The Enigmatic Sixth Wave of the Electrocardiogram: the U Wave
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Computational Diagnostic Techniques for Electrocardiogram Signal Analysis
sensors Review Computational Diagnostic Techniques for Electrocardiogram Signal Analysis Liping Xie * , Zilong Li, Yihan Zhou, Yiliu He and Jiaxin Zhu College of Medicine and Biological Information Engineering, Northeastern University, Shenyang 110169, China; [email protected] (Z.L.); [email protected] (Y.Z.); [email protected] (Y.H.); [email protected] (J.Z.) * Correspondence: [email protected] Received: 8 September 2020; Accepted: 4 November 2020; Published: 5 November 2020 Abstract: Cardiovascular diseases (CVDs), including asymptomatic myocardial ischemia, angina, myocardial infarction, and ischemic heart failure, are the leading cause of death globally. Early detection and treatment of CVDs significantly contribute to the prevention or delay of cardiovascular death. Electrocardiogram (ECG) records the electrical impulses generated by heart muscles, which reflect regular or irregular beating activity. Computer-aided techniques provide fast and accurate tools to identify CVDs using a patient’s ECG signal, which have achieved great success in recent years. Latest computational diagnostic techniques based on ECG signals for estimating CVDs conditions are summarized here. The procedure of ECG signals analysis is discussed in several subsections, including data preprocessing, feature engineering, classification, and application. In particular, the End-to-End models integrate feature extraction and classification into learning algorithms, which not only greatly simplifies the process of data analysis, but also shows excellent accuracy and robustness. Portable devices enable users to monitor their cardiovascular status at any time, bringing new scenarios as well as challenges to the application of ECG algorithms. Computational diagnostic techniques for ECG signal analysis show great potential for helping health care professionals, and their application in daily life benefits both patients and sub-healthy people. -

Young Adults. Look for ST Elevation, Tall QRS Voltage, "Fishhook" Deformity at the J Point, and Prominent T Waves
EKG Abnormalities I. Early repolarization abnormality: A. A normal variant. Early repolarization is most often seen in healthy young adults. Look for ST elevation, tall QRS voltage, "fishhook" deformity at the J point, and prominent T waves. ST segment elevation is maximal in leads with tallest R waves. Note high take off of the ST segment in leads V4-6; the ST elevation in V2-3 is generally seen in most normal ECG's; the ST elevation in V2- 6 is concave upwards, another characteristic of this normal variant. Characteristics’ of early repolarization • notching or slurring of the terminal portion of the QRS wave • symmetric concordant T waves of large amplitude • relative temporal stability • most commonly presents in the precordial leads but often associated with it is less pronounced ST segment elevation in the limb leads To differentiate from anterior MI • the initial part of the ST segment is usually flat or convex upward in AMI • reciprocal ST depression may be present in AMI but not in early repolarization • ST segments in early repolarization are usually <2 mm (but have been reported up to 4 mm) To differentiate from pericarditis • the ST changes are more widespread in pericarditis • the T wave is normal in pericarditis • the ratio of the degree of ST elevation (measured using the PR segment as the baseline) to the height of the T wave is greater than 0.25 in V6 in pericarditis. 1 II. Acute Pericarditis: Stage 1 Pericarditis Changes A. Timing 1. Onset: Day 2-3 2. Duration: Up to 2 weeks B. Findings 1. -

Interpreting CVP Waveforms Summary EK
INTERPRETING CENTRAL VENOUS PRESSURE WAVEFORMS IN TERPRETING CEN TRAL VEN OUS PRESSURE W AVEFORMS INTRODUCTION A central venous pressure waveform provides important information about the hemodynamic state of the patient and compliance of the syste m. - CENTRAL VEN OUS PRESSURE (CVP) W AVEFORMS • Measures pressure in the central venous circulation • Obtained by using a central venous catheter ideally placed at the junction of the superior vena cava (SVC) and the right atrium • Depends on: 1. Compliance of the cardiovascular system 2. Overall volume status Figure 1: Central venou s catheter placement at the SV C-RA junction INTERPRETING CVP W AVEFORMS Remember that the waveform represents atrial pressure which is the relationship between atrial compliance and volume. One CVP Waveform represents one complete beat of the heart. • a-wave: atrial contraction • Corresponds with timing of P wave on ECG • Noncompliant right atrium: = large a-wave • c-wave: movement of the tric uspid valve into the right atrium • Corresponds with timing of R wave on ECG • Transient decrease in atrial compliance/increase in atrial pressure • c-wave and a-wave can be difficult to differentiate when patient is ta tachycardic • x-descent: atrial relaxation • Corresponds with timing of QRS complex on ECG Figure 2: The different parts of a central venous • Tricuspid valve descends towards the apex of the right ventricle pressure waveform causing a decrease in right atrial pressure • v-wave: atrial filling • Corresponds with timing of T wave on ECG • A large v-wave may indicate tricuspid regurgitation QRS • If right atrium is very compliant, tricuspid regurgitation is possible complex without generation of large v-wave • y-descent: atrial emptying • Corresponds with timing just prior to P wave on ECG P wave T wave Figure 3: ECG showing timing of CVP waveform components This document is meant to be used as an educational resource for physicians and other healthcare professionals. -

