumorothèque du C2RC de Lille, F-59037 Lille, France. 7 Department of Digestive Surgery and Transplantation, CHU Lille, Univ Lille, 2 Avenue Oscar Lambret, 59037, Lille Cedex, France. 8 Department of hepato-gastroenterology, Rouen University Hospital, Normandie Univ, UNIROUEN, Inserm U1245, IRON group, F-76000 Rouen, France. 9 Department of Pathology, Normandy University, INSERM 1245, Rouen University Hospital, F 76 000 Rouen, France. 10 Department of Pathology, MESOPATH-MESOBANK, Centre León Bérard, Lyon, France. 11 Thoracic Oncology Department, CIC1425/CLIP2 Paris-Nord, Hôpital Bichat-Claude Bernard, Paris, France. -
HCC and Cancer Mutated Genes Summarized in the Literature Gene Symbol Gene Name References*
HCC and cancer mutated genes summarized in the literature Gene symbol Gene name References* A2M Alpha-2-macroglobulin (4) ABL1 c-abl oncogene 1, receptor tyrosine kinase (4,5,22) ACBD7 Acyl-Coenzyme A binding domain containing 7 (23) ACTL6A Actin-like 6A (4,5) ACTL6B Actin-like 6B (4) ACVR1B Activin A receptor, type IB (21,22) ACVR2A Activin A receptor, type IIA (4,21) ADAM10 ADAM metallopeptidase domain 10 (5) ADAMTS9 ADAM metallopeptidase with thrombospondin type 1 motif, 9 (4) ADCY2 Adenylate cyclase 2 (brain) (26) AJUBA Ajuba LIM protein (21) AKAP9 A kinase (PRKA) anchor protein (yotiao) 9 (4) Akt AKT serine/threonine kinase (28) AKT1 v-akt murine thymoma viral oncogene homolog 1 (5,21,22) AKT2 v-akt murine thymoma viral oncogene homolog 2 (4) ALB Albumin (4) ALK Anaplastic lymphoma receptor tyrosine kinase (22) AMPH Amphiphysin (24) ANK3 Ankyrin 3, node of Ranvier (ankyrin G) (4) ANKRD12 Ankyrin repeat domain 12 (4) ANO1 Anoctamin 1, calcium activated chloride channel (4) APC Adenomatous polyposis coli (4,5,21,22,25,28) APOB Apolipoprotein B [including Ag(x) antigen] (4) AR Androgen receptor (5,21-23) ARAP1 ArfGAP with RhoGAP domain, ankyrin repeat and PH domain 1 (4) ARHGAP35 Rho GTPase activating protein 35 (21) ARID1A AT rich interactive domain 1A (SWI-like) (4,5,21,22,24,25,27,28) ARID1B AT rich interactive domain 1B (SWI1-like) (4,5,22) ARID2 AT rich interactive domain 2 (ARID, RFX-like) (4,5,22,24,25,27,28) ARID4A AT rich interactive domain 4A (RBP1-like) (28) ARID5B AT rich interactive domain 5B (MRF1-like) (21) ASPM Asp (abnormal -

Stromal Cell Interactions Mediated by Hypoxia-Inducible Factors Promote Angiogenesis, Lymphangiogenesis, and Metastasis
Oncogene (2013) 32, 4057–4063 & 2013 Macmillan Publishers Limited All rights reserved 0950-9232/13 www.nature.com/onc REVIEW Cancer–stromal cell interactions mediated by hypoxia-inducible factors promote angiogenesis, lymphangiogenesis, and metastasis GL Semenza Interactions between cancer cells and stromal cells, including blood vessel endothelial cells (BECs), lymphatic vessel endothelial cells (LECs), bone marrow-derived angiogenic cells (BMDACs) and other bone marrow-derived cells (BMDCs) play important roles in cancer progression. Intratumoral hypoxia, which affects both cancer and stromal cells, is associated with a significantly increased risk of metastasis and mortality in many human cancers. Recent studies have begun to delineate the molecular mechanisms underlying the effect of intratumoral hypoxia on cancer progression. Reduced O2 availability induces the activity of hypoxia- inducible factors (HIFs), which activate the transcription of target genes encoding proteins that play important roles in many critical aspects of cancer biology. Included among these are secreted factors, including angiopoietin 2, angiopoietin-like 4, placental growth factor, platelet-derived growth factor B, stem cell factor (kit ligand), stromal-derived factor 1, and vascular endothelial growth factor. These factors are produced by hypoxic cancer cells and directly mediate functional interactions with BECs, LECs, BMDACs and other BMDCs that promote angiogenesis, lymphangiogenesis, and metastasis. In addition, lysyl oxidase (LOX) and LOX-like proteins, -

Altiratinib Inhibits Tumor Growth, Invasion, Angiogenesis, and Microenvironment-Mediated Drug Resistance Via Balanced Inhibition of MET, TIE2, and VEGFR2 Bryan D
Published OnlineFirst August 18, 2015; DOI: 10.1158/1535-7163.MCT-14-1105 Small Molecule Therapeutics Molecular Cancer Therapeutics Altiratinib Inhibits Tumor Growth, Invasion, Angiogenesis, and Microenvironment-Mediated Drug Resistance via Balanced Inhibition of MET, TIE2, and VEGFR2 Bryan D. Smith1, Michael D. Kaufman1, Cynthia B. Leary1, Benjamin A. Turner1, Scott C. Wise1, Yu Mi Ahn1, R. John Booth1, Timothy M. Caldwell1, Carol L. Ensinger1, Molly M. Hood1, Wei-Ping Lu1, Tristan W. Patt1, William C. Patt1, Thomas J. Rutkoski1, Thiwanka Samarakoon1, Hanumaiah Telikepalli1, Lakshminarayana Vogeti1, Subha Vogeti1, Karen M. Yates1, Lawrence Chun2, Lance J. Stewart2, Michael Clare1, and Daniel L. Flynn1,3 Abstract Altiratinib (DCC-2701) was designed based on the rationale of wild-type and mutated forms, in vitro and in vivo. Through its engineering a single therapeutic agent able to address multiple balanced inhibitory potency versus MET, TIE2, and VEGFR2, hallmarks of cancer (1). Specifically, altiratinib inhibits not only altiratinib provides an agent that inhibits three major evasive mechanisms of tumor initiation and progression, but also drug (re)vascularization and resistance pathways (HGF, ANG, and resistance mechanisms in the tumor and microenvironment VEGF) and blocks tumor invasion and metastasis. Altiratinib through balanced inhibition of MET, TIE2 (TEK), and VEGFR2 exhibits properties amenable to oral administration and exhibits (KDR) kinases. This profile was achieved by optimizing binding substantial blood–brain barrier penetration, an attribute of into the switch control pocket of all three kinases, inducing type II significance for eventual treatment of brain cancers and brain inactive conformations. Altiratinib durably inhibits MET, both metastases. Mol Cancer Ther; 14(9); 1–12.