Systematic Review of the Effect of Intravenous Lipid Emulsion Therapy for Non-Local Anesthetics Toxicity
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

(12) Patent Application Publication (10) Pub. No.: US 2006/0110428A1 De Juan Et Al
US 200601 10428A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2006/0110428A1 de Juan et al. (43) Pub. Date: May 25, 2006 (54) METHODS AND DEVICES FOR THE Publication Classification TREATMENT OF OCULAR CONDITIONS (51) Int. Cl. (76) Inventors: Eugene de Juan, LaCanada, CA (US); A6F 2/00 (2006.01) Signe E. Varner, Los Angeles, CA (52) U.S. Cl. .............................................................. 424/427 (US); Laurie R. Lawin, New Brighton, MN (US) (57) ABSTRACT Correspondence Address: Featured is a method for instilling one or more bioactive SCOTT PRIBNOW agents into ocular tissue within an eye of a patient for the Kagan Binder, PLLC treatment of an ocular condition, the method comprising Suite 200 concurrently using at least two of the following bioactive 221 Main Street North agent delivery methods (A)-(C): Stillwater, MN 55082 (US) (A) implanting a Sustained release delivery device com (21) Appl. No.: 11/175,850 prising one or more bioactive agents in a posterior region of the eye so that it delivers the one or more (22) Filed: Jul. 5, 2005 bioactive agents into the vitreous humor of the eye; (B) instilling (e.g., injecting or implanting) one or more Related U.S. Application Data bioactive agents Subretinally; and (60) Provisional application No. 60/585,236, filed on Jul. (C) instilling (e.g., injecting or delivering by ocular ion 2, 2004. Provisional application No. 60/669,701, filed tophoresis) one or more bioactive agents into the Vit on Apr. 8, 2005. reous humor of the eye. Patent Application Publication May 25, 2006 Sheet 1 of 22 US 2006/0110428A1 R 2 2 C.6 Fig. -

2D6 Substrates 2D6 Inhibitors 2D6 Inducers
Physician Guidelines: Drugs Metabolized by Cytochrome P450’s 1 2D6 Substrates Acetaminophen Captopril Dextroamphetamine Fluphenazine Methoxyphenamine Paroxetine Tacrine Ajmaline Carteolol Dextromethorphan Fluvoxamine Metoclopramide Perhexiline Tamoxifen Alprenolol Carvedilol Diazinon Galantamine Metoprolol Perphenazine Tamsulosin Amiflamine Cevimeline Dihydrocodeine Guanoxan Mexiletine Phenacetin Thioridazine Amitriptyline Chloropromazine Diltiazem Haloperidol Mianserin Phenformin Timolol Amphetamine Chlorpheniramine Diprafenone Hydrocodone Minaprine Procainamide Tolterodine Amprenavir Chlorpyrifos Dolasetron Ibogaine Mirtazapine Promethazine Tradodone Aprindine Cinnarizine Donepezil Iloperidone Nefazodone Propafenone Tramadol Aripiprazole Citalopram Doxepin Imipramine Nifedipine Propranolol Trimipramine Atomoxetine Clomipramine Encainide Indoramin Nisoldipine Quanoxan Tropisetron Benztropine Clozapine Ethylmorphine Lidocaine Norcodeine Quetiapine Venlafaxine Bisoprolol Codeine Ezlopitant Loratidine Nortriptyline Ranitidine Verapamil Brofaramine Debrisoquine Flecainide Maprotline olanzapine Remoxipride Zotepine Bufuralol Delavirdine Flunarizine Mequitazine Ondansetron Risperidone Zuclopenthixol Bunitrolol Desipramine Fluoxetine Methadone Oxycodone Sertraline Butylamphetamine Dexfenfluramine Fluperlapine Methamphetamine Parathion Sparteine 2D6 Inhibitors Ajmaline Chlorpromazine Diphenhydramine Indinavir Mibefradil Pimozide Terfenadine Amiodarone Cimetidine Doxorubicin Lasoprazole Moclobemide Quinidine Thioridazine Amitriptyline Cisapride -

