Anesthesia Techniques, Sclerotherapy, Duplex-Guided
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The National Drugs List
^ ^ ^ ^ ^[ ^ The National Drugs List Of Syrian Arab Republic Sexth Edition 2006 ! " # "$ % &'() " # * +$, -. / & 0 /+12 3 4" 5 "$ . "$ 67"5,) 0 " /! !2 4? @ % 88 9 3: " # "$ ;+<=2 – G# H H2 I) – 6( – 65 : A B C "5 : , D )* . J!* HK"3 H"$ T ) 4 B K<) +$ LMA N O 3 4P<B &Q / RS ) H< C4VH /430 / 1988 V W* < C A GQ ") 4V / 1000 / C4VH /820 / 2001 V XX K<# C ,V /500 / 1992 V "!X V /946 / 2004 V Z < C V /914 / 2003 V ) < ] +$, [2 / ,) @# @ S%Q2 J"= [ &<\ @ +$ LMA 1 O \ . S X '( ^ & M_ `AB @ &' 3 4" + @ V= 4 )\ " : N " # "$ 6 ) G" 3Q + a C G /<"B d3: C K7 e , fM 4 Q b"$ " < $\ c"7: 5) G . HHH3Q J # Hg ' V"h 6< G* H5 !" # $%" & $' ,* ( )* + 2 ا اوا ادو +% 5 j 2 i1 6 B J' 6<X " 6"[ i2 "$ "< * i3 10 6 i4 11 6! ^ i5 13 6<X "!# * i6 15 7 G!, 6 - k 24"$d dl ?K V *4V h 63[46 ' i8 19 Adl 20 "( 2 i9 20 G Q) 6 i10 20 a 6 m[, 6 i11 21 ?K V $n i12 21 "% * i13 23 b+ 6 i14 23 oe C * i15 24 !, 2 6\ i16 25 C V pq * i17 26 ( S 6) 1, ++ &"r i19 3 +% 27 G 6 ""% i19 28 ^ Ks 2 i20 31 % Ks 2 i21 32 s * i22 35 " " * i23 37 "$ * i24 38 6" i25 39 V t h Gu* v!* 2 i26 39 ( 2 i27 40 B w< Ks 2 i28 40 d C &"r i29 42 "' 6 i30 42 " * i31 42 ":< * i32 5 ./ 0" -33 4 : ANAESTHETICS $ 1 2 -1 :GENERAL ANAESTHETICS AND OXYGEN 4 $1 2 2- ATRACURIUM BESYLATE DROPERIDOL ETHER FENTANYL HALOTHANE ISOFLURANE KETAMINE HCL NITROUS OXIDE OXYGEN PROPOFOL REMIFENTANIL SEVOFLURANE SUFENTANIL THIOPENTAL :LOCAL ANAESTHETICS !67$1 2 -5 AMYLEINE HCL=AMYLOCAINE ARTICAINE BENZOCAINE BUPIVACAINE CINCHOCAINE LIDOCAINE MEPIVACAINE OXETHAZAINE PRAMOXINE PRILOCAINE PREOPERATIVE MEDICATION & SEDATION FOR 9*: ;< " 2 -8 : : SHORT -TERM PROCEDURES ATROPINE DIAZEPAM INJ. -

Management of Cutaneous Hemangiomas in Pediatric Patients
PEDIATRIC DERMATOLOGY Series Editor: Camila K. Janniger, MD Management of Cutaneous Hemangiomas in Pediatric Patients Maria Letizia Musumeci, MD, PhD; Karina Schlecht, MD, PhD; Rosario Perrotta, MD; Robert A. Schwartz, MD, MPH; Giuseppe Micali, MD Cutaneous hemangiomas (CHs) are common benign during the first year of life and slow involution that vascular tumors of childhood. Clinically, they are usually is completed by 5 to 10 years of age.1 For characterized by a typical evolution profile, consist- this reason, no treatment is necessary in most cases. ing of a rapid proliferation during the first year of However, when CHs are located in areas at risk for life and slow involution that usually is completed functional complications; are of considerable size; or by 5 to 10 years of age. In most cases, no treat- repeatedly undergo bleeding, ulceration, or superin- ment is necessary. However, when CHs are located fection, a prompt and adequate treatment approach in areas at risk for functional complications; are of is required.2 considerable size; or repeatedly undergo bleeding, ulceration, or superinfection, a prompt and adequate Epidemiology treatment approach is required. First-line approaches CHs are present in 1.0% to 2.6% of neonates and in include topical, intralesional, and systemic corti- 10% to 12% of infants by 12 months of age.3 Thirty costeroids. Second-line options include interferon percent of CHs are first evident at birth; the remain- alfa-2a and -2b, laser therapy, and surgical therapy. der appear during the second month of life. The Third-line approaches include cytotoxins, emboliza- frequency of these benign tumors increases in pre- tion, and angiogenesis inhibitors. -

Pruritus: Scratching the Surface
