PERFORATED PEPTIC ULCER. Patient Usually Experiences
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Perforated Ulcers Shaleen Sathe, MS4 Christina Lebedis, MD CASE HISTORY
Perforated Ulcers Shaleen Sathe, MS4 Christina LeBedis, MD CASE HISTORY 54-year-old male with known history of hypertension presents with 2 days of acute onset abdominal pain, nausea, vomiting, and diarrhea, with periumbilical tenderness and abdominal distention on exam, without guarding or rebound tenderness. Labs, including CBC, CMP, and lipase, were unremarkable in the emergency department. Radiograph Perforated Duodenal Ulcer Radiograph of the chest in the AP projection shows large amount of free air under diaphragm (blue arrows), suggestive of intraperitoneal hollow viscus perforation. CT Perforated Duodenal Ulcer CT of the abdomen in the axial projection (I+, O-), at the level of the inferior liver edge, shows large amount of intraperitoneal free air (blue arrows) in lung window (b), and submucosal edema in the gastric antrum and duodenal bulb (red arrows), suggestive of a diagnosis of perforated bowel, most likely in the region of the duodenum. US Perforated Gastric Ulcer US of the abdomen shows perihepatic fluid (blue arrow) and free fluid in the right paracolic gutter (not shown), concerning for intraperitoneal pathology. Radiograph Perforated Gastric Ulcer Supine radiograph of the abdomen shows multiple air- filled dilated loops of large bowel, with air lucencies on both sides of the sigmoid colon wall (green arrows), consistent with Rigler sign and perforation. CT Perforated Gastric Ulcer CT of the abdomen in the axial (a) and sagittal (b) projections (I+, O-) shows diffuse wall thickening of the gastric body and antrum (green arrows) with an ulcerating lesion along the posterior wall of the stomach (red arrows), and free air tracking adjacent to the stomach (blue arrow), concerning for gastric ulcer perforation. -

Diagnosis and Treatment of Perianal Crohn Disease: NASPGHAN Clinical Report and Consensus Statement
CLINICAL REPORT Diagnosis and Treatment of Perianal Crohn Disease: NASPGHAN Clinical Report and Consensus Statement ÃEdwin F. de Zoeten, zBrad A. Pasternak, §Peter Mattei, ÃRobert E. Kramer, and yHoward A. Kader ABSTRACT disease. The first description connecting regional enteritis with Inflammatory bowel disease is a chronic inflammatory disorder of the perianal disease was by Bissell et al in 1934 (2), and since that time gastrointestinal tract that includes both Crohn disease (CD) and ulcerative perianal disease has become a recognized entity and an important colitis. Abdominal pain, rectal bleeding, diarrhea, and weight loss consideration in the diagnosis and treatment of CD. Perianal characterize both CD and ulcerative colitis. The incidence of IBD in the Crohn disease (PCD) is defined as inflammation at or near the United States is 70 to 150 cases per 100,000 individuals and, as with other anus, including tags, fissures, fistulae, abscesses, or stenosis. autoimmune diseases, is on the rise. CD can affect any part of the The symptoms of PCD include pain, itching, bleeding, purulent gastrointestinal tract from the mouth to the anus and frequently will include discharge, and incontinence of stool. perianal disease. The first description connecting regional enteritis with perianal disease was by Bissell et al in 1934, and since that time perianal INCIDENCE AND NATURAL HISTORY disease has become a recognized entity and an important consideration in the Limited pediatric data describe the incidence and prevalence diagnosis and treatment of CD. Perianal Crohn disease (PCD) is defined as of PCD. The incidence of PCD in the pediatric age group has been inflammation at or near the anus, including tags, fissures, fistulae, abscesses, estimated to be between 13.6% and 62% (3). -