Thoroughbred Racing
178CSR1 Title 178 Legislative Rule West Virginia Racing Commission Series 1 Thoroughbred Racing Effective: July 9, 2014 West Virginia Racing Commission 900 Pennsylvania Avenue Suite 533 Charleston WV 25302 305.558.2150 Fax 304.558.6319 Web Site: www.racing.wv.gov 178CSR1 Table of Contents SERIES 1 THOROUGHBRED RACING ____________________________________________________________________ 1 §178-1-1. General. ____________________________________________________________________________________ 1 PART 1. DEFINITIONS. _________________________________________________________________________________ 1 §178-1-2. Definitions. _________________________________________________________________________________ 1 PART 2. GENERAL AUTHORITY. ________________________________________________________________________ 9 §178-1-3. General Authority of the Racing Commission. ______________________________________________________ 9 §178-1-4. Power Of Entry. ______________________________________________________________________________ 9 §178-1-5. Racing Commission personnel. __________________________________________________________________ 9 §178-1-6. Ejection/Exclusion. __________________________________________________________________________ 12 PART 3. RACING OFFICIALS. __________________________________________________________________________ 12 §178-1-7. General Provisions. __________________________________________________________________________ 12 §178-1-8. Stewards. __________________________________________________________________________________ 14 -
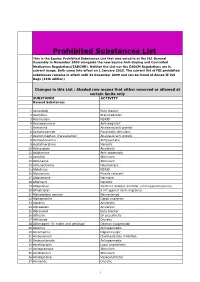
Prohibited Substances List
Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). Neither the List nor the EADCM Regulations are in current usage. Both come into effect on 1 January 2010. The current list of FEI prohibited substances remains in effect until 31 December 2009 and can be found at Annex II Vet Regs (11th edition) Changes in this List : Shaded row means that either removed or allowed at certain limits only SUBSTANCE ACTIVITY Banned Substances 1 Acebutolol Beta blocker 2 Acefylline Bronchodilator 3 Acemetacin NSAID 4 Acenocoumarol Anticoagulant 5 Acetanilid Analgesic/anti-pyretic 6 Acetohexamide Pancreatic stimulant 7 Acetominophen (Paracetamol) Analgesic/anti-pyretic 8 Acetophenazine Antipsychotic 9 Acetylmorphine Narcotic 10 Adinazolam Anxiolytic 11 Adiphenine Anti-spasmodic 12 Adrafinil Stimulant 13 Adrenaline Stimulant 14 Adrenochrome Haemostatic 15 Alclofenac NSAID 16 Alcuronium Muscle relaxant 17 Aldosterone Hormone 18 Alfentanil Narcotic 19 Allopurinol Xanthine oxidase inhibitor (anti-hyperuricaemia) 20 Almotriptan 5 HT agonist (anti-migraine) 21 Alphadolone acetate Neurosteriod 22 Alphaprodine Opiod analgesic 23 Alpidem Anxiolytic 24 Alprazolam Anxiolytic 25 Alprenolol Beta blocker 26 Althesin IV anaesthetic 27 Althiazide Diuretic 28 Altrenogest (in males and gelidngs) Oestrus suppression 29 Alverine Antispasmodic 30 Amantadine Dopaminergic 31 Ambenonium Cholinesterase inhibition 32 Ambucetamide Antispasmodic 33 Amethocaine Local anaesthetic 34 Amfepramone Stimulant 35 Amfetaminil Stimulant 36 Amidephrine Vasoconstrictor 37 Amiloride Diuretic 1 Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). -

Kentucky Horse Racing Commission Withdrawal Guidelines Thoroughbred; Standardbred; Quarter Horse, Appaloosa, and Arabian KHRC 8-020-2 (11/2018)
Kentucky Horse Racing Commission Withdrawal Guidelines Thoroughbred; Standardbred; Quarter Horse, Appaloosa, and Arabian KHRC 8-020-2 (11/2018) General Notice Unless otherwise specified in these withdrawal guidelines or the applicable regulations and statutes, the following withdrawal guidelines are voluntary and advisory. The guidelines are recommendations based on current scientific knowledge that may change over time. A licensee may present evidence of full compliance with these guidelines to the Kentucky Horse Racing Commission (the “Commission” or “KHRC”) and the stewards as a mitigating factor to be used in determining violations and penalties. These withdrawal interval guidelines assume that administration of medications will be performed at doses that are not greater than the manufacturer’s maximum recommended dosage. Medications administered at dosages above manufacturer’s recommendations, in compounded formulations and/or in combination with other medications and/or administration inside the withdrawal interval may result in test sample concentrations above threshold concentrations that could lead to positive test results and the imposition of penalties. The time of administration of an orally administered substance, for the purposes of withdrawal interval, shall be considered to be the time of complete ingestion of the medication by the horse via eating or drinking. Brand names of medications, where applicable, are listed in parentheses or brackets following the generic name of a drug. In addition to the requirements contained in KRS Chapter 13A, the KHRC shall give notice of an amendment or addition to these withdrawal guidelines by posting the change on the KHRC website and at all Kentucky racetracks at least two weeks before the amendment or addition takes legal effect. -

