Head and Neck Cancers
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Microvasculature of Human Infant Oral Mucosa Using Vascular Corrosion Casts and India Ink Injection II
Scanning Microscopy Volume 8 Number 1 Article 13 3-31-1994 The Microvasculature of Human Infant Oral Mucosa Using Vascular Corrosion Casts and India Ink Injection II. Palate and Lip Q. X. Yu Sun Yat-Sen University of Medical Sciences K. M. Pang University of Hong Kong W. Ran Sun Yat-Sen University of Medical Sciences H. P. Philipsen University of Hong Kong X. H. Chen Sun Yat-Sen University of Medical Sciences Follow this and additional works at: https://digitalcommons.usu.edu/microscopy Part of the Biology Commons Recommended Citation Yu, Q. X.; Pang, K. M.; Ran, W.; Philipsen, H. P.; and Chen, X. H. (1994) "The Microvasculature of Human Infant Oral Mucosa Using Vascular Corrosion Casts and India Ink Injection II. Palate and Lip," Scanning Microscopy: Vol. 8 : No. 1 , Article 13. Available at: https://digitalcommons.usu.edu/microscopy/vol8/iss1/13 This Article is brought to you for free and open access by the Western Dairy Center at DigitalCommons@USU. It has been accepted for inclusion in Scanning Microscopy by an authorized administrator of DigitalCommons@USU. For more information, please contact [email protected]. Scanning Microscopy, Vol. 8, No. l, 1994 (Pages 133-139) 0891-7035/94$5.00+ .25 Scanning Microscopy International, Chicago (AMF O'Hare), IL 60666 USA THE MICROVASCULATURE OF HUMAN INFANT ORAL MUCOSA USING VASCULAR CORROSION CASTS AND INDIA INK INJECTION II. PALATE AND LIP Q.X. Yu 1,'", K.M. Pang2, W. Ran 1, H.P. Philipsen 2 and X.H. Chen 1 1Faculty of Stomatology, Sun Yat-Sen University of Medical Sciences, Guangzhou, China. -

Head and Neck
DEFINITION OF ANATOMIC SITES WITHIN THE HEAD AND NECK adapted from the Summary Staging Guide 1977 published by the SEER Program, and the AJCC Cancer Staging Manual Fifth Edition published by the American Joint Committee on Cancer Staging. Note: Not all sites in the lip, oral cavity, pharynx and salivary glands are listed below. All sites to which a Summary Stage scheme applies are listed at the begining of the scheme. ORAL CAVITY AND ORAL PHARYNX (in ICD-O-3 sequence) The oral cavity extends from the skin-vermilion junction of the lips to the junction of the hard and soft palate above and to the line of circumvallate papillae below. The oral pharynx (oropharynx) is that portion of the continuity of the pharynx extending from the plane of the inferior surface of the soft palate to the plane of the superior surface of the hyoid bone (or floor of the vallecula) and includes the base of tongue, inferior surface of the soft palate and the uvula, the anterior and posterior tonsillar pillars, the glossotonsillar sulci, the pharyngeal tonsils, and the lateral and posterior walls. The oral cavity and oral pharynx are divided into the following specific areas: LIPS (C00._; vermilion surface, mucosal lip, labial mucosa) upper and lower, form the upper and lower anterior wall of the oral cavity. They consist of an exposed surface of modified epider- mis beginning at the junction of the vermilion border with the skin and including only the vermilion surface or that portion of the lip that comes into contact with the opposing lip. -

