Visually Significant Traumatic Cataract
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

5267830313.Pdf
DR. AGARWAL’S EYE HOSPITAL LIMITED 1 CONTENTS Page No. Company Information 2 Financial Highlights 3 Notice to Shareholders 4 Directors’ Report 11 Management Discussion and Analysis 15 Corporate Governance Report 15 Auditors’ Certificate on Corporate Governance 26 Independent Auditors’ Report to the Members 28 Secretarial Compliance Certificate 32 Balance Sheet 36 Profit and Loss Account 37 Cash Flow Statement 38 Notes on Financial Statement 41 Attendance Slip and Proxy Form 59 2 DR. AGARWAL’S EYE HOSPITAL LIMITED COMPANY INFORMATION Board of Directors Dr. Amar Agarwal (Chairman cum Managing Director) Dr. Athiya Agarwal (Wholetime Director) Dr. Adil Agarwal (Wholetime Director) Dr. Anosh Agarwal (Wholetime Director) Dr. Jasvinder Singh Saroya Mr. M. R. G. Apparao Mr. Prabhat Toshniwal Mr. Sanjay Anand Auditors M/s. M. K. Dandeker & Co. Chartered Accountants, 244, Angappa Naicken Street, Chennai 600 001. Registered Office 19 (Old No.13), Cathedral Road, Chennai 600 086. Bankers (1) State Bank of India, Gopalapuram Branch, Chennai - 600 086. (2) State Bank of India, Industrial Finance Branch, Chennai 600 002. Share Transfer Agents Integrated Enterprises (India) Ltd. 2nd Floor, Kences Towers, No.1, Ramakrishna Street, North Usman Road, T.Nagar, Chennai 600 017. Tel: 2814 0801-03 Email: [email protected] DR. AGARWAL’S EYE HOSPITAL LIMITED HOSPITAL EYE AGARWAL’S DR. Financial Highlights Rs. in crore For the year ended 2012-13 2011-12 2010-11 2009-10 2008-09 2007-08 2006-07 2005-06 2004-05 2003-04 Total Income 109.73 105.68 104.01 -

Agarwal AR 19.Indd
Contents Page No Chairman’s Desk 3 Board of Directors 5 A Word from Chairman - Clinical Board 9 Industrial Update 12 Notice to Shareholders 15 Directors’ Report 29 Management Discussions and Analysis Report 46 Corporate Governance Report 50 A word from the CFO 61 Financial Highlights 62 Independent Auditor’s Report 65 Balance Sheet as at 31st March, 2019 72 Statement of Profit and Loss for the year ended 31st March 2019 73 Statement of changes in equity for the year ended 31st March 2019 74 Cash Flow Statement as on 31st March 2019 75 Notes Forming Part of the Financial Statements for the year ended 76 31st March 2019 Press Clippings 120 NABH Accredited 126 Route map to AGM venue 128 CORPORATE Chairman’s INFORMATION Desk DIRECTORS Dr. Amar Agarwal (DIN: 00435684) ..................... Chairman Cum Managing Director Dr. Athiya Agarwal (DIN: 01365659) .................... Whole-time Director Dr. Adil Agarwal (DIN: 01074272) ........................ Director Mr. Sanjay Anand (DIN: 02501139) ...................... Independent Director Mr T. R. Ramasubramanian (DIN: 08207929) ........ Independent Director Mrs. Lakshmmi Subramanian (DIN: 00001439) .... Independent Director CHIEF FINANCIAL OFFICER Dear Shareholders, Ms. Saradha Govindarajan I look back nearly 60 years to when we initially set out to build the first Eye care hospital under our name, and then to the journey thereafter, in nurturing it into the world-class Eye care institution it COMPANY SECRETARY & COMPLIANCE OFFICER has grown into today. Now the hospital chain in its 62nd year of service has a total presence of 22 Ms. Jully H. Jivani hospitals across India. Our motivation for the pursuit of our goals has not wavered a bit through this eventful and challenging journey.We believe we are best suited to lead the eye care space in the AUDITORS coming years M/s. -

