Sizing and Centering the Capsulorhexis by WILLIAM BOND, MD; BROCK K
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

5267830313.Pdf
DR. AGARWAL’S EYE HOSPITAL LIMITED 1 CONTENTS Page No. Company Information 2 Financial Highlights 3 Notice to Shareholders 4 Directors’ Report 11 Management Discussion and Analysis 15 Corporate Governance Report 15 Auditors’ Certificate on Corporate Governance 26 Independent Auditors’ Report to the Members 28 Secretarial Compliance Certificate 32 Balance Sheet 36 Profit and Loss Account 37 Cash Flow Statement 38 Notes on Financial Statement 41 Attendance Slip and Proxy Form 59 2 DR. AGARWAL’S EYE HOSPITAL LIMITED COMPANY INFORMATION Board of Directors Dr. Amar Agarwal (Chairman cum Managing Director) Dr. Athiya Agarwal (Wholetime Director) Dr. Adil Agarwal (Wholetime Director) Dr. Anosh Agarwal (Wholetime Director) Dr. Jasvinder Singh Saroya Mr. M. R. G. Apparao Mr. Prabhat Toshniwal Mr. Sanjay Anand Auditors M/s. M. K. Dandeker & Co. Chartered Accountants, 244, Angappa Naicken Street, Chennai 600 001. Registered Office 19 (Old No.13), Cathedral Road, Chennai 600 086. Bankers (1) State Bank of India, Gopalapuram Branch, Chennai - 600 086. (2) State Bank of India, Industrial Finance Branch, Chennai 600 002. Share Transfer Agents Integrated Enterprises (India) Ltd. 2nd Floor, Kences Towers, No.1, Ramakrishna Street, North Usman Road, T.Nagar, Chennai 600 017. Tel: 2814 0801-03 Email: [email protected] DR. AGARWAL’S EYE HOSPITAL LIMITED HOSPITAL EYE AGARWAL’S DR. Financial Highlights Rs. in crore For the year ended 2012-13 2011-12 2010-11 2009-10 2008-09 2007-08 2006-07 2005-06 2004-05 2003-04 Total Income 109.73 105.68 104.01 -

Utah Eye Centers Now Offers the Latest Advance in Laser Eye Surgery
Mark G. Ballif, M.D. Scott O. Sykes, M.D. Michael B. Wilcox, M.D. John D. Armstrong, M.D. Robert W. Wing, M.D., FACS Keith Linford, O.D. Jed T. Poll, M.D. Claron D. Alldredge, M.D. Devin B. Farr, O.D. Michael L. Bullard, M.D. Court R. Wilkins, O.D. Utah Eye Centers Now Offers the Latest Advance In Laser Eye Surgery The New VICTUS® Femtosecond Laser Platform, from Bausch + Lomb is Designed to Support Positive Patient Experience and Outstanding Visual Results in Cataract and LASIK Procedures FOR RELEASE April 17, 2015 Ogden, Utah— Utah Eye Centers, the leading comprehensive ophthalmology practice in northern Utah, announced today the Mount Ogden facility now offers eye surgery for cataracts and LASIK with an advanced laser system, the VICTUS® femtosecond laser platform. They are the only practice north of Salt Lake City with a fixed site femtosecond laser for cataracts and LASIK. The versatile VICTUS platform is designed to provide greater precision compared to manual cataract and LASIK surgery techniques. According to Scott Sykes, M.D., the Victus laser is the only laser approved to perform treatments for both cataract and LASIK surgeries. "With the VICTUS platform, we are able to automate some of the steps that we have commonly performed manually," said Mark Ballif, M.D. "While we have performed thousands of successful cataract and LASIK surgeries, the VICTUS platform helps us to improve the procedures to give our patients the best outcomes possible." The VICTUS platform features a sophisticated, curved patient interface with computer-monitored pressure sensors designed to provide comfort during the procedure. -