General Signs and Symptoms of Abdominal Diseases
General signs and symptoms of abdominal diseases Dr. Förhécz Zsolt Semmelweis University 3rd Department of Internal Medicine Faculty of Medicine, 3rd Year 2018/2019 1st Semester • For descriptive purposes, the abdomen is divided by imaginary lines crossing at the umbilicus, forming the right upper, right lower, left upper, and left lower quadrants. • Another system divides the abdomen into nine sections. Terms for three of them are commonly used: epigastric, umbilical, and hypogastric, or suprapubic Common or Concerning Symptoms • Indigestion or anorexia • Nausea, vomiting, or hematemesis • Abdominal pain • Dysphagia and/or odynophagia • Change in bowel function • Constipation or diarrhea • Jaundice “How is your appetite?” • Anorexia, nausea, vomiting in many gastrointestinal disorders; and – also in pregnancy, – diabetic ketoacidosis, – adrenal insufficiency, – hypercalcemia, – uremia, – liver disease, – emotional states, – adverse drug reactions – Induced but without nausea in anorexia/ bulimia. • Anorexia is a loss or lack of appetite. • Some patients may not actually vomit but raise esophageal or gastric contents in the absence of nausea or retching, called regurgitation. – in esophageal narrowing from stricture or cancer; also with incompetent gastroesophageal sphincter • Ask about any vomitus or regurgitated material and inspect it yourself if possible!!!! – What color is it? – What does the vomitus smell like? – How much has there been? – Ask specifically if it contains any blood and try to determine how much? • Fecal odor – in small bowel obstruction – or gastrocolic fistula • Gastric juice is clear or mucoid. Small amounts of yellowish or greenish bile are common and have no special significance. • Brownish or blackish vomitus with a “coffee- grounds” appearance suggests blood altered by gastric acid. -

Emergent Repair of a Perforated Giant Duodenal Ulcer in a Patient with an Unmanaged Ulcer History
Open Access Case Report DOI: 10.7759/cureus.12198 Emergent Repair of a Perforated Giant Duodenal Ulcer in a Patient With an Unmanaged Ulcer History Eli B. Eisman 1, 2 , Nicole C. Jamieson 2 , Rashona A. Moss 3 , Melina M. Henderson 4 , Richard C. Spinale 2 1. College of Osteopathic Medicine, Michigan State University, East Lansing, USA 2. General Surgery, Garden City Hospital, Garden City, USA 3. Internal Medicine, Garden City Hospital, Garden City, USA 4. Obstetrics and Gynecology, Garden City Hospital, Garden City, USA Corresponding author: Eli B. Eisman, [email protected] Abstract Giant duodenal ulcers (GDUs) are full-thickness disruptions of the gastrointestinal epithelium greater than 3cm in diameter. The significant size and disease chronicity lead to deleterious outcomes and high mortality risk if ulcer progression is not halted. While still prevalent in developing countries, GDUs are increasingly rare in industrialized nations. Here, we present the case of an 82-year-old woman with perforated GDU requiring emergent surgical intervention complicated by prior duodenal surgery requiring a previously unreported triple-layered omental patch. Discussion of this technique and novel approaches to GDU repair ensue. Categories: Internal Medicine, Gastroenterology, General Surgery Keywords: complicated peptic ulcer disease, duodenal ulcers, duodenal ulceration, perforated duodenal ulcer, gastrointestinal perforation, chronic ulcer, graham patch repair Introduction Giant duodenal ulcers (GDUs) were first characterized in 1931, though initially difficult to diagnose on barium study due to the mistaken identification of ulcers as deformed duodenal caps [1]. Nussbaum and Schusterman codified GDUs as full-thickness ulcers greater than 2cm, usually involving but not limited to the duodenal bulb [2]. -