REFRACTIVE Laser
4 Cover Story REFRACTIVE Laser QUEST FOR PERFECTION LASIK banks on mature technology and reduced complication rates to stay ahead of the competition by Dermot McGrath aser-assisted in situ how many patients fall under the terminally complication rates in recent years. keratomileusis (LASIK) has dissatisfied category over the long term, the “There has definitely been an been assessed and improved by fact that the FDA in the US received just improvement over the past few years which I still believe many more than a decade of clinical 140 “negative reports relating to LASIK” I would attribute to improved technology, “patients disappear studiesL and technological innovation since for the time period 1998-2006 suggests to with better preoperative diagnostics and from their surgeon’s the procedure was first introduced. As some observers that LASIK complication also much better patient screening in terms practices after the one one of the most popular elective surgical and/or dissatisfaction rates are probably of anterior and posterior surface, corneal year of ‘free’ follow- procedures in the world, with one of the under-reported. thickness, and even family history to help up care that most highest safety profiles, LASIK remains the A 2008 study on LASIK complications prevent complications such as post-LASIK provide. Consequently, primary dynamo driving today’s global carried out at Wills Eye Institute (J ectasia,” said Francesco Carones MD, refractive surgery market. Cataract Refract Surg. 2008 Jan;34(1):32- Co-founder and medical director of the I do believe we have However, given the huge volume of 9.), for instance, found that only 29 per Carones Ophthalmology Centre in been underestimating procedures performed since its inception, cent of patients referred for problems Milan, Italy. -

Model Curriculum Handbook
Ministry of Health and Family Welfare Allied Health Section 2015-16 Model Curriculum Handbook OPTOMETRY Model Curriculum Handbook OPTOMETRY Ministry of Health and Family Welfare Allied Health Section Contents Contributors to drafting and review ............................................................................................................... 3 List of Abbreviations ..................................................................................................................................... 5 Chapter 1: Introduction to the Handbook.................................................................................................... 11 Who is an Allied and Healthcare Professional? ......................................................................................... 11 Scope and need for allied and healthcare professionals in the Indian healthcare system ............................ 11 Learning goals and objectives for allied and healthcare professionals ....................................................... 12 Introduction of new elements in allied and healthcare education .............................................................. 17 Competency-based curriculum ............................................................................................................. 17 Promoting self-directed learning of the professionals ........................................................................... 17 Credit hours vs traditional system ....................................................................................................... -

SHOULD LASIK BE REBRANDED? Experts Debate Whether the Leading Refractive Surgery Procedure Needs a New Name
COVER FOCUS COVER POINT/COUNTERPOINT: SHOULD LASIK BE REBRANDED? Experts debate whether the leading refractive surgery procedure needs a new name. BY SOOSAN JACOB, MS, FRCS, DNB; AMAR AGARWAL, MS, FRCS, FRCOPHTH; MARC MULLIE, MD, FRCSC; MICHAEL LAWLESS, MBBS, FRANZCO, FRACS; DAN Z. REINSTEIN, MD, MA(CANTAB), FRCSC, DABO, FRCOPHTH, FEBO; VANCE THOMPSON, MD; AND J. TREVOR WOODHAMS, MD Point: refractive surgery procedure. The advantages that this tech- nique offers are numerous. For starters, the absence of a flap A LASIK Rebrand is in Order and the use of a small incision together act to eliminate flap- By Soosan Jacob, MS, FRCS, DNB; Amar Agarwal, MS, related complications such as striae, flap dislodgement, and FRCS, FRCOphth; and Marc Mullie, MD, FRCSC epithelial ingrowth. Similarly, because of decreased disruption of the anterior corneal innervation, there is faster recovery Rebrand Refractive Surgery of corneal sensitivity and less patient experience of dry eye by Introducing a New Procedure than is seen with LASIK.3 Most important, the presence of the Soosan Jacob, MS, FRCS, DNB; and nearly intact anterior stromal layer of the cornea allows better Amar Agarwal, MS, FRCS, FRCOphth maintenance of biomechanical strength after SMILE compared Corneal refractive surgery has evolved with LASIK.4,5 The entire procedure is completed with a single over the years, progressing through techniques from cuts in the cornea (RK), to excimer laser surface ablation (PRK), to intrastromal ablation under a flap (LASIK). The last of these approaches has been the most successful technique thus AT A GLANCE far, with widespread worldwide acceptance and penetration. WHAT YOUR PEERS ARE SAYING The LASIK flap itself has evolved, from being created with a ABOUT LASIK REBRANDING mechanical microkeratome to being cut with a femtosecond • Instead of rebranding LASIK specifically, it could be laser. -

