Breech Childbirth
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Childbirth Education Booklet
Childbirth Education Contents Normal Discomforts of Pregnancy 2 Call Your Doctor 4 Late Pregnancy 5 Labor: Stage 1 6 Labor: Stages 2 & 3 8 Breastfeeding in the Hospital 9 Breathing Techniques 10 Birth Plans 10 Labor Positions 11 How Your Partner and Doula Can Help 13 Packing for the Hospital 15 Normal Discomforts of Pregnancy Fatigue Backache • Listen to your body, take naps, get extra rest • Maintain correct posture • Do pelvic tilt exercises while standing and on hands Stuffy Nose and knees • Warm compresses to nose • While on all fours, crawl forwards and backwards, • Cool mist humidifier in your home or rock, and do pelvic tilts bedroom at night • When picking up something lift with your legs to protect your back Shortness of Breath • Don’t stay that way, slow down and catch your breath • For prolonged standing, elevate 1 foot on a step stool • Sleep propped up with pillows or in recliner • Receive back massages • Maintain correct posture Dribble Urine • Moderate intensity exercising (walking, stationary • Do Kegel exercises – at least 50 a day bike, swim, flexibility moves) (do 10 every time you wash your hands) • How can you tell if you are dribbling urine or your Heartburn/Nausea water broke? Call your OB or midwife, and remember • Don’t eat 3 big meals a day, eat 5-6 smaller meals this acronym: • Drink 8 cups of water a day COAT. C=color, O=odor, A=amount, T=time. • Have dry crackers/cereal to nibble on–keep in purse and at bedside • Don’t let stomach become empty • Eat well balanced diet–vitamin B may help to decrease • Avoid -

The Effects of Alcohol in Newborns Efeitos Do Álcool No Recém-Nascido
REVIEW The effects of alcohol in newborns Efeitos do álcool no recém-nascido Maria dos Anjos Mesquita* ABSTRACT alcoólicas leva a prejuízos individuais, para a sua família e para The purpose of this article was to present a review of the effects toda a sociedade. Apesar disso, a dificuldade do seu diagnóstico e of alcohol consumption by pregnant mothers on their newborn. a inexperiência dos profissionais de saúde faz com que o espectro Definitions, prevalence, pathophysiology, clinical features, diagnostic dessas lesões seja pouco lembrado e até desconhecido. As lesões criteria, follow-up, treatment and prevention were discussed. A causadas pela ação do álcool no concepto são totalmente prevenidas search was performed in Medline, LILACS, and SciELO databases se a gestante não consumir bebidas alcoólicas durante a gestação. using the following terms: “fetus”, “newborn”, “pregnant woman”, Assim, é fundamental a detecção das mulheres consumidoras “alcohol”, “alcoholism”, “fetal alcohol syndrome”, and “alcohol- de álcool durante a gravidez e o desenvolvimento de programas related disorders”. Portuguese and English articles published from específicos de alerta sobre as consequências do álcool durante a 2000 to 2009 were reviewed. The effects of alcohol consumed by gestação e amamentação. pregnant women on newborns are extremely serious and occur frequently; it is a major issue in Public Health worldwide. Fetal alcohol Descritores: Bebidas alcoólicas/efeitos adversos; Feto; Recém-nascido; spectrum disorders cause harm to individuals, their families, and the Síndrome alcoólica fetal; Transtornos relacionados ao uso de álcool entire society. Nevertheless, diagnostic difficulties and inexperience of healthcare professionals result in such damage, being remembered rarely or even remaining uncovered. -

