Ventricular Tachycardia Drugs Versus Devices John Camm St
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
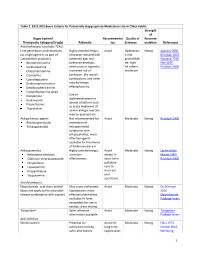
Table 2. 2012 AGS Beers Criteria for Potentially
Table 2. 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Strength of Organ System/ Recommendat Quality of Recomm Therapeutic Category/Drug(s) Rationale ion Evidence endation References Anticholinergics (excludes TCAs) First-generation antihistamines Highly anticholinergic; Avoid Hydroxyzin Strong Agostini 2001 (as single agent or as part of clearance reduced with e and Boustani 2007 combination products) advanced age, and promethazi Guaiana 2010 Brompheniramine tolerance develops ne: high; Han 2001 Carbinoxamine when used as hypnotic; All others: Rudolph 2008 Chlorpheniramine increased risk of moderate Clemastine confusion, dry mouth, Cyproheptadine constipation, and other Dexbrompheniramine anticholinergic Dexchlorpheniramine effects/toxicity. Diphenhydramine (oral) Doxylamine Use of diphenhydramine in Hydroxyzine special situations such Promethazine as acute treatment of Triprolidine severe allergic reaction may be appropriate. Antiparkinson agents Not recommended for Avoid Moderate Strong Rudolph 2008 Benztropine (oral) prevention of Trihexyphenidyl extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Antispasmodics Highly anticholinergic, Avoid Moderate Strong Lechevallier- Belladonna alkaloids uncertain except in Michel 2005 Clidinium-chlordiazepoxide effectiveness. short-term Rudolph 2008 Dicyclomine palliative Hyoscyamine care to Propantheline decrease Scopolamine oral secretions. Antithrombotics Dipyridamole, oral short-acting* May -

Vernakalant Versus Ibutilide for Immediate Conversion of Recent-Onset Atrial Fibrillation Vogiatzis I, Papavasiliou E, Dapcevitch I, Pittas S, Koulouris E
HIPPOKRATIA 2017, 21, 2: 67-73 RESEARCH ARTICLE Vernakalant versus ibutilide for immediate conversion of recent-onset atrial fibrillation Vogiatzis I, Papavasiliou E, Dapcevitch I, Pittas S, Koulouris E Department of Cardiology, General Hospital of Veroia, Veroia, Greece Abstract Background: The pharmacological cardioversion of recent-onset atrial fibrillation (AF) is a challenge for the clinician. The aim of the study was to compare the efficacy, the safety, and the overall cost of intravenous (iv) administration of vernakalant, which is a relatively new atrial-selective antiarrhythmic agent, versus ibutilide, in cardioversion of recent- onset AF. Methods: We enrolled in this study 78 patients (56 men, 22 women; mean age 63.72 ± 6.67 years) who presented with recent-onset AF. Cardioversion was attempted in 36 patients (group A: 24 men, 12 women; mean age 62.44 ± 7.24 years) by iv administration of vernakalant (3 mg/kg over 10 min and if needed after 15 min, a second dose 2 mg/kg over 10 min) while in 42 patients (group B: 32 men, 10 women; mean age 64.81 ± 6 years) iv ibutilide was administered (1 mg over 10 min and if needed after 10 min, a second dose 1 mg over 10 min). Results: AF was successfully converted in 52.78 % of (n =19) patients of group A vs 52.38 % of (n =22) patients of group B (p =0.58), with an average time of conversion 11.8 ± 4.3 min for group A patients vs 33.9 ± 20.25 min for group B patients (p <0.0001). The average length of hospital stay for patients of group A was 17.64 ± 15.96 hours vs 41.09 ± 17.6 hours for patients of Group B (p <0.0001). -

Safety and Efficacy of Dronedarone from Clinical Trials to Real