Pruritus: Scratching the surface Iris Ale, MD Director Allergy Unit, University Hospital Professor of Dermatology Republic University, Uruguay Member of the ICDRG ITCH • defined as an “unpleasant sensation of the skin leading to the desire to scratch” -- Samuel Hafenreffer (1660) • The definition offered by the German physician Samuel Hafenreffer in 1660 has yet to be improved upon. • However, it turns out that itch is, indeed, inseparable from the desire to scratch. Savin JA. How should we define itching? J Am Acad Dermatol. 1998;39(2 Pt 1):268-9. Pruritus • “Scratching is one of nature’s sweetest gratifications, and the one nearest to hand….” -- Michel de Montaigne (1553) “…..But repentance follows too annoyingly close at its heels.” The Essays of Montaigne Itch has been ranked, by scientific and artistic observers alike, among the most distressing physical sensations one can experience: In Dante’s Inferno, falsifiers were punished by “the burning rage / of fierce itching that nothing could relieve” Pruritus and body defence • Pruritus fulfils an essential part of the innate defence mechanism of the body. • Next to pain, itch may serve as an alarm system to remove possibly damaging or harming substances from the skin. • Itch, and the accompanying scratch reflex, evolved in order to protect us from such dangers as malaria, yellow fever, and dengue, transmitted by mosquitoes, typhus-bearing lice, plague-bearing fleas • However, chronic itch lost this function. Chronic Pruritus • Chronic pruritus is a common and distressing symptom, that is associated with a variety of skin conditions and systemic diseases • It usually has a dramatic impact on the quality of life of the affected individuals Chronic Pruritus • Despite being the major symptom associated with skin disease, our understanding of the pathogenesis of most types of itch is limited, and current therapies are often inadequate. -
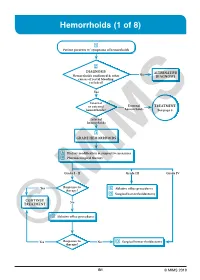
Hemorrhoids (1 of 8)
Hemorrhoids (1 of 8) 1 Patient presents w/ symptoms of hemorrhoids 2 DIAGNOSIS No ALTERNATIVE Hemorrhoids confi rmed & other DIAGNOSIS causes of rectal bleeding excluded? Yes Internal or external External TREATMENT hemorrhoids? hemorrhoids See page 3 Internal hemorrhoids 3 GRADE HEMORRHOIDS A Dietary modifi cation & supportive measures B Pharmacological therapy Grade I - II Grade III Grade IV Yes Response to C Ablative offi ce procedures therapy? D Surgical hemorrhoidectomy CONTINUE No TREATMENT C Ablative offi ce procedures Yes Response to No D Surgical hemorrhoidectomy ©therapy? MIMS B1 © MIMS 2019 Hemorrhoids (2 of 8) 1 SYMPTOMS ATTRIBUTED TO HEMORRHOIDS • Rectal bleeding - Most common presenting symptom - Bright red blood which may drip or squirt into the toilet bowl or scanty amounts may be seen on toilet tissue • Discomfort due to rectal protrusion or lump • Anal pain • HEMORRHOIDS Anal itching 2 DIAGNOSIS Medical History • Assess nature, duration & severity of symptoms - Ask about bleeding, its amount & frequency - Ask about presence of prolapsing tissue, its timing & reproducibility • Elicit possible risk factors for development of hemorrhoidal symptoms - Low-fi ber diets cause small-caliber stools, resulting in straining during defecation & engorgement of hemorrhoids - Prolonged sitting on a toilet which may cause a problem in the venous return in the perianal area - Pregnancy - Advanced age • Th e signs & symptoms of hemorrhoids are not specifi c to the disease, so care must be taken to avoid missing other causes of pathology • Obtain -
![Ehealth DSI [Ehdsi V2.2.2-OR] Ehealth DSI – Master Value Set](https://docslib.b-cdn.net/cover/8870/ehealth-dsi-ehdsi-v2-2-2-or-ehealth-dsi-master-value-set-1028870.webp)
Ehealth DSI [Ehdsi V2.2.2-OR] Ehealth DSI – Master Value Set