Human Anatomy As Related to Tumor Formation Book Four
SEER Program Self Instructional Manual for Cancer Registrars Human Anatomy as Related to Tumor Formation Book Four Second Edition U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutesof Health SEER PROGRAM SELF-INSTRUCTIONAL MANUAL FOR CANCER REGISTRARS Book 4 - Human Anatomy as Related to Tumor Formation Second Edition Prepared by: SEER Program Cancer Statistics Branch National Cancer Institute Editor in Chief: Evelyn M. Shambaugh, M.A., CTR Cancer Statistics Branch National Cancer Institute Assisted by Self-Instructional Manual Committee: Dr. Robert F. Ryan, Emeritus Professor of Surgery Tulane University School of Medicine New Orleans, Louisiana Mildred A. Weiss Los Angeles, California Mary A. Kruse Bethesda, Maryland Jean Cicero, ART, CTR Health Data Systems Professional Services Riverdale, Maryland Pat Kenny Medical Illustrator for Division of Research Services National Institutes of Health CONTENTS BOOK 4: HUMAN ANATOMY AS RELATED TO TUMOR FORMATION Page Section A--Objectives and Content of Book 4 ............................... 1 Section B--Terms Used to Indicate Body Location and Position .................. 5 Section C--The Integumentary System ..................................... 19 Section D--The Lymphatic System ....................................... 51 Section E--The Cardiovascular System ..................................... 97 Section F--The Respiratory System ....................................... 129 Section G--The Digestive System ......................................... 163 Section -
Digestive Tract
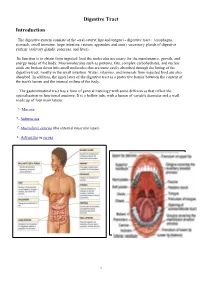
Digestive Tract Introduction The digestive system consists of the -oral cavity( lips and tongue) - digestive tract : (esophagus, stomach, small intestine, large intestine, rectum, appendex and anus) -accessory glands of digestive system: (salivary glands, pancreas, and liver). Its function is to obtain from ingested food the molecules necessary for the maintenance, growth, and energy needs of the body. Macromolecules such as proteins, fats, complex carbohydrates, and nucleic acids are broken down into small molecules that are more easily absorbed through the lining of the digestive tract, mostly in the small intestine. Water, vitamins, and minerals from ingested food are also absorbed. In addition, the inner layer of the digestive tract is a protective barrier between the content of the tract's lumen and the internal milieu of the body. The gastrointestinal tract has a form of general histology with some differences that reflect the specialization in functional anatomy. It is a hollow tube with a lumen of variable diameter and a wall made up of four main layers: 1- Mucosa 2- Submucosa 3- Muscularis externa (the external muscular layer) 4- Adventitia or serosa 1 Mucosa The mucosa is the innermost layer of the gastrointestinal tract that is surrounding the lumen, or open space within the tube. This layer comes in direct contact with digested food . The mucosa is made up of three layers: A- Epithelium - innermost layer. Responsible for most digestive, absorptive and secretory processes. B- Lamina propria - a thin layer of connective tissue . C- Muscularis mucosae - is a thin layer of smooth muscle that supports the mucosa and provides it with the ability to move and fold. -

The Impact of Reporting Practices on State and Local Lip Cancer Rates, Or: How Many Per Million Depends on the Vermilion
The impact of reporting practices on state and local lip cancer rates, or: How many per million depends on the vermilion Francis P. Boscoe, Ph.D. Christopher J. Johnson, MPH New York State Cancer Registry Cancer Data Registry of Idaho July 7, 2015 July 7, 2015 Lipupper parts 2 Skin of upper lip, upper lip Upper lip vermillion, upper lip, upper lipstick area Philtrum Upper lip NOS Oral commissure Lower lip NOS Lower lip vermillion, lower lip, lower lipstick area Mentolabial sulcus Skin of lower lip, lower lip Vermillion border July 7, 2015 3 In the U.S., oral cancer and pharynx incidence ranges from 7.8 per 100,000 (Utah) to 13.5 (Kentucky) – less than a two- fold difference Lip cancer incidence ranges from 0.3 (Ohio) to 2.7 (Idaho) – a nine-fold difference Source: CINA+ 2007-2011 July 7, 2015 4 In Canada, oral cancer and pharynx incidence ranges from 8.9 per 100,000 (Saskatchewan) to 15.9 (Northwest Territories) – less than a two-fold difference Lip cancer incidence ranges from 0.25 (New Brunswick) to 3.0 (Manitoba) – a 12-fold difference Source: CINA+ 2007-2011 July 7, 2015 5 July 7, 2015 6 Utah Idaho Iowa Oral Cavity 7.9 (1) 12.6 (40) 11.7 (26) and Pharynx Oral Cavity 6.0 (1) 9.6 (50) 8.0 (29) Oral Cavity 5.3 (1) 7.1 (26) 6.7 (11) excluding lip Lip 0.7 (25) 2.5 (50) 1.3 (45) Rates (age-adjusted per 100,000) and state ranks (1=lowest rate), 2007-2011, white non-Hispanics July 7, 2015 7 There could actually be two problems: • True skin cancers reported as lip cancers (which inflates lip cancer rates) • True lip cancers being counted as skin cancers and not being reported at all (which deflates lip cancer rates) July 7, 2015 8 True skin cancers reported as lip cancers: NYSCR reviewed all lip cancers in NYS from 1995 to present containing the word “skin”, “basal”, or “BCC” anywhere in the text fields. -