Care During Pregnancy and Delivery ACCESSIBLE, QUALITY HEALTH CARE DURING PREGNANCY and DELIVERY
Care during Pregnancy and Delivery ACCESSIBLE, QUALITY HEALTH CARE DURING PREGNANCY AND DELIVERY Why It’s Important Having a healthy pregnancy and access to quality birth facilities are the best ways to promote a healthy birth and have a thriving newborn. Getting early and regular prenatal care is vital. Prenatal care is the health care that women receive during their entire pregnancy. Prenatal care is more than doctor’s visits and ultrasounds; it is an opportunity to improve the overall well-being and health of the mom which directly affects the health of her baby. Prenatal visits give parents a chance to ask questions, discuss concerns, treat complications in a timely manner, and ensure that mom and baby are safe during pregnancy and delivery. Receiving quality prenatal care can have positive effects long after birth for both the mother and baby. When it is time for the mother to give birth, having access to safe, high quality birth facilities is critical. Early prenatal care, starting in the 1st trimester, is crucial to the health of mothers and babies. But more important than just initiating early prenatal care is receiving adequate prenatal care, having the appropriate number of prenatal care visits at the appropriate intervals throughout the pregnancy. Babies of mothers who do not get prenatal care are three times more likely to be born low birth weight and five times more likely to die than those born to mothers who do get care.1 In 2017 in Minnesota, only 77.1 percent of women received prenatal care within their first trimester of pregnancy. -
Turning Your Breech Baby to a Head-Down Position (External Cephalic Version)
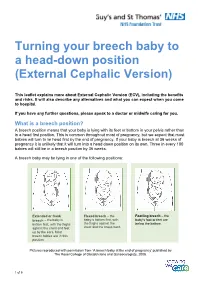
Turning your breech baby to a head-down position (External Cephalic Version) This leaflet explains more about External Cephalic Version (ECV), including the benefits and risks. It will also describe any alternatives and what you can expect when you come to hospital. If you have any further questions, please speak to a doctor or midwife caring for you. What is a breech position? A breech position means that your baby is lying with its feet or bottom in your pelvis rather than in a head first position. This is common throughout most of pregnancy, but we expect that most babies will turn to lie head first by the end of pregnancy. If your baby is breech at 36 weeks of pregnancy it is unlikely that it will turn into a head down position on its own. Three in every 100 babies will still be in a breech position by 36 weeks. A breech baby may be lying in one of the following positions: Extended or frank Flexed breech – the Footling breech – the breech – the baby is baby is bottom first, with baby’s foot or feet are bottom first, with the thighs the thighs against the below the bottom. against the chest and feet chest and the knees bent. up by the ears. Most breech babies are in this position. Pictures reproduced with permission from ‘A breech baby at the end of pregnancy’ published by The Royal College of Obstetricians and Gynaecologists, 2008. 1 of 5 What causes breech? Breech is more common in women who are expecting twins, or in women who have a differently-shaped womb (uterus). -

14. Management of Diabetes in Pregnancy: Standards of Medical
Diabetes Care Volume 42, Supplement 1, January 2019 S165 14. Management of Diabetes in American Diabetes Association Pregnancy: Standards of Medical Care in Diabetesd2019 Diabetes Care 2019;42(Suppl. 1):S165–S172 | https://doi.org/10.2337/dc19-S014 14. MANAGEMENT OF DIABETES IN PREGNANCY The American Diabetes Association (ADA) “Standards of Medical Care in Diabetes” includes ADA’s current clinical practice recommendations and is intended to provide the components of diabetes care, general treatment goals and guidelines, and tools to evaluate quality of care. Members of the ADA Professional Practice Committee, a multidisciplinary expert committee, are responsible for updating the Standards of Care annually, or more frequently as warranted. For a detailed description of ADA standards, statements, and reports, as well as the evidence-grading system for ADA’s clinical practice recommendations, please refer to the Standards of Care Introduction. Readers who wish to comment on the Standards of Care are invited to do so at professional.diabetes.org/SOC. DIABETES IN PREGNANCY The prevalence of diabetes in pregnancy has been increasing in the U.S. The majority is gestational diabetes mellitus (GDM) with the remainder primarily preexisting type 1 diabetes and type 2 diabetes. The rise in GDM and type 2 diabetes in parallel with obesity both in the U.S. and worldwide is of particular concern. Both type 1 diabetes and type 2 diabetes in pregnancy confer significantly greater maternal and fetal risk than GDM, with some differences according to type of diabetes. In general, specific risks of uncontrolled diabetes in pregnancy include spontaneous abortion, fetal anomalies, preeclampsia, fetal demise, macrosomia, neonatal hypoglycemia, and neonatal hyperbilirubinemia, among others. -

