Head Injury Office Hours Telephone Triage Protocols | Pediatric | 2017
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Diagnoses to Include in the Problem List Whenever Applicable
Diagnoses to include in the problem list whenever applicable Tips: 1. Always say acute or open when applicable 2. Always relate to the original trauma 3. Always include acid-base abnormalities, AKI due to ATN, sodium/osmolality abnormalities 4. Address in the plan of your note 5. Do NOT say possible, potential, likely… Coders can only use a real diagnosis. Make a real diagnosis. Neurological/Psych: Head: 1. Skull fracture of vault – open vs closed 2. Basilar skull fracture 3. Facial fractures 4. Nerve injury____________ 5. LOC – include duration (max duration needed is >24 hrs) and whether they returned to neurological baseline 6. Concussion with or without return to baseline consciousness 7. DAI/severe concussion with or without return to baseline consciousness 8. Type of traumatic brain injury (hemorrhages and contusions) – include size a. Tiny = <0.6 cm b. Small/moderate = 0.6-1 cm c. Large/extensive = >1 cm 9. Cerebral contusion/hemorrhage 10. Cerebral edema 11. Brainstem compression 12. Anoxic brain injury 13. Seizures 14. Brain death Spine: 1. Cervical spine fracture with (complete or incomplete) or without cord injury 2. Thoracic spine fracture with (complete or incomplete) or without cord injury 3. Lumbar spine fracture with (complete or incomplete) or without cord injury 4. Cord syndromes: central, anterior, or Brown-Sequard 5. Paraplegia or quadriplegia (any deficit in the upper extremity is consistent with quadriplegia) Cardiovascular: 1. Acute systolic heart failure 40 2. Acute diastolic heart failure 3. Chronic systolic heart failure 4. Chronic diastolic heart failure 5. Combined heart failure 6. Cardiac injury or vascular injuries 7. -

Cervical Spine Injury Risk Factors in Children with Blunt Trauma Julie C
Cervical Spine Injury Risk Factors in Children With Blunt Trauma Julie C. Leonard, MD, MPH,a Lorin R. Browne, DO,b Fahd A. Ahmad, MD, MSCI,c Hamilton Schwartz, MD, MEd,d Michael Wallendorf, PhD,e Jeffrey R. Leonard, MD,f E. Brooke Lerner, PhD,b Nathan Kuppermann, MD, MPHg BACKGROUND: Adult prediction rules for cervical spine injury (CSI) exist; however, pediatric rules abstract do not. Our objectives were to determine test accuracies of retrospectively identified CSI risk factors in a prospective pediatric cohort and compare them to a de novo risk model. METHODS: We conducted a 4-center, prospective observational study of children 0 to 17 years old who experienced blunt trauma and underwent emergency medical services scene response, trauma evaluation, and/or cervical imaging. Emergency department providers recorded CSI risk factors. CSIs were classified by reviewing imaging, consultations, and/or telephone follow-up. We calculated bivariable relative risks, multivariable odds ratios, and test characteristics for the retrospective risk model and a de novo model. RESULTS: Of 4091 enrolled children, 74 (1.8%) had CSIs. Fourteen factors had bivariable associations with CSIs: diving, axial load, clotheslining, loss of consciousness, neck pain, inability to move neck, altered mental status, signs of basilar skull fracture, torso injury, thoracic injury, intubation, respiratory distress, decreased oxygen saturation, and neurologic deficits. The retrospective model (high-risk motor vehicle crash, diving, predisposing condition, neck pain, decreased neck mobility (report or exam), altered mental status, neurologic deficits, or torso injury) was 90.5% (95% confidence interval: 83.9%–97.2%) sensitive and 45.6% (44.0%–47.1%) specific for CSIs. -