Descriptive Study Regarding the Etiological Factors Responsible for Secondary Bacterial Peritonitis in Patients Admitted in a Te
International Journal of Health Sciences and Research Vol.10; Issue: 7; July 2020 Website: www.ijhsr.org Original Research Article ISSN: 2249-9571 Descriptive Study Regarding the Etiological Factors Responsible for Secondary Bacterial Peritonitis in Patients Admitted in a Tertiary Care Hospital in Trans Himalayan Region Raj Kumar1, Rahul Gupta2, Anjali Sharma3, Rajesh Chaudhary4 1MS General Surgery, Civil Hospital Baijnath, Himachal Pradesh 2MD Community Medicine, District Programme Officer, Health and Family Welfare, Himachal Pradesh 3Resident Doctor, Department of Microbiology, DRPGMC Kangra at Tanda, Himachal Pradesh 4MS General Surgery, Civil Hospital Nagrota Bagwan, Himachal Pradesh Corresponding Author: Rahul Gupta ABSTRACT Peritonitis is an inflammation of the peritoneum. Primary peritonitis which is spontaneous bacterial peritonitis, Secondary peritonitis due to infection from intraabdominal source or spillage of its contents and Tertiary peritonitis which is recurrent or reactivation of secondary peritonitis. The present study was aimed to determine the etiology of generalized secondary peritonitis among the patients admitted in Department of General Surgery, Dr RPGMC Kangra at Tanda. This descriptive observational study was conducted in the department of surgery Dr. Rajendra Prasad Government Medical College Kangra at Tanda consisting of patients having acute generalised secondary peritonitis presented in emergency department or Surgery outdoor patient department over a period of one year from December 2016 through November 2017. The most common etiology of generalized secondary peritonitis in our patients was peptic ulcer disease (77.13%) followed by perforated appendicitis (9.8%). Etiological factors of secondary generalised peritonitis have a different pattern in different geographical regions. Peptic ulcer disease remains the commonest etiology of secondary peritonitis in India followed by enteric perforation which is in contrast to the western studies where appendicular and colon perforations are more common. -

Perforated Peptic Ulcer: Different Ethnic, Climatic and Fasting Risk Factors for Morbidity in Al-Ain Medical District, United Arab Emirates
Original Article Perforated Peptic Ulcer: Different Ethnic, Climatic and Fasting Risk Factors for Morbidity in Al-Ain Medical District, United Arab Emirates Fawaz Chikh Torab, Mohamed Amer, Fikri M. Abu-Zidan and Frank James Branicki, Department of Surgery, Faculty of Medicine & Health Sciences, UAE University, UAE. AIM: To evaluate risk factors, morbidity and mortality rates of perforated peptic ulcer (PPU) and to inves- tigate factors affecting postoperative complications of PPU. BACKGROUND: The incidence of PPU has remained constant, simple closure with omental patch repair being the mainstay of treatment. PATIENTS AND METHODS: One hundred and nineteen patients admitted to Al-Ain Hospital with PPU between January 2000 and March 2004 was studied retrospectively; two with deficient data were excluded from the analysis. Logistic regression was used to define factors affecting postoperative complications. RESULTS: The mean age of patients was 35.3 years (range, 20–65). 45.7% of patients were Bangladeshi, and 85.3% originated from the Indian subcontinent. One patient, subsequently found to have a perfo- rated gastric cancer, died. In 116 patients, 26 complications were recorded in 20 patients (17.2%). Common risk factors for perforation were smoking, history of peptic ulcer disease (PUD) and use of non-steroidal anti-inflammatory drugs (NSAIDs). A significantly increased risk of perforation was evident during the daytime fasting month of Ramadan. An increase in the acute physiology and chronic health evaluation (APACHE) II score (p = 0.047) and a reduced white blood cell count (0.04) were highly significant for the prediction of postoperative complications. CONCLUSION: Patients with dyspeptic symptoms and a history of previous PUD should be considered for prophylactic treatment to prevent ulcer recurrence during prolonged daytime fasting in Ramadan, especially during the winter time. -

THE ACUTE ABDOMEN Definition Abdominal Pain of Short Duration
THE ACUTE ABDOMEN Definition Abdominal pain of short duration that is usually associated with muscular rigidity, distension and vomiting, and which requires a decision whether an emergent operation is required. Problems and management options History and physical examination are central in the evaluation of the acute abdomen. However, in an ICU patient, these are often limited by sedation, paralysis and mechanical ventilation, and obscured by a protracted, complicated inhospital course. Often an acute abdomen is inferred from unexplained sepsis, hypovolaemia and abdominal distension. The need for prompt diagnosis and early treatment by no means equates with operative management. While it is a truism that correct diagnosis is the essential preliminary to correct treatment, this is probably more so in nonoperative management. On occasions, the need for operation is more obvious than the diagnosis and no delay should be incurred in an attempt to confirm the diagnosis before surgery. Frequently fluid resuscitation and antibiotics are required concurrently with the evaluation process. The approach is to evaluate the ICU patient in the context of the underlying disorder and decide on one of the following options: ∙ Immediate operation (surgery now)– the ‘bleeder’ e.g. ruptured ectopic pregnancy, ruptured abdominal aortic aneurysm (AAA) in the salvageable patient ∙ Emergent operation (surgery tonight)– the ‘septic’ e.g. generalized peritonitis from perforated viscus ∙ Early operation (surgery tomorrow)– the ‘obstructed’, e.g. obstructed colonic cancer ∙ Radiologically guided drainage – e.g. localized abscesses, acalculous cholecystitis, pyonephrosis ∙ Active observation and frequent reevaluation – e.g localized peritoneal signs other than in the RLQ, selected cases of endoscopic perforation . -

