Head & Neck Surgery Course
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Gross Anatomy
www.BookOfLinks.com THE BIG PICTURE GROSS ANATOMY www.BookOfLinks.com Notice Medicine is an ever-changing science. As new research and clinical experience broaden our knowledge, changes in treatment and drug therapy are required. The authors and the publisher of this work have checked with sources believed to be reliable in their efforts to provide information that is complete and generally in accord with the standards accepted at the time of publication. However, in view of the possibility of human error or changes in medical sciences, neither the authors nor the publisher nor any other party who has been involved in the preparation or publication of this work warrants that the information contained herein is in every respect accurate or complete, and they disclaim all responsibility for any errors or omissions or for the results obtained from use of the information contained in this work. Readers are encouraged to confirm the infor- mation contained herein with other sources. For example and in particular, readers are advised to check the product information sheet included in the package of each drug they plan to administer to be certain that the information contained in this work is accurate and that changes have not been made in the recommended dose or in the contraindications for administration. This recommendation is of particular importance in connection with new or infrequently used drugs. www.BookOfLinks.com THE BIG PICTURE GROSS ANATOMY David A. Morton, PhD Associate Professor Anatomy Director Department of Neurobiology and Anatomy University of Utah School of Medicine Salt Lake City, Utah K. Bo Foreman, PhD, PT Assistant Professor Anatomy Director University of Utah College of Health Salt Lake City, Utah Kurt H. -

Fossa of Rosenmüller Rosenmüller
Quick Review: Fossa of pharyngeal recess or the fossa of Rosenmüller Rosenmüller. The nasopharynx is a fibromuscular sling suspended from the skull base. The human nasopharynx is mainly derived from the primitive pharynx. It represents the nasal portion of the pharynx behind the nasal cavity and above the free border of the soft palate. The nasopharynx communicates with the nasal cavities through posterior nasal apertures. The choanal orifices along with the posterior edge of the Saggital section of the postnasal space (L E Loh et al 1991) nasal septum form the anterior boundary of the nasopharynx. The The superior constrictor muscle does superior surface of the soft palate not reach the base of skull hence a constitutes its floor and lateral gap (sinus of Morgagni) is velopharyngeal isthum provides created. Fossa of Rosenmüller is a communication between nasopharynx herniation of the nasopharyngeal and oropharynx. The body of mucosa through this deficiency sphenoid, basiocciput and first and between skull base and superior most second cervical vertebrae combine to fibers of the superior constrictor form roof of the nasopharynx. muscle. Through this gap bridged only by the pharyngobasilar fascia, the The part of nasopharynx proximal to eustachian tube enters the the tubal orifice is innervated by the nasopharynx with its two muscles, one maxillary division of the trigeminal (V) on each side. Along the inferior border nerve, and that posterior to the tubal of the two muscles the Fossa of orifice by the glossopharyngeal (IX) Rosenmüller is separated from the nerve. parapharyngeal space by mucosa and pharyngobasilar fascia. Functional studies with contrast and cinefluorography reveal structural The borders of the Fossa of differences between the two Rosenmüller are: components. -
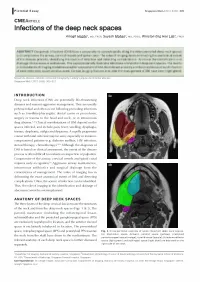
Infections of the Deep Neck Spaces
!Pictorial Essay Singapore Med J 2012; 53(5) 305 CM EARTICLE Infections of the deep neck spaces Amogh Hegdel, MD, FRCR, Suyash Mohan2, MD, PDCC, Winston Eng Hoe Lima, FRCR ABSTRACT Deep neck infections (DNI) have a propensity to spread rapidly along the interconnected deep neck spaces and compromise the airway, cervical vessels and spinal canal. The value of imaging lies in delineating the anatomical extent of the disease process, identifying the source of infection and detecting complications. Its role in the identification and drainage of abscesses is well known. This paper pictorially illustrates infections of important deep neck spaces. The merits and drawbacks of imaging modalities used for assessment of DNI, the relevant anatomy and the possible sources of infection of each deep neck space are discussed. Certain imaging features that alter the management of DNI have been highlighted. Keywords: abscess, cellulitis, computed tomography, Ludwig's angina, peritonsillar abscess Singapore Med J2012; 53(5): 305-312 INTRODUCTION la Deep neck infections (DNI) are potentially life -threatening diseases and warrant aggressive management. They are usually polymicrobial and often occur following preceding infections such as tonsillitis/pharyngitis, dental caries or procedures, surgery or trauma to the head and neck, or in intravenous drug abusers.(1,2) Clinical manifestations of DNI depend on the EJ spaces infected, and include pain, fever, swelling, dysphagia, trismus, dysphonia, otalgia and dyspnoea. A rapidly progressive course with fatal outcome may be seen, especially in immuno- compromised patients (e.g. diabetes mellitus, HIV infection, steroid therapy, chemotherapy).(' -3) Although the diagnosis of DNI is based on clinical assessment, the extent of the disease process is often difficult to evaluate on inspection or palpation. -