Image of the Month the Human Choroid, Reconstructed in 3D
APRIL 2016 # 29 Image of the Month Upfront Profession Sitting Down With The human choroid, Growing your own Benchmarking your practice Amar Agarwal, Chairman of reconstructed in 3D crystalline lens against your peers Dr Agarwal’s Eye Hospital 03 08 – 10 60 – 64 66 – 67 www.theophthalmologist.com DUAL-SEGMENT PUMP TECHNOLOGY + Precise fluidics + Pulsatile-free + Quick vacuum rise + Versatile performance PERFORMANCE IN EVERY DETAIL Superior chamber stability through superior engineering.†,1,2 That’s the Centurion® Effect. Active Fluidics™ Technology • Helps to Maintain Chamber Stability: Detects and compensates to help provide superior chamber stability3 compared to INFINITI®4 • Less Surge: Less surge at any tested vacuum level3,5 • More Consistent IOP4 : Up to 80% less surge area3,5 Contact your Alcon representative to schedule a demonstration and experience the Centurion® Effect for yourself. †As compared to the INFINITI® Vision System, bottle gravity system. 1. Lorente R, Fanney D, Injev V, Sharif-Kashani P. Quantification of occlusion break surge in peristaltic-based phacoemulsification systems. ASCRS-ASOA Symposium and Congress; April 25-29, 2014; Boston, USA.2. Nicoli M, Miller K, Dimalanta R, Loke D; Jules Stein Eye Institute, UCLA. IOP Stability Measurement and Comparison Between Gravity-Fed and Actively Controlled Phacoemulsification Systems. 2014. 3. Sharif-Kashani P, Fanney D, Injev V. Comparison of occlusion break responses and vacuum rise times of phacoemulsification systems. BMC Ophthalmol. 2014;14:96. 4. Nicoli CM, Dimalanta R, Miller K. Experimental anterior chamber maintenance in active versus passive phacoemulsification fluidics systems. J Cataract Refract Surg. 2016;42(1):157-162. 5. Alcon data on file. -

Educational Qualifications
CURRICULUM VITAE PERSONAL NAME : Dr. Sunita Agarwal I have been fortunate to be born in a family of ophthalmologists. My grandfather Dr. Raghvir S. Agarwal was a noted ophthalmologist of his time in India. My father Dr. Jaivir Agarwal is the founder of Dr. Agarwal ‘s Eye Institute, Chennai, mother Dr. Mrs. Tahira Agarwal is also a renowned ophthalmic surgeon currently practicing as a corneal specialist. My brother Dr. Amar Agarwal and myself both are ophthalmic surgeons, extensively engaged in ophthalmic research, teaching are currently practicing with our parents at Chennai. Dr. Athiya Agarwal, wife of Dr Amar Agarwal is also a part of the team. EDUCATIONAL QUALIFICATIONS 1. COMPLETED MATRICULATION FROM SACRED HEART CHURCH PARK SCHOOL IN 1975 I had a complete childhood with schooling from one of the finest institutions in the country. As is well known convent education brings with it a flare to the child and close proximity with God. In any format the individual gets to think of the less fortunate and realizes the pain and anguish of our school teachers and convent nuns. I was extremely mischievous and was called out to the Principals office very often still in this developed a close camaraderie with my Principal Teacher Sister Clare. So much so that till today she remembers me fondly of tying my unruly hair in her own ribbons or admonishing me for one of my little crimes. I also happened to be the School pupil leader in the my last year occasion came on a day when I had just come back from Delhi after winning the national gold medal for swimming for 1974, and as I entered school the election had taken place in my absence, this was one of few times I saw tears (of joy) in my fathers year. -