Pathophysiology, Diagnosis, and Management of Pediatric Ascites
INVITED REVIEW Pathophysiology, Diagnosis, and Management of Pediatric Ascites ÃMatthew J. Giefer, ÃKaren F. Murray, and yRichard B. Colletti ABSTRACT pressure of mesenteric capillaries is normally about 20 mmHg. The pediatric population has a number of unique considerations related to Intestinal lymph drains from regional lymphatics and ultimately the diagnosis and treatment of ascites. This review summarizes the physio- combines with hepatic lymph in the thoracic duct. Unlike the logic mechanisms for cirrhotic and noncirrhotic ascites and provides a sinusoidal endothelium, the mesenteric capillary membrane is comprehensive list of reported etiologies stratified by the patient’s age. relatively impermeable to albumin; the concentration of protein Characteristic findings on physical examination, diagnostic imaging, and in mesenteric lymph is only about one-fifth that of plasma, so there abdominal paracentesis are also reviewed, with particular attention to those is a significant osmotic gradient that promotes the return of inter- aspects that are unique to children. Medical and surgical treatments of stitial fluid into the capillary. In the normal adult, the flow of lymph ascites are discussed. Both prompt diagnosis and appropriate management of in the thoracic duct is about 800 to 1000 mL/day (3,4). ascites are required to avoid associated morbidity and mortality. Ascites from portal hypertension occurs when hydrostatic Key Words: diagnosis, etiology, management, pathophysiology, pediatric and osmotic pressures within hepatic and mesenteric capillaries ascites produce a net transfer of fluid from blood vessels to lymphatic vessels at a rate that exceeds the drainage capacity of the lym- (JPGN 2011;52: 503–513) phatics. It is not known whether ascitic fluid is formed predomi- nantly in the liver or in the mesentery. -
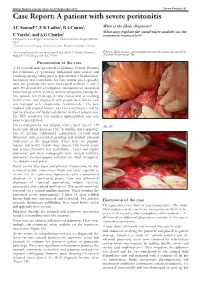
Case Report: a Patient with Severe Peritonitis
Malawi Medical Journal; 25(3): 86-87 September 2013 Severe Peritonitis 86 Case Report: A patient with severe peritonitis J C Samuel1*, E K Ludzu2, B A Cairns1, What is the likely diagnosis? 2 1 What may explain the small white nodules on the C Varela , and A G Charles transverse mesocolon? 1 Department of Surgery, University of North Carolina, Chapel Hill NC USA 2 Department of Surgery, Kamuzu Central Hospital, Lilongwe Malawi Corresponding author: [email protected] 4011 Burnett Womack Figure1. Intraoperative photograph showing the transverse mesolon Bldg CB 7228, Chapel Hill NC 27599 (1a) and the pancreas (1b). Presentation of the case A 42 year-old male presented to Kamuzu Central Hospital for evaluation of worsening abdominal pain, nausea and vomiting starting 3 days prior to presentation. On admission, his history was remarkable for four similar prior episodes over the previous five years that lasted between 3 and 5 days. He denied any constipation, obstipation or associated hematemesis, fevers, chills or urinary symptoms. During the first episode five years ago, he was evaluated at an outlying health centre and diagnosed with peptic ulcer disease and was managed with omeprazole intermittently . His past medical and surgical history was non contributory and he had no allergies and he denied alcohol intake or tobacco use. His HIV serostatus was negative approximately one year prior to presentation. On examination he was afebrile, with a heart rate of 120 (Fig 1B) beats/min, blood pressure 135/78 mmHg and respiratory rate of 22/min. Abdominal examination revealed mild distension with generalized guarding and marked rebound tenderness in the epigastrium. -