Ventricular Tachycardia Drugs Versus Devices John Camm St
Cardiology Update 2015 Davos, Switzerland: 8-12th February 2015 Ventricular Arrhythmias Ventricular Tachycardia Drugs versus Devices John Camm St. George’s University of London, UK Imperial College, London, UK Declaration of Interests Chairman: NICE Guidelines on AF, 2006; ESC Guidelines on Atrial Fibrillation, 2010 and Update, 2012; ACC/AHA/ESC Guidelines on VAs and SCD; 2006; NICE Guidelines on ACS and NSTEMI, 2012; NICE Guidelines on heart failure, 2008; NICE Guidelines on Atrial Fibrillation, 2006; ESC VA and SCD Guidelines, 2015 Steering Committees: multiple trials including novel anticoagulants DSMBs: multiple trials including BEAUTIFUL, SHIFT, SIGNIFY, AVERROES, CASTLE- AF, STAR-AF II, INOVATE, and others Events Committees: one trial of novel oral anticoagulants and multiple trials of miscellaneous agents with CV adverse effects Editorial Role: Editor-in-Chief, EP-Europace and Clinical Cardiology; Editor, European Textbook of Cardiology, European Heart Journal, Electrophysiology of the Heart, and Evidence Based Cardiology Consultant/Advisor/Speaker: Astellas, Astra Zeneca, ChanRX, Gilead, Merck, Menarini, Otsuka, Sanofi, Servier, Xention, Bayer, Boehringer Ingelheim, Bristol- Myers Squibb, Daiichi Sankyo, Pfizer, Boston Scientific, Biotronik, Medtronic, St. Jude Medical, Actelion, GlaxoSmithKline, InfoBionic, Incarda, Johnson and Johnson, Mitsubishi, Novartis, Takeda Therapy for Ventricular Tachycardia Medical therapy Antiarrhythmic drugs Autonomic management Ventricular tachycardia Monomorphic Polymorphic Ventricular fibrillation Ventricular storms Ablation therapy Device therapy Surgical Defibrillation Catheter Antitachycardia pacing History of Antiarrhythmic Drugs 1914 - Quinidine 1950 - Lidocaine 1951 - Procainamide 1946 – Digitalis 1956 – Ajmaline 1962 - Verapamil 1962 – Disopyramide 1964 - Propranolol 1967 – Amiodarone 1965 – Bretylium 1972 – Mexiletine 1973 – Aprindine, Tocainide 1969 - Diltiazem 1975- Flecainide 1976 – Propafenone Encainide Ethmozine 2000 - Sotalol D-sotalol 1995 - Ibutilide (US) Recainam 2000 – Dofetilide US) IndecainideX Etc. -

Drug and Medication Classification Schedule
KENTUCKY HORSE RACING COMMISSION UNIFORM DRUG, MEDICATION, AND SUBSTANCE CLASSIFICATION SCHEDULE KHRC 8-020-1 (11/2018) Class A drugs, medications, and substances are those (1) that have the highest potential to influence performance in the equine athlete, regardless of their approval by the United States Food and Drug Administration, or (2) that lack approval by the United States Food and Drug Administration but have pharmacologic effects similar to certain Class B drugs, medications, or substances that are approved by the United States Food and Drug Administration. Acecarbromal Bolasterone Cimaterol Divalproex Fluanisone Acetophenazine Boldione Citalopram Dixyrazine Fludiazepam Adinazolam Brimondine Cllibucaine Donepezil Flunitrazepam Alcuronium Bromazepam Clobazam Dopamine Fluopromazine Alfentanil Bromfenac Clocapramine Doxacurium Fluoresone Almotriptan Bromisovalum Clomethiazole Doxapram Fluoxetine Alphaprodine Bromocriptine Clomipramine Doxazosin Flupenthixol Alpidem Bromperidol Clonazepam Doxefazepam Flupirtine Alprazolam Brotizolam Clorazepate Doxepin Flurazepam Alprenolol Bufexamac Clormecaine Droperidol Fluspirilene Althesin Bupivacaine Clostebol Duloxetine Flutoprazepam Aminorex Buprenorphine Clothiapine Eletriptan Fluvoxamine Amisulpride Buspirone Clotiazepam Enalapril Formebolone Amitriptyline Bupropion Cloxazolam Enciprazine Fosinopril Amobarbital Butabartital Clozapine Endorphins Furzabol Amoxapine Butacaine Cobratoxin Enkephalins Galantamine Amperozide Butalbital Cocaine Ephedrine Gallamine Amphetamine Butanilicaine Codeine -