Ventricular Repolarization Components on the Electrocardiogram Cellular Basis and Clinical Significance Gan-Xin Yan, MD, PHD, Ramarao S
View metadata, citation and similar papers at core.ac.uk brought to you by CORE Journal of the American College of Cardiology providedVol. by Elsevier 42, No. - 3,Publisher 2003 Connector © 2003 by the American College of Cardiology Foundation ISSN 0735-1097/03/$30.00 Published by Elsevier Inc. doi:10.1016/S0735-1097(03)00713-7 STATE-OF-THE-ART PAPER Ventricular Repolarization Components on the Electrocardiogram Cellular Basis and Clinical Significance Gan-Xin Yan, MD, PHD, Ramarao S. Lankipalli, MD, James F. Burke, MD, FACC, Simone Musco, MD, Peter R. Kowey, MD, FACC Wynnewood, Pennsylvania Ventricular repolarization components on the surface electrocardiogram (ECG) include J (Osborn) waves, ST-segments, and T- and U-waves, which dynamically change in morphol- ogy under various pathophysiologic conditions and play an important role in the development of ventricular arrhythmias. Our primary objective in this review is to identify the ionic and cellular basis for ventricular repolarization components on the body surface ECG under normal and pathologic conditions, including a discussion of their clinical significance. A specific attempt to combine typical clinical ECG tracings with transmembrane electrical recordings is made to illustrate their logical linkage. A transmural voltage gradient during initial ventricular repolarization, which results from the presence of a prominent transient ϩ outward K current (Ito)-mediated action potential (AP) notch in the epicardium, but not endocardium, manifests as a J-wave on the ECG. The J-wave is associated with the early repolarization syndrome and Brugada syndrome. ST-segment elevation, as seen in Brugada syndrome and acute myocardial ischemia, cannot be fully explained by using the classic concept of an “injury current” that flows from injured to uninjured myocardium. -

Determinants of Myocardial Lactate Production During Acetylcholine
ORIGINAL RESEARCH Determinants of Myocardial Lactate Production During Acetylcholine Provocation Test in Patients With Coronary Spasm Koichi Kaikita, MD, PhD; Masanobu Ishii, MD; Koji Sato, MD, PhD; Masafumi Nakayama, MD, PhD; Yuichiro Arima, MD, PhD; Tomoko Tanaka, MD, PhD; Koichi Sugamura, MD, PhD; Kenji Sakamoto, MD, PhD; Yasuhiro Izumiya, MD, PhD; Eiichiro Yamamoto, MD, PhD; Kenichi Tsujita, MD, PhD; Megumi Yamamuro, MD, PhD; Sunao Kojima, MD, PhD; Hirofumi Soejima, MD, PhD; Seiji Hokimoto, MD, PhD; Kunihiko Matsui, MD, MPH; Hisao Ogawa, MD, PhD Background-—Myocardial lactate production in the coronary circulation during acetylcholine (ACh)-provocation test (abbreviated as lactate production) provides supporting evidence for coronary spasm–induced myocardial ischemia. The purpose of this study was to examine the clinical features, predictive factors, and prognosis of patients with coronary vasospastic angina (VSA) and lactate production. Methods and Results-—We examined all 712 patients who underwent both myocardial lactate measurement during ACh- provocation test in the left coronary artery and genetic screening test of a –786T/C polymorphism in the 50-flanking region of the endothelial nitric oxide synthase (eNOS) gene between January 1991 and December 2010. Lactate production was observed in 252 of the 712 patients and in 219 of 356 VSA patients diagnosed by ACh-provocation test. Compared with lactate production– negative VSA patients, the lactate production–positive counterparts were more likely to be nonsmoker female diabetics with – 786T/C eNOS polymorphism (61% vs 31%, P<0.001, 62% vs 34%, P<0.001, 24% vs 14%, P=0.016, and 25% vs 15%, P=0.018, respectively). Multivariable logistic regression analysis identified female sex, diabetes mellitus, and –786T/C eNOS polymorphism to correlate with lactate production (odds ratio 3.51, 95% CI 2.16 to 5.70, P<0.001; odds ratio 2.53, 95% CI 1.38 to 4.65, P=0.003; and odds ratio 1.85, 95% CI 1.02 to 3.35, P=0.044, respectively). -