Multifocal Intraocular Lens Exchange in Patients with Ocular Comorbidities: Indications and Outcomes
Multifocal Intraocular Lens Exchange in Patients with Ocular Comorbidities: Indications and Outcomes Brian Kenny Armstrong ( [email protected] ) Cleveland Clinic Abu Dhabi https://orcid.org/0000-0001-6337-6265 Jason Goldsmith Cleveland Clinic Abu Dhabi Terrence Lee St John Cleveland Clinic Abu Dhabi Samuel Navon Cleveland Clinic Abu Dhabi Research Article Keywords: multifocal IOL intolerance, trifocal IOLs, IOL exchange, ocular comorbidities, patient dissatisfaction Posted Date: March 13th, 2021 DOI: https://doi.org/10.21203/rs.3.rs-284924/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 1/10 Abstract Purpose: To investigate all cases of multifocal intraocular lens (MFIOL) exchange, with specic focus on indications for exchange and evaluation of postoperative outcomes, in a tertiary care, multi-specialty ophthalmology practice. Setting/Venue: Academic Referral Center/Cleveland Clinic Abu Dhabi – Abu Dhabi, United Arab Emirates Methods: This retrospective case series identied all patients that presented to a large academic practice over a 4-year period that were intolerant to MFIOL technology and thus required intraocular lens (IOL) exchange. All patients reported poor vision despite correction of reversible ocular comorbidities, including dry eye and residual refractive error. Outcomes reviewed include subjective visual complaints, IOL-type, visual acuity, refractive error, ocular comorbidities, and surgical outcomes. Endpoints examined include mean uncorrected distance visual acuity (UDVA), mean corrected distance visual acuity (CDVA), mean refractive spherical equivalent (MRSE), and residual refractive astigmatism. Results: Six eyes of ve patients required MFIOL exchange. All IOL’s exchanged were trifocal IOL’s. IOL exchange occurred between 6 to 72 months following primary phacoemulsication. -

44 • M a R C H 2 0
44 • MARCH 2018 Cataract Complications Eight difficult cases that require complex management decisions. HIS PAST NOVEMBER, THE 16TH ANNUAL SPOTLIGHT ON CATARACT SURGERY Symposium at AAO 2017 was entitled “Clinical Decision-Making With Cataract Complications: TYou Make the Call.” Cochaired by Mitchell P. Weikert, MD, and myself, this 4-hour symposium was organized around 8 video cases that presented a range of cataract surgical challenges and complications. The 8 cases were selected from my own practice. As I presented the videos, I would pause at selected points to note a complication or introduce the need to make a management decision. The attendees were then asked to make clinical decisions using their electronic audience response keypads. This was followed by several rapid-fire didactic presentations by invited experts on topics of relevance to the case. Next, a rotating panel of 2 discussants (who had never viewed the case) was asked to make a manage- ment recommendation before the video of the outcome was shown. Following additional audience polling about preferences and practices, the 2 panelists would provide their own opinions and pearls. In all, nearly 40 presenters and panelists spoke about a wide variety of topics, including managing a postvitrectomy cataract, posterior capsular rupture in a multifocal or toric IOL patient, traumatic cataracts, ultrabrunescent cataracts, small pupils, crowded anterior segments, unhappy multifocal IOL patients, iris prolapse, traumatic iris defects, and retained cortex. Alan S. Crandall, MD, concluded the symposium by delivering the 13th annual Academy Charles D. Kelman Lecture, “Phaco at 50: The Collision of Cataract and Glaucoma (Plus).” This EyeNet article reports the results of the 35 audience response questions, accompanied by written commentary from the symposium speakers and panelists. -

Sizing and Centering the Capsulorhexis by WILLIAM BOND, MD; BROCK K
CATARACT SURGERY PHACO PEARLS Sizing and Centering the Capsulorhexis BY WILLIAM BOND, MD; BROCK K. BAKEWELL, MD; AMAR AGARWAL, MS, FRCS, FRCOPHTH; AND DAVID SPALTON, FRCS, FRCP, FRCOPHTH Most surgeons have performed the capsulorhexis since its groundbreaking, simultaneous introduction in 1990 by Thomas Neuhann, MD, and Howard Gimbel, MD.1 Now, as the use of aspheric and presbyopia-correcting IOLs becomes widespread, the sizing and centration of the capsulorhexis have never been more essential. Sufficiently sized for the intend- ed IOL and adequately centered, the capsulorhexis is the framework for the production of a stable postoperative IOL/bag complex and the achievement of excellent postoperative vision. How do surgeons optimize the capsulorhexis? —William J. Fishkind, MD, Section Editor WILLIAM BOND, MD tear reappears, of course, I redirect it parallel to the iris Over the years, I have favored a large capsulorhexis for and less peripherally. better access to the lens proper, because I believe that the The other common cause of extending a capsulorhex- anterior capsule is part of the cataract. In the event of a is too far is not to regrasp the tearing flap frequently posterior capsular rupture, there is virtually always enough. The tear will circumferentially expand as the enough anterior capsule to support a PCIOL in the sulcus, edge gets farther from the forceps. This scenario seems no matter how large the capsulorhexis was initially. Fur- elementary but can easily happen. A minimum of two thermore, it has been my experience that there are many regrabbings close to the tearing flap’s edge, after the ini- more longitudinal tears in the anterior capsule in the tial grab, is what I find easiest. -