Hairy Leukoplakia James E
Marquette University e-Publications@Marquette School of Dentistry Faculty Research and Dentistry, School of Publications 5-5-2017 Hairy Leukoplakia James E. Cade Meharry Medical College School of Dentistry Richard P. Vinson Paul L Foster School of Medicine Jeff urB gess University of Washington School of Dental Medicine Sanjiv S. Agarwala Temple University Shool of Medicine Denis P. Lynch Marquette University, [email protected] See next page for additional authors Published version. Medscape Drugs & Diseases (May 5, 2017). Publisher link. © 2017 by WebMD LLC. Used with permission. Authors James E. Cade, Richard P. Vinson, Jeff urB gess, Sanjiv S. Agarwala, Denis P. Lynch, and Gary L. Stafford This blog post/website is available at e-Publications@Marquette: https://epublications.marquette.edu/dentistry_fac/252 Overview Background Oral hairy leukoplakia (OHL) is a disease of the mucosa first described in 1984. This pathology is associated with Epstein-Barr virus (EBV) and occurs mostly in people with HIV infection, both immunocompromised and immunocompetent, and can affect patients who are HIV negative.{ref1}{ref2} The first case in an HIV-negative patient was reported in 1999 in a 56-year-old patient with acute lymphocytic leukemia. Later, many cases were reported in heart, kidney, and bone marrow transplant recipients and patients with hematological malignancies.{ref3}{ref4} Pathophysiology The Epstein-Barr virus (EBV), a ubiquitous herpesvirus estimated to infect 90% of the world's population, is linked to a growing number of diseases, especially in immunocompromised hosts. Like all herpesviruses, EBV establishes a life-long, persistent infection of its host. The pathogenesis of hairy leukoplakia is clearly complex, potentially requiring a convergence of factors including EBV co-infection, productive EBV replication, EBV genetic evolution, expression of specific EBV "latent" genes, and immune escape. -
On the Tip of the Tongue
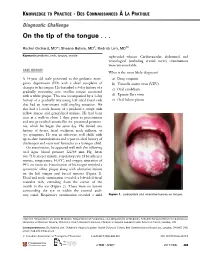
KNOWLEDGE TO PRACTICE DES CONNAISSANCES ÀLA PRATIQUE Diagnostic Challenge On the tip of the tongue . Rachel Orchard, MD*; Sheena Belisle, MD†; Rodrick Lim, MD†‡ Keywords: pediatric, rash, tongue, vesicle right-sided wheeze. Cardiovascular, abdominal, and neurological (including cranial nerve) examinations were unremarkable. CASE HISTORY What is the most likely diagnosis? A 14-year-old male presented to the pediatric emer- a) Drug eruption gency department (ED) with a chief complaint of b) Varicella zoster virus (VZV) changes to his tongue. He described a 3-day history of a c) Oral candidiasis gradually worsening sore, swollen tongue associated with a white plaque. This was accompanied by a 3-day d) Epstein-Barr virus history of a gradually worsening left-sided facial rash e) Oral lichen planus that had an intermittent mild tingling sensation. He also had a 1-week history of a productive cough with yellow mucus and generalized malaise. He had been seen at a walk-in clinic 2 days prior to presentation and was prescribed amoxicillin for presumed pneumo- nia, which he began the same day. He denied any history of fevers, facial weakness, neck stiffness, or eye symptoms. He was an otherwise well child, with up-to-date immunizations and a past medical history of chickenpox and recurrent furuncles as a younger child. On examination, he appeared well with the following vital signs: blood pressure 122/64 mm Hg, heart rate 73 beats per minute, respiratory rate 18 breaths per minute, temperature 36.8°C, and oxygen saturation of 99% on room air. Examination of his tongue revealed a symmetric white plaque along with ulcerative lesions on the left tongue and buccal mucosa (Figure 1). -