Transoral Robotic Assisted Resection of the Parapharyngeal Space
UCLA UCLA Previously Published Works Title Transoral robotic assisted resection of the parapharyngeal space. Permalink https://escholarship.org/uc/item/0wh104s6 Journal Head & neck, 37(2) ISSN 1043-3074 Author Mendelsohn, Abie H Publication Date 2015-02-01 DOI 10.1002/hed.23724 Peer reviewed eScholarship.org Powered by the California Digital Library University of California OPERATIVE TECHNIQUES–PICTORIAL ESSAY Transoral robotic assisted resection of the parapharyngeal space Abie H. Mendelsohn, MD* Director - Robotic Head & Neck Surgery Program, Department of Head and Neck Surgery, David Geffen School of Medicine at University of California – Los Angeles, Los Angeles, California and Jonsson Comprehensive Cancer Center, David Geffen School of Medicine at University of California – Los Angeles, Los Angeles, California. Accepted 28 April 2014 Published online 15 November 2014 in Wiley Online Library (wileyonlinelibrary.com). DOI 10.1002/hed.23724 ABSTRACT: Background. Preliminary case series have reported clinical Results. Transoral robotic assisted resection of a 54- 3 46-mm paraphar- feasibility and safety of a transoral minimally invasive technique to yngeal space mass was performed, utilizing 97 minutes of robotic surgical approach parapharyngeal space masses. With the assistance of the sur- time. Pictorial demonstration of the robotic resection is provided. gical robotic system, tumors within the parapharyngeal space can now Conclusion. Parapharyngeal space tumors have traditionally been be excised safely without neck incisions. A detailed technical description approached via transcervical skin incisions, typically including blunt dissection is included. from tactile feedback. The transoral robotic approach offers magnified 3D Methods. After developing compressive symptoms from a parapharyng- visualization of the parapharyngeal space that allows for complete and safe eal space lipomatous tumor, the patient was referred by his primary oto- resection. -

Deep Neck Infections 55
Deep Neck Infections 55 Behrad B. Aynehchi Gady Har-El Deep neck space infections (DNSIs) are a relatively penetrating trauma, surgical instrument trauma, spread infrequent entity in the postpenicillin era. Their occur- from superfi cial infections, necrotic malignant nodes, rence, however, poses considerable challenges in diagnosis mastoiditis with resultant Bezold abscess, and unknown and treatment and they may result in potentially serious causes (3–5). In inner cities, where intravenous drug or even fatal complications in the absence of timely rec- abuse (IVDA) is more common, there is a higher preva- ognition. The advent of antibiotics has led to a continu- lence of infections of the jugular vein and carotid sheath ing evolution in etiology, presentation, clinical course, and from contaminated needles (6–8). The emerging practice antimicrobial resistance patterns. These trends combined of “shotgunning” crack cocaine has been associated with with the complex anatomy of the head and neck under- retropharyngeal abscesses as well (9). These purulent col- score the importance of clinical suspicion and thorough lections from direct inoculation, however, seem to have a diagnostic evaluation. Proper management of a recog- more benign clinical course compared to those spreading nized DNSI begins with securing the airway. Despite recent from infl amed tissue (10). Congenital anomalies includ- advances in imaging and conservative medical manage- ing thyroglossal duct cysts and branchial cleft anomalies ment, surgical drainage remains a mainstay in the treat- must also be considered, particularly in cases where no ment in many cases. apparent source can be readily identifi ed. Regardless of the etiology, infection and infl ammation can spread through- Q1 ETIOLOGY out the various regions via arteries, veins, lymphatics, or direct extension along fascial planes. -