Europace (2019) 21, 1764–1775 REVIEW doi:10.1093/europace/euz193 Safety and efficacy of dronedarone from clinical Downloaded from https://academic.oup.com/europace/article-abstract/21/12/1764/5536329 by Uppsala Universitetsbibliotek user on 20 February 2020 trials to real-world evidence: implications for its use in atrial fibrillation Giuseppe Boriani1, Carina Blomstro¨m-Lundqvist2, Stefan H. Hohnloser3, Lennart Bergfeldt4,5, Giovanni L. Botto6, Alessandro Capucci7, Ignacio Ferna´ndez Lozano8, Andreas Goette9,10, Carsten W. Israel3,11, Jose´ L. Merino12, and A. John Camm13* 1Division of Cardiology, Department of Biomedical, Metabolic and Neural Sciences, University of Modena and Reggio Emilia, Policlinico di Modena, Modena, Italy; 2Department of Medical Science and Cardiology, Uppsala University, Uppsala, Sweden; 3Division of Clinical Electrophysiology, Department of Cardiology, J W Goethe University, Frankfurt, Germany; 4Department of Molecular and Clinical Medicine, Institute of Medicine, Sahlgrenska Academy, University of Gothenburg, Gothenburg, Sweden; 5Va¨stra Go¨taland, Department of Cardiology, Sahlgrenska University Hospital, Gothenburg, Sweden; 6ASST Rhodense, Ospedale di Circolo Rho, Milan, Italy; 7Universita` Politecnica delle Marche, Ancona, Italy; 8Sociedad Espanola~ de Cardiologı´a, Madrid, Spain; 9Medical Clinic II, Cardiology Department, St Vincenz-Krankenhaus Paderborn, Paderborn, Germany; 10Working Group Molecular Electrophysiology, University Hospital Magdeburg, Magdeburg, Germany; 11Clinic of Internal Medicine, Bethel-Clinic, Bielefeld, Germany; 12Arrhythmia & Robotic EP Unit, Hospital Universitario La Paz-IdiPaz, Madrid, Spain; and 13Cardiology Clinical Academic Group, Molecular and Clinical Sciences Institute, St George’s University of London, Cranmer Terrace, London SW17 0RE, UK Received 17 May 2019; editorial decision 13 June 2019; accepted 20 June 2019; online publish-ahead-of-print 19 July 2019 Efficacy and safety of dronedarone was shown in the ATHENA trial for paroxysmal or persistent atrial fibrillation (AF) patients. -

Arrhythmias in the Intensive Care Patient Hans-Joachim Trappe, Bodo Brandts and Peter Weismueller
Arrhythmias in the intensive care patient Hans-Joachim Trappe, Bodo Brandts and Peter Weismueller Purpose of review ventricular fibrillation. The use of automatic external Atrial fibrillation, atrial flutter, AV–nodal reentry tachycardia defibrillators by basic life support ambulance providers or first with rapid ventricular response, atrial ectopic tachycardia, and responder in early defibrillation programs has been associated preexcitation syndromes combined with atrial fibrillation or with a significant increase in survival rates. Drugs such as ventricular tachyarrhythmias are typical arrhythmias in intensive lidocaine, procainamide, sotalol, amiodarone, or magnesium care patients. Most frequently, the diagnosis of the underlying were recommended for treatment of ventricular arrhythmia is possible from the physical examination, the tachyarrhythmias in intensive care patients. Amiodarone is a response to maneuvers or drugs, and the 12-lead surface highly efficacious antiarrhythmic agent for many cardiac electrocardiogram. In all patients with unstable hemodynamics, arrhythmias, ranging from atrial fibrillation to malignant immediate DC-cardioversion is indicated. Conversion of atrial ventricular tachyarrhythmias, and seems to be superior to other fibrillation to sinus rhythm is possible using antiarrhythmic antiarrhythmic agents. drugs. Amiodarone has a conversion rate in atrial fibrillation of up to 80%. However, caution in the use of short-term Keywords administration of intravenous amiodarone in critically ill patients atrial fibrillation, -