Oral Leukoplakia
Division of Oral Medicine and Dentistry Oral Leukoplakia What is oral leukoplakia? What causes oral leukoplakia? Oral leukoplakia (leuko=white, plakia=patch) is a white patch in Alcohol and tobacco use, both known risk factors for the mouth that cannot be rubbed of and cannot be diagnosed oral cancer, are similarly well-established risk factors for as any other condition. Lichen planus, yeast infections development of oral leukoplakia. Other risk factors include a (“thrush”), chronic cheek and tongue chewing injuries, and weakened immune system, long-term treatment with immune hairy/coated tongue are some of the specifc conditions suppressing medications, a personal or family history of cancer, that appear white in the mouth and are therefore NOT oral and, in some cultures, the chewing of areca nut and betel leaf. In leukoplakia. When all such known conditions have been ruled many patients with oral leukoplakia, however, there are no risk out, a patient is diagnosed with oral leukoplakia. While the factors and we don’t know why it develops. long-term history of these lesions is impossible to predict, it How do we know it is oral leukoplakia? is known that true leukoplakias are considered “potentially malignant,” meaning that they have the potential, over time, to If your doctor suspects that a white lesion in your mouth is due develop into oral cancer. to irritation, the source of the irritation will be removed and you will be asked to return in a few weeks for re-evaluation. If the Oral leukoplakia occurs in 1-2% of the population and is most white area is still present at the next visit, a biopsy will likely be common in patients over age 40. -

Clinical Features and Histological Description of Tongue Lesions in a Large Northern Italian Population
Med Oral Patol Oral Cir Bucal. 2015 Sep 1;20 (5):e560-5. Retrospective study on tongue lesions Journal section: Oral Medicine and Pathology doi:10.4317/medoral.20556 Publication Types: Research http://dx.doi.org/doi:10.4317/medoral.20556 Clinical features and histological description of tongue lesions in a large Northern Italian population Alessio Gambino 1, Mario Carbone 1, Paolo-Giacomo Arduino 1, Marco Carrozzo 2, Davide Conrotto 1, Carlotta Tanteri 1, Lucio Carbone 3, Alessandra Elia 1, Zaira Maragon 3, Roberto Broccoletti 1 1 Department of Surgical Sciences, Oral Medicine Section, CIR - Dental School, University of Turin, Turin, Italy 2 Oral Medicine Department, Centre for Oral Health Research, Newcastle University, Newcastle upon Tyne, UK 3 Private practice, Turin Correspondence: Oral Medicine Section University of Turin CIR – Dental School Gambino A, Carbone M, Arduino PG, Carrozzo M, Conrotto D, Tanteri Via Nizza 230, 10126 C, Carbone L, Elia A, Maragon Z, Broccoletti R. Clinical features and Turin, Italy histological description of tongue lesions in a lar�������������������������ge Northern Italian popu- [email protected] lation. Med Oral Patol Oral Cir Bucal. 2015 Sep 1;20 (5):e560-5. http://www.medicinaoral.com/medoralfree01/v20i5/medoralv20i5p560.pdf Article Number: 20556 http://www.medicinaoral.com/ Received: 21/12/2014 © Medicina Oral S. L. C.I.F. B 96689336 - pISSN 1698-4447 - eISSN: 1698-6946 Accepted: 25/04/2015 eMail: [email protected] Indexed in: Science Citation Index Expanded Journal Citation Reports Index Medicus, MEDLINE, PubMed Scopus, Embase and Emcare Indice Médico Español Abstract Background: Only few studies on tongue lesions considered sizable populations, and contemporary literature does not provide a valid report regarding the epidemiology of tongue lesions within the Italian population. -

Cheilitis Glandularis Apostematosa in a Female Patient – a Case Report
CASE REPORTS Serbian Journal of Dermatology and Venereology 2013; 5 (4): 177-182 DOI: 10.2478/sjdv-2013-0015 Cheilitis Glandularis Apostematosa in a Female Patient – a Case Report Mirjana PARAVINA* Faculty of Medicine, University of Niš, Serbia *Correspondence: Mirjana Paravina, E-mail: [email protected] OPEN UDC 616.317-002-092-08 Abstract Cheilitis is an infl ammatory condition of the vermilion border of the lips, which is the junction between the skin and the mucosa. Cheilitis may arise as a primary disorder of the vermilion zone; the infl ammation may extend from the nearby skin, or less often from the oral mucosa. Primary cheilitis lesions are either superfi cial or deep. Deep types include cheilitis glandularis (infl ammatory changes and lip gland swelling), and granulomatous cheilitis (chronic swelling of the lip due to granulomatous infl ammation mostly of unknown origin). Cheilitis glandularis is a rare condition that mostly affects the lower lip and it is characterized by nodular enlargement, reduced mobility and lip erosion. Based on clinical presentation, cheilitis glandularis may be classifi ed into three subtypes: simplex (described as Puente and Acevedo), superfi cial suppurative (described by Baelz-Unna), and the most severe type – deep suppurative, also known as cheilitis glandularis apostematosa (Volkmann’s cheilitis) characterized by deep-seated infl ammation forming abscesses and fi stulous tracts. This is a case report of a female patient with a deep suppurative type of cheilitis affecting both lips. Treatment with systemic antibiotics (using antibiogram tests), corticosteroids and topical therapy resulted in signifi cant improvement. Key words Cheilitis + diagnosis + etiology + classifi cation + therapy; Disease Progression; Prognosis; Treatment Outcome heilitis is an infl ammatory condition of the the lower lip with clinical manifestations of nodular Cvermilion border of the lips, which is the enlargement, reduced mobility and lip inversion (5). -

