ODONTOGENTIC INFECTIONS Infection Spread Determinants
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Management of Saliva and Drooling Excessive Saliva and Drooling Affects up to 50% of People with Parkinson’S (PD)
Management of Saliva and Drooling Excessive saliva and drooling affects up to 50% of people with Parkinson’s (PD). Drooling can be embarrassing and can limit social interactions for the person with PD. Saliva and Drooling Parkinson Information Parkinson It can also be an important symptom of swallowing difficulty, which can increase the risk of choking on saliva. People with Parkinson’s disease do not swallow automatically due to rigidity and impaired mobility of the muscles of the palate, throat and esophagus. Saliva pools in the mouth and can potentially become a hazard since swallowing into the lungs carries the risk of pneumonia. If you have poor posture, saliva collects in the front of the mouth, resulting in drooling. Cause and symptoms Decreased control of saliva is most often caused by changes in the ability to swallow, rather than from producing too much saliva. A common cause of drooling for people with PD is the weakening and/or loss of motor control of the muscles involved in swallowing. You may experience one or more of the following symptoms: • Decreased ability to keep your mouth closed at rest, known as the “open mouth posture” • Difficulty keeping lips closed • Lack of awareness of the saliva in your mouth • Wetness at the sides of your mouth • A wet sounding voice • Drooling with posture changes • Coughing and/or choking Evaluation and treatment Speak with your physician about all symptoms that may not be related to PD. If you are experiencing drooling or choking on your saliva, you may require a swallowing evaluation by a Speech Language Pathologist. -

Natural History of Odontogenic Infection
Natural History of Odontogenic Infection The usual cause of odontogenic infections is necrosis of the pulp of the tooth, which is followed by bacterial invasion through the pulp chamber and into the deeper tissues. Necrosis of the pulp is the result of deep caries in the tooth, to which the pulp responds with a typical inflammatory reaction. Vasodilation and edema cause pressure in the tooth and severe pain as the rigid walls of the tooth prevent swelling. If left untreated the pressure leads to strangulation of the blood supply to the tooth through the apex and consequent necrosis. The necrotic pulp then provides a perfect setting for bacterial invasion into the bone tissue. Once the bacteria have invaded the bone, the infection spreads equally in all directions until a cortical plate is encountered. During the time of intrabony spread, the patient usually experiences sufficient pain to seek treatment. Extraction of the tooth (or removal of the necrotic pulp by an endodontic procedure) results in resolution of the infection. Direction of Spread of Infection The direction of the infection's spread from the tooth apex depends on the thickness of the overlying bone and the relationship of the bone's perforation site to the muscle attachments of the jaws. If no treatment is provided for it, the infection erodes through the thinnest, nearest cortical plate of bone and into the overlying soft tissue. If the root apex is centrally located, the infection erodes through the thinnest bone first. In the maxilla the thinner bone is the labial-buccal side; the palatal cortex is thicker. -

Accidental Displacement of Mandibular Third Molar Root Into the Submandibular Space: a Case Report
Case Report ERA’S JOURNAL OF MEDICAL RESEARCH VOL.6 NO.1 ACCIDENTAL DISPLACEMENT OF MANDIBULAR THIRD MOLAR ROOT INTO THE SUBMANDIBULAR SPACE: A CASE REPORT Mayur Vilas Limbhore, Viren S Patil, Shandilya Ramanojam, Vrushika Mahajan, Pallavi Rathi, Kisna Tadas Department of Oral and Maxillofacial surgery Bharati Vidyapeeth Dental College, Katraj, Pune, Maharashtra, India-411030 Received on : 01-04-2018 Accpected on : 10-04-2018 ABSTRACT Address for correspondence Accidental displacement of an impacted third molar, either a crown, Dr. Mayur Vilas Limbhore root piece, or the entire tooth, is a rare complication that occurs Department of Oral and Maxillofacial Surgery during surgical removal. The most common sites of dislodgment of an impacted mandibular third molar root are the submandibular, Bharati Vidyapeth Dental College, sublingual and pterygomandibular spaces. Removal of a displaced Katraj, Pune, Maharashtra, India-411030 root from these spaces may be complex due to poor visualization Email: [email protected] and limited access. A thorough evaluation of all significant risk Contact no: +91-8552887325 factors must be performed in advance to prevent complications. This case report reveals the management of accidental displaced mandibular third molar root into the submandibular space. An 39 years-old male patient underwent a third mandibular molar extraction. Accidentally, the mandibular right third molar distal root was displaced into the submandibular space, making necessary a second surgical step. After 2 days awaiting an asymptomatic health status, the second surgical step was successfully performed using multislice CBCT as preoperative imaging guide. The present case report highlights the clinical usefulness of CBCT in proper treatment of the patient. -

