Pulmonary Embolism 2
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
X-Ray Interpretation
Objectives Describe a systematic method for interpretation of chest and abdomen x-rays List findings to accurately identify common X-ray Interpretation pathology in chest & abdomen x-rays Describe a systematic method to approach the Denise Ramponi, DNP, FNP-C, ENP-BC, FAANP, FAEN important components in interpretation of upper & lower extremity x-rays Chest X-ray: Standard Views Lateral Film Postero-anterior (PA): (LAT) view can determine th On inspiration – diaphragm descends to 10 rib the anterior-posterior posteriorly structures along the axis of the body Normal LAT film Counting Ribs AP View - Portable http://www.lumen.luc.edu/lumen/MedEd/medicine/pulmonar/cxr/cxr_f.htm When the patient is unable to tolerate routine views with pts sitting or supine No participation from the patient Film is against the patient's back (supine) 1 Consolidation, Atelectasis, Chest radiograph Interstitial involvement Consolidation - any pathologic process that fills the alveoli with Left and right heart fluid, pus, blood, cells or other borders well defined substances Interstitial - involvement of the Both hemidiaphragms supporting tissue of the lung visible to midline parenchyma resulting in fine or coarse reticular opacities Right - higher Atelectasis - collapse of a part of Heart less than 50% of the lung due to a decrease in the amount of air resulting in volume diameter of the chest loss and increased density. Infiltrate, Consolidation vs. Congestive Heart Failure Atelectasis Fluid leaking into interstitium Kerley B 2 Kerley B lines Prominent interstitial markings Kerley lines Magnified CXR Cardiomyopathy & interstitial pulmonary edema Short 1-2 cm white lines at lung periphery horizontal to pleural surface Distended interlobular septa - secondary to interstitial edema. -

Diagnosing Pulmonary Embolism M Riedel
309 Postgrad Med J: first published as 10.1136/pgmj.2003.007955 on 10 June 2004. Downloaded from REVIEW Diagnosing pulmonary embolism M Riedel ............................................................................................................................... Postgrad Med J 2004;80:309–319. doi: 10.1136/pgmj.2003.007955 Objective testing for pulmonary embolism is necessary, embolism have a low long term risk of subse- quent VTE.2 5–7 because clinical assessment alone is unreliable and the consequences of misdiagnosis are serious. No single test RISK FACTORS AND RISK has ideal properties (100% sensitivity and specificity, no STRATIFICATION risk, low cost). Pulmonary angiography is regarded as the The factors predisposing to VTE broadly fit Virchow’s triad of venous stasis, injury to the final arbiter but is ill suited for diagnosing a disease vein wall, and enhanced coagulability of the present in only a third of patients in whom it is suspected. blood (box 1). The identification of risk factors Some tests are good for confirmation and some for aids clinical diagnosis of VTE and guides decisions about repeat testing in borderline exclusion of embolism; others are able to do both but are cases. Primary ‘‘thrombophilic’’ abnormalities often non-diagnostic. For optimal efficiency, choice of the need to interact with acquired risk factors before initial test should be guided by clinical assessment of the thrombosis occurs; they are usually discovered after the thromboembolic event. Therefore, the likelihood of embolism and by patient characteristics that risk of VTE is best assessed by recognising the may influence test accuracy. Standardised clinical presence of known ‘‘clinical’’ risk factors. estimates can be used to give a pre-test probability to However, investigations for thrombophilic dis- orders at follow up should be considered in those assess, after appropriate objective testing, the post-test without another apparent explanation. -