Head and Neck Pathology (1317-1386)
LABORATORY INVESTIGATION THE BASIC AND TRANSLATIONAL PATHOLOGY RESEARCH JOURNAL LI VOLUME 98 | SUPPLEMENT 1 | MARCH 2018 2018 ABSTRACTS HEAD AND NECK PATHOLOGY (1317-1386) 107TH ANNUAL MEETING GEARED TO LEARN Vancouver Convention Centre MARCH 17-23, 2018 Vancouver, BC, Canada PLATFORM & 2018 ABSTRACTS POSTER PRESENTATIONS EDUCATION COMMITTEE Jason L. Hornick, Chair Amy Chadburn Rhonda Yantiss, Chair, Abstract Review Board Ashley M. Cimino-Mathews and Assignment Committee James R. Cook Laura W. Lamps, Chair, CME Subcommittee Carol F. Farver Steven D. Billings, Chair, Interactive Microscopy Meera R. Hameed Shree G. Sharma, Chair, Informatics Subcommittee Michelle S. Hirsch Raja R. Seethala, Short Course Coordinator Anna Marie Mulligan Ilan Weinreb, Chair, Subcommittee for Rish Pai Unique Live Course Offerings Vinita Parkash David B. Kaminsky, Executive Vice President Anil Parwani (Ex-Officio) Deepa Patil Aleodor (Doru) Andea Lakshmi Priya Kunju Zubair Baloch John D. Reith Olca Basturk Raja R. Seethala Gregory R. Bean, Pathologist-in-Training Kwun Wah Wen, Pathologist-in-Training Daniel J. Brat ABSTRACT REVIEW BOARD Narasimhan Agaram Mamta Gupta David Meredith Souzan Sanati Christina Arnold Omar Habeeb Dylan Miller Sandro Santagata Dan Berney Marc Halushka Roberto Miranda Anjali Saqi Ritu Bhalla Krisztina Hanley Elizabeth Morgan Frank Schneider Parul Bhargava Douglas Hartman Juan-Miguel Mosquera Michael Seidman Justin Bishop Yael Heher Atis Muehlenbachs Shree Sharma Jennifer Black Walter Henricks Raouf Nakhleh Jeanne Shen Thomas Brenn John -

RRP Medical Reference Service
RRP Medical Reference Service An RRP Foundation Publication edited by Dave Wunrow and Bill Stern Fall 2001 ___________________ Volume 8 • Number 2 Preface The RRP Medical Reference Service is intended to be of potential interest to RRP patients/families seeking treatment, practitioners providing care, molecular biological researchers as well as others interested in developing a comprehensive understanding of recurrent respiratory papillomatosis. This issue focuses on a selection of references with abstracts from recent (2000 and later) RRP related publications.These listings are sorted in approximate reverse chronological order as indicated by the "Unique Identifier" numbers. Each listing is formatted as follows: Journal or reference Title Language (if it is not specified assume article is in English) Author(s) Primary affiliation (when specified) Abstract Unique identifier If copies of complete articles are desired, we suggest that you request a reprint from one of the authors. If you need assistance in this regard or if you have any other questions or comments please feel free to contact: Bill Stern RRP Foundation P.O. Box 6643 Lawrenceville NJ 08648-0643 (609) 530-1443 or (609)452-6545 E-mail: [email protected] Dave Wunrow 210 Columbus Drive Marshfield WI 54449 (715) 387-8824 E-mail: [email protected] RRPF Selected Articles and Abstracts ( Accepted for publication in Arch Otolaryngol Head Neck Surg ) Can Mumps Vaccine Induce Remission in Recurrent Respiratory Papilloma? N.R.T. Pashley Presbyterian/St. Lukes Hospital, Denver, Colorado Study Objective: To describe our experience using laser excision and locally injected mumps vaccine to induce remission in patients with recurrent respiratory papilloma (RRP).