Early Management of Retained Hemothorax in Blunt Head and Chest Trauma
World J Surg https://doi.org/10.1007/s00268-017-4420-x ORIGINAL SCIENTIFIC REPORT Early Management of Retained Hemothorax in Blunt Head and Chest Trauma 1,2 1,8 1,7 1 Fong-Dee Huang • Wen-Bin Yeh • Sheng-Shih Chen • Yuan-Yuarn Liu • 1 1,3,6 4,5 I-Yin Lu • Yi-Pin Chou • Tzu-Chin Wu Ó The Author(s) 2018. This article is an open access publication Abstract Background Major blunt chest injury usually leads to the development of retained hemothorax and pneumothorax, and needs further intervention. However, since blunt chest injury may be combined with blunt head injury that typically requires patient observation for 3–4 days, other critical surgical interventions may be delayed. The purpose of this study is to analyze the outcomes of head injury patients who received early, versus delayed thoracic surgeries. Materials and methods From May 2005 to February 2012, 61 patients with major blunt injuries to the chest and head were prospectively enrolled. These patients had an intracranial hemorrhage without indications of craniotomy. All the patients received video-assisted thoracoscopic surgery (VATS) due to retained hemothorax or pneumothorax. Patients were divided into two groups according to the time from trauma to operation, this being within 4 days for Group 1 and more than 4 days for Group 2. The clinical outcomes included hospital length of stay (LOS), intensive care unit (ICU) LOS, infection rates, and the time period of ventilator use and chest tube intubation. Result All demographics, including age, gender, and trauma severity between the two groups showed no statistical differences. -

Anesthesia for Trauma
Anesthesia for Trauma Maribeth Massie, CRNA, MS Staff Nurse Anesthetist, The Johns Hopkins Hospital Assistant Professor/Assistant Program Director Columbia University School of Nursing Program in Nurse Anesthesia OVERVIEW • “It’s not the speed which kills, it’s the sudden stop” Epidemiology of Trauma • ~8% worldwide death rate • Leading cause of death in Americans from 1- 45 years of age • MVC’s leading cause of death • Blunt > penetrating • Often drug abusers, acutely intoxicated, HIV and Hepatitis carriers Epidemiology of Trauma • “Golden Hour” – First hour after injury – 50% of patients die within the first seconds to minutesÆ extent of injuries – 30% of patients die in next few hoursÆ major hemorrhage – Rest may die in weeks Æ sepsis, MOSF Pre-hospital Care • ABC’S – Initial assessment and BLS in trauma – GO TEAM: role of CRNA’s at Maryland Shock Trauma Center • Resuscitation • Reduction of fractures • Extrication of trapped victims • Amputation • Uncooperative patients Initial Management Plan • Airway maintenance with cervical spine protection • Breathing: ventilation and oxygenation • Circulation with hemorrhage control • Disability • Exposure Initial Assessment • Primary Survey: – AIRWAY • ALWAYS ASSUME A CERVICAL SPINE INJURY EXISTS UNTIL PROVEN OTHERWISE • Provide MANUAL IN-LINE NECK STABILIZATION • Jaw-thrust maneuver Initial Assessment • Airway cont’d: – Cervical spine evaluation • Cross table lateral and swimmer’s view Xray • Need to see all seven cervical vertebrae • Only negative CT scan R/O injury Initial Assessment • Cervical -

CASE REPORT Injuries Following Segway Personal
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Injuries Following Segway Personal Transporter Accidents: Case Report and Review of the Literature Permalink https://escholarship.org/uc/item/37r4387d Journal Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health, 16(5) ISSN 1936-900X Authors Ashurst, John Wagner, Benjamin Publication Date 2015 DOI 10.5811/westjem.2015.7.26549 License https://creativecommons.org/licenses/by/4.0/ 4.0 Peer reviewed eScholarship.org Powered by the California Digital Library University of California CASE REPORT Injuries Following Segway Personal Transporter Accidents: Case Report and Review of the Literature John Ashurst DO, MSc Conemaugh Memorial Medical Center, Department of Emergency Medicine, Benjamin Wagner, DO Johnstown, Pennsylvania Section Editor: Rick A. McPheeters, DO Submission history: Submitted April 20, 2015; Accepted July 9, 2015 Electronically published October 20, 2015 Full text available through open access at http://escholarship.org/uc/uciem_westjem DOI: 10.5811/westjem.2015.7.26549 The Segway® self-balancing personal transporter has been used as a means of transport for sightseeing tourists, military, police and emergency medical personnel. Only recently have reports been published about serious injuries that have been sustained while operating this device. This case describes a 67-year-old male who sustained an oblique fracture of the shaft of the femur while using the Segway® for transportation around his community. We also present a review of the literature. [West J Emerg Med. 2015;16(5):693-695.] INTRODUCTION no parasthesia was noted. In 2001, Dean Kamen developed a self-balancing, zero Radiograph of the right femur demonstrated an oblique emissions personal transportation vehicle, known as the fracture of the proximal shaft of the femur with severe Segway® Personal Transporter (PT).1 The Segway’s® top displacement and angulation (Figure). -