Nontraumatic Head and Neck Injuries: a Clinical Approach. Part 2 183
Radiología. 2017;59(3):182---195 www.elsevier.es/rx UPDATE IN RADIOLOGY Nontraumatic head and neck injuries: A clinical ଝ approach. Part 2 ∗ B. Brea Álvarez , L. Esteban García, M. Tunón˜ Gómez, Y. Cepeda Ibarra Hospital Universitario Puerta de Hierro-Majadahonda, Majadahonda, Madrid, Spain Received 3 May 2016; accepted 16 February 2017 KEYWORDS Abstract Nontraumatic emergencies of the head and neck represent a challenge in the field of Emergencies; neuroradiology for two reasons. As explained in the first part of this update, these entities affect Neck injuries; an area where the thorax joins the cranial cavity and can thus compromise both structures; Orbital diseases; second, they are uncommon, so they are not well known. Diseases of the Maintaining the same approach as in the first part, focusing on the clinical presentations in the paranasal sinus; emergency department rather than on the anatomic regions affected, we will study the entities Sialadenitis; that present with two patterns: those that present with a combination of cervical numbness, Cellulitis; dysphagia, and dyspnoea and those that present with acute sensory deficits. In the latter group, Diagnostic imaging; we will specifically focus on visual deficits, because this is the most common symptom that calls Computed for urgent imaging studies. tomography; © 2017 SERAM. Published by Elsevier Espana,˜ S.L.U. All rights reserved. Magnetic resonance imaging PALABRAS CLAVE Urgencias no traumáticas de cabeza y cuello: aproximación desde la clínica. Parte 2 Urgencias; Resumen Las urgencias no traumáticas de cabeza y cuello son un reto en el campo neurorra- Lesiones del cuello; Enfermedades diológico por los motivos referidos en la primera parte: su área de afectación, en la encrucijada orbitarias; del tórax y la cavidad craneal, y su baja incidencia en la urgencia, lo que supone que sean poco conocidas. -

6. the Pharynx the Pharynx, Which Forms the Upper Part of the Digestive Tract, Consists of Three Parts: the Nasopharynx, the Oropharynx and the Laryngopharynx
6. The Pharynx The pharynx, which forms the upper part of the digestive tract, consists of three parts: the nasopharynx, the oropharynx and the laryngopharynx. The principle object of this dissection is to observe the pharyngeal constrictors that form the back wall of the vocal tract. Because the cadaver is lying face down, we will consider these muscles from the back. Figure 6.1 shows their location. stylopharyngeus suuperior phayngeal constrictor mandible medial hyoid bone phayngeal constrictor inferior phayngeal constrictor Figure 6.1. Posterior view of the muscles of the pharynx. Each of the three pharyngeal constrictors has a left and right part that interdigitate (join in fingerlike branches) in the midline, forming a raphe, or union. This raphe forms the back wall of the pharynx. The superior pharyngeal constrictor is largely in the nasopharynx. It has several origins (some texts regard it as more than one muscle) one of which is the medial pterygoid plate. It assists in the constriction of the nasopharynx, but has little role in speech production other than helping form a site against which the velum may be pulled when forming a velic closure. The medial pharyngeal constrictor, which originates on the greater horn of the hyoid bone, also has little function in speech. To some extent it can be considered as an elevator of the hyoid bone, but its most important role for speech is simply as the back wall of the vocal tract. The inferior pharyngeal constrictor also performs this function, but plays a more important role constricting the pharynx in the formation of pharyngeal consonants. -