Nd:YAG CAPS ULOTOMY AS a PRIMARY TREATMENT
PSEUDOPHAKIC MALIGNANT GLAUCOMA: Nd:YAG CAPS ULOTOMY AS A PRIMARY TREATMENT B. C. LITTLE and R. A. HITCHINGS London SUMMARY anisms of ciliolenticular block of aqueous flow leading to Malignant glaucoma is one of the most serious but rare the misdirection of aqueous posteriorly into or in front of complications of anterior segment surgery. It is best the vitreous gel leading to the characteristic diffuse shal known following trabeculectomy but has been reported lowing of the anterior chamber accompanied by a precipi following a wide variety of anterior segment procedures tous rise in intraocular pressure. The mechanistic including extracapsular cataract extraction with pos understanding of its pathogenesis has led to the use of the terior chamber lens implantation. It is notoriously refrac synonyms 'ciliolenticular block',7 'ciliovitreal block', tory to medical treatment alone and surgical intervention 'iridovitreal block',8 'aqueous misdirection' and 'aqueous has had only limited success. An additional treatment diversion syndrome'. Although probably more precise option in pseudophakic eyes is that of peripheral these are unlikely to succeed the original term 'malignant Nd:YAG posterior capsulotomy, which is minimally glaucoma', which more accurately evokes the fulminant invasive and can re-establish forward flow of posteriorly nature of the condition as well as the justified anxiety asso misdirected aqueous through into the drainage angle of ciated with it. Medical treatment alone is rarely successful the anterior chamber. We report our experience of seven in establishing control of the intraocular pressure.2•8 Pars cases of malignant glaucoma in pseudophakic eyes and of plana vitrectomy has been used in the surgical managment the successful use of Nd:YAG posterior capsulotomy in of malignant glaucoma with some definite but limited suc re-establishing pressure control in' five of these eyes, cess in phakic as well as pseudophakic eyes.9•10 thereby obviating the need for acute surgical However, when malignant glaucoma develops in intervention. -

Outcome of Lens Aspiration and Intraocular Lens Implantation in Children Aged 5 Years and Under
540 Br J Ophthalmol 2001;85:540–542 Outcome of lens aspiration and intraocular lens implantation in children aged 5 years and under Lorraine Cassidy, Jugnoo Rahi, Ken Nischal, Isabelle Russell-Eggitt, David Taylor Abstract However, final refraction is variable, such that Aims—To determine the visual outcome emmetropia in adulthood cannot be guaran- and complications of lens aspiration with teed, as there are insuYcient long term studies. intraocular lens implantation in children There have been many reports of the visual aged 5 years and under. outcome and complications of posterior cham- Methods—The hospital notes of all chil- ber lens implantation in children.4–12 Most of dren aged 5 years and under, who had these have been based on older children, undergone lens aspiration with intraocu- secondary lens implants, a high number of lar lens implantation between January traumatic cataracts, and many have reported 1994 and September 1998, and for whom early outcome. We report visual outcome and follow up data of at least 1 year were avail- complications of primary IOL implantation at able, were reviewed. least 1 year after surgery, in children aged 5 Results—Of 50 children who underwent years and under, with mainly congenital or surgery, 45 were eligible based on the juvenile lens opacities. follow up criteria. 34 children had bilat- eral cataracts and, of these, 30 had surgery Methods on both eyes. Cataract was unilateral in 11 SUBJECTS cases; thus, 75 eyes of 45 children had sur- We reviewed the notes of all children aged 5 gery. Cataracts were congenital in 28 years and under, who had undergone lens aspi- cases, juvenile in 16, and traumatic in one ration with primary posterior chamber in- case. -

Laser Learning Lecture and Lab: YAG Caps, LPI, And
5/9/17 Overview Laser Learning Lecture and Lab: • Why we use lasers YAG caps, LPI, and SLT • YAG capsulotomy • Laser Peripheral Iridotomy (LPI or PI) Aaron McNulty, O.D., F.A.A.O. • Argon Laser Peripheral Iridoplasty (ALPI) Nate Lighthizer, O.D., F.A.A.O. • Argon Laser Trabeculoplasty (ALT) • Selective Laser Trabeculoplasty (SLT) • Other Laser Trabeculoplasty Why do we use lasers? Posterior Capsular Opacification (PCO) • Vision is decreased from PCO following cataract surgery • Lens capsular bag has an anterior and • Narrow angles/angle closure posterior surface • Glaucoma is progressing in a pt on max meds – Anterior surface usually removed w/ capsulorhexis – Something else needs to be done – Surgery not wanted yet • PCO is the formation of a cloudy membrane • Compliance issues on the posterior surface of the capsular bag • Cost issues following ECCE • Convenience issues – AKA: Secondary cataract • Doctor preference PCO YAG Laser • Incidence: • Nd: YAG laser – Most common complication of post ECCE – Neodymium: Yttrium aluminum garnet laser – 10-80% of eyes following cataract surgery – Can form anywhere from a few days to years post surgery • Tissue interaction: Photodisruptive laser – Younger patients higher risk of PCO – High light energy levels cause the tissues to be reduced – IOL’s to plasma, disintegrating the tissue • Silicone > acrylic – A large amount of energy is delivered into very small focal spots in a very brief duration of time • Prevention: • 4 nsec – – Capsulotomy during surgery No thermal reaction/No coagulation when bv’s are hit – Posterior capsular polishing – Pigment independent* 1 5/9/17 YAG Cap Risks, Complications, YAG Cap Pre-op Exam Contraindications • Visual acuity, glare testing, PAM/Heine lambda Contraindications Risks/complications – Vision 20/30 or worse 1. -