NIH Public Access Author Manuscript J Neuropathol Exp Neurol
NIH Public Access Author Manuscript J Neuropathol Exp Neurol. Author manuscript; available in PMC 2010 September 24. NIH-PA Author ManuscriptPublished NIH-PA Author Manuscript in final edited NIH-PA Author Manuscript form as: J Neuropathol Exp Neurol. 2009 July ; 68(7): 709±735. doi:10.1097/NEN.0b013e3181a9d503. Chronic Traumatic Encephalopathy in Athletes: Progressive Tauopathy following Repetitive Head Injury Ann C. McKee, MD1,2,3,4, Robert C. Cantu, MD3,5,6,7, Christopher J. Nowinski, AB3,5, E. Tessa Hedley-Whyte, MD8, Brandon E. Gavett, PhD1, Andrew E. Budson, MD1,4, Veronica E. Santini, MD1, Hyo-Soon Lee, MD1, Caroline A. Kubilus1,3, and Robert A. Stern, PhD1,3 1 Department of Neurology, Boston University School of Medicine, Boston, Massachusetts 2 Department of Pathology, Boston University School of Medicine, Boston, Massachusetts 3 Center for the Study of Traumatic Encephalopathy, Boston University School of Medicine, Boston, Massachusetts 4 Geriatric Research Education Clinical Center, Bedford Veterans Administration Medical Center, Bedford, Massachusetts 5 Sports Legacy Institute, Waltham, MA 6 Department of Neurosurgery, Boston University School of Medicine, Boston, Massachusetts 7 Department of Neurosurgery, Emerson Hospital, Concord, MA 8 CS Kubik Laboratory for Neuropathology, Department of Pathology, Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts Abstract Since the 1920s, it has been known that the repetitive brain trauma associated with boxing may produce a progressive neurological deterioration, originally termed “dementia pugilistica” and more recently, chronic traumatic encephalopathy (CTE). We review the 47 cases of neuropathologically verified CTE recorded in the literature and document the detailed findings of CTE in 3 professional athletes: one football player and 2 boxers. -

In Drivers of Open-Wheel Open Cockpit Race Cars
SPORTS MEDICINE SPINE FRACTURES IN DRIVERS OF OPEN-WHEEL OPEN COCKPIT RACE CARS – Written by Terry Trammell and Kathy Flint, USA This paper is intended to explain the mechanisms responsible for production of spinal fracture in the driver of an open cockpit single seat, open-wheel racing car (Indy Car) and what can be done to lessen the risk of fracture. In a report of fractures in multiple racing • Seated angle (approximately 45°) • Lumbar spine flexed series drivers (Championship Auto Racing • Hips and knees flexed • Seated semi-reclining Cars [CART]/Champ cars, Toyota Atlantics, Indy Racing League [IRL], Indy Lights and Figure 1: Body alignment in the Indy Car. Formula 1 [F1]), full details of the crash and mechanism of injury were captured and analysed. This author was the treating physician in all cases from 1996 to 2011. All images, medical records, data available BASILAR SKULL FRACTURE Use of this specific safety feature from the Accident Data Recorder-2 (ADR), Following a fatal distractive basilar is compulsory in most professional crash video, specific on track information, skull fracture in 1999, the Head and Neck motorsport sanctions and has resulted in a post-accident investigation of damage and Support (HANS) device was introduced into dramatic reduction to near elimination of direction of major impact correlated with Indy Cars. Basilar skull fracture occurs when fatal basilar skull fractures. No basilar skull ADR-2 data were analysed. Results provided neck tension exceeds 3113.75 N forces. fractures have occurred in the IRL since the groundwork for understanding spine No data demonstrates that HANS introduction of the HANS and since 2006 fracture and forces applied to the driver in predisposes the wearer to other cervical there has been only one cervical fracture. -