If You Are Pregnant: INFORMATION on FETAL DEVELOPMENT, ABORTION and ALTERNATIVES August 2019
If You Are Pregnant: INFORMATION ON FETAL DEVELOPMENT, ABORTION AND ALTERNATIVES August 2019 IF YOU ARE PREGNANT: INFORMATION ON FETAL DEVELOPMENT, ABORTION AND ALTERNATIVES If You Are Pregnant: Information on Fetal Development, Abortion and Alternatives Resources used by the Minnesota Department of Health for this publication are Human Embryology and Developmental Biology, Fifth Edition, 2014; Larsen’s Human Embryology, Fifth Edition, 2014; The Developing Human, 10th Edition, 2016; and In the Womb, 2006. The photographs in this booklet are credited to Lennart Nilsson/TT Images and are used by permission; except for week 38 copyright Minnesota Department of Health. The illustrations found throughout this booklet were created by Peg Gerrity, Houston, Texas. Copyright: http://www.peggerrity.com. Minnesota Department of Health Division of Child and Family Health PO Box 64882 St. Paul, MN 55164-0882 651-201-3580 Women's Right to Know (https://www.health.state.mn.us/people/wrtk/index.html) Upon request, this material will be made available in an alternative format such as large print, Braille or audio recording. Printed on recycled paper. 2 IF YOU ARE PREGNANT: INFORMATION ON FETAL DEVELOPMENT, ABORTION AND ALTERNATIVES Contents If You Are Pregnant: INFORMATION ON FETAL DEVELOPMENT, ABORTION AND ALTERNATIVES............................................................................................................................. 1 Introduction ............................................................................................................................... -

Vaginal Breech Birth Mary Olusile Lecturer in Practice
1 Vaginal Breech birth Mary Olusile Lecturer in Practice Breech: is where the fetal buttocks is the presenting part. Occurs in 15% of pregnancies at 28wks reducing to 3-4% at term Usually associated with: Uterine & pelvic anomalies - bicornuate uterus, lax uterus, fibroids and cysts Fetal anomalies - anencephaly, hydrocephaly, multiple gestation, oligohydraminous and polyhydraminous Cornually placed placenta (probably the commonest cause). Diagnosis: by abdominal examination or vaginal examination and confirmed by ultrasound scan Vaginal Breech VS. Caesarean Section Trial by Hannah et al (2001) found CS to produce better outcomes than vaginal breech but does acknowledge that may be due to lost skills of operators Therefore recommended mode of delivery is CS Limitations of trial by Hannah et al have since been highlighted questioning results and conclusion (Kotaska 2004) Now some advocates for vaginal breech birth when selection is based on clear prelabour and intrapartum criteria (Alarab et al 2004) Breech birth is u sually not an option except at clients choice Important considerations are size of fetus, presentation, attitude, size of maternal pelvis and parity of the woman NICE recommendation: External cephalic version (ECV) to be considered and offered if appropriate Produced by CETL 2007 2 Vaginal Breech birth Anterior posterior diameter of the pelvic brim is 11 cm Oblique diameter of the pelvic brim is 12 cm Transverse diameter of the pelvic brim is 13 cm Anterior posterior diameter of the outlet is 13 cm Produced by CETL 2007 3 -

Pregnancy-Related Changes You Can Expect Before and After Baby Comes
Pregnancy-related changes you can expect before and after baby comes When you start sharing the news that you’re pregnant, everyBABY single mother you know will inevitably bombard you with opinions, stories and advice on what to do NEWBEAUTY.COM during the nine months of constant change. While the well-meaning do really mean well, not every mom-to- be will experience the same concerns. To sort through 150 the stockpile of information, we asked experts to share their tips on how to keep skin happy through each trimester, and what to do when it’s not. SPRING 2021 SPRING ON BOARDby Tatiana Bido VICTOR DYOMIN/GETTY IMAGES, IMAGE USED FOR ILLUSTRATIVE PURPOSES ONLY ONLY PURPOSES ILLUSTRATIVE FOR USED IMAGE IMAGES, DYOMIN/GETTY VICTOR Maternity vs. Nursing Glow Recipe Bras Turns out, the often talked about “pregnancy glow” is real. “Due to excess sebum production from glandular tissue and increased blood volume, skin swells and Breast changes start happening many women experience what is known as a pregnancy glow,” explains New pretty early on—around six to eight York gynecologist Dr. Monica Grover. However, many women also experience weeks—and many moms-to-be find uncomfortable pregnancy-related skin changes as early as the first trimester, that they outgrow their everyday while others don’t until their second or third. “This is why it’s so important to bras very quickly. Normal weight use skin-care products that are clean and clinical because they will support gain and an expanding rib cage are the most common pregnancy-related skin issues and have the highest-quality to blame for the first set of changes, standards and be made in a sterile environment with the most carefully followed by expanding mammary sourced ingredients,” advises master aesthetician Abigail Zsenai. -

