International Consensus Guidance for Management of Myasthenia Gravis 2020 Update
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cutaneous Adverse Effects of Biologic Medications
REVIEW CME MOC Selena R. Pasadyn, BA Daniel Knabel, MD Anthony P. Fernandez, MD, PhD Christine B. Warren, MD, MS Cleveland Clinic Lerner College Department of Pathology Co-Medical Director of Continuing Medical Education; Department of Dermatology, Cleveland Clinic; of Medicine of Case Western and Department of Dermatology, W.D. Steck Chair of Clinical Dermatology; Director of Clinical Assistant Professor, Cleveland Clinic Reserve University, Cleveland, OH Cleveland Clinic Medical and Inpatient Dermatology; Departments of Lerner College of Medicine of Case Western Dermatology and Pathology, Cleveland Clinic; Assistant Reserve University, Cleveland, OH Clinical Professor, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University, Cleveland, OH Cutaneous adverse effects of biologic medications ABSTRACT iologic therapy encompasses an expo- B nentially expanding arena of medicine. Biologic therapies have become widely used but often As the name implies, biologic therapies are de- cause cutaneous adverse effects. The authors discuss the rived from living organisms and consist largely cutaneous adverse effects of tumor necrosis factor (TNF) of proteins, sugars, and nucleic acids. A clas- alpha inhibitors, epidermal growth factor receptor (EGFR) sic example of an early biologic medication is inhibitors, small-molecule tyrosine kinase inhibitors insulin. These therapies have revolutionized (TKIs), and cell surface-targeted monoclonal antibodies, medicine and offer targeted therapy for an including how to manage these reactions -

SPECIALTY MEDICATION ADMINISTRATION – SITE of CARE REVIEW GUIDELINES Policy Number: PHARMACY 276.15 T2 Effective Date: September 1, 2017
UnitedHealthcare® Oxford Clinical Policy SPECIALTY MEDICATION ADMINISTRATION – SITE OF CARE REVIEW GUIDELINES Policy Number: PHARMACY 276.15 T2 Effective Date: September 1, 2017 Table of Contents Page Related Policies INSTRUCTIONS FOR USE .......................................... 1 Actemra® (Tocilizumab) Injection for Intravenous CONDITIONS OF COVERAGE ...................................... 1 Infusion BENEFIT CONSIDERATIONS ...................................... 2 Entyvio® (Vedolizumab) COVERAGE RATIONALE ............................................. 2 Exondys 51™ (Eteplirsen) DEFINITIONS .......................................................... 3 Home Health Care DESCRIPTION OF SERVICES ...................................... 3 Infliximab (Remicade®, Inflectra™, Renflexis™) CLINICAL EVIDENCE ................................................. 3 ® REFERENCES ........................................................... 4 Orencia (Abatacept) Injection for Intravenous POLICY HISTORY/REVISION INFORMATION ................. 5 Infusion Radicava™ (Edaravone) Simponi Aria® (Golimumab) Injection for Intravenous Infusion Soliris® (Eculizumab) INSTRUCTIONS FOR USE This Clinical Policy provides assistance in interpreting Oxford benefit plans. Unless otherwise stated, Oxford policies do not apply to Medicare Advantage members. Oxford reserves the right, in its sole discretion, to modify its policies as necessary. This Clinical Policy is provided for informational purposes. It does not constitute medical advice. The term Oxford includes Oxford -

New Biological Therapies: Introduction to the Basis of the Risk of Infection
New biological therapies: introduction to the basis of the risk of infection Mario FERNÁNDEZ RUIZ, MD, PhD Unit of Infectious Diseases Hospital Universitario “12 de Octubre”, Madrid ESCMIDInstituto de Investigación eLibraryHospital “12 de Octubre” (i+12) © by author Transparency Declaration Over the last 24 months I have received honoraria for talks on behalf of • Astellas Pharma • Gillead Sciences • Roche • Sanofi • Qiagen Infections and biologicals: a real concern? (two-hour symposium): New biological therapies: introduction to the ESCMIDbasis of the risk of infection eLibrary © by author Paul Ehrlich (1854-1915) • “side-chain” theory (1897) • receptor-ligand concept (1900) • “magic bullet” theory • foundation for specific chemotherapy (1906) • Nobel Prize in Physiology and Medicine (1908) (together with Metchnikoff) Infections and biologicals: a real concern? (two-hour symposium): New biological therapies: introduction to the ESCMIDbasis of the risk of infection eLibrary © by author 1981: B-1 antibody (tositumomab) anti-CD20 monoclonal antibody 1997: FDA approval of rituximab for the treatment of relapsed or refractory CD20-positive NHL 2001: FDA approval of imatinib for the treatment of chronic myelogenous leukemia Infections and biologicals: a real concern? (two-hour symposium): New biological therapies: introduction to the ESCMIDbasis of the risk of infection eLibrary © by author Functional classification of targeted (biological) agents • Agents targeting soluble immune effector molecules • Agents targeting cell surface receptors -