Agarwal AR 19.Indd
Contents Page No Chairman’s Desk 3 Board of Directors 5 A Word from Chairman - Clinical Board 9 Industrial Update 12 Notice to Shareholders 15 Directors’ Report 29 Management Discussions and Analysis Report 46 Corporate Governance Report 50 A word from the CFO 61 Financial Highlights 62 Independent Auditor’s Report 65 Balance Sheet as at 31st March, 2019 72 Statement of Profit and Loss for the year ended 31st March 2019 73 Statement of changes in equity for the year ended 31st March 2019 74 Cash Flow Statement as on 31st March 2019 75 Notes Forming Part of the Financial Statements for the year ended 76 31st March 2019 Press Clippings 120 NABH Accredited 126 Route map to AGM venue 128 CORPORATE Chairman’s INFORMATION Desk DIRECTORS Dr. Amar Agarwal (DIN: 00435684) ..................... Chairman Cum Managing Director Dr. Athiya Agarwal (DIN: 01365659) .................... Whole-time Director Dr. Adil Agarwal (DIN: 01074272) ........................ Director Mr. Sanjay Anand (DIN: 02501139) ...................... Independent Director Mr T. R. Ramasubramanian (DIN: 08207929) ........ Independent Director Mrs. Lakshmmi Subramanian (DIN: 00001439) .... Independent Director CHIEF FINANCIAL OFFICER Dear Shareholders, Ms. Saradha Govindarajan I look back nearly 60 years to when we initially set out to build the first Eye care hospital under our name, and then to the journey thereafter, in nurturing it into the world-class Eye care institution it COMPANY SECRETARY & COMPLIANCE OFFICER has grown into today. Now the hospital chain in its 62nd year of service has a total presence of 22 Ms. Jully H. Jivani hospitals across India. Our motivation for the pursuit of our goals has not wavered a bit through this eventful and challenging journey.We believe we are best suited to lead the eye care space in the AUDITORS coming years M/s. -