The International Childbirth Initiative (ICI)
The International Childbirth Initiative (ICI) 12 Steps to Safe and Respectful MotherBaby-Family Maternity Care The International Childbirth Initiative (ICI) was developed in a consultative consensus process with supporting and endorsing partner organizations. International Federation of Gynaecology and Obstetrics (FIGO) International MotherBaby Childbirth Organization (IMBCO) White Ribbon Alliance for Safe Motherhood (WRA) International Confederation of Midwives (ICM) International Pediatrics Association (IPA) Lamaze International International Childbirth Education Association (ICEA) Every Mother Counts Bumi Sehat Foundation DONA International Mercy in Action ICI Executive Group Contact Information André Lalonde Debra Pascali Bonaro FIGO Liaison and ICI Executive Chairperson IMBCO Liaison Email: [email protected] Email: [email protected] Tel: +1 613 804 1801 Tel: +1 201 851 101 Skype: andre180143 Skype: debrapb ICI Website www.internationalchildbirth.com SEPTEMBER 2018 1 Introduction The International Childbirth Initiative (ICI) 12 Steps to Safe and Respectful MotherBaby-Family Maternity Care1 Introduction Background In 2008, the International MotherBaby Childbirth Organization (IMBCO) launched the International MotherBaby Childbirth Initiative (IMBCI): 10 Steps to Optimal MotherBaby Maternity Services. The IMBCI embodied the Principles and Steps of the US-based Mother-Friendly Childbirth Initiative (MFCI), adapting it for use at the global level (1). In 2014, the International Federation of Gynecology and Obstetrics (FIGO), collaborating with the World Health Organization (WHO), the International Confederation of Midwives (ICM), the International Pediatrics Association (IPA) and the White Ribbon Alliance (WRA), launched the FIGO Guidelines to Mother-Baby Friendly Birthing Facilitie, (2) inspired by the WHO/UNICEF Baby-Friendly Hospital Initiative (BFHI), and grounded philosophically and ethically in the White Ribbon Alliance charter on Respectful Maternity Care: The Universal Rights of Childbearing Women. -

Childbirth Education
International Journal of Childbirth Education Open Focus The official publication of the International Childbirth Education Association VOLUME 31 NUMBER 3 JULY 2016 2016 October 13 ‐15 Core Conference October 11 & 12 Preconference workshops Renaissance Denver Stapleton Hotel 3801 Quebec Street | Denver, CO 80207 Free airport shuttle Reaching the Highest Peaks in Evidence‐Based Practice Join us for the 2016 Conference! Sessions this year will include information on: Learning Lab Skills Sessions Waterbirth Science and Safety Preconference Workshops: Somatic Trauma Resolution . Professional Childbirth Self – Care for the birth professional Educator Workshop Perinatal Mood and Anxiety Disorders . Birth Doula Workshop ICEA Member reception hosted by the President . Postpartum Doula Workshop . Early Lactation Care Workshop We are excited to feature these Internationally acclaimed childbirth activists and speakers: NEW THIS YEAR! “Tools For Success” Workshop: Part 1 Creating & Developing an Effective Curriculum Part 2 PowerPoint‐ Creativity, Productivity and Professionalism Barbara Harper RN CD CCE Jennie Joseph LM CPM Rep. Kelly Townsend Doula & member of AZ House of Representatives FREE Certificate For the first time ever Attendees who attend all Concurrent Session Speakers Include: general sessions with Jennie Nicette Jukelevics | Birdie Gunyon Meyer | Jeanne Green Joseph will receive a certificate Donna Walls | Connie Livingston | Tamela Hatcher | Lisa Wilson as a Maternal Child Health Jennifer Shryock | Colleen Weeks | Jana McCarthy -