Medication Guide MULTAQ (MUL-Tak) (Dronedarone) Tablets
17.2 Medication Guide Medication Guide MULTAQ (MUL-tak) (dronedarone) Tablets Read this Medication Guide before you start taking MULTAQ and each time you get a refill. There may be new information. This information does not take the place of talking with your doctor about your medical condition or your treatment. What is the most important information I should know about MULTAQ? MULTAQ can cause serious side effects. Do not take MULTAQ if you: 1. have symptoms of heart failure that recently worsened and you were hospitalized, or if you have severe heart failure. MULTAQ doubles your risk of dying if you have these conditions. Heart failure means your heart does not pump blood through your body as well as it should. Call your doctor right away if you have any signs or symptoms of heart failure during treatment with MULTAQ: • shortness of breath or wheezing at rest • wheezing, chest tightness or coughing up frothy sputum at rest, nighttime or after minor exercise • trouble sleeping or waking up at night because of breathing problems • using more pillows to prop yourself up at night so you can breathe more easily • gaining more than 5 pounds quickly • increasing swelling of feet or legs 2. have a type of atrial fibrillation (irregular heart rhythm) called permanent atrial fibrillation (AF). You and your doctor may decide not to try to change your heart rhythm back to a normal heart rhythm or your heart rhythm cannot be changed back to a normal rhythm. If you have permanent AF and take MULTAQ, you have a higher risk of death, stroke, and needing to be treated in a hospital for your heart failure. -

2D6 Substrates 2D6 Inhibitors 2D6 Inducers
Physician Guidelines: Drugs Metabolized by Cytochrome P450’s 1 2D6 Substrates Acetaminophen Captopril Dextroamphetamine Fluphenazine Methoxyphenamine Paroxetine Tacrine Ajmaline Carteolol Dextromethorphan Fluvoxamine Metoclopramide Perhexiline Tamoxifen Alprenolol Carvedilol Diazinon Galantamine Metoprolol Perphenazine Tamsulosin Amiflamine Cevimeline Dihydrocodeine Guanoxan Mexiletine Phenacetin Thioridazine Amitriptyline Chloropromazine Diltiazem Haloperidol Mianserin Phenformin Timolol Amphetamine Chlorpheniramine Diprafenone Hydrocodone Minaprine Procainamide Tolterodine Amprenavir Chlorpyrifos Dolasetron Ibogaine Mirtazapine Promethazine Tradodone Aprindine Cinnarizine Donepezil Iloperidone Nefazodone Propafenone Tramadol Aripiprazole Citalopram Doxepin Imipramine Nifedipine Propranolol Trimipramine Atomoxetine Clomipramine Encainide Indoramin Nisoldipine Quanoxan Tropisetron Benztropine Clozapine Ethylmorphine Lidocaine Norcodeine Quetiapine Venlafaxine Bisoprolol Codeine Ezlopitant Loratidine Nortriptyline Ranitidine Verapamil Brofaramine Debrisoquine Flecainide Maprotline olanzapine Remoxipride Zotepine Bufuralol Delavirdine Flunarizine Mequitazine Ondansetron Risperidone Zuclopenthixol Bunitrolol Desipramine Fluoxetine Methadone Oxycodone Sertraline Butylamphetamine Dexfenfluramine Fluperlapine Methamphetamine Parathion Sparteine 2D6 Inhibitors Ajmaline Chlorpromazine Diphenhydramine Indinavir Mibefradil Pimozide Terfenadine Amiodarone Cimetidine Doxorubicin Lasoprazole Moclobemide Quinidine Thioridazine Amitriptyline Cisapride -
Research in Your Backyard Developing Cures, Creating Jobs