16. Questions and Answers
16. Questions and Answers 1. Which of the following is not associated with esophageal webs? A. Plummer-Vinson syndrome B. Epidermolysis bullosa C. Lupus D. Psoriasis E. Stevens-Johnson syndrome 2. An 11 year old boy complains that occasionally a bite of hotdog “gives mild pressing pain in his chest” and that “it takes a while before he can take another bite.” If it happens again, he discards the hotdog but sometimes he can finish it. The most helpful diagnostic information would come from A. Family history of Schatzki rings B. Eosinophil counts C. UGI D. Time-phased MRI E. Technetium 99 salivagram 3. 12 year old boy previously healthy with one-month history of difficulty swallowing both solid and liquids. He sometimes complains food is getting stuck in his retrosternal area after swallowing. His weight decreased approximately 5% from last year. He denies vomiting, choking, gagging, drooling, pain during swallowing or retrosternal pain. His physical examination is normal. What would be the appropriate next investigation to perform in this patient? A. Upper Endoscopy B. Upper GI contrast study C. Esophageal manometry D. Modified Barium Swallow (MBS) E. Direct laryngoscopy 4. A 12 year old male presents to the ER after a recent episode of emesis. The parents are concerned because undigested food 3 days old was in his vomit. He admits to a sensation of food and liquids “sticking” in his chest for the past 4 months, as he points to the upper middle chest. Parents relate a 10 lb (4.5 Kg) weight loss over the past 3 months. -

Ludwig's Angina: Causes Symptoms and Treatment
Aishwarya Balakrishnan et al /J. Pharm. Sci. & Res. Vol. 6(10), 2014, 328-330 Ludwig’s Angina: Causes Symptoms and Treatment Aishwarya Balakrishnan,M.S Thenmozhi, Saveetha Dental College Abstract : Ludwigs angina is a disease which is characterised by the infection in the floor of the oral cavity. Ludwig's angina is also otherwise commonly known as "angina". Previously this disease was deemed as fatal but later on it was concluded that with proper treatment this infection can be removed and the pateint can recover. It mostly occurs in adults and children are not affected by this disease. As the infection spreads further it would affect the wind pipe and lead to swellings of the neck. The skin around the neck would also be infected severely and lead to redness. The individual would mostly be febrile during this time. Since the airway is blocked the individual would suffer from difficulty in breathing. If the infection spreads to the internal ear then the individual may have audio impairment. The main cause for this disease is dental infections caused due to improper dental hygiene. Keywords: Ludwigsangina ,trasechtomy, fiberoptic intubation INTRODUCTION: piercing(6)(8)(7). In a study that was conducted on 16 Ludwig's angina, otherwise known as Angina Ludovici, is a different patients suffering from ludwigs angina, serious, potentially life-threatening cellulitis, or connective Odontogenic infection was the commonest aetiologic factor tissue infection, of the floor of the mouth, usually occurring observed in 12 cases (75%), trauma was responsible for 2 in adults with concomitant dental infections and if left (12.5%) while in the remaining 2 patients (12.5%) the untreated, may obstruct the airways, necessitating cause could not be determined. -