MTC eHealth DSI [eHDSI v2.2.2-OR] eHealth DSI – Master Value Set Catalogue Responsible : eHDSI Solution Provider PublishDate : Wed Nov 08 16:16:10 CET 2017 © eHealth DSI eHDSI Solution Provider v2.2.2-OR Wed Nov 08 16:16:10 CET 2017 Page 1 of 490 MTC Table of Contents epSOSActiveIngredient 4 epSOSAdministrativeGender 148 epSOSAdverseEventType 149 epSOSAllergenNoDrugs 150 epSOSBloodGroup 155 epSOSBloodPressure 156 epSOSCodeNoMedication 157 epSOSCodeProb 158 epSOSConfidentiality 159 epSOSCountry 160 epSOSDisplayLabel 167 epSOSDocumentCode 170 epSOSDoseForm 171 epSOSHealthcareProfessionalRoles 184 epSOSIllnessesandDisorders 186 epSOSLanguage 448 epSOSMedicalDevices 458 epSOSNullFavor 461 epSOSPackage 462 © eHealth DSI eHDSI Solution Provider v2.2.2-OR Wed Nov 08 16:16:10 CET 2017 Page 2 of 490 MTC epSOSPersonalRelationship 464 epSOSPregnancyInformation 466 epSOSProcedures 467 epSOSReactionAllergy 470 epSOSResolutionOutcome 472 epSOSRoleClass 473 epSOSRouteofAdministration 474 epSOSSections 477 epSOSSeverity 478 epSOSSocialHistory 479 epSOSStatusCode 480 epSOSSubstitutionCode 481 epSOSTelecomAddress 482 epSOSTimingEvent 483 epSOSUnits 484 epSOSUnknownInformation 487 epSOSVaccine 488 © eHealth DSI eHDSI Solution Provider v2.2.2-OR Wed Nov 08 16:16:10 CET 2017 Page 3 of 490 MTC epSOSActiveIngredient epSOSActiveIngredient Value Set ID 1.3.6.1.4.1.12559.11.10.1.3.1.42.24 TRANSLATIONS Code System ID Code System Version Concept Code Description (FSN) 2.16.840.1.113883.6.73 2017-01 A ALIMENTARY TRACT AND METABOLISM 2.16.840.1.113883.6.73 2017-01 -

Diagnosis and Treatment of Varicose Veins in the Legs
Diagnosis and treatment of varicose veins in the legs KCE reports 164C Belgian Health Care Knowledge Centre Federaal Kenniscentrum voor de Gezondheidszorg Centre fédéral d’expertise des soins de santé 2011 The Belgian Health Care Knowledge Centre Introduction: The Belgian Health Care Knowledge Centre (KCE) is an organization of public interest, created on the 24th of December 2002 under the supervision of the Minister of Public Health and Social Affairs. KCE is in charge of conducting studies that support the political decision making on health care and health insurance. Executive Board Actual Members: Pierre Gillet (President), Dirk Cuypers (Vice-president), Jo De Cock (Vice-president), Frank Van Massenhove (Vice-president), Maggie De Block, Jean-Pierre Baeyens, Ri de Ridder, Olivier De Stexhe, Johan Pauwels, Daniel Devos, Jean-Noël Godin, Xavier De Cuyper, Paul Palstermans, Xavier Brenez, Rita Thys, Marc Moens, Marco Schetgen, Patrick Verertbruggen, Michel Foulon, Myriam Hubinon, Michael Callens, Bernard Lange, Jean-Claude Praet. Substitute Members: Rita Cuypers, Christiaan De Coster, Benoît Collin, Lambert Stamatakis, Karel Vermeyen, Katrien Kesteloot, Bart Ooghe, Frederic Lernoux, Leo Neels, Greet Musch, Geert Messiaen, Anne Remacle, Roland Lemeye, Annick Poncé, Pierre Smiets, Jan Bertels, Celien Van Moerkerke, Yolande Husden, Ludo Meyers, Olivier Thonon, François Perl. Government commissioner: Yves Roger Management Chief Executive Officer: Raf Mertens Assistant Chief Executive Officer: Jean-Pierre Closon Information Federaal Kenniscentrum -

Basic Skin Care and Topical Therapies for Atopic Dermatitis
REVIEWS Basic Skin Care and Topical Therapies for Atopic Dermatitis: Essential Approaches and Beyond Sala-Cunill A1*, Lazaro M2*, Herráez L3, Quiñones MD4, Moro-Moro M5, Sanchez I6, On behalf of the Skin Allergy Committee of Spanish Society of Allergy and Clinical Immunology (SEAIC) 1Allergy Section, Internal Medicine Department, Hospital Universitario Vall d'Hebron, Barcelona, Spain 2Allergy Department, Hospital Universitario de Salamanca, Alergoasma, Salamanca, Spain 3Allergy Department, Hospital Universitario 12 de Octubre, Madrid, Spain 4Allergy Section, Hospital Monte Naranco, Oviedo, Spain 5Allergy Department, Hospital Universitario Fundación Alcorcón, Alcorcón, Madrid, Spain 6Clínica Dermatología y Alergia, Badajoz, Spain *Both authors contributed equally to the manuscript J Investig Allergol Clin Immunol 2018; Vol. 28(6): 379-391 doi: 10.18176/jiaci.0293 Abstract Atopic dermatitis (AD) is a recurrent and chronic skin disease characterized by dysfunction