Management of Iatrogenic Displacement of Maxillary Third Molar Into Pterygomandibular Space: Case Report
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Accidental Displacement of Mandibular Third Molar Root Into the Submandibular Space: a Case Report
Case Report ERA’S JOURNAL OF MEDICAL RESEARCH VOL.6 NO.1 ACCIDENTAL DISPLACEMENT OF MANDIBULAR THIRD MOLAR ROOT INTO THE SUBMANDIBULAR SPACE: A CASE REPORT Mayur Vilas Limbhore, Viren S Patil, Shandilya Ramanojam, Vrushika Mahajan, Pallavi Rathi, Kisna Tadas Department of Oral and Maxillofacial surgery Bharati Vidyapeeth Dental College, Katraj, Pune, Maharashtra, India-411030 Received on : 01-04-2018 Accpected on : 10-04-2018 ABSTRACT Address for correspondence Accidental displacement of an impacted third molar, either a crown, Dr. Mayur Vilas Limbhore root piece, or the entire tooth, is a rare complication that occurs Department of Oral and Maxillofacial Surgery during surgical removal. The most common sites of dislodgment of an impacted mandibular third molar root are the submandibular, Bharati Vidyapeth Dental College, sublingual and pterygomandibular spaces. Removal of a displaced Katraj, Pune, Maharashtra, India-411030 root from these spaces may be complex due to poor visualization Email: [email protected] and limited access. A thorough evaluation of all significant risk Contact no: +91-8552887325 factors must be performed in advance to prevent complications. This case report reveals the management of accidental displaced mandibular third molar root into the submandibular space. An 39 years-old male patient underwent a third mandibular molar extraction. Accidentally, the mandibular right third molar distal root was displaced into the submandibular space, making necessary a second surgical step. After 2 days awaiting an asymptomatic health status, the second surgical step was successfully performed using multislice CBCT as preoperative imaging guide. The present case report highlights the clinical usefulness of CBCT in proper treatment of the patient. -

CASE REPORT Fibromatosis of Infratemporal Space Riaz Ahmed Warraich, Tooba Saeed, Nabila Riaz, Asma Aftab
217 CASE REPORT Fibromatosis of infratemporal space Riaz Ahmed Warraich, Tooba Saeed, Nabila Riaz, Asma Aftab Abstract chemotherapy or non-cytotoxic drugs are also Fibromatosis is a rare benign mesenchymal neoplasm considerable modalities for AF management, to avoid which primarily originates in the muscle, connective sacrifising functional integrity as a price of attaining tissue, fascial sheaths, and musculoaponeurotic tumour-free margins. 3 structures. It is commonly seen as abdominal tumour but Case Report in maxillofacial region, the occurrence of these tumours is very rare and exceedingly rare in infratemporal space. A 35-year-old female visited Oral and Maxillofacial Often misdiagnosed due to its varied clinical behaviour, Department of Mayo Hospital on October 5, 2014. Written fibromatosis is benign, slow-growing, infiltrative tumour informed consent was obtained from the patient for without any metastatic potential, but is locally aggressive publication of this report and accompanying images. Her causing organ dysfunction along with high recurrence chief complaint was of progressive reduction in mouth rate. We report a case of fibromatosis involving the left opening gradually for the preceding 4 years. Medical infratemporal space in a 35-year-old female who history revealed that she had extra pulmonary presented with chief complaint of limited mouth opening tuberculous lesion in left side of her neck which was for the preceding 4 years. treated 10 years earlier. Clinical examination revealed slight thickening and fibrosis of left cheek with zero Keywords: Aggressive fibromatosis, Infratemporal, mouth opening. Overlying skin was normal. There was no Benign, Infiltrative. Introduction Aggressive fibromatosis (AF) or extra-abdominal desmoid tumours are rare tumours of fibroblastic origin involving the proliferation of cytologically benign fibrocytes. -
Anatomical Overview
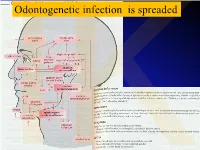
IKOdontogenetic infection is spreaded Možné projevy zlomenin a zánětů IKPossible signs of fractures or inflammations Submandibular space lies between the bellies of the digastric muscles, mandible, mylohyoid muscle and hyoglossus and styloglossus muscles IK IK IK IK IK Submandibulární absces Submandibular abscess IK Sběhlý submandibulární absces Submandibular abscess is getting down IK Submental space lies between the mylohyoid muscles and the investing layer of deep cervical fascia superficially IK IK Spatium peritonsillare IK IK Absces v peritonsilární krajině Abscess in peritonsilar region IK Fasciae Neck fasciae cervicales Demarcate spaces • fasciae – Superficial (investing): • f. nuchae, f. pectoralis, f. deltoidea • invests m. sternocleidomastoideus + trapezius • f. supra/infrahyoidea – pretrachealis (middle neck f.) • form Δ, invests infrahyoid mm. • vagina carotica (carotic sheet) – Prevertebral (deep cervical f.) • Covers scaleni mm. IK• Alar fascia Fascie Fascia cervicalis superficialis cervicales Fascia cervicalis media Fascia cervicalis profunda prevertebralis IKsuperficialis pretrachealis Neck spaces - extent • paravisceral space – Continuation of parafaryngeal space – Nervous and vascular neck bundle • retrovisceral space – Between oesophagus and prevertebral f. – Previsceral space – mezi l. pretrachealis a orgány – v. thyroidea inf./plx. thyroideus impar • Suprasternal space – Between spf. F. and pretracheal one IK– arcus venosus juguli 1 – sp. suprasternale suprasternal Spatia colli 2 – sp. pretracheale pretracheal 3 – -