Chest and Abdominal Radiograph 101
Chest and Abdominal Radiograph 101 Ketsia Pierre MD, MSCI July 16, 2010 Objectives • Chest radiograph – Approach to interpreting chest films – Lines/tubes – Pneumothorax/pneumomediastinum/pneumopericar dium – Pleural effusion – Pulmonary edema • Abdominal radiograph – Tubes – Bowel gas pattern • Ileus • Bowel obstruction – Pneumoperitoneum First things first • Turn off stray lights, optimize room lighting • Patient Data – Correct patient – Patient history – Look at old films • Routine Technique: AP/PA, exposure, rotation, supine or erect Approach to Reading a Chest Film • Identify tubes and lines • Airway: trachea midline or deviated, caliber change, bronchial cut off • Cardiac silhouette: Normal/enlarged • Mediastinum • Lungs: volumes, abnormal opacity or lucency • Pulmonary vessels • Hila: masses, lymphadenopathy • Pleura: effusion, thickening, calcification • Bones/soft tissues (four corners) Anatomy of a PA Chest Film TUBES Endotracheal Tubes Ideal location for ETT Is 5 +/‐ 2 cm from carina ‐Normal ETT excursion with flexion and extension of neck 2 cm. ETT at carina Right mainstem Intubation ‐Right mainstem intubation with left basilar atelectasis. ETT too high Other tubes to consider DHT down right mainstem DHT down left mainstem NGT with tip at GE junction CENTRAL LINES Central Venous Line Ideal location for tip of central venous line is within superior vena cava. ‐ Risk of thrombosis decreased in central veins. ‐ Catheter position within atrium increases risk of perforation Acceptable central line positions • Zone A –distal SVC/superior atriocaval junction. • Zone B – proximal SVC • Zone C –left brachiocephalic vein. Right subclavian central venous catheter directed cephalad into IJ Where is this tip? Hemiazygous Or this one? Right vertebral artery Pulmonary Arterial Catheter Ideal location for tip of PA catheter within mediastinal shadow. -

TB: Recognizing It on a Chest X-Ray
TB: Recognizing it on a Chest X‐Ray Disclosures • Grant support from Michigan Department of Community Health – Despite conflict of interest I still want to: – There’s enough TB for job security. Objectives • You will – Be able to identify major structures on a normal chest x‐ray – Identify and correctly name CXR abnormalities seen commonly in TB – Recognize chest x‐ray patterns that suggest TB & when you find them you will Basics of Diagnostic X‐ray Physics • X‐rays are directed at the . patient and variably absorbed – When not absorbed • Pass through patient & strike the x‐ray film or – When completely absorbed • Don’t strike x‐ray film or – When scattered • Some strike the x‐ray film Absorption Shade / Density • Absorption depends • Whitest = Most Dense on the – Metal – Energy of the x‐ray beam – Contrast material (dye) – Density of the tissue – Calcium – Bone – Water – Soft Tissue – Fat – Air / Gas • Blackest = Least Dense Normal Frontal Chest X‐ray: Posterior Anterior Note silhouette formed by • lung adjacent to heart • lung adjacent to diaphragm Silhouette Sign Lifeinthefastlane.com Normal Lateral Chest X‐ray Normal PA & Lateral X‐ray: Hilum Hilum –Major bronchi, Pulmonary veins & arteries, Lymph nodes at the root of the lung. Normal PA & Lateral X‐ray: Mediastinum Mediastinum –Central chest organs (not lungs) – Heart, Aorta, Trachea, Thymus, Esophagus, Lymph nodes, Nerves (Between 2 pleuras or linings of the lungs) Normal PA & Lateral X‐ray: Apex • Apex of lung – Area of lung above the level of the anterior end of the 1st rib Wink -