Neuromyelitis Optica Spectrum Disorder
© Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 | Fax 503-947-2596 Drug Class Review with New Drug Evaluation: Biologics for Autoimmune Disorders-Neuromyelitis Optica Spectrum Disorder Date of Review: April 2021 Date of Last Review: n/a Dates of Literature Search: 1/1/1996 – 1/20/2021 Generic Name: Brand Name (Manufacturer): Eculizumab Soliris® (Alexion Pharmaceuticals) Inebilizumab-cdon Uplizna™ (Viela Bio) Satralizumab-mwge Enspryng™ (Genentech/Roche) Dossiers Received: Yes Current Status of PDL Class: See Appendix 1. Purpose for Class Update: To define place in therapy for 3 immunosuppressive agents, eculizumab, inebilizumab-cdon, and satralizumab-mwge, recently approved by the Food and Drug Administration (FDA) for the treatment adults with neuromyelitis optica spectrum disorder (NMOSD). Research Questions: 1. What is the effectiveness of eculizumab, inebilizumab, and satralizumab in reducing time to relapse in adult patients with NMOSD who are anti-aquaporin-4 (AQP4) antibody positive? 2. What are the harms of eculizumab, inebilizumab-cdon and satralizumab in adults with NMOSD? 3. Is there comparative evidence that eculizumab, inebilizumab, and satralizumab differ in efficacy or harms for management of NMOSD? 4. Are there certain sub-populations (based on age, gender, ethnicity, comorbidities, disease duration or severity) in which eculizumab, inebilizumab, or satralizumab may be beneficial -

Annex I Summary of Product Characteristics
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT YERVOY 5 mg/ml concentrate for solution for infusion 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each ml of concentrate contains 5 mg ipilimumab. One 10 ml vial contains 50 mg of ipilimumab. One 40 ml vial contains 200 mg of ipilimumab. Ipilimumab is a fully human anti-CTLA-4 monoclonal antibody (IgG1κ) produced in Chinese hamster ovary cells by recombinant DNA technology. Excipients with known effect: Each ml of concentrate contains 0.1 mmol sodium, which is 2.30 mg sodium. For the full list of excipients, see section 6.1. 3. PHARMACEUTICAL FORM Concentrate for solution for infusion (sterile concentrate). Clear to slightly opalescent, colourless to pale yellow liquid that may contain light (few) particulates and has a pH of 7.0 and an osmolarity of 260-300 mOsm/kg. 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Melanoma YERVOY as monotherapy is indicated for the treatment of advanced (unresectable or metastatic) melanoma in adults, and adolescents 12 years of age and older (see section 4.4). YERVOY in combination with nivolumab is indicated for the treatment of advanced (unresectable or metastatic) melanoma in adults. Relative to nivolumab monotherapy, an increase in progression-free survival (PFS) and overall survival (OS) for the combination of nivolumab with ipilimumab is established only in patients with low tumour PD-L1 expression (see sections 4.4 and 5.1). Renal cell carcinoma (RCC) YERVOY in combination with nivolumab is indicated for the first-line treatment of adult patients with intermediate/poor-risk advanced renal cell carcinoma (see section 5.1). -