Esophagopharyngeal Perforation and Prevertebral Abscess After Anterior Cervical Discectomy and Fusion: a Case Report
232 Case Report Esophagopharyngeal perforation and prevertebral abscess after anterior cervical discectomy and fusion: a case report Jay K. Shah1^, Filippo Romanelli1, Jason Yang2, Naina Rao3, Michael C. Gerling4 1Division of Orthopedic Surgery, Department of Orthopedic Surgery, Jersey City Medical Center – Robertwood Johnson Barnabas Health, Jersey City, NJ, USA; 2Robert Wood Johnson University Hospital, RWJBarnabas Health, New Brunswick, NJ, USA; 3New York Grossman School of Medicine, NYU Langone Health, New York, NY, USA; 4Chief of Spine Surgery, Department of Orthopaedic Surgery, New York University Langone Hospital-Brooklyn, Tribeca, New York, NY, USA Correspondence to: Jay K. Shah, DO. Division of Orthopedic Surgery, Department of Orthopedic Surgery, Jersey City Medical Center – Robertwood Johnson Barnabas Health, 355 Grand Street, Jersey City, NJ 07302, USA. Email: [email protected]. Abstract: Anterior cervical discectomy and fusion (ACDF) represents one of the most commonly performed spine surgeries. Dysphagia secondary to esophageal injury during retraction is one of the most common complications, and usually leads to self-limiting dysphagia. However, actual perforation and violation of the esophageal tissue is much rarer and can lead to delayed deep infections. Prevertebral abscess’ are one of the most feared complications after ACDF, as they can lead to severe tissue swelling, osteomyelitis, hardware failure, and even death. Due to their rarity, a gold standard of workup and treatment is still unknown. A healthy 47-year-old female presents 9 months after a C4–C7 ACDF done at an outside institution with a large prevertebral abscess, osteomyelitis, hardware failure, and pseudoarthrosis secondary to esophagopharyngeal defect and prominent hardware. Overall, the patient underwent eight surgeries, and required an extended course of intravenous (IV) antibiotics, multiple diagnostic procedures, and complex soft tissue coverage using an anterolateral thigh free flap. -

Head and Neck Specimens
Head and Neck Specimens DEFINITIONS AND GENERAL COMMENTS: All specimens, even of the same type, are unique, and this is particularly true for Head and Neck specimens. Thus, while this outline is meant to provide a guide to grossing the common head and neck specimens at UAB, it is not all inclusive and will not capture every scenario. Thus, careful assessment of each specimen with some modifications of what follows below may be needed on a case by case basis. When in doubt always consult with a PA, Chief/Senior Resident and/or the Head and Neck Pathologist on service. Specimen-derived margin: A margin taken directly from the main specimen-either a shave or radial. Tumor bed margin: A piece of tissue taken from the operative bed after the main specimen has been resected. This entire piece of tissue may represent the margin, or it could also be specifically oriented-check specimen label/requisition for any further orientation. Margin status as determined from specimen-derived margins has been shown to better predict local recurrence as compared to tumor bed margins (Surgical Pathology Clinics. 2017; 10: 1-14). At UAB, both methods are employed. Note to grosser: However, even if a surgeon submits tumor bed margins separately, the grosser must still sample the specimen margins. Figure 1: Shave vs radial (perpendicular) margin: Figure adapted from Surgical Pathology Clinics. 2017; 10: 1-14): Red lines: radial section (perpendicular) of margin Blue line: Shave of margin Comparison of shave and radial margins (Table 1 from Chiosea SI. Intraoperative Margin Assessment in Early Oral Squamous Cell Carcinoma. -

Board Review for Anatomy
Board Review for Anatomy John A. McNulty, Ph.D. Spring, 2005 . LOYOLA UNIVERSITY CHICAGO Stritch School of Medicine Key Skeletal landmarks • Head - mastoid process, angle of mandible, occipital protuberance • Neck – thyroid cartilage, cricoid cartilage • Thorax - jugular notch, sternal angle, xiphoid process, coracoid process, costal arch • Back - vertebra prominence, scapular spine (acromion), iliac crest • UE – epicondyles, styloid processes, carpal bones. • Pelvis – ant. sup. iliac spine, pubic tubercle • LE – head of fibula, malleoli, tarsal bones Key vertebral levels • C2 - angle of mandible • C4 - thyroid notch • C6 - cricoid cartilage - esophagus, trachea begin • C7 - vertebra prominence • T2 - jugular notch; scapular spine • T4/5 - sternal angle - rib 2 articulates, trachea divides • T9 - xiphisternum • L1/L2 - pancreas; spinal cord ends. • L4 - iliac crest; umbilicus; aorta divides • S1 - sacral promontory Upper limb nerve lesions Recall that any muscle that crosses a joint, acts on that joint. Also recall that muscles innervated by individual nerves within compartments tend to have similar actions. • Long thoracic n. - “winged” scapula. • Upper trunk (C5,C6) - Erb Duchenne - shoulder rotators, musculocutaneous • Lower trunk (C8, T1) - Klumpke’s - ulnar nerve (interossei muscle) • Radial nerve – (Saturday night palsy) - wrist drop • Median nerve (recurrent median) – thenar compartment - thumb • Ulnar nerve - interossei muscles. Lower limb nerve lesions Review actions of the various compartments. • Lumbosacral lesions - usually -