Mass/Multiple Casualty Triage
9.1 MASS/MULTIPLE CASUALTY TRIAGE PURPOSE · The goal of the mass/multiple Casualty Triage protocol is to prepare for a unified, coordinated, and immediate EMS mutual aid response by prehospital and hospital agencies to effectively expedite the emergency management of the victims of any type of Mass Casualty Incident (MCI). · Successful management of any MCI depends upon the effective cooperation, organization, and planning among health care professionals, hospital administrators and out-of-hospital EMS agencies, state and local government representatives, and individuals and/or organizations associated with disaster-related support agencies. · Adoption of Model Uniform Core Criteria (MUCC). DEFINITIONS Multiple Casualty Situations · The number of patients and the severity of the injuries do not exceed the ability of the provider to render care. Patients with life-threatening injuries are treated first. Mass Casualty Incidents · The number of patients and the severity of the injuries exceed the capability of the provider, and patients sustaining major injuries who have the greatest chance of survival with the least expenditure of time, equipment, supplies, and personnel are managed first. H a z GENERAL CONSIDERATIONS m Initial assessment to include the following: a t · Location of incident. & · Type of incident. M · Any hazards. C · Approximate number of victims. I · Type of assistance required. 9 . 1 COMMUNICATION · Within the scope of a Mass Casualty Incident, the EMS provider may, within the limits of their scope of practice, perform necessary ALS procedures, that under normal circumstances would require a direct physician’s order. · These procedures shall be the minimum necessary to prevent the loss of life or the critical deterioration of a patient’s condition. -
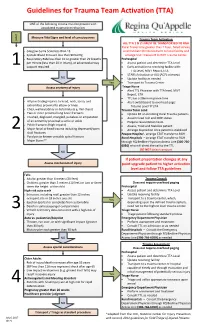
Guidelines for Trauma Team Activation (TTA)
Guidelines for Trauma Team Activation (TTA) ONE of the following criteria must be present with associated traumatic mechanism L e v e Measure Vital Signs and level of consciousness l Trauma Team Activation ALL TTA 1 & 2's MUST BE TRANSPORTED TO RGH Rural Travel time greater than 1 hour, failed airway · Glasgow Coma Scale less than 13 or immediate life threat divert to local facility and · Systolic Blood Pressure less than 90mmHg arrange STAT transport to RGH Trauma Center · Respiratory Rate less than 10 or greater then 29 breaths Prehospital per minute (less than 20 in infant), or advanced airway · Assess patient and determine TTA Level 1 support required · Early activation to receiving facility with: TTA Level, MIVT Report, ETA · STARS Activation or ALS (ACP) intercept NO · Update facility as needed Yes · Transport to Trauma Center Assess anatomy of injury Triage Nurse · Alert TTL Physician with TTA level, MIVT Report, ETA · TTL has a 20min response time · All penetrating injuries to head, neck, torso, and · Alert switchboard to overhead page: extremities proximal to elbow or knee Trauma Level ‘#’ ETA · Chest wall instability or deformity (e.g. flail chest) Trauma Team Lead · Two or more proximal long-bone fractures · Update ER on incoming Rural Trauma patients · Crushed, degloved, mangled, pulseless or amputation · Assume lead role and MRP status of an extremity proximal to wrist or ankle · Prepare resuscitation team · Pelvic fractures (high impact) · Assess, Treat and Stabilize patient 2 · Major facial or head trauma including depressed/open -

MASS CASUALTY TRAUMA TRIAGE PARADIGMS and PITFALLS July 2019
1 Mass Casualty Trauma Triage - Paradigms and Pitfalls EXECUTIVE SUMMARY Emergency medical services (EMS) providers arrive on the scene of a mass casualty incident (MCI) and implement triage, moving green patients to a single area and grouping red and yellow patients using triage tape or tags. Patients are then transported to local hospitals according to their priority group. Tagged patients arrive at the hospital and are assessed and treated according to their priority. Though this triage process may not exactly describe your agency’s system, this traditional approach to MCIs is the model that has been used to train American EMS As a nation, we’ve got a lot providers for decades. Unfortunately—especially in of trailers with backboards mass violence incidents involving patients with time- and colored tape out there critical injuries and ongoing threats to responders and patients—this model may not be feasible and may result and that’s not what the focus in mis-triage and avoidable, outcome-altering delays of mass casualty response is in care. Further, many hospitals have not trained or about anymore. exercised triage or re-triage of exceedingly large numbers of patients, nor practiced a formalized secondary triage Dr. Edward Racht process that prioritizes patients for operative intervention American Medical Response or transfer to other facilities. The focus of this paper is to alert EMS medical directors and EMS systems planners and hospital emergency planners to key differences between “conventional” MCIs and mass violence events when: • the scene is dynamic, • the number of patients far exceeds usual resources; and • usual triage and treatment paradigms may fail. -