Retained Surgical Items Evidence Table
Guideline for Prevention of Retained Surgical Items Evidence Table CITATION CONCLUSION(S) SAMPLE SIZE REFERENCE # POPULATION COMPARISON EVIDENCE TYPE INTERVENTIONS CONSENSUS SCORE OUTCOME MEASURE 1 Wilson C. Foreign bodies left in the Case series of foreign bodies left in the abdomen. Cases VC Literature n/a n/a n/a n/a Retained abdomen after laparotomy. Trans Am found through publication, interviews, and the author's own Review, Clinician sponges Gynecol Soc. 1884;9:94-117. experience. Experience, and Case Report 2 The Joint Commission. Preventing The Joint Commission recommends that facilities develop IVB Consensus n/a n/a n/a n/a n/a unintended retained foreign objects. effective processes and procedures for preventing Sentinel Event Alert. October 17, unintended retained foreign objects. Their recommendations 2013;51. include a standardized and highly reliable counting system; http://www.jointcommission.org/sea_i development of policies and procedures; practices for ssue_51/. Accessed November 10, counting, wound opening, and closing procedures; 2015. performance of intraoperative radiographs; use of effective communication to include briefings and debriefings; documentation of counts; and assistive technologies (ie, RF tags, RFID, radiopaque, bar coding). Also, the hospital should define a process for conducting RCA for sentinel events, such as URFO. Page 1 of 60 Guideline for Prevention of Retained Surgical Items Evidence Table CITATION CONCLUSION(S) SAMPLE SIZE REFERENCE # POPULATION COMPARISON EVIDENCE TYPE INTERVENTIONS CONSENSUS SCORE OUTCOME MEASURE 3 Moffatt-Bruce SD, Cook CH, Steinberg 7 elevated risk factors for RSI in pooled data in case-control IIIA Systematic USA hospitals, n/a n/a 3 studies: Estimated SM, Stawicki SP. -

Anatomy of the Pterygomandibular Space — Clinical Implication and Review
FOLIA MEDICA CRACOVIENSIA 79 Vol. LIII, 1, 2013: 79–85 PL ISSN 0015-5616 MARCIN LIPSKI1, WERONIKA LIPSKA2, SYLWIA MOTYL3, Tomasz Gładysz4, TOMASZ ISKRA1 ANATOMY OF THE PTERYGOMANDIBULAR SPACE — CLINICAL IMPLICATION AND REVIEW Abstract: A i m: The aim of this study was to present review of the pterygomandibular space with some referrals to clinical practice, specially to the methods of lower teeth anesthesia. C o n c l u s i o n s: Pterygomandibular space is a clinically important region which is commonly missing in anatomical textbooks. More attention should be paid to it both from theoretical and practical point of view, especially in teaching the students of first year of dental studies. Key words: pterygomandibular space, Gow-Gates anesthesia, inferior alveolar nerve. INTRODUCTION Numerous cranial regions have been subjects of various anatomical and anthro- pological studies [1, 2]. Most of them indicate necessity of undertaking of such studies first of all because of clinical importance [3–5]. Inferior alveolar nerve blocs, one of the most common procedures in dentistry requires deep anatomical knowledge of the pterygomandibular space [6, 7]. This space is a narrow gap, which contains mostly loose areolar tissue. It communi- cates however through the mandibular foramen with the mandibular canal, which is traversed by inferior alveolar nerve, artery and comitant vein (IANAV). Many of the structures placed in this space are of certain importance for local anesthesia. Khoury at al. [8, 9] mention here the following: inferior alveolar nerve, artery and vein, lingual nerve, nerve to mylohyoid and the sphenomandibular ligament. The space contains mostly loose areolar tissue. -