Drugs and Medication Guidelines Brochure
Equine Medication Monitoring Program Drugs and Medication Guidelines January 2021 1 Introduction The California Equine Medication Monitoring Program (EMMP) is an industry funded program to ensure the integrity of public equine events and sales in California through the control of performance and disposition enhancing drugs and permitting limited therapeutic use of drugs and medications. The EMMP and the industry is dedicated and committed to promote the health, welfare and safety of the equine athlete. Owners, trainers, exhibitors, veterinarians and consignors of equines to public sales have a responsibility to be familiar with the California EMMP and the California Equine Medication Rule. California law (Food and Agricultural Code Sections 24000-24018) outlines the equine medication rule for public equine events in California. The owner, trainer and consignor have responsibility to ensure full compliance with all elements of the California Equine Medication Rule. Owners, trainers, exhibitors, veterinarians and consignors of equines to public sales must comply with both the California Equine Medication Rule and any sponsoring organization drug and medication rule for an event. The more stringent medication rule applies for the event. The California Equine Medication Rule is posted on the website: http://www.cdfa.ca.gov/ahfss/Animal_Health/emmp/ The information contained in this document provides advice regarding the California Equine Medication Rule and application of the rule to practical situations. The EMMP recognizes that situations arise where there is an indication for legitimate therapeutic treatment near the time of competition at equine events. The EMMP regulations permit the use of therapeutic medication in certain circumstances to accommodate legitimate therapy in compliance with the requirements of the rule. -

Methadone Or Butorphanol As Pre-Anaesthetic Agents Combined with Romifidine in Horses Undergoing Elective Surgery: Qualitative Assessment of Sedation and Induction
animals Article Methadone or Butorphanol as Pre-Anaesthetic Agents Combined with Romifidine in Horses Undergoing Elective Surgery: Qualitative Assessment of Sedation and Induction Sara Nannarone 1,* , Giacomo Giannettoni 2 , Chiara Laurenza 3, Andrea Giontella 1 and Giulia Moretti 1 1 Department of Veterinary Medicine, Perugia University, Via San Costanzo 4, 06126 Perugia, Italy; [email protected] (A.G.); [email protected] (G.M.) 2 ADVETIA Centre Hospitalier Vétérinaire, Vélizy-Villacoublay, Île-de-France, 78140 Paris, France; [email protected] 3 Section of Anesthésiologie, Université de Lyon, VetAgro Sup, Marcy l’Etoile, 69280 Lyon, France; [email protected] * Correspondence: [email protected]; Tel.: +39-075-585-7715 Simple Summary: When considering sedation or general anaesthesia in horses, a multimodal strat- egy is commonly preferred over a single drug. This includes the association of alpha-2 adrenoceptor agonists, phenothiazines or opioids, to improve the overall sedative and analgesic effects accordingly. However, the use of opioids alone is limited in horses due to the risk of sympathetic stimulation, central nervous system stimulation, excitement and head jerking. In some countries, butorphanol Citation: Nannarone, S.; Giannettoni, is currently the only licensed and most used opioid in equine medicine. We aimed to evaluate the G.; Laurenza, C.; Giontella, A.; pre-anaesthetic association of romifidine with either butorphanol or methadone. The two combi- Moretti, G. Methadone or nations -

Open Access Journal of Cardiology Ventricular Tachycardia During Ajmaline Challenge
Open Access Journal of Cardiology Ventricular Tachycardia During Ajmaline Challenge Estrada Parra I, Pavón Jimenez R, Leal del Ojo J, Garcia Medina D, Case Report Picon Heras R* and Pastor Torres L Volume 1 Issue 1 Received Date: May 22, 2017 Departamento de Cardiologia, Hospital Universitario Virgen de Valme, Spain Published Date: August 19, 2017 *Corresponding author: Rocio Picon, Departamento de Cardiologia, Hospital Universitario Virgen de Valme, Spain, E- mail: [email protected] Abstract We report the case of a 63 year old woman who comes to an ajmaline challenged. After 8 minutes of infusion her baseline ECG showed significant QRS complex prolongation and switched over to the typical coved-type ECG. Subsequently a sustained monomorphic ventricular tachycardia was developed, followed by a sustained polymorphyc VT onset, which finally degenerated in a hemodynamically non relevant sustained monomorphic VT. Finally, a 200J defibrillation was required to terminate the arrythmia. Sustained ventricular arrhytmia (SVA) is infrequent but not an exceptional event (0.1-18%) and ajmaline is considered a valuable drug. In addition, provocation testing must be performed in an appropiate environment with advanced life support facilities. The evidence shows that the occurrence of ajmaline-induced sustained ventricular arryhtmia in patients with BS might not identify a category at higher risk for further arrhythmic events during follow-up. Keywords: Brugada syndrome; Sodium channel blocker Challenge; Ajmaline Challenge; Ventricular arrhythmias; Proarrhythmia Abbrevations: ECG: Electrocardiography; BS: Brugada infusion she showed significant QRS complex Syndrome; SCB: Sodium Channel Blockers; VT: prolongation (174 ms) and ST elevation in the right Ventricular Tachycardia; SVA: Sustained ventricular precordial leads, which switched over to the typical arrhytmia coved-type ECG (Figure 2). -