CASE REPORT Fibromatosis of Infratemporal Space Riaz Ahmed Warraich, Tooba Saeed, Nabila Riaz, Asma Aftab
217 CASE REPORT Fibromatosis of infratemporal space Riaz Ahmed Warraich, Tooba Saeed, Nabila Riaz, Asma Aftab Abstract chemotherapy or non-cytotoxic drugs are also Fibromatosis is a rare benign mesenchymal neoplasm considerable modalities for AF management, to avoid which primarily originates in the muscle, connective sacrifising functional integrity as a price of attaining tissue, fascial sheaths, and musculoaponeurotic tumour-free margins. 3 structures. It is commonly seen as abdominal tumour but Case Report in maxillofacial region, the occurrence of these tumours is very rare and exceedingly rare in infratemporal space. A 35-year-old female visited Oral and Maxillofacial Often misdiagnosed due to its varied clinical behaviour, Department of Mayo Hospital on October 5, 2014. Written fibromatosis is benign, slow-growing, infiltrative tumour informed consent was obtained from the patient for without any metastatic potential, but is locally aggressive publication of this report and accompanying images. Her causing organ dysfunction along with high recurrence chief complaint was of progressive reduction in mouth rate. We report a case of fibromatosis involving the left opening gradually for the preceding 4 years. Medical infratemporal space in a 35-year-old female who history revealed that she had extra pulmonary presented with chief complaint of limited mouth opening tuberculous lesion in left side of her neck which was for the preceding 4 years. treated 10 years earlier. Clinical examination revealed slight thickening and fibrosis of left cheek with zero Keywords: Aggressive fibromatosis, Infratemporal, mouth opening. Overlying skin was normal. There was no Benign, Infiltrative. Introduction Aggressive fibromatosis (AF) or extra-abdominal desmoid tumours are rare tumours of fibroblastic origin involving the proliferation of cytologically benign fibrocytes. -

Dental Management of the Head and Neck Cancer Patient Treated
Dental Management of the Head and Neck Cancer Patient Treated with Radiation Therapy By Carol Anne Murdoch-Kinch, D.D.S., Ph.D., and Samuel Zwetchkenbaum, D.D.S., M.P.H. pproximately 36,540 new cases of oral cavity and from radiation injury to the salivary glands, oral mucosa pharyngeal cancer will be diagnosed in the USA and taste buds, oral musculature, alveolar bone, and this year; more than 7,880 people will die of this skin. They are clinically manifested by xerostomia, oral A 1 disease. The vast majority of these cancers are squamous mucositis, dental caries, accelerated periodontal disease, cell carcinomas. Most cases are diagnosed at an advanced taste loss, oral infection, trismus, and radiation dermati- stage: 62 percent have regional or distant spread at the tis.4 Some of these effects are acute and reversible (muco- time of diagnosis.2 The five-year survival for all stages sitis, taste loss, oral infections and xerostomia) while oth- combined is 61 percent.1 Localized tumors (Stage I and II) ers are chronic (xerostomia, dental caries, accelerated can usually be treated surgically, but advanced cancers periodontal disease, trismus, and osteoradionecrosis.) (Stage III and IV) require radiation with or without che- Chemotherapeutic agents may be administered as an ad- motherapy as adjunctive or definitive treatment.1 See Ta- junct to RT. Patients treated with multimodality chemo- ble 1.3 Therefore, most patients with oral cavity and pha- therapy and RT may be at greater risk for oral mucositis ryngeal cancer receive head and neck radiation therapy and secondary oral infections such as candidiasis. -
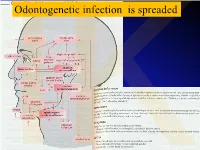
Anatomical Overview
IKOdontogenetic infection is spreaded Možné projevy zlomenin a zánětů IKPossible signs of fractures or inflammations Submandibular space lies between the bellies of the digastric muscles, mandible, mylohyoid muscle and hyoglossus and styloglossus muscles IK IK IK IK IK Submandibulární absces Submandibular abscess IK Sběhlý submandibulární absces Submandibular abscess is getting down IK Submental space lies between the mylohyoid muscles and the investing layer of deep cervical fascia superficially IK IK Spatium peritonsillare IK IK Absces v peritonsilární krajině Abscess in peritonsilar region IK Fasciae Neck fasciae cervicales Demarcate spaces • fasciae – Superficial (investing): • f. nuchae, f. pectoralis, f. deltoidea • invests m. sternocleidomastoideus + trapezius • f. supra/infrahyoidea – pretrachealis (middle neck f.) • form Δ, invests infrahyoid mm. • vagina carotica (carotic sheet) – Prevertebral (deep cervical f.) • Covers scaleni mm. IK• Alar fascia Fascie Fascia cervicalis superficialis cervicales Fascia cervicalis media Fascia cervicalis profunda prevertebralis IKsuperficialis pretrachealis Neck spaces - extent • paravisceral space – Continuation of parafaryngeal space – Nervous and vascular neck bundle • retrovisceral space – Between oesophagus and prevertebral f. – Previsceral space – mezi l. pretrachealis a orgány – v. thyroidea inf./plx. thyroideus impar • Suprasternal space – Between spf. F. and pretracheal one IK– arcus venosus juguli 1 – sp. suprasternale suprasternal Spatia colli 2 – sp. pretracheale pretracheal 3 – -
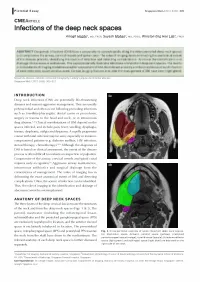
Infections of the Deep Neck Spaces
!Pictorial Essay Singapore Med J 2012; 53(5) 305 CM EARTICLE Infections of the deep neck spaces Amogh Hegdel, MD, FRCR, Suyash Mohan2, MD, PDCC, Winston Eng Hoe Lima, FRCR ABSTRACT Deep neck infections (DNI) have a propensity to spread rapidly along the interconnected deep neck spaces and compromise the airway, cervical vessels and spinal canal. The value of imaging lies in delineating the anatomical extent of the disease process, identifying the source of infection and detecting complications. Its role in the identification and drainage of abscesses is well known. This paper pictorially illustrates infections of important deep neck spaces. The merits and drawbacks of imaging modalities used for assessment of DNI, the relevant anatomy and the possible sources of infection of each deep neck space are discussed. Certain imaging features that alter the management of DNI have been highlighted. Keywords: abscess, cellulitis, computed tomography, Ludwig's angina, peritonsillar abscess Singapore Med J2012; 53(5): 305-312 INTRODUCTION la Deep neck infections (DNI) are potentially life -threatening diseases and warrant aggressive management. They are usually polymicrobial and often occur following preceding infections such as tonsillitis/pharyngitis, dental caries or procedures, surgery or trauma to the head and neck, or in intravenous drug abusers.(1,2) Clinical manifestations of DNI depend on the EJ spaces infected, and include pain, fever, swelling, dysphagia, trismus, dysphonia, otalgia and dyspnoea. A rapidly progressive course with fatal outcome may be seen, especially in immuno- compromised patients (e.g. diabetes mellitus, HIV infection, steroid therapy, chemotherapy).(' -3) Although the diagnosis of DNI is based on clinical assessment, the extent of the disease process is often difficult to evaluate on inspection or palpation. -