Diapositiva 1
Ingegneria delle tecnologie per la salute Fondamenti di anatomia e istologia Lezione 4.a.b.c aa. 2018-19 Ingegneria delle tecnologie per la salute Fondamenti di anatomia e istologia aa. 2018-179 Sistema locomotore • Ossa 4.a • Articolazioni 4.b • Muscoli 4.c BONES 4.a BONE TISSUE & SKELETAL SYSTEM After this lesson, you will be able to: • List and describe the functions of bones • Describe the classes of bones • Discuss the process of bone formation and development Functions of the Skeletal System Bone (osseous tissue) = hard, dense connective tissue that forms most of the adult skeleton, the support structure of the body. Cartilage = a semi-rigid form of connective tissue, in the areas of the skeleton where bones move provides flexibility and smooth surfaces for movement. Skeletal system = body system composed of bones and cartilage and performing following functions: • supports the body • facilitates movement • protects internal organs • produces blood cells • stores and releases minerals and fat Bone Classification 206 bones composing skeleton, divided into 5 categories based on their shapes ( distinct function) Bone Classification Bone Structure Bone tissue differs greatly from other tissues in the body: is hard (many of its functions depend on this hardness) and also dynamic (its shape adjusts to accommodate stresses). histology gross anatomy Gross Anatomy of Bone structure of a LONG BONE, 2 parts: 1. diaphysis: tubular shaft that runs between the proximal and distal ends of the bone, where the hollow region is called medullary cavity (filled with yellow marrow) and the walls are composed of dense and hard compact bone 2. -

Infratemporal Abscess in an Adolescent Following a Dental Procedure
Central Annals of Pediatrics & Child Health Research Article *Corresponding author Vijay CS, Department of Pediatrics, West Virginia University, Medical Center Dr, Morgantown, USA, Tel: 304-293-6307; Fax: 304-293-1216; Email: Infratemporal Abscess in an Submitted: 30 November 2018 Adolescent Following a Dental Accepted: 02 January 2019 Published: 04 January 2019 ISSN: 2373-9312 Procedure Copyright © 2019 Vijay et al. Vijay CS* and Chen CB OPEN ACCESS Department of Pediatrics, West Virginia University, USA Keywords • Abscess Abstract • Infratemporal fossa Infections in the infratemporal region can be a major source of morbidity and have • Odontogenic infections been known to occur after dental procedures. Neurovascular structures running through the infratemporal fossa serve as a source for infections to track to different areas of the head and neck. The proximity of the infratemporal fossa to other major structures makes timely diagnosis critical. Infratemporal fossa abscesses are a rare complication and only a few cases have been described in the literature. As the clinical symptoms may be non-specific, the diagnosis may be challenging for healthcare providers. We describe a patient who presented with facial swelling and trismus following wisdom tooth extraction who was found to have an infratemporal fossa abscess. ABBREVIATIONS CASE PRESENTATION CT: Computed Tomography; MRI: Magnetic Resonance A 14-year-old previously healthy male presented with Imaging left-sided facial swelling and jaw stiffness. He complained of associated tenderness to palpation over the left side of his face INTRODUCTION The infratemporal fossa is an extremely important site, as it initially started three days after he had four wisdom teeth communicates with several surrounding structures including the extracted.and jaw and As his difficulty symptoms opening did not his resolve, mouth. -