Research in Your Backyard Developing Cures, Creating Jobs PHARMACEUTICAL CLINICAL TRIALS IN ILLINOIS Dots show locations of clinical trials in the state. Executive Summary This report shows that biopharmaceutical research com- Quite often, biopharmaceutical companies hire local panies continue to be vitally important to the economy research institutions to conduct the tests and in Illinois, and patient health in Illinois, despite the recession. they help to bolster local economies in communities all over the state, including Chicago, Decatur, Joliet, Peoria, At a time when the state still faces significant economic Quincy, Rock Island, Rockford and Springfield. challenges, biopharmaceutical research companies are conducting or have conducted more than 4,300 clinical For patients, the trials offer another potential therapeutic trials of new medicines in collaboration with the state’s option. Clinical tests may provide a new avenue of care for clinical research centers, university medical schools and some chronic disease sufferers who are still searching for hospitals. Of the more than 4,300 clinical trials, 2,334 the medicines that are best for them. More than 470 of the target or have targeted the nation’s six most debilitating trials underway in Illinois are still recruiting patients. chronic diseases—asthma, cancer, diabetes, heart dis- ease, mental illnesses and stroke. Participants in clinical trials can: What are Clinical Trials? • Play an active role in their health care. • Gain access to new research treatments before they In the development of new medicines, clinical trials are are widely available. conducted to prove therapeutic safety and effectiveness and compile the evidence needed for the Food and Drug • Obtain expert medical care at leading health care Administration to approve treatments. -

Constrictive Pericarditis Causing Ventricular Tachycardia.Pdf
EP CASE REPORT ....................................................................................................................................................... A visually striking calcific band causing monomorphic ventricular tachycardia as a first presentation of constrictive pericarditis Kian Sabzevari 1*, Eva Sammut2, and Palash Barman1 1Bristol Heart Institute, UH Bristol NHS Trust UK, UK; and 2Bristol Heart Institute, UH Bristol NHS Trust UK & University of Bristol, UK * Corresponding author. Tel: 447794900287; fax: 441173425926. E-mail address: [email protected] Introduction Constrictive pericarditis (CP) is a rare condition caused by thickening and stiffening of the pericar- dium manifesting in dia- stolic dysfunction and enhanced interventricu- lar dependence. In the developed world, most cases are idiopathic or are associated with pre- vious cardiac surgery or irradiation. Tuberculosis remains a leading cause in developing areas.1 Most commonly, CP presents with symptoms of heart failure and chest discomfort. Atrial arrhythmias have been described as a rare pre- sentation, but arrhyth- mias of ventricular origin have not been reported. Figure 1 (A) The 12 lead electrocardiogram during sustained ventricular tachycardia is shown; (B and C) Case report Different projections of three-dimensional reconstructions of cardiac computed tomography demonstrating a A 49-year-old man with a striking band of calcification around the annulus; (D) Carto 3DVR mapping—the left hand panel (i) demonstrates a background of diabetes, sinus beat with late potentials at the point of ablation in the coronary sinus, the right hand panel (iii) shows the hypertension, and hyper- pacemap with a 89% match to the clinical tachycardia [matching the morphology seen on 12 lead ECG (A)], and cholesterolaemia and a the middle panel (ii) displays the three-dimensional voltage map. -

Supplementary Information