Equine Anesthesia
• EQUINE ANESTHESIA Lyon Lee DVM PhD DACVA Introduction • Higher morbidity and mortality associated with general anesthesia (1:100) in comparison to small animals (1:1000) or human (1: 200,000) • No change of the risk ratio for the last 30 years, but the duration of surgery extended. • Unique anatomic and physiologic characteristics presents additional challenge • More pronounced cardiovascular depression (hypotension and reduced cardiac output) at equipotent MAC than other species such as dogs and cats • The size, weight temperament and tendency to panic of the adult horse introduce the risk of injury to the patient and to the personnel. • Prolonged recumbency is unnatural in the horse • When a horse is placed in dorsal recumbency, the weight of the abdominal contents presses on the diaphragm and limits lung expansion, leading to hypoventilation. If the drugs used to produce anesthesia depress cardiovascular function, these changes will be exaggerated due to a ventilation-perfusion mismatch. Standing chemical restraint and preanesthetic agents • Due to higher risk associated with general anesthesia in this species, standing chemical restraint can offer safer alternative for many procedures • Neuroleptanalgesia (neuroleptics + opioids) or sedative/opioid combination are most popular • Produced by the concurrent administration of a sedative/tranquilizer and a narcotic analgesic (e.g. detomidine and butorphanol; acepromazine and morphine) • Better restraint and analgesia (the combination is synergistic, not merely additive) • Many procedures can be performed which would not be possible with the tranquilizer or sedative alone • Dose sparing effect on both drugs • Better cardiovascular preservation • Can provide satisfactory working condition for minor surgery when combined with local anesthesia • Less expense, less risk, less logistics • This combination can also be effective as preanesthetic medication to produce reliable sedation (e.g. -

The Anti-Addiction Drug Ibogaine and the Heart: a Delicate Relation
Molecules 2015, 20, 2208-2228; doi:10.3390/molecules20022208 OPEN ACCESS molecules ISSN 1420-3049 www.mdpi.com/journal/molecules Review The Anti-Addiction Drug Ibogaine and the Heart: A Delicate Relation Xaver Koenig * and Karlheinz Hilber * Department of Neurophysiology and Neuropharmacology, Center for Physiology and Pharmacology, Medical University of Vienna, Schwarzspanierstrasse 17, Vienna 1090, Austria * Authors to whom correspondence should be addressed; E-Mails: [email protected] (X.K.); [email protected] (K.H.); Tel.: +43-1-40160-31232 (X.K.); +43-1-40160-31230 (K.H.); Fax: +43-1-40160-931300 (X.K. & K.H.). Academic Editor: Patricia Valentao Received: 24 October 2014 / Accepted: 26 November 2014 / Published: 29 January 2015 Abstract: The plant indole alkaloid ibogaine has shown promising anti-addictive properties in animal studies. Ibogaine is also anti-addictive in humans as the drug alleviates drug craving and impedes relapse of drug use. Although not licensed as therapeutic drug and despite safety concerns, ibogaine is currently used as an anti-addiction medication in alternative medicine in dozens of clinics worldwide. In recent years, alarming reports of life-threatening complications and sudden death cases, temporally associated with the administration of ibogaine, have been accumulating. These adverse reactions were hypothesised to be associated with ibogaine’s propensity to induce cardiac arrhythmias. The aim of this review is to recapitulate the current knowledge about ibogaine’s effects on the heart and the cardiovascular system, and to assess the cardiac risks associated with the use of this drug in anti- addiction therapy. The actions of 18-methoxycoronaridine (18-MC), a less toxic ibogaine congener with anti-addictive properties, are also considered.