Tively Assess Myocardial Function: New Hypothesis and Validation Experiment Regarding the U Wave
Journal of ISSN:2378-6914 Heart and Cardiology OPEN ACCESS Research Article DOI: 10.15436/2378-6914.20.2813 Changing Electrocardiogram Waveforms to Quantita- tively Assess Myocardial function: New Hypothesis and Validation Experiment regarding the U Wave Kenneth Tsan He1*, Helena Ai He2 1Princeton International School of Mathematics and Science, 11th grade student, 19 Lambert Drive, Princeton 2Princeton International School of Mathematics and Science, 10th grade student, 19 Lambert Drive, Princeton *Corresponding author: Kenneth Tsan He, Princeton International School of Mathematics and Science, 11th grade student, 19 Lambert Drive, Princeton, NJ, Tel: 08540; 1-732-705-0282; Email: [email protected] Abstract A hypothesis regarding the U wave is proposed, where the collision of the heart apex and chest wall causes delayed repolar- ization of some myocardial cells due to compression and deformation, leading to the presence of the U wave on ECG. Under normal conditions, the stronger the myocardial contractility, the greater the mass of the heart, the closer the distance to the chest wall, the more intense the apex beat, the more cells deformed and repolarization delayed, and the longer the delay time. To test the hypothesis, 41 high school student volunteers participated in a clinical trial. The results showed that when the position was changed from the supine position to the left lateral position, the U wave increased significantly (0.24±0.095×0.1 mv, a=99%), the T wave significantly decreased (-1.3±0.74×0.1 mv, a=99%), the time difference between the two peaks significantly increased (0.38±0.12×40 ms, a= 99%), indicating a strong co-rrelation between those three values ( r= 0.87 and 0.39). -

The Heart the Pulse and the ECG Booklet.Indd
AF A ® www.afa.org.uk The heart, the pulse and the electrocardiograph Providing information, support and access to established, new or innovative treatments for atrial fi brillation www.afa.org.uk Registered Charity No. 1122442 Glossary Arrhythmia Heart rhythm disorder Contents Arrhythmia Nurse Specialist A nurse who is Glossary trained in heart rhythm disorders The heart Atrial Fibrillation (AF) An irregular heart rhythm due to a rapid, disorganised electrical disturbance of The pulse the heart’s upper chambers (the atria) How to take a pulse Atrial Flutter (Afl ) A rhythm disorder of a more organised electrical disturbance in the heart’s upper The electrocardiograph chambers. The heart rhythm may be either regular (ECG) or irregular Bradycardia A rhythm disorder characterised by a slow heart rate of less than 60 beats per minute Cardiologist A doctor who specialises in the diagnosis and treatment of patients with heart conditions Echocardiogram An image of the heart using echocardiography or soundwave-based technology. An echocardiogram (echo) shows a three dimensional shot of the heart Electrocardiograph (ECG) A 2D graphic of the heart’s electrical activity. An ECG is taken from electrodes on the skin surface Heart Failure The inability (failure) of the heart to pump suffi cient oxygenated blood around the body to meet physiological requirements Sinus Rhythm Normal behaviour of the heart Syncope Fainting/passing out from a temporary lack of oxygen going to certain areas of the brain Tachycardia A rhythm disorder characterised by a rapid heart rate of more than 100 beats per minute 2 The heart The heart Structurally, the heart consists of two sides, a right and normal and a left. -