Computed Tomography of the Buccomasseteric Region: 1
605 Computed Tomography of the Buccomasseteric Region: 1. Anatomy Ira F. Braun 1 The differential diagnosis to consider in a patient presenting with a buccomasseteric James C. Hoffman, Jr. 1 region mass is rather lengthy. Precise preoperative localization of the mass and a determination of its extent and, it is hoped, histology will provide a most useful guide to the head and neck surgeon operating in this anatomically complex region. Part 1 of this article describes the computed tomographic anatomy of this region, while part 2 discusses pathologic changes. The clinical value of computed tomography as an imaging method for this region is emphasized. The differential diagnosis to consider in a patient with a mass in the buccomas seteric region, which may either be developmental, inflammatory, or neoplastic, comprises a rather lengthy list. The anatomic complexity of this region, defined arbitrarily by the soft tissue and bony structures including and surrounding the masseter muscle, excluding the parotid gland, makes the accurate anatomic diagnosis of masses in this region imperative if severe functional and cosmetic defects or even death are to be avoided during treatment. An initial crucial clinical pathoanatomic distinction is to classify the mass as extra- or intraparotid. Batsakis [1] recommends that every mass localized to the cheek region be considered a parotid tumor until proven otherwise. Precise clinical localization, however, is often exceedingly difficult. Obviously, further diagnosis and subsequent therapy is greatly facilitated once this differentiation is made. Computed tomography (CT), with its superior spatial and contrast resolution, has been shown to be an effective imaging method for the evaluation of disorders of the head and neck. -

Foreign Body Imaging-Experience with 6 Cases of Retained Foreign Bodies in the Emergency
Arch Clin Med Case Rep 2020; 4 (5): 952-968 DOI: 10.26502/acmcr.96550285 Case Series Foreign Body Imaging-Experience with 6 Cases of Retained Foreign Bodies in the Emergency Radiology Unit Muniraju Maralakunte MD1, Uma Debi MD1*, Lokesh Singh MD1, Himanshu Pruthi MD1, Vikas Bhatia MD, DNB DM1, Gita Devi MD1, Sandhu MS MD1 2Department of Radio diagnosis, PGIMER, Chandigarh, India *Corresponding Author: Dr. Uma Debi, Radiodiagnosis and Imaging, PGIMER, Chandigarh, India, Tel: 0091- 172-2756381; Fax: 0091-172-2745768; E-mail: [email protected] Received: 22 June 2020; Accepted: 14 August 2020; Published: 21 September 2020 Abstract Introduction: Retained foreign bodies are the external objects lying within the body, which are placed with voluntary or involuntary intentions. The involuntarily or accidentally, and complicated cases with the retained foreign body may come to the emergency services, which may require rapid and adequate imaging assessment. Materials and methods: We share our experience with six different cases with retained foreign bodies, who visited emergency radiological services with acute presentation of symptoms. The choice of radiological investigation considered based on the clinical presentation of the subjects with a retained foreign body. Conclusion: Patients with the retained foreign body may present acute symptoms to the emergency medical or surgical services, radiologists play a central role in rapid imaging evaluation. Radiological investigation plays a crucial role in identification, localization, characterization, and reporting the complication of the retained foreign bodies, and in many scenarios, radiological investigations may expose the unsuspected or concealed foreign bodies in the human body. Ultimately radiological services are useful rapid assessment tools that aid in triage and guide in the medical or surgical management of patients with a retained foreign body.