Supplementary Information Network-based Drug Repurposing for Novel Coronavirus 2019-nCoV Yadi Zhou1,#, Yuan Hou1,#, Jiayu Shen1, Yin Huang1, William Martin1, Feixiong Cheng1-3,* 1Genomic Medicine Institute, Lerner Research Institute, Cleveland Clinic, Cleveland, OH 44195, USA 2Department of Molecular Medicine, Cleveland Clinic Lerner College of Medicine, Case Western Reserve University, Cleveland, OH 44195, USA 3Case Comprehensive Cancer Center, Case Western Reserve University School of Medicine, Cleveland, OH 44106, USA #Equal contribution *Correspondence to: Feixiong Cheng, PhD Lerner Research Institute Cleveland Clinic Tel: +1-216-444-7654; Fax: +1-216-636-0009 Email: [email protected] Supplementary Table S1. Genome information of 15 coronaviruses used for phylogenetic analyses. Supplementary Table S2. Protein sequence identities across 5 protein regions in 15 coronaviruses. Supplementary Table S3. HCoV-associated host proteins with references. Supplementary Table S4. Repurposable drugs predicted by network-based approaches. Supplementary Table S5. Network proximity results for 2,938 drugs against pan-human coronavirus (CoV) and individual CoVs. Supplementary Table S6. Network-predicted drug combinations for all the drug pairs from the top 16 high-confidence repurposable drugs. 1 Supplementary Table S1. Genome information of 15 coronaviruses used for phylogenetic analyses. GenBank ID Coronavirus Identity % Host Location discovered MN908947 2019-nCoV[Wuhan-Hu-1] 100 Human China MN938384 2019-nCoV[HKU-SZ-002a] 99.99 Human China MN975262 -

Systematic Review of the Effect of Intravenous Lipid Emulsion Therapy for Non-Local Anesthetics Toxicity
Clinical Toxicology ISSN: 1556-3650 (Print) 1556-9519 (Online) Journal homepage: http://www.tandfonline.com/loi/ictx20 Systematic review of the effect of intravenous lipid emulsion therapy for non-local anesthetics toxicity Michael Levine, Robert S. Hoffman, Valéry Lavergne, Christine M. Stork, Andis Graudins, Ryan Chuang, Samuel J. Stellpflug, Martin Morris, Andrea Miller-Nesbitt, Sophie Gosselin & for the Lipid Emulsion Workgroup* To cite this article: Michael Levine, Robert S. Hoffman, Valéry Lavergne, Christine M. Stork, Andis Graudins, Ryan Chuang, Samuel J. Stellpflug, Martin Morris, Andrea Miller-Nesbitt, Sophie Gosselin & for the Lipid Emulsion Workgroup* (2016) Systematic review of the effect of intravenous lipid emulsion therapy for non-local anesthetics toxicity, Clinical Toxicology, 54:3, 194-221, DOI: 10.3109/15563650.2015.1126286 To link to this article: http://dx.doi.org/10.3109/15563650.2015.1126286 Published online: 06 Feb 2016. Submit your article to this journal Article views: 692 View related articles View Crossmark data Citing articles: 2 View citing articles Full Terms & Conditions of access and use can be found at http://www.tandfonline.com/action/journalInformation?journalCode=ictx20 Download by: [UPSTATE Medical University Health Sciences Library] Date: 03 August 2016, At: 08:19 CLINICAL TOXICOLOGY, 2016 VOL. 54, NO. 3, 194–221 http://dx.doi.org/10.3109/15563650.2015.1126286 REVIEW Systematic review of the effect of intravenous lipid emulsion therapy for non-local anesthetics toxicity Michael Levinea, Robert S. Hoffmanb, Vale´ry Lavergnec, Christine M. Storkd, Andis Graudinse, Ryan Chuangf, Samuel J. Stellpflugg, Martin Morrish, Andrea Miller-Nesbitth, Sophie Gosselini and for the Lipid Emulsion Workgroup* aDepartment of Emergency Medicine, Section of Medical Toxicology, University of Southern California, Los Angeles, CA, USA; bDivision of Medical Toxicology, Ronald O. -

)&F1y3x PHARMACEUTICAL APPENDIX to THE