Basic Cardiac Rhythms – Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives
Basic Cardiac Rhythms – Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives ▪ Describe the normal cardiac anatomy and physiology and normal electrical conduction through the heart. ▪ Identify and relate waveforms to the cardiac cycle. Cardiac Anatomy ▪ 2 upper chambers ▪ Right and left atria ▪ 2 lower chambers ▪ Right and left ventricle ▪ 2 Atrioventricular valves (Mitral & Tricuspid) ▪ Open with ventricular diastole ▪ Close with ventricular systole ▪ 2 Semilunar Valves (Aortic & Pulmonic) ▪ Open with ventricular systole ▪ Open with ventricular diastole The Cardiovascular System ▪ Pulmonary Circulation ▪ Unoxygenated – right side of the heart ▪ Systemic Circulation ▪ Oxygenated – left side of the heart Anatomy Coronary Arteries How The Heart Works Anatomy Coronary Arteries ▪ 2 major vessels of the coronary circulation ▪ Left main coronary artery ▪ Left anterior descending and circumflex branches ▪ Right main coronary artery ▪ The left and right coronary arteries originate at the base of the aorta from openings called the coronary ostia behind the aortic valve leaflets. Physiology Blood Flow Unoxygenated blood flows from inferior and superior vena cava Right Atrium Tricuspid Valve Right Ventricle Pulmonic Valve Lungs Through Pulmonary system Physiology Blood Flow Oxygenated blood flows from the pulmonary veins Left Atrium Mitral Valve Left Ventricle Aortic Valve Systemic Circulation ▪ Blood Flow Through The Heart ▪ Cardiology Rap Physiology ▪ Cardiac cycle ▪ Represents the actual time sequence between -
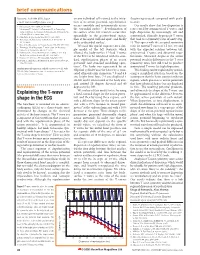
Explaining the T-Wave Shape in The
brief communications Inuyama, Aichi 484-8506, Japan on any individual cell is timed to the initia- (beginning-to-peak compared with peak- e-mail: [email protected] tion of its action potential, repolarization to-end). 1. Matsuzawa, T. Nature 315, 57–59 (1985). occurs smoothly and systematically across Our results show that low dispersion is 5,6 2. Matsuzawa, T., Itakura, S. & Tomonaga, M. in Primatology the epicardial surface . Repolarization of represented by asymmetrical T waves, and Today (eds Ehara, A., Kumura, T., Takenaka, O. & Iwamoto, M.) the surface of the left ventricle occurs first high dispersion by increasingly tall and 317–320 (Elsevier, Amsterdam, 1991). epicardially in the postero-basal region, symmetrical, clinically hyperacute T waves 3. Murofushi, K. Jpn. Psychol. Res. 39, 140–153 (1997). 6 4. Tomonaga, M., Matsuzawa, T. & Itakura, S. Primate Res. 9, then at the septal wall and apex , and finally that tend to a symmetry ratio of unity (Fig. 67–77 (1993). at the endocardial surface7. 1). This agrees with the accepted symmetry 5. Biro, D. & Matsuzawa, T. J. Comp. Psychol. 113, 178–185 (1999). We used this spatial sequence on a sim- ratio for normal T waves of 1.5 (ref. 10) and 6. Tomonaga, M. & Matsuzawa, T. Anim. Cogn. (in the press). 7. Miller, G. A. Psychol. Rev. 63, 81–97 (1956). ple model of the left ventricle which with the expected relation between tall, 8. Rumbaugh, D., Savage-Rumbaugh, E. S. & Hegel, M. J. Exp. allowed the body-surface 12-lead T waves symmetrical T waves and abnormal repo- Psychol. -