IOL Scaffold in Phacoemulsification to Prevent Posterior Capsule Tear
Title: IOL scaffold in phacoemulsification to prevent posterior capsule tear. 1 Dr. Ashraful Huq Ridoy, 2 Dr. Niaz Abdur Rahman 3 Dr. Mahziba Rahman Chowdhury, 4 Dr. Syeed Mehbub Ul Kadir, 5 Dr. Mahbubur Rahman Chowdhury Purpose – To prevent posterior capsule tear and evaluate the post-operative outcomes of phacoemulsification with IOL scaffold technique. Design – Single-center, prospective, interventional, non-comparative, consecutive case series. Materials and Methods – A total of 17 eyes of 17 patients with morgagnian (04 eyes) and hard (nuclear sclerosis grade – IV of 13 eyes) cataract who had undergone phacoemulsification with IOL scaffold technique to prevent posterior capsule tear in a tertiary clinic. All surgeries were performed by a single surgeon. 6.0 mm optic, acrylic, foldable IOL was implanted in all eyes. The pre- operative and post-operative parameters evaluated were uncorrected distance visual acuity, corrected distance visual acuity, cornea status, intraocular pressure and anterior segment inflammation. Results – Posterior capsule tear were prevented in all eyes. At 1-month follow- up, a significant improvement was noted in uncorrected distance visual acuity post-operatively (P-value <0.0001) and 6/6 visual acuity achieved in 71% eyes. Corrected visual acuity 6/6 achieved in 18% eyes. Mean post-operative IOP at 1-day and 1-month follow-up without any medication were 12.79 mmHg and 13.06 mmHg respectively. Immediate post-operative grade-2 anterior segment reaction (02 eyes) and minimal corneal edema (03 eyes) noted which were resolved by 1-month. Conclusion - IOL scaffold provides a safe and effective way to prevent posterior capsule tear in phacoemulsification of morgagnian and hard cataracts, with a good visual outcome. -
Glued IOL Scaffold Technique
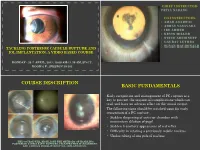
TACKLING POSTERIOR CAPSULE RUPTURE AND IOL IMPLANTATION: A VIDEO BASED COURSE MONDAY - 20 th APRIL, 2015: 10.00 AM-11.30 AM, SD CC, ROOM 6 F ; SESSION 20-202 COURSE DESCRIPTION BASIC FUNDAMENTALS Early recognition and management of PC rupture is a key to prevent the sequential complications which can trail and have an adverse effect on the visual output. The following signs should be watched upon for early recognition of a PC rupture. • Sudden deepening of anterior chamber with momentary dilation of pupil • Sudden transitory appearance of red reflex • Difficulty in rotating a previously mobile nucleus • Undue tilting of one pole of nucleus …THE COURSE WILL HIGHLIGHT THE METHODS OF HANDLING POSTERIOR CAPSULE (PC) RUPTURE, ITS EFFECTIVE MANAGEMENT AND VARIOUS MODALITIES OF IOL IMPLANTATION. MANAGEMENT PROTOCOL OF PC BASICS RUPTURE AND IOL IMPLANTATION • In the context of a ruptured posterior capsule, the immediate reflex • Lower down phaco parameters action to be deterred on behalf of the surgeon is to withdraw the • Low flow rate phacoemulsification probe suddenly from the eye. A dispersive OVD from the side port incision should be used to plug-in the posterior • Moderate vacuum capsule defect and fill and stabilise the anterior chamber followed by withdrawal of the phacoemulsification probe. • Low to moderate phaco burst energy to promote • The posterior capsule rupture when small is converted into a posterior capsulorhexis with stable margin facilitating the follow ability implantation of a one piece foldable acrylic IOL in the capsular bag. But if the capsular rupture opening is large, sulcus fixation of an IOL is preferable in cases with adequate anterior capsular margin support.