Middle Level IM-MS and CIU Experiments for Improved Therapeutic Immunoglobulin Subclass Fingerprinting ACS Paragon Plus Environment Analytical Chemistry T
Middle level IM-MS and CIU experiments for improved therapeutic immunoglobulin subclass fingerprinting ACS Paragon Plus Environment Analytical Chemistry T. Botzanowski, O. Hernandez-Alba, M. Malissard, E. Wagner-Rousset, E. Desligniere, O. Colas, F. Haeuw J., A. Beck, S. Cianferani To cite this version: T. Botzanowski, O. Hernandez-Alba, M. Malissard, E. Wagner-Rousset, E. Desligniere, et al.. Middle level IM-MS and CIU experiments for improved therapeutic immunoglobulin subclass fingerprinting ACS Paragon Plus Environment Analytical Chemistry. Analytical Chemistry, American Chemical Society, 2020, 92 (13), pp.8827-8835. 10.1021/acs.analchem.0c00293. hal-02960844 HAL Id: hal-02960844 https://hal.archives-ouvertes.fr/hal-02960844 Submitted on 8 Oct 2020 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. Analytical Chemistry This document is confidential and is proprietary to the American Chemical Society and its authors. Do not copy or disclose without written permission. If you have received this item in error, notify the sender and delete all copies. -

Submission of Eculizumab for NMOSD to PBAC Meeting November 2020
PBAC Secretariat MDP 952 Department of Health and Ageing GPO Box 9848 Canberra ACT 2601 7 October 2020 Re: Submission of eculizumab for NMOSD to PBAC meeting November 2020 This is a joint submission to the Pharmaceutical Benefits Advisory Committee (PBAC) in relation to eculizumab (Soliris) for neuromyelitis optica spectrum disorder (NMOSD) from MS Research Australia, the Centre for Community-Driven Research and MS Australia. • MS Research Australia is the largest national not-for-profit organisation dedicated to funding MS discoveries and coordinating MS research in Australia. • The Centre for Community-Driven Research is a non-profit organisation with expertise in gathering patient experience and expectations data. • MS Australia is the national voice for people with multiple sclerosis. MS Australia works in advocacy and communications and collaborates with their stakeholders to benefit thousands of people affected by MS across the country. MS Research Australia and MS Australia are writing to support the inclusion of eculizumab on the Pharmaceutical Benefits Scheme (PBS) for people with NMOSD. The Centre for Community-Driven Research is keen to inform the PBAC about the experience of people with NMOSD and their expectations of new treatments. The NMOSD community in Australia is not represented by a national peak body and as NMOSD and MS have some similarities, we are proud to advocate on behalf of those living with NMOSD. One area we are all particularly passionate about is the provision of affordable and accessible treatments that can improve the lives of people with NMOSD. About NMOSD NMOSD is a recently defined inflammatory disorder of the central nervous system (CNS) that was previously either misdiagnosed as MS or identified as Devic’s disease. -
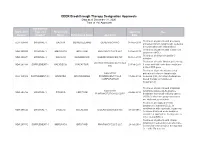
CDER Breakthrough Therapy Designation Approvals Data As of December 31, 2020 Total of 190 Approvals
CDER Breakthrough Therapy Designation Approvals Data as of December 31, 2020 Total of 190 Approvals Submission Application Type and Proprietary Approval Use Number Number Name Established Name Applicant Date Treatment of patients with previously BLA 125486 ORIGINAL-1 GAZYVA OBINUTUZUMAB GENENTECH INC 01-Nov-2013 untreated chronic lymphocytic leukemia in combination with chlorambucil Treatment of patients with mantle cell NDA 205552 ORIGINAL-1 IMBRUVICA IBRUTINIB PHARMACYCLICS LLC 13-Nov-2013 lymphoma (MCL) Treatment of chronic hepatitis C NDA 204671 ORIGINAL-1 SOVALDI SOFOSBUVIR GILEAD SCIENCES INC 06-Dec-2013 infection Treatment of cystic fibrosis patients age VERTEX PHARMACEUTICALS NDA 203188 SUPPLEMENT-4 KALYDECO IVACAFTOR 21-Feb-2014 6 years and older who have mutations INC in the CFTR gene Treatment of previously untreated NOVARTIS patients with chronic lymphocytic BLA 125326 SUPPLEMENT-60 ARZERRA OFATUMUMAB PHARMACEUTICALS 17-Apr-2014 leukemia (CLL) for whom fludarabine- CORPORATION based therapy is considered inappropriate Treatment of patients with anaplastic NOVARTIS lymphoma kinase (ALK)-positive NDA 205755 ORIGINAL-1 ZYKADIA CERITINIB 29-Apr-2014 PHARMACEUTICALS CORP metastatic non-small cell lung cancer (NSCLC) who have progressed on or are intolerant to crizotinib Treatment of relapsed chronic lymphocytic leukemia (CLL), in combination with rituximab, in patients NDA 206545 ORIGINAL-1 ZYDELIG IDELALISIB GILEAD SCIENCES INC 23-Jul-2014 for whom rituximab alone would be considered appropriate therapy due to other co-morbidities -