Effect of Intravenous Adrenaline on Electrocardiogram, Blood Pressure, and Serum Potassium
Br Heart J: first published as 10.1136/hrt.49.1.90 on 1 January 1983. Downloaded from Br Heart J 1983; 49: 90-3 Effect of intravenous adrenaline on electrocardiogram, blood pressure, and serum potassium A D STRUTHERS, J L REID, R WHITESMITH, J C RODGER From the University Department ofMateria Medica, and Department ofBiochemistry, StobhiU General Hospital, Glasgow, and Medical Unit, Monklands and District General Hospital, Airdrie, Lanarkshire SUMMARY Increased catecholamines after myocardial infarction may contribute to the development ofarrhythmias. We have infused adrenaline intravenously in nine normal volunteers to levels similar to those seen after myocardial infarction. Adrenaline caused an increase in systolic blood pressure, a decrease in diastolic blood pressure, and an increase in heart rate. Adrenaline also produced a decrease in T wave amplitude and an increase in the QTc interval. The serum potassium fell dramatically during the adrenaline infusion from a control value of 4*06 mmot/l to 3-22 mmol/l. Hypokalaemia after myocardial infarction is associated with an increased incidence of ventricular arrhythmias. Thus, circulating adrenaline may increase the frequency of arrhythmias both directly via changes in ventricular repolarisation and indirectly via adrenaline induced hypokalaemia. Hypokalaemia is not uncommonly observed in the All subjects gave their informed consent to the acute phase of myocardial infarctionl 2 when it is investigation which had the approval of the hospital's associated with serious ventricular arrhythmias.3 We research and ethical committee. have found that in this circumstance hypokalaemia is Subjects were investigated in the morning after a http://heart.bmj.com/ transient, it resolves without potassium supplements, standard light breakfast. -

Dysrhythmias
CARDIOVASCULAR DISORDERS DYSRHYTHMIAS I. BASIC PRINCIPLES OF CARDIAC CONDUCTION DISTURBANCES A. Standard ECG and rhythm strips 1. Recordings are obtained at a paper speed of 25 mm/sec. 2. The vertical axis measures distance; the smallest divisions are 1 mm ×1 mm. 3. The horizontal axis measures time; each small division is 0.04 sec/mm. B. Normal morphology Courtesy of Dr. Michael McCrea 1. P wave = atrial depolarization a. Upright in leads I, II, III, aVL, and aVF; inverted in lead aVR b. Measures <0.10 seconds wide and <3 mm high c. Normal PR interval is 0.12–0.20 seconds. 2. QRS complex = ventricular depolarization a. Measures 0.06-0.10 seconds wide b. Q wave (1) <0.04 seconds wide and <3 mm deep (2) Abnormal if it is >3 mm deep or >1/3 of the QRS complex. c. R wave ≤7.5 mm high 3. QT interval varies with rate and sex but is usually 0.33–0.42 seconds; at normal heart rates, it is normally <1/2 the preceding RR interval. 4. T wave = ventricular repolarization a. Upright in leads I, II, V3–V6; inverted in aVR b. Slightly rounded and asymmetric in configuration c. Measures ≤5 mm high in limb leads and ≤10 mm high in the chest leads 5. U wave = a ventricular afterpotential a. Any deflection after the T wave (usually low voltage) b. Same polarity as the T wave c. Most easily detected in lead V3 d. Can be a normal component of the ECG e. Prominent U waves may indicate one of the following: (1) Hypokalemia (<3 mEq/L) (2) Hypercalcemia (3) Therapy with digitalis, phenothiazines, quinidine, epinephrine, inotropic agents, or amiodarone (4) Thyrotoxicosis f. -

"U" Wave Kenneth M Eyer* 369 Old Sawmill Road, Sagle, Idaho 83860, USA Letter to the Editor U Wave
Journal of Integrative Cardiology Letter to the Editor ISSN: 2058-3702 The etiology of the ECG "U" wave Kenneth M Eyer* 369 Old Sawmill Road, Sagle, Idaho 83860, USA Letter to the Editor U wave. What followed were years of watching ECG's and the U waves to see if there was ever an exception to this rule. When I was a Cardiology Fellow in the 1950's at the University of Washington, I was curious why the U wave had been observed for 100 Post extra-systolic pulsus alternans is a well-known sign of impaired years but had never been explained. Because it looked like a miniature left ventricular function. I reasoned that the ECG should also show U T wave researchers had assumed it had to be late repolarization wave alternans and I watched for it. One night on the coronary care unit the resident showed me a rhythm strip on a patient and there it somewhere in the heart. But search as they may, they couldn't find it. was. I took members of the house staff to the patient's bedside and we I looked at the large book "The U Wave" by Katz and found the each put a finger on a pulse. A PVC came along and we each noticed most help on the first page. They are largest in the chest leads of transient pulsus alternans. young males and always follow the aortic second sound. I attached Later, six of my patients who had been in heart failure volunteered a phonocardiogram and ECG leads to myself and varied my stroke to be monitored in our Heart Center.