Diagnosis and Treatment of Cerebrospinal Fluid Rhinorrhea Following Accidental Traumatic Anterior Skull Base Fractures
Neurosurg Focus 32 (6):E3, 2012 Diagnosis and treatment of cerebrospinal fluid rhinorrhea following accidental traumatic anterior skull base fractures MATEO ZIU, M.D., JENNIFER GENTRY SAVAGE, M.D., AND DAVID F. JIMENEZ, M.D. Department of Neurosurgery, University of Texas Health Science Center at San Antonio, Texas Cerebrospinal fluid rhinorrhea is a serious and potentially fatal condition because of an increased risk of menin- gitis and brain abscess. Approximately 80% of all cases occur in patients with head injuries and craniofacial fractures. Despite technical advances in the diagnosis and management of CSF rhinorrhea caused by craniofacial injury through the introduction of MRI and endoscopic extracranial surgical approaches, difficulties remain. The authors review here the pathophysiology, diagnosis, and management of CSF rhinorrhea relevant exclusively to traumatic anterior skull base injuries and attempt to identify areas in which further work is needed. (http://thejns.org/doi/abs/10.3171/2012.4.FOCUS1244) KEY WORDS • craniomaxillofacial trauma • head trauma • cerebrospinal fluid rhinorrhea • meningitis • dural repair • endoscopic surgery • skull base fracture EREBROSPINAL fluid rhinorrhea is a serious and po- Furthermore, the issues related to CSF leak caused tentially fatal condition that still presents a major by traumatic injury are complex and multiple. Having challenge in terms of its diagnosis and manage- conducted a thorough review of existing literature, we Cment. It is estimated that meningitis develops in approxi- discuss here the pathophysiology, diagnosis, and man- mately 10%–25% of patients with this disorder, and 10% agement of CSF rhinorrhea relevant to traumatic anterior of them die as a result. Approximately 80% of all cases of skull base injuries and attempt to identify areas in which CSF rhinorrhea are caused by head injuries that are asso- further research is needed. -

Guidelines for BLS/ALS Medical Providers Current As of March 2019
Tactical Emergency Casualty Care (TECC) Guidelines for BLS/ALS Medical Providers Current as of March 2019 DIRECT THREAT CARE (DTC) / HOT ZONE Guidelines: 1. Mitigate any immediate threat and move to a safer position (e.g. initiate fire attack, coordinated ventilation, move to safe haven, evacuate from an impending structural collapse, etc). Recognize that threats are dynamic and may be ongoing, requiring continuous threat assessments. 2. Direct the injured first responder to stay engaged in the operation if able and appropriate. 3. Move patient to a safer position: a. Instruct the alert, capable patient to move to a safer position and apply self-aid. b. If the patient is responsive but is injured to the point that he/she cannot move, a rescue plan should be devised. c. If a patient is unresponsive, weigh the risks and benefits of an immediate rescue attempt in terms of manpower and likelihood of success. Remote medical assessment techniques should be considered to identify patients who are dead or have non-survivable wounds. 4. Stop life threatening external hemorrhage if present and reasonable depending on the immediate threat, severity of the bleeding and the evacuation distance to safety. Consider moving to safety prior to application of the tourniquet if the situation warrants. a. Apply direct pressure to wound, or direct capable patient to apply direct pressure to own wound and/or own effective tourniquet. b. Tourniquet application: i. Apply the tourniquet as high on the limb as possible, including over the clothing if present. ii. Tighten until cessation of bleeding and move to safety.