of the epithelial barrier, skin inflammation, and immune dysregulation, with changes in the skin microbiota and colonization by Staphylococcus aureus being common. For this reason, the therapeutic approach to AD is complex and should be directed at restoring skin barrier function, reducing dehydration, maintaining acidic pH, and avoiding superinfection and exposure to possible allergens. There is no curative treatment for AD. However, a series of measures are recommended to alleviate the disease and enable patients to improve their quality of life. These include adequate skin hydration and restoration of the skin barrier with the use of emollients, antibacterial measures, specific approaches to reduce pruritus and scratching, wet wrap applications, avoidance of typical AD triggers, and topical anti-inflammatory drugs. Anti-inflammatory treatment is generally recommended during acute flares or, more recently, for preventive management. -

Bulk Drug Substances Nominated for Use in Compounding Under Section 503B of the Federal Food, Drug, and Cosmetic Act
Updated June 07, 2021 Bulk Drug Substances Nominated for Use in Compounding Under Section 503B of the Federal Food, Drug, and Cosmetic Act Three categories of bulk drug substances: • Category 1: Bulk Drug Substances Under Evaluation • Category 2: Bulk Drug Substances that Raise Significant Safety Risks • Category 3: Bulk Drug Substances Nominated Without Adequate Support Updates to Categories of Substances Nominated for the 503B Bulk Drug Substances List1 • Add the following entry to category 2 due to serious safety concerns of mutagenicity, cytotoxicity, and possible carcinogenicity when quinacrine hydrochloride is used for intrauterine administration for non- surgical female sterilization: 2,3 o Quinacrine Hydrochloride for intrauterine administration • Revision to category 1 for clarity: o Modify the entry for “Quinacrine Hydrochloride” to “Quinacrine Hydrochloride (except for intrauterine administration).” • Revision to category 1 to correct a substance name error: o Correct the error in the substance name “DHEA (dehydroepiandosterone)” to “DHEA (dehydroepiandrosterone).” 1 For the purposes of the substance names in the categories, hydrated forms of the substance are included in the scope of the substance name. 2 Quinacrine HCl was previously reviewed in 2016 as part of FDA’s consideration of this bulk drug substance for inclusion on the 503A Bulks List. As part of this review, the Division of Bone, Reproductive and Urologic Products (DBRUP), now the Division of Urology, Obstetrics and Gynecology (DUOG), evaluated the nomination of quinacrine for intrauterine administration for non-surgical female sterilization and recommended that quinacrine should not be included on the 503A Bulks List for this use. This recommendation was based on the lack of information on efficacy comparable to other available methods of female sterilization and serious safety concerns of mutagenicity, cytotoxicity and possible carcinogenicity in use of quinacrine for this indication and route of administration. -

Vein Medication Experts
Vein Medication Experts Purchase vein care medications directly from an FDA 503B Outsourcing Facility Olympia Compounding Pharmacy is a registered and inspected FDA Outsourcing Facility in Orlando, FL. Because of the extremely high standards required to operate as an FDA facility, there are only fifty FDA compounders in the United States at this time. All compounded items from Olympia Pharmacy are compounded under the new cGMP guidelines to insure the safest, highest quality compounded medications available. For more information, or to open an account please contact: Dan Powell Director of Business Development for Olympia Pharmacy Direct: 407-383-7644 Email: [email protected] Olympia Pharmacy | FDA Outsourcing Facility | 6700 