Early Postoperative Rotational Stability and Its Related Factors of a Single-Piece Acrylic Toric Intraocular Lens
Eye (2020) 34:474–479 https://doi.org/10.1038/s41433-019-0521-0 ARTICLE Early Postoperative Rotational stability and its related factors of a single-piece acrylic toric intraocular lens 1,2 3 4 5 1 1 1 Shuyi Li ● Xi Li ● Suhong He ● Qianyin Zheng ● Xiang Chen ● Xingdi Wu ● Wen Xu Received: 30 November 2018 / Accepted: 18 June 2019 / Published online: 12 July 2019 © The Author(s) 2019. This article is published with open access Abstract Purpose In the present study, we aimed to evaluate the early postoperative rotational stability of TECNIS toric intraocular lens (IOL) and analyse its correlation with preoperative and intraoperative parameters. Methods A total of 102 eyes from 87 cataract patients who underwent implantation of TECNIS toric IOL during July 2016 to November 2017 were enrolled in this retrospective study. Preoperative parameters including corneal astigmatism, axial length (AL), lens thickness (LT), anterior chamber depth (ACD) and sulcus-to-sulcus (STS), were determined. The area of capsulorhexis was measured with Rhinoceros 5.0 software. The follow-up examinations including the residual astigmatism (RAS) and postoperative toric IOL axis, were performed at 1 month and 3 months after surgery. − − 1234567890();,: 1234567890();,: Results RAS was 0.84 ± 0.88 D at 1 month and 0.81 ± 0.89 D at 3 months after surgery. The rotation of toric IOL at 3 months was 4.83 ± 3.65°. The Pearson’s r of ACD, horizontal and vertical STS, and toric IOL target axis was 0.011, 0.039, 0.045 and 0.082. The toric IOL rotation was positively correlated with the area of capsulorhexis (r = 0.522, P = 0.0003), LT (r = 0.288, P = 0.003) and AL (r = 0.259, P = 0.009). -
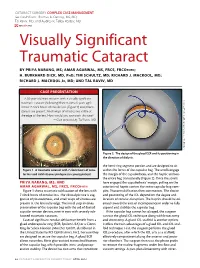
Visually Significant Traumatic Cataract
CATARACT SURGERY COMPLEX CASE MANAGEMENT Section Editors: Thomas A. Oetting, MS, MD; Tal Raviv, MD; and Audrey R. Talley Rostov, MD eyetube.net Visually Significant Traumatic Cataract BY PRIYA NARANG, MS; AMAR AGARWAL, MS, FRCS, FRCOPHTH; H. BURKHARD DICK, MD, PHD; TIM SCHULTZ, MD; RICHARD J. MACKOOL, MD; RICHARD J. MACKOOL JR, MD; AND TAL RAVIV, MD CASE PRESENTATION A 50-year-old man presents with a visually significant (Courtesy of Priya Narang, MS, and Amar Agarwal, FRCS, FRCOphth.) traumatic cataract (following blunt trauma 5 years ago). About 7 clock hours of zonular loss (Figure 1) and phaco- donesis are present. Small wisps of vitreous are visible at the edge of the lens. How would you approach this case? —Case prepared by Tal Raviv, MD. (Courtesy of Tal Raviv, MD.) Figure 2. The design of the glued ECR and its positioning in the direction of dialysis. the hemi-ring segment portion and are designed to sit Figure 1. A traumatic cataract with 7 clock hours of zonu- within the fornix of the capsular bag. The scrolls engage lar loss and mild vitreous prolapse in a young patient. the margin of the capsulorhexis, and the haptic anchors the entire bag transsclerally (Figure 2). Once the scrolls PRIYA NARANG, MS, AND have engaged the capsulorhexis’ margin, pulling on the AMAR AGARWAL, MS, FRCS, FRCOPHTH exteriorized haptic centers the entire capsular bag com- Figure 1 shows traumatic subluxation of the lens with plex. Phacoemulsification then commences. The choice 7 clock hours of zonular loss. The clinical picture is sug- and positioning of the IOL depend on the degree and gestive of phacodonesis, and small wisps of vitreous are location of zonular disruption. -

REFRACTIVE Laser
4 Cover Story REFRACTIVE Laser QUEST FOR PERFECTION LASIK banks on mature technology and reduced complication rates to stay ahead of the competition by Dermot McGrath aser-assisted in situ how many patients fall under the terminally complication rates in recent years. keratomileusis (LASIK) has dissatisfied category over the long term, the “There has definitely been an been assessed and improved by fact that the FDA in the US received just improvement over the past few years which I still believe many more than a decade of clinical 140 “negative reports relating to LASIK” I would attribute to improved technology, “patients disappear studiesL and technological innovation since for the time period 1998-2006 suggests to with better preoperative diagnostics and from their surgeon’s the procedure was first introduced. As some observers that LASIK complication also much better patient screening in terms practices after the one one of the most popular elective surgical and/or dissatisfaction rates are probably of anterior and posterior surface, corneal year of ‘free’ follow- procedures in the world, with one of the under-reported. thickness, and even family history to help up care that most highest safety profiles, LASIK remains the A 2008 study on LASIK complications prevent complications such as post-LASIK provide. Consequently, primary dynamo driving today’s global carried out at Wills Eye Institute (J ectasia,” said Francesco Carones MD, refractive surgery market. Cataract Refract Surg. 2008 Jan;34(1):32- Co-founder and medical director of the I do believe we have However, given the huge volume of 9.), for instance, found that only 29 per Carones Ophthalmology Centre in been underestimating procedures performed since its inception, cent of patients referred for problems Milan, Italy. -

(YAG) Laser Capsulotomy Reference Number: CP.VP.65 Coding Implications Last Review Date: 12/2020 Revision Log
Clinical Policy: Yttrium Aluminium Garnet (YAG) Laser Capsulotomy Reference Number: CP.VP.65 Coding Implications Last Review Date: 12/2020 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description This policy describes the medical necessity requirements for yttrium aluminium garnet (YAG) laser capsulotomy. Policy/Criteria I. It is the policy of health plans affiliated with Centene Corporation® (Centene) that YAG laser capsulotomy is medically necessary for the following indications: A. Posterior capsular opacification following cataract surgery resulting in best corrected visual acuity of 20/30 or worse associated with symptoms of blurred vision, visual distortion or glare affecting activities of daily living; B. Contraction of the posterior capsule with resulting displacement of the intraocular lens; C. Posterior capsular opacification resulting in best corrected visual acuity of 20/25 or worse, reducing the ability to evaluate and treat retinal detachment. Background YAG capsulotomy is the incision of an opaque posterior lens capsule in an aphakic or pseudophakic eye. This incision allows the capsule to retract and no longer serve as an obstruction to the passage of light through the media to the retina. The incision is performed with YAG laser. The eye examination must confirm the diagnosis of posterior capsular opacification and excludes other ocular causes of functional impairment by one of the following methods: The eye examination should demonstrate decreased light transmission (visual acuity worse than 20/30 or 20/25 if the procedure is performed to assist in the diagnosis and treatment of retinal detachment). Manifest refraction must be recorded with decrease in best-corrected visual acuity. -