Chest X-Ray Made Ridiculously Plain, Basic, Or Uncomplicated in Form, Nature, Or Design; Without Much Decoration Or Ornamentation
Chest X-Ray Made ridiculously plain, basic, or uncomplicated in form, nature, or design; without much decoration or ornamentation Steve Cohen, MD, PA-C Associate Professor, Dept. of Surgery & Director of PA Clinical Education Florida International University Really Simple Step 3 The END, Bye-Bye Thanks for Coming! Posterior Anterior (PA) Workhorse PA Films Properties • X-ray is a “NEGATIVE” – Light is dark (ex. Air) – Less x-ray get through = shows white (eg. bone) • Beam is divergent – Posterior elements magnified – Dense posterior elements may hide anterior structures What can you see on CXR? 4 3 2 5 5 1 3 6 What are we looking at? Quickie Anatomy What are we looking at? Quickie Anatomy Airway • Film “Position” – Patients left on your right • Trachea – Midline (mostly) – Open • Mostly equal from wall to wall Ribs • Rib count – Extent quality • Bony integrity – Fracture, dislocation • Left first rib – Posterior at top • Beam hits first – Anterior at bottom Ribs • Use 1st rib to count • Posterior ribs usually most visible – beam hits first • Seen here = 8 ribs • Clavicles – Integrity (fx, displacement) – Assessing midline • Same distance from trachea Diaphragm – Stomach Bubble • Right higher than left diaphragm – Liver • Costophrenic angles – Fluid “haziness” • Air under diaphragm • Stomach bubble – variable Left Vessels and Heart • Subclavian Artery • Coming off arch • Aortic Arch • Pulmonary Artery • Returning to heart • Left Atrium • Left Ventricle Right Vessels and Heart • Ascending Aorta • Leaving heart • Superior Vena Cava • Entering -
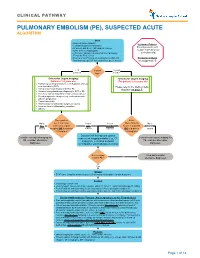
Pulmonary Embolism (Pe), Suspected Acute Algorithm
CLINICAL PATHWAY PULMONARY EMBOLISM (PE), SUSPECTED ACUTE ALGORITHM Start · Room air pulse oximetry Inclusion Criteria: · Consider supplemental oxygen · IV access and STAT CBC and DIC screen Patient presents with · Urine β-HCG, if appropriate suspected Pulmonary · CXR (PA + lateral), EKG and call the Cardiology Embolism (PE) Fellow for Echo review · Review criteria* for urgent imaging for possible PE Exclusion Criteria based on age-specific risk factors (see green boxes) No suspected PE < 18 Patient 18 years years old age? or older *Criteria for Urgent Imaging: *Criteria for Urgent Imaging: Patients < 18 years old For patients ≥ 18 years old · Painful leg swelling or known recent diagnosis of deep vein thrombosis (DVT) Please refer to the Wells Criteria · Family or personal history of DVT or PE Algorithm on page 7. · Known clotting disorder predisposing to DVT or PE · Recent or current indwelling central venous catheter · Elevated systemic estrogen (e.g., oral contraceptive pill use, pregnancy) · Recent immobility · Recent major or orthopedic surgery or trauma · Acute or chronic inflammatory condition · Obesity Does patient Is the No to meet 1 or more Yes to Yes to Wells Criteria No to ALL criteria for urgent ANY EITHER Score > 4 points BOTH criteria imaging OR is d-dimer criteria criterion OR is d-dimer criteria > 0.5ug/mL? > 0.5ug/mL? Discuss CXR findings and optimal Consider non-urgent imaging for subsequent imaging modality (e.g., CT Consider non-urgent imaging for PE, consider alternative angiogram, ventilation perfusion PE, consider -

CHEST RADIOLOGY: Goals and Objectives
Harlem Hospital Center Department of Radiology Residency Training Program CHEST RADIOLOGY: Goals and Objectives ROTATION 1 (Radiology Years 1): Resident responsibilities: • ED chest CTs • Inpatient and outpatient plain films including the portable intensive care unit radiographs • Consultations with referring clinicians MEDICAL KNOWLEDGE: • Residents must demonstrate knowledge about established and evolving biomedical, clinical, and cognitive sciences and the application of this knowledge to patient care. At the end of the rotation, the resident should be able to: • Identify normal radiographic and CT anatomy of the chest • Identify and describe common variants of normal, including aging changes. • Demonstrate a basic knowledge of radiographic interpretation of atelectasis, pulmonary infection, congestive heart failure, pleural effusion and common neoplastic diseases of the chest • Identify the common radiologic manifestation of thoracic trauma, including widened mediastinum, signs of aortic laceration, pulmonary contusion/laceration, esophageal and diaphragmatic rupture. • Know the expected postoperative appearance in patients s/p thoracic surgery and the expected location of the life support and monitoring devices on chest radiographs of critically ill patients (intensive care radiology); be able to recognize malpositioned devices. • Identify cardiac enlargement and know the radiographic appearance of the dilated right vs. left atria and right vs. left ventricles, and pulmonary vascular congestion • Recognize common life-threatening -