Immune Checkpoint Inhibitor Therapy-Associated Encephalitis: a Case Series and Review of the Literature
Original article | Published 23 November 2020 | doi:10.4414/smw.2020.20377 Cite this as: Swiss Med Wkly. 2020;150:w20377 Immune checkpoint inhibitor therapy-associated encephalitis: a case series and review of the literature Stuby Johanna, Herren Thomasb, Schwegler Naumburger Guidoc, Papet Claudiad, Rudiger Alaina a Internal Medicine, Department II, Limmattal Hospital Zurich, Schlieren, Switzerland b Cardiology, Department II, Limmattal Hospital Zurich, Schlieren, Switzerland c Neurology, Department II, Limmattal Hospital Zurich, Schlieren, Switzerland d Oncology/Haematology, Department II, Limmattal Hospital Zurich, Schlieren, Switzerland Summary EEG should be performed. Therapy with intravenous corti- costeroids is recommended. Steroid unresponsiveness is BACKGROUND: Immune checkpoint inhibitors (ICIs) can rare and should lead to a review of the diagnosis. Alterna- cause a wide spectrum of immune-related adverse events, tive treatment options are IVIG, plasma exchange therapy including encephalitis. To date, no prospective ran- and rituximab. domised controlled trials examining the patient charac- teristics, treatment and outcomes of ICI-associated en- Keywords: immune checkpoint inhibitor, nivolumab, pem- cephalitis have been published. Therefore, we aimed to brolizumab, ipilimumab, encephalitis review case reports and to provide recommendations for the management of ICI-associated encephalitis. Introduction METHODS: A literature search using Google Scholar and Immune checkpoint inhibitors (ICIs) re-establish the anti- PubMed was performed in December 2019. Published tumour activity of T-lymphocytes by blocking immune in- case reports and case series of ICI-associated encephali- hibitory receptors such as programmed cell death protein 1 tis were reviewed, and a case series from the Limmattal (PD-1, e.g., nivolumab, pembrolizumab and lambrolizum- Hospital in Schlieren, Switzerland was added. -
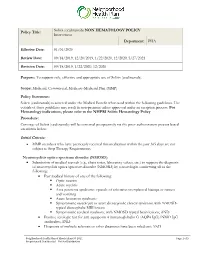

Soliris (Eculizumab) NON HEMATOLOGY POLICY Intravenous Department: PHA
Policy Title: Soliris (eculizumab) NON HEMATOLOGY POLICY Intravenous Department: PHA Effective Date: 01/01/2020 Review Date: 09/18/2019, 12/20/2019, 1/22/2020, 12/2020, 5/27/2021 Revision Date: 09/18/2019, 1/22/2020, 12/2020 Purpose: To support safe, effective and appropriate use of Soliris (eculizumab). Scope: Medicaid, Commercial, Medicare-Medicaid Plan (MMP) Policy Statement: Soliris (eculizumab) is covered under the Medical Benefit when used within the following guidelines. Use outside of these guidelines may result in non-payment unless approved under an exception process. For Hematology indications, please refer to the NHPRI Soliris Hematology Policy Procedure: Coverage of Soliris (eculizumab) will be reviewed prospectively via the prior authorization process based on criteria below. Initial Criteria: MMP members who have previously received this medication within the past 365 days are not subject to Step Therapy Requirements. Neuromyelitis optica spectrum disorder (NMOSD) Submission of medical records (e.g., chart notes, laboratory values, etc.) to support the diagnosis of neuromyelitis optica spectrum disorder (NMOSD) by a neurologist confirming all of the following: Past medical history of one of the following: . Optic neuritis . Acute myelitis . Area postrema syndrome: episode of otherwise unexplained hiccups or nausea and vomiting . Acute brainstem syndrome . Symptomatic narcolepsy or acute diencephalic clinical syndrome with NMOSD- typical diencephalic MRI lesions . Symptomatic cerebral syndrome with NMOSD-typical brain -