Digestive Tract Tuberculosis
World Gastroenterology Organisation Global Guidelines Digestive tract tuberculosis March 2021 WGO Review Team Mohamed Tahiri (Chair, Morocco), K.L. Goh (Co-Chair, Malaysia), Zaigham Abbas (Pakistan), David Epstein (South Africa), Chen Min-Hu (China), Chris Mulder (Netherlands), Amarender Puri (India), Michael Schultz (New Zealand), Anton LeMair (Netherlands) Funding and conflict of interest statement All of the authors have stated that there were no conflicts of interest in relation to their authorship of this paper. Anton LeMair acts as guideline development consultant for WGO. WGO Global Guidelines Digestive tract tuberculosis 2 Contents 1 Introduction .............................................................................................................................. 4 1.1 About WGO cascades ................................................................................................................. 5 1.2 Definitions .................................................................................................................................. 5 1.3 Epidemiology .............................................................................................................................. 6 1.3.1 WHO 2018 global tuberculosis report .............................................................................. 6 1.4 Etiopathogenesis and risk factors .............................................................................................. 7 2 Clinical features ....................................................................................................................... -

Abdominal Examination
Abdominal Examination Introduction Wash hands, Introduce self, ask Patients name & DOB & what they like to be called, Explain examination and get consent Expose and lie patient flat General Inspection Patient: stable, pain/discomfort, jaundice, pallor, muscle wasting/cachexia Around bed: vomit bowels etc Hands Flapping tremor (hepatic encephalopathy) Nails: clubbing (cirrhosis, IBD, coeliacs), leukonychia (hypoalbuminemia in liver cirrhosis), koilonychia (iron deficiency anaemia) Palms: palmar erythema (hyperdynamic circulation due to ↑oestrogen levels in liver disease/ pregnancy), Dupuytren’s contracture (familial, liver disease), fingertip capillary glucose monitoring marks (diabetes) Head Eyes: sclera for jaundice (liver disease), conjunctival pallor (anaemia e.g. bleeding, malabsorption), periorbital xanthelasma (hyperlipidaemia in cholestasis) Mouth: glossitis/stomatitis (iron/ B12 deficiency anaemia), aphthous ulcers (IBD), breath odor (e.g. faeculent in obstruction; ketotic in ketoacidosis; alcohol) Neck and torso Ask patient to sit forwards: Neck: feel for lymphadenopathy from behind – especially Virchow's node (gastric malignancy) Back inspection: spider naevi (>5 significant), skin lesions (immunosuppression) Ask patient to relax back: Chest inspection: spider naevi (>5 significant), gynaecomastia, loss of axillary hair (all due to ↑oestrogen levels in liver disease/ pregnancy) Abdomen Inspection: distension (Fluid, Flatus, Fat, Foetus, Faeces), incisional hernias (ask patient to cough), scars, striae (pregnancy, -

A Rare Case of Ascites
Clinical Medicine 2019 Vol 19, No 2: s73 CLINICAL A r a r e c a s e o f a s c i t e s Authors: S h u a n n S h w a n a , A d n a n U r R a h m a n a n d E l i z a b e t h S l o w i n s k a A i m s most cases depends on whether it is idiopathic or secondary. The mainstay of treatment is corticosteroids; if there is no response, A 69-year-old gentleman presented with a 5-week history of immunosuppressive therapy can be used. Case-series data exist, abdominal distension. He had a past history of diabetes and which show that high-dose corticosteroids like prednisolone are myocardial infarction, and was an ex-smoker with no significant effective in reducing the chronic inflammatory response caused by history of alcohol intake. Examination demonstrated a distended, retroperitoneal fibrosis; however, there is a high rate of recurrence non-tender abdomen with shifting dullness, no organomegaly and once the steroids are withdrawn. Mycophenolate mofetil in addition no signs of chronic liver disease. to corticosteroids has been shown to reduce duration of steroid use without affecting the efficacy and reduces disease recurrence. ■ M e t h o d s Investigations included an ultrasound scan of the abdomen, an Conflict of interest statement ascitic tap, a computed tomography (CT) of the abdomen/pelvis N o n e d e c l a r e d .