Chapter 17 Dyspnea Sabina Braithwaite and Debra Perina
Chapter 17 Dyspnea Sabina Braithwaite and Debra Perina ■ PERSPECTIVE Pathophysiology Dyspnea is the term applied to the sensation of breathlessness The actual mechanisms responsible for dyspnea are unknown. and the patient’s reaction to that sensation. It is an uncomfort- Normal breathing is controlled both centrally by the respira- able awareness of breathing difficulties that in the extreme tory control center in the medulla oblongata, as well as periph- manifests as “air hunger.” Dyspnea is often ill defined by erally by chemoreceptors located near the carotid bodies, and patients, who may describe the feeling as shortness of breath, mechanoreceptors in the diaphragm and skeletal muscles.3 chest tightness, or difficulty breathing. Dyspnea results Any imbalance between these sites is perceived as dyspnea. from a variety of conditions, ranging from nonurgent to life- This imbalance generally results from ventilatory demand threatening. Neither the clinical severity nor the patient’s per- being greater than capacity.4 ception correlates well with the seriousness of underlying The perception and sensation of dyspnea are believed to pathology and may be affected by emotions, behavioral and occur by one or more of the following mechanisms: increased cultural influences, and external stimuli.1,2 work of breathing, such as the increased lung resistance or The following terms may be used in the assessment of the decreased compliance that occurs with asthma or chronic dyspneic patient: obstructive pulmonary disease (COPD), or increased respira- tory drive, such as results from severe hypoxemia, acidosis, or Tachypnea: A respiratory rate greater than normal. Normal rates centrally acting stimuli (toxins, central nervous system events). -

Mayo Clinic Medical Manual This Page Intentionally Left Blank Mayo Clinic Medical Manual
Mayo Clinic Medical Manual This page intentionally left blank Mayo Clinic Medical Manual Editors Guilherme H. M. Oliveira, M.D. Gillian C. Nesbitt, M.D. Joseph G. Murphy, M.D. MAYO CLINIC SCIENTIFIC PRESS TAYLOR & FRANCIS GROUP ISBN 0849390877 The triple-shield Mayo logo and the words MAYO, MAYO CLINIC, and MAYO CLINIC SCIENTIFIC PRESS are marks of Mayo Foundation for Medical Education and Research. ©2006 by Mayo Foundation for Medical Education and Research. All rights reserved. This book is protected by copyright. No part of it may be reproduced, stored in a retrieval system, or transmitted, in any form or by any means—electronic, mechanical, photocopying, record- ing, or otherwise—without the prior written consent of the copyright holder, except for brief quotations embodied in critical articles and reviews. Inquiries should be addressed to Scientific Publications, Plummer 10, Mayo Clinic, 200 First Street SW, Rochester, MN 55905. For order inquiries, contact Taylor & Francis Group, 6000 Broken Sound Parkway NW, Suite #300, Boca Raton, FL 33487. www.taylorandfrancis.com Catalog record is available from the Library of Congress. Care has been taken to confirm the accuracy of the information presented and to describe generally accepted practices. However, the authors, editors, and publisher are not responsible for errors or omissions or for any consequences from application of the information in this book and make no warranty, express or implied, with respect to the contents of the publication. This book should not be relied on apart from the advice of a qualified health care provider. The authors, editors, and publisher have exerted efforts to ensure that drug selection and dosage set forth in this text are in accordance with current recommendations and practice at the time of publication. -

Pleural Effusion, Hypovascularity in Lung Zone (Westermark’S Sign) & Pyramid Shape Infiltrate with Peak Directed to Hilus (Hampton’S Hump)
Author(s): Michele M. Nypaver, MD, 2011 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/ We have reviewed this material in accordance with U.S. Copyright Law and have tried to maximize your ability to use, share, and adapt it. Copyright holders of content included in this material should contact [email protected] with any questions, corrections, or clarification regarding the use of content. For more information about how to cite these materials visit http://open.umich.edu/privacy-and-terms-use. Any medical information in this material is intended to inform and educate and is not a tool for self-diagnosis or a replacement for medical evaluation, advice, diagnosis or treatment by a healthcare professional. Please speak to your physician if you have questions about your medical condition. Viewer discretion is advised: Some medical content is graphic and may not be suitable for all viewers. Citation Key for more information see: http://open.umich.edu/wiki/CitationPolicy Use + Share + Adapt { Content the copyright holder, author, or law permits you to use, share and adapt. } Public Domain – Government: Works that are produced by the U.S. Government. (17 USC § 105) Public Domain – Expired: Works that are no longer protected due to an expired copyright term. Public Domain – Self Dedicated: Works that a copyright holder has dedicated to the public domain. Creative Commons – Zero Waiver Creative Commons – Attribution License Creative Commons – Attribution Share Alike License Creative Commons – Attribution Noncommercial License Creative Commons – Attribution Noncommercial Share Alike License GNU – Free Documentation License Make Your Own Assessment { Content Open.Michigan believes can be used, shared, and adapted because it is ineligible for copyright. -