The Antitumor Immunity of Ipilimumab: (T-Cell) Memories to Last a Lifetime?
Published OnlineFirst February 15, 2012; DOI: 10.1158/1078-0432.CCR-12-0409 Clinical Cancer CCR Translations Research Commentary on Prieto et al., p. 2039 The Antitumor Immunity of Ipilimumab: (T-cell) Memories to Last a Lifetime? Michael A. Postow1,3, Margaret K. Callahan1,3, and Jedd D. Wolchok1,2,3,4 Ipilimumab has shown an overall survival benefit in 2 randomized phase III studies. A minority of patients achieve long-term disease control, highlighting the potential of this immunotherapeutic approach. In ongoing efforts, investigators are continuing to characterize these patients’ unique clinical courses and correlate their responses with underlying mechanisms of antitumor immunity. Clin Cancer Res; 18(7); 1821–3. Ó2012 AACR. In this issue of Clinical Cancer Research, Prieto and col- Prieto and colleagues have assembled findings from the leagues (1) report long-term follow-up data for 177 patients largest reported long-term clinical experience with ipilimu- treated with ipilimumab in some of the earliest trials in its mab. They provide updated data from 3 previously development. Their results underscore the remarkable, published studies that examined ipilimumab with gp100 durable benefits a subset of patients with melanoma achieve vaccination [protocol 1 (6)]; ipilimumab with concomitant from ipilimumab, hint at the promise of combining ipili- IL-2 [protocol 2 (7)]; and ipilimumab via a strategy of mumab with interleukin 2 (IL-2), and raise the provocative intrapatient dose escalation (Æ gp100) until occurrence of question of whether, in some patients, metastatic melano- response or intolerable side effects [protocol 3 (8)]. The ma can be cured. authors evaluate a total of 177 patients treated with ipili- Ipilimumab (Yervoy; Bristol-Myers Squibb) is a fully mumab, with a median follow-up of 92, 84, and 71 months, human monoclonal antibody that blocks cytotoxic respectively. -

Ipilimumab for the Treatment of Metastatic Melanoma Hansoo Kim*, Samantha Comey, Karl Hausler and Greg Cook
Kim et al. Journal of Pharmaceutical Policy and Practice (2018) 11:4 DOI 10.1186/s40545-018-0131-4 RESEARCH Open Access A real world example of coverage with evidence development in Australia - ipilimumab for the treatment of metastatic melanoma Hansoo Kim*, Samantha Comey, Karl Hausler and Greg Cook Abstract Background: Australian Government subsidisation of ipilimumab for the treatment of patients with metastatic melanoma was conditional on the sponsor entering a ‘managed entry scheme’ to assess the 2-year overall survival rate in metastatic melanoma patients who received ipilimumab in the first year of Pharmaceutical Benefits Scheme listing. Methods: All unresectable stage IIIc / IV metastatic melanoma patients treated with at least one dose of ipilimumab therapy in Australia from the PBS listing date to a time point 12 months later (i.e. from 1-Aug-2013 to 31-Jul-2014) were invited to participate. Overall survival at 2 years post treatment initiation was measured, with Cox regression analysis used to examine the relationship between survival and patient baseline characteristics. Results: The evaluable population (910 patients) was on average 63.3 years old, male (70.1%) and treated in a public hospital (64.4%) in an urban area (76.5%). The majority of patients were treatment naïve (63.3%), did not have brain metastases (71.1%), and were classified as ECOG performance status 0 or 1 (90.4%). The 2 year overall survival rate was conservatively calculated to be at least 23.9% and potentially as high as 34.2%. A significant difference in overall survival at 2 years was demonstrated across the categories of ECOG performance status (p < 0.0001), M-status (p = 0.0005) and treatment status (p = 0.0114).