Refractory Odontogenic Infection Associated to Candida Albicans: a Case Report
Case Report Clinics in Surgery Published: 31 Mar, 2017 Refractory Odontogenic Infection Associated to Candida Albicans: A Case Report Daya A Mikhail*, Mederos Heidi BS and McClure Shawn Department of Oral and Maxillofacial Surgery, Nova Southeastern University /Broward Health Medical Center, USA Abstract Background: Multifascial space infections from an odontogenic origin have been attributed to a different number of microorganisms. These infections can be serious, involving multiple deep spaces in the head and neck, and potentially compromising the airway. Fungal etiology including C. albicans has been reported in the past as a rare agent involving multifascial space infections. Case Description: We present an unusual case of a severe deep space infection associated with carious teeth numbers 31 and 32. This specific infection proved to be resistant to multiple antibiotic therapy and required incision and drainage on two different occasions. After the initial surgery, the patient remained febrile with an elevated white blood cell count; thus, the patient was taken to the operating room again for a re-drainage and new cultures. Cultures obtained during the second surgery were positive for C. albicans. The patient was responsive to antifungal therapy, showing quick improvement in his condition. Conclusion: Although multiple factors could have contributed to this patient’s vulnerability to odontogenic infection of fungal etiology including history of alcoholism and broad spectrum antibiotic therapy, it remains an infrequent finding in the literature. This case illustrates the need to consider a fungal cause in patients with odontogenic infections who are not responsive to broad spectrum antibiotics and surgical drainage. Keywords: Odontogenic infection; Candida albicans; Microorganisms Introduction OPEN ACCESS Many microorganisms have been identified in multifascial space infections of the head and *Correspondence: neck region. -

Anatomy of the Pterygomandibular Space — Clinical Implication and Review
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Jagiellonian Univeristy Repository FOLIA MEDICA CRACOVIENSIA 79 Vol. LIII, 1, 2013: 79–85 PL ISSN 0015-5616 MARCIN LIPSKI1, WERONIKA LIPSKA2, SYLWIA MOTYL3, Tomasz Gładysz4, TOMASZ ISKRA1 ANATOMY OF THE PTERYGOMANDIBULAR SPACE — CLINICAL IMPLICATION AND REVIEW Abstract: A i m: The aim of this study was to present review of the pterygomandibular space with some referrals to clinical practice, specially to the methods of lower teeth anesthesia. C o n c l u s i o n s: Pterygomandibular space is a clinically important region which is commonly missing in anatomical textbooks. More attention should be paid to it both from theoretical and practical point of view, especially in teaching the students of first year of dental studies. Key words: pterygomandibular space, Gow-Gates anesthesia, inferior alveolar nerve. INTRODUCTION Numerous cranial regions have been subjects of various anatomical and anthro- pological studies [1, 2]. Most of them indicate necessity of undertaking of such studies first of all because of clinical importance [3–5]. Inferior alveolar nerve blocs, one of the most common procedures in dentistry requires deep anatomical knowledge of the pterygomandibular space [6, 7]. This space is a narrow gap, which contains mostly loose areolar tissue. It communi- cates however through the mandibular foramen with the mandibular canal, which is traversed by inferior alveolar nerve, artery and comitant vein (IANAV). Many of the structures placed in this space are of certain importance for local anesthesia. Khoury at al. [8, 9] mention here the following: inferior alveolar nerve, artery and vein, lingual nerve, nerve to mylohyoid and the sphenomandibular ligament. -