Redalyc.POSTERS EXPOSTOS
Revista Portuguesa de Pneumología ISSN: 0873-2159 [email protected] Sociedade Portuguesa de Pneumologia Portugal POSTERS EXPOSTOS Revista Portuguesa de Pneumología, vol. 23, núm. 3, noviembre, 2017 Sociedade Portuguesa de Pneumologia Lisboa, Portugal Disponível em: http://www.redalyc.org/articulo.oa?id=169753668003 Como citar este artigo Número completo Sistema de Informação Científica Mais artigos Rede de Revistas Científicas da América Latina, Caribe , Espanha e Portugal Home da revista no Redalyc Projeto acadêmico sem fins lucrativos desenvolvido no âmbito da iniciativa Acesso Aberto Document downloaded from http://www.elsevier.es, day 06/12/2017. This copy is for personal use. Any transmission of this document by any media or format is strictly prohibited. POSTERS EXPOSTOS PE 001 PE 002 A PLEASANT FINDING MALIGNANT CHEST PAIN A Pais, AI Coutinho, M Cardoso, A Pignatelli, C Bárbara A Pais, C Pereira, C Antunes, V Pereira, AI Coutinho, A Feliciano, Centro Hospitalar de Lisboa Norte C Quadros, A Ribeiro, L Carvalho, C Bárbara Centro Hospitalar de Lisboa Norte Key-words: mass, debridement, hamartoma Key-words: pain, S100, sarcoma 37-year-old male patient, salesman. Sporadic smoker. With a past history of allergic rhinitis and chronic gastritis. With no usual 26-year-old male patient, supermarket employee. Smoker of 10 medication. In January 2017, he was diagnosed with a respiratory pack-year. Past history of bronchial asthma in childhood. No rel - infection, having completed ten days of empirical antibiotic ther - evant family history. Without usual ambulatory medication. With apy with amoxicillin / clavulanic acid, with clinical improvement. a history of dry cough and chest pain in the posterior region of In May 2017, he underwent thoracic xray, which revealed homoge - the left hemithorax, for about two years, having had at that time, neous opacity of triangular morphology in the middle lobe of the chest X-ray without pathological findings, and the clinical picture right lung. -

Pneumonia (CAP)
肺實質化病變與肺塌陷 胸腔內科周百謙醫師 Dr. Pai-chien Chou MD PhD Department of Thoracic Medicine Taipei Medical University Hospital Chest X-ray • P-A view • Lateral view • Oblique view • Lordotic view • Expiratory film • Decubitus view • Overpenetrated grid film The Elements of a chest x-ray (CXR) • The Broncho-vascular markings in the lung • The borders of the heart • The contours of the mediastinum and pleural space • The ribs and spine Segmental anatomy Segmental Anatomy Cardiomediastinal outlines on Chest X-ray Density of image ◆ Gas ◆ Water ◆ Fat ◆ Metal and bone ◆ Thinking of pathogenesis Basic thinking of a lesion on Chest X-ray ◆ Size ◆ Location (Silhouette sign) – Anterior, posterior – Which lobe is involved ◆ Intrapulmonary (Air bronchogram sign) ◆ Extrapulmonary (Incomplete border sign) Infiltrate in the lungs • Fluid accumulates in lung, predominate in the alveolar (airspace) compartment or the interstitial compartment. interstitial compartment Lymphatic compartment Alveolar unit Vascular unit Air space opacification The opacification is caused by fluid or solid material within the airways that causes a difference in the relative attenuation of the lung: • transudate, e.g. pulmonary edema secondary to heart failure • pus, e.g. bacterial pneumonia • blood, e.g. pulmonary hemorrhage • cells, e.g. bronchoalveolar carcinoma • protein, e.g. alveolar proteinosis • fat, e.g. lipoid pneumonia • gastric contents, e.g. aspiration pneumonia • water, e.g. drowning When considering the likely causes of airspace opacification, it is useful to determine chronicity