OB/GYN – Childbirth/Labor/Delivery Protocol 6 - 2
Section SECTION: Obstetrical and Gynecological Emergencies REVISED: 06/2015 6 1. Physiologic Changes with Pregnancy Protocol 6 - 1 2. OB/GYN – Childbirth/Labor/Delivery Protocol 6 - 2 3. Medical – Newborn/Neonatal Protocol 6 - 3 OB / GYN Resuscitation 4. OB/GYN – Pregnancy Related Protocol 6 - 4 Emergencies (Delivery – Shoulder Dystocia) 5. OB/GYN – Pregnancy Related Protocol 6 - 5 Emergencies (Delivery – Breech Presentation) 6. OB/GYN – Pregnancy Related Protocol 6 - 6 Emergencies (Ectopic Pregnancy/Rupture) 7. OB/GYN – Pregnancy Related Protocol 6 - 7 EMERGENCIES Emergencies (Abruptio Placenta) 8. OB/GYN – Pregnancy Related Protocol 6 - 8 Emergencies (Placenta Previa) 9. OB/GYN – Pregnancy Related Protocol 6 - 9 Emergencies (Umbilical Cord Prolapse) 10. OB/GYN - Eclampsia Protocol 6 - 10 (Hypertension/Eclampsia/HELLPS) 11. OB/GYN – Pregnancy Related Protocol 6 - 11 Emergencies (Premature Rupture of Membranes (PROM)) 12. OB/GYN - Pre-term Labor Protocol 6 - 12 (Pre-term Labor) 13. OB/GYN – Post-partum Hemorrhage Protocol 6 - 13 Created, Developed, and Produced by the Old Dominion EMS Alliance Section 6 Continued This page intentionally left blank. OB / GYN EMERGENCIES Created, Developed, and Produced by the Old Dominion EMS Alliance Protocol SECTION: Obstetrical/Gynecological Emergencies PROTOCOL TITLE: Physiologic Changes with Pregnancy 6-1 REVISED: 06/2017 OVERVIEW: Many changes occur in the pregnant woman’s body, starting from the time of conception and throughout the pregnancy. The most obvious body system to undergo change is the reproductive system, but all of the others will change as well. Brief summaries of the physiologic changes that occur during pregnancy have been listed by system. Most of these physiologic changes will resolve during the postpartum period. -

Gestational Diabetes Fact Sheet
Gestational diabetes Between 3 – 20% of pregnant What is Gestational Diabetes Mellitus (GDM)? women develop GDM, GDM is a type of diabetes that occurs during pregnancy. Your body cannot depending on their risk factors. produce enough insulin to handle the effects of a growing baby and changing Risk Factors for GDM hormone levels. Insulin helps your body to control the level of glucose (sugar) in your blood. If your body cannot produce enough insulin, your blood sugar Being: levels will rise. • 35 years of age or older The good news • From a high-risk group (African, Arab, Asian, Hispanic, • Your baby will not be born with diabetes. Indigenous, or South Asian) • GDM can be managed and you can expect to have a happy, healthy baby Using: What does GDM mean for me? • Corticosteroid medication A diagnosis of GDM means you will be working closely with your health-care team to manage your blood sugar levels and keep them in the target range. Having: This will help you avoid complications in labor and delivery. After your baby • Obesity (BMI of 30 kg/m2 or is born, blood sugar levels will usually return to normal. However, you are greater) at greater risk for GDM in your next pregnancy and of developing type 2 • Prediabetes diabetes in the future. Achieving a healthy weight in the normal BMI range • GDM in a previous pregnancy can help reduce this risk. • Given birth to a baby that What does GDM mean for my baby? weighed more than 4 kg (9 lbs) If left undiagnosed or untreated, GDM can lead to high blood sugar levels.