ODONTOGENTIC INFECTIONS Infection Spread Determinants
ODONTOGENTIC INFECTIONS The Host The Organism The Environment In a state of homeostasis, there is Peter A. Vellis, D.D.S. a balance between the three. PROGRESSION OF ODONTOGENIC Infection Spread Determinants INFECTIONS • Location, location , location 1. Source 2. Bone density 3. Muscle attachment 4. Fascial planes “The Path of Least Resistance” Odontogentic Infections Progression of Odontogenic Infections • Common occurrences • Periapical due primarily to caries • Periodontal and periodontal • Soft tissue involvement disease. – Determined by perforation of the cortical bone in relation to the muscle attachments • Odontogentic infections • Cellulitis‐ acute, painful, diffuse borders can extend to potential • fascial spaces. Abscess‐ chronic, localized pain, fluctuant, well circumscribed. INFECTIONS Severity of the Infection Classic signs and symptoms: • Dolor- Pain Complete Tumor- Swelling History Calor- Warmth – Chief Complaint Rubor- Redness – Onset Loss of function – Duration Trismus – Symptoms Difficulty in breathing, swallowing, chewing Severity of the Infection Physical Examination • Vital Signs • How the patient – Temperature‐ feels‐ Malaise systemic involvement >101 F • Previous treatment – Blood Pressure‐ mild • Self treatment elevation • Past Medical – Pulse‐ >100 History – Increased Respiratory • Review of Systems Rate‐ normal 14‐16 – Lymphadenopathy Fascial Planes/Spaces Fascial Planes/Spaces • Potential spaces for • Primary spaces infectious spread – Canine between loose – Buccal connective tissue – Submandibular – Submental -
A Dictionary of Neurological Signs
FM.qxd 9/28/05 11:10 PM Page i A DICTIONARY OF NEUROLOGICAL SIGNS SECOND EDITION FM.qxd 9/28/05 11:10 PM Page iii A DICTIONARY OF NEUROLOGICAL SIGNS SECOND EDITION A.J. LARNER MA, MD, MRCP(UK), DHMSA Consultant Neurologist Walton Centre for Neurology and Neurosurgery, Liverpool Honorary Lecturer in Neuroscience, University of Liverpool Society of Apothecaries’ Honorary Lecturer in the History of Medicine, University of Liverpool Liverpool, U.K. FM.qxd 9/28/05 11:10 PM Page iv A.J. Larner, MA, MD, MRCP(UK), DHMSA Walton Centre for Neurology and Neurosurgery Liverpool, UK Library of Congress Control Number: 2005927413 ISBN-10: 0-387-26214-8 ISBN-13: 978-0387-26214-7 Printed on acid-free paper. © 2006, 2001 Springer Science+Business Media, Inc. All rights reserved. This work may not be translated or copied in whole or in part without the written permission of the publisher (Springer Science+Business Media, Inc., 233 Spring Street, New York, NY 10013, USA), except for brief excerpts in connection with reviews or scholarly analysis. Use in connection with any form of information storage and retrieval, electronic adaptation, computer software, or by similar or dis- similar methodology now known or hereafter developed is forbidden. The use in this publication of trade names, trademarks, service marks, and similar terms, even if they are not identified as such, is not to be taken as an expression of opinion as to whether or not they are subject to propri- etary rights. While the advice and information in this book are believed to be true and accurate at the date of going to press, neither the authors nor the editors nor the publisher can accept any legal responsibility for any errors or omis- sions that may be made. -

Treatment for Acute Pain: an Evidence Map Technical Brief Number 33
Technical Brief Number 33 R Treatment for Acute Pain: An Evidence Map Technical Brief Number 33 Treatment for Acute Pain: An Evidence Map Prepared for: Agency for Healthcare Research and Quality U.S. Department of Health and Human Services 5600 Fishers Lane Rockville, MD 20857 www.ahrq.gov Contract No. 290-2015-0000-81 Prepared by: Minnesota Evidence-based Practice Center Minneapolis, MN Investigators: Michelle Brasure, Ph.D., M.S.P.H., M.L.I.S. Victoria A. Nelson, M.Sc. Shellina Scheiner, PharmD, B.C.G.P. Mary L. Forte, Ph.D., D.C. Mary Butler, Ph.D., M.B.A. Sanket Nagarkar, D.D.S., M.P.H. Jayati Saha, Ph.D. Timothy J. Wilt, M.D., M.P.H. AHRQ Publication No. 19(20)-EHC022-EF October 2019 Key Messages Purpose of review The purpose of this evidence map is to provide a high-level overview of the current guidelines and systematic reviews on pharmacologic and nonpharmacologic treatments for acute pain. We map the evidence for several acute pain conditions including postoperative pain, dental pain, neck pain, back pain, renal colic, acute migraine, and sickle cell crisis. Improved understanding of the interventions studied for each of these acute pain conditions will provide insight on which topics are ready for comprehensive comparative effectiveness review. Key messages • Few systematic reviews provide a comprehensive rigorous assessment of all potential interventions, including nondrug interventions, to treat pain attributable to each acute pain condition. Acute pain conditions that may need a comprehensive systematic review or overview of systematic reviews include postoperative postdischarge pain, acute back pain, acute neck pain, renal colic, and acute migraine.