Intraocular Pressure During Phacoemulsification
J CATARACT REFRACT SURG - VOL 32, FEBRUARY 2006 Intraocular pressure during phacoemulsification Christopher Khng, MD, Mark Packer, MD, I. Howard Fine, MD, Richard S. Hoffman, MD, Fernando B. Moreira, MD PURPOSE: To assess changes in intraocular pressure (IOP) during standard coaxial or bimanual micro- incision phacoemulsification. SETTING: Oregon Eye Center, Eugene, Oregon, USA. METHODS: Bimanual microincision phacoemulsification (microphaco) was performed in 3 cadaver eyes, and standard coaxial phacoemulsification was performed in 1 cadaver eye. A pressure transducer placed in the vitreous cavity recorded IOP at 100 readings per second. The phacoemulsification pro- cedure was broken down into 8 stages, and mean IOP was calculated across each stage. Intraocular pressure was measured during bimanual microphaco through 2 different incision sizes and with and without the Cruise Control (Staar Surgical) connected to the aspiration line. RESULTS: Intraocular pressure exceeded 60 mm Hg (retinal perfusion pressure) during both standard coaxial and bimanual microphaco procedures. The highest IOP occurred during hydrodissection, oph- thalmic viscosurgical device injection, and intraocular lens insertion. For the 8 stages of the phaco- emulsification procedure delineated in this study, IOP was lower for at least 1 of the bimanual microphaco eyes compared with the standard coaxial phaco eye in 4 of the stages (hydro steps, nu- clear disassembly, irritation/aspiration, anterior chamber reformation). CONCLUSION: There was no consistent difference in IOP between the bimanual microphaco eyes and the eye that had standard coaxial phacoemulsification. Bimanual microincision phacoemul- sification appears to be as safe as standard small incision phacoemulsification with regard to IOP. J Cataract Refract Surg 2006; 32:301–308 Q 2006 ASCRS and ESCRS Bimanual microincision phacoemulsification, defined as capable of insertion through these microincisions become cataract extraction through 2 incisions of less than 1.5 mm more widely available. -

Eyes Before Cataract Surgery
HIGH-RISK EYES Recognising ‘high-risk’ eyes before cataract surgery Parikshit Gogate Mark Wood Head, Department of Paediatric Ophthalmology, Community Consultant Ophthalmologist, CCBRT Hospital, Eye Care, HV Desai Eye Hospital, Pune 411028, India. Box 23310, Dar es Salaam, Tanzania. Email: [email protected] Email: [email protected] Certain eyes are at a higher risk of compli- Conjunctivitis should be treated with cation during cataract surgery. Operations topical antibiotics prior to intraocular on such ‘high-risk’ eyes are also more likely surgery. to yield a poor visual outcome (defined as Noble Bruce best corrected vision less than 6/60 after Potential visualisation surgery).1 Learning to recognise when eyes are at problems during surgery greater risk, and acting accordingly, will help Corneal opacity you to avoid complications. Even so, before Leucoma-grade opacity will make your task the operation takes place, it is good practice Conjunctivitis extremely difficult. You will find it difficult to to explain to such patients that a poor see details, in particular the capsulotomy. outcome is a possibility. This makes these There may be residual lens matter • Measuring intraocular pressure. It is patients’ expectations more realistic and remaining in the bag, which will be difficult important to measure intraocular pressure improves postoperative compliance and to see. It will also be challenging to place in all patients, for example to identify follow-up. In most cases, patients who are the intraocular lens (IOL) in the posterior glaucoma. blind with complicated cataract will be chamber with both haptics under the iris. • A fundus examination. The fundus can happy with even a modest improvement of be seen through all but the densest Patients suffering from trachoma with their vision.