Transoral Robotic Assisted Resection of the Parapharyngeal Space
UCLA UCLA Previously Published Works Title Transoral robotic assisted resection of the parapharyngeal space. Permalink https://escholarship.org/uc/item/0wh104s6 Journal Head & neck, 37(2) ISSN 1043-3074 Author Mendelsohn, Abie H Publication Date 2015-02-01 DOI 10.1002/hed.23724 Peer reviewed eScholarship.org Powered by the California Digital Library University of California OPERATIVE TECHNIQUES–PICTORIAL ESSAY Transoral robotic assisted resection of the parapharyngeal space Abie H. Mendelsohn, MD* Director - Robotic Head & Neck Surgery Program, Department of Head and Neck Surgery, David Geffen School of Medicine at University of California – Los Angeles, Los Angeles, California and Jonsson Comprehensive Cancer Center, David Geffen School of Medicine at University of California – Los Angeles, Los Angeles, California. Accepted 28 April 2014 Published online 15 November 2014 in Wiley Online Library (wileyonlinelibrary.com). DOI 10.1002/hed.23724 ABSTRACT: Background. Preliminary case series have reported clinical Results. Transoral robotic assisted resection of a 54- 3 46-mm paraphar- feasibility and safety of a transoral minimally invasive technique to yngeal space mass was performed, utilizing 97 minutes of robotic surgical approach parapharyngeal space masses. With the assistance of the sur- time. Pictorial demonstration of the robotic resection is provided. gical robotic system, tumors within the parapharyngeal space can now Conclusion. Parapharyngeal space tumors have traditionally been be excised safely without neck incisions. A detailed technical description approached via transcervical skin incisions, typically including blunt dissection is included. from tactile feedback. The transoral robotic approach offers magnified 3D Methods. After developing compressive symptoms from a parapharyng- visualization of the parapharyngeal space that allows for complete and safe eal space lipomatous tumor, the patient was referred by his primary oto- resection. -