)&f1y3X PHARMACEUTICAL APPENDIX TO THE HARMONIZED TARIFF SCHEDULE )&f1y3X PHARMACEUTICAL APPENDIX TO THE TARIFF SCHEDULE 3 Table 1. This table enumerates products described by International Non-proprietary Names (INN) which shall be entered free of duty under general note 13 to the tariff schedule. The Chemical Abstracts Service (CAS) registry numbers also set forth in this table are included to assist in the identification of the products concerned. For purposes of the tariff schedule, any references to a product enumerated in this table includes such product by whatever name known. Product CAS No. Product CAS No. ABAMECTIN 65195-55-3 ACTODIGIN 36983-69-4 ABANOQUIL 90402-40-7 ADAFENOXATE 82168-26-1 ABCIXIMAB 143653-53-6 ADAMEXINE 54785-02-3 ABECARNIL 111841-85-1 ADAPALENE 106685-40-9 ABITESARTAN 137882-98-5 ADAPROLOL 101479-70-3 ABLUKAST 96566-25-5 ADATANSERIN 127266-56-2 ABUNIDAZOLE 91017-58-2 ADEFOVIR 106941-25-7 ACADESINE 2627-69-2 ADELMIDROL 1675-66-7 ACAMPROSATE 77337-76-9 ADEMETIONINE 17176-17-9 ACAPRAZINE 55485-20-6 ADENOSINE PHOSPHATE 61-19-8 ACARBOSE 56180-94-0 ADIBENDAN 100510-33-6 ACEBROCHOL 514-50-1 ADICILLIN 525-94-0 ACEBURIC ACID 26976-72-7 ADIMOLOL 78459-19-5 ACEBUTOLOL 37517-30-9 ADINAZOLAM 37115-32-5 ACECAINIDE 32795-44-1 ADIPHENINE 64-95-9 ACECARBROMAL 77-66-7 ADIPIODONE 606-17-7 ACECLIDINE 827-61-2 ADITEREN 56066-19-4 ACECLOFENAC 89796-99-6 ADITOPRIM 56066-63-8 ACEDAPSONE 77-46-3 ADOSOPINE 88124-26-9 ACEDIASULFONE SODIUM 127-60-6 ADOZELESIN 110314-48-2 ACEDOBEN 556-08-1 ADRAFINIL 63547-13-7 ACEFLURANOL 80595-73-9 ADRENALONE -

What Are Premature Ventricular Contractions?
What Are Premature Ventricular Contractions? Premature ventricular contractions (VPCs or PVCs) are irregular beats that originate from the heart’s pumping chambers (ventricles). These beats interrupt the normal regular (sinus) rhythm, and result in irregularity to the heart rhythm. Although single PVCs are not life- threatening, they may indicate the presence of underlying heart disease, or when they become more severe can cause rapid and dangerous increases in heart rate (ventricular tachycardia). WHAT CAUSES PREMATURE VENTRICULAR CONTRACTIONS? PVCs can occur secondary to a variety of causes, most concerning being cardiac disease. PVCs are most commonly seen in dogs with Dilated Cardiomyopathy, but can also occur in the later stages of disease with Myxomatous Mitral Valve Degeneration. PVCs and other ventricular arrhythmias can also with no evidence of underlying structural heart disease. The workup for PVCs can be frustrating, because PVCs can also occur secondary to conditions unrelated to the heart. Most commonly they can occur secondary to gastrointestinal disease, systemic disease, and pain. HOW ARE PREMATURE VENTRICULAR CONTRACTIONS DIAGNOSED? Most commonly, your veterinarian will hear an irregular heart rhythm and recommend an electrocardiogram (ECG) to assess the heart rhythm. The ECG will enable your veterinarian to determine whether the irregular rhythm is due to PVCs. Following this diagnosis, there are several additional recommended tests. TESTING Following this diagnosis, there are several additional recommended tests. ECHOCARDIOGRAPHY Echocardiography (heart ultrasound) is recommended to make sure that there is no evidence of structural cardiac disease causing the abnormal heart rhythm. 24-HOUR HOLTER Single PVCs usually do not require treatment, however a Holter monitor will determine whether the frequency or severity of the MONITOR PVCs warrant anti-arrhythmic medication, and make sure that there is no evidence of ventricular tachycardia, which is a life threatening heart rhythm.