29360-Oral Cavity Dr. Alexandra Borges.Pdf
ORAL CAVITY: ANATOMY AND PATHOLOGIES Alexandra Borges, MD COI Disclosure Instituto Português de Oncologia de Lisboa I have nothing to disclose Champalimaud Foundation Lisbon, Portugal ECHNNR 2021 ECHNNR 2021 MR ANATOMY LEARNING OBJECTIVES • Become familiar with OC anatomy and the importance of using adequate terminology when reporting OC studies NASOPHARYNX NASAL CAVITY • Learn how to tailor imaging studies • Understand the different patterns of malignant tumor spread according to the different tumor subsites OROPHARYNX ORAL CAVITY HYPOPHARYNX BOUNDARIES CONTENTS: ORAL TONGUE Superior: • hard palate • superior alveolar ridge Inferior: • floor of the mouth • inferior alveolar ridge ITM Laterally: • cheeks and buccal mucosaosa Anterior: • Lips Posterior: • oropharynx ORAL TONGUE: Extrinsic tongue muscles EM: Styloglossus tongue retraction and elevation Styloglossus Palatoglossus Hyoglossus SG Geniglossus HG GG CN XII CN X EM: Palatoglossus elevation of the tongue EM: Hyoglossus tongue depression and retraction EM: Genioglossus tongue protrusion ORAL TONGUE: Extrinsic muscles GG GH TONGUE INNERVATION ORAL CAVITY IX sensitive and Spatial subdivision taste CN X Motor • Mucosal area • Tongue root • Sublingual space CN XII Motor • Submandibular space Lingual nerve: Sensitive (branch of V3) • Buccomasseteric region Taste (chorda tympani) ORAL MUCOSAL SPACE ROOT OF THE TONGUE 1. Lips 2. Gengiva (sup. alveolar ridge) 3. Gengiva (inf. alveolar ridge) 4. Buccal 5. Palatal 6. Sublingual/FOM 7. Retromolar trigone GG 8. Tongue ROT BOT Vestibule GH Mucosa -

Head & Neck Surgery Course
Head & Neck Surgery Course Parapharyngeal space: surgical anatomy Dr Pierfrancesco PELLICCIA Pr Benjamin LALLEMANT Service ORL et CMF CHU de Nîmes CH de Arles Introduction • Potential deep neck space • Shaped as an inverted pyramid • Base of the pyramid: skull base • Apex of the pyramid: greater cornu of the hyoid bone Introduction • 2 compartments – Prestyloid – Poststyloid Anatomy: boundaries • Superior: small portion of temporal bone • Inferior: junction of the posterior belly of the digastric and the hyoid bone Anatomy: boundaries Anatomy: boundaries • Posterior: deep fascia and paravertebral muscle • Anterior: pterygomandibular raphe and medial pterygoid muscle fascia Anatomy: boundaries • Medial: pharynx (pharyngobasilar fascia, pharyngeal wall, buccopharyngeal fascia) • Lateral: superficial layer of deep fascia • Medial pterygoid muscle fascia • Mandibular ramus • Retromandibular portion of the deep lobe of the parotid gland • Posterior belly of digastric muscle • 2 ligaments – Sphenomandibular ligament – Stylomandibular ligament Aponeurosis and ligaments Aponeurosis and ligaments • Stylopharyngeal aponeurosis: separates parapharyngeal spaces to two compartments: – Prestyloid – Poststyloid • Cloison sagittale: separates parapharyngeal and retropharyngeal space Aponeurosis and ligaments Stylopharyngeal aponeurosis Muscles stylohyoidien Stylopharyngeal , And styloglossus muscles Prestyloid compartment Contents: – Retromandibular portion of the deep lobe of the parotid gland – Minor or ectopic salivary gland – CN V branch to tensor