Conroy Rd, Orlando FL 32835| Ph: 407-673-2222 |olympiapharmacy.com Polidocanol / STS Price List - Physicians Prescription Fax: 407-673-1234 Shipping: [ ] UPS Ground [ ] UPS 2nd Day [ ] UPS next business day Physician/Practice Name: ______________________________________________________________________ Ship to Address: ___________________________________________________ Phone: ____________________ City/State/Zip: ________________________________________________ Fax: ____________________ Physician License: ________________________________ Drug Concentration Volume Price Order Qty Polidocanol 1.25%, 1.5% 5ml $28 Polidocanol 3% 5ml $33 Polidocanol 5% 5ml $40 Polidocanol 10% 5ml $50 Glycerin 72%/ Lidocaine 1%/ with Epinephrine 1:100,000 N/A 5ml $24 Glycerin 72% Plain N/A 5ml $28 Nifedipine Ointment 0.3%/ N/A 30g -

WO 2018/089540 Al 17 May 2018 (17.05.2018) W ! P O P C T
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2018/089540 Al 17 May 2018 (17.05.2018) W ! P O P C T (51) International Patent Classification: (74) Agent: ERLACHER, Heidi, A. et al; Cooley LLP, 1299 A61K 9/00 (2006.01) A61K 48/00 (2006.01) Pennsylvania Avenue, NW, Suite 700, Washington, District A61K 9/19 (2006.01) A61K 9/S1 (2006.01) of Columbia 20004-2400 (US). (21) International Application Number: (81) Designated States (unless otherwise indicated, for every PCT/US20 17/060704 kind of national protection available): AE, AG, AL, AM, AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, BZ, (22) International Filing Date: CA, CH, CL, CN, CO, CR, CU, CZ, DE, DJ, DK, DM, DO, 08 November 201 7 (08. 11.201 7) DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, HN, (25) Filing Language: English HR, HU, ID, IL, IN, IR, IS, JO, JP, KE, KG, KH, KN, KP, KR, KW, KZ, LA, LC, LK, LR, LS, LU, LY, MA, MD, ME, (26) Publication Language: English MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, (30) Priority Data: OM, PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SA, 62/419,459 08 November 2016 (08. 11.20 16) US SC, SD, SE, SG, SK, SL, SM, ST, SV, SY,TH, TJ, TM, TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, ZM, ZW. -

See the Meds for Vets Catalog
Quality Guarantee Fast Turnaround Many Items in Stock Affordable Quality Superior Customer Service Meds for Vets values your business and your patients’ health. We look forward to partnering with you to solve Happy Pets • Happy Owners • Happy Vets™ your most difficult medication challenges. Happy Pets. Happy Owners. Happy Vets.™ Visit us at MedsForVets.com & Facebook.com/MedsForVets YOUR COMPLETE SOURCE FOR COMPOUNDED VETERINARY PHARMACEUTICALS • CALL TOLL FREE: 866 MED-4VET (866-633-4838) A portion of all proceeds is donated to animal-related causes. Solving your most difficult medication challenges While many veterinary patients are amena- designed to hide even the most persistent ble to the limited array of commercially medication tastes. Our Triple Meat suspension available dosage forms, many are not. of chicken, pork and ham works equally well for Commercially produced products are often dogs. Chewable treats and flavored feed addi- designed for humans at strengths too high tives afford the benefits of customized flavor- for the majority of veterinary patients. Tablets ing with pre-measured dosing. Flavored oral and capsules are often too large. Fruity flavorings, while well suited to the majority of pastes offer a convenient equine dosage both exotics, are poorly accepted by many dogs at home and at the track. These and other dos- and cats. Owners often have difficulties age forms can be designed to meet specialized administering even the simplest of dosage needs such as sodium restrictions, sugar-free forms. Add to this the unwillingness of some preparations and others upon request. patients to tolerate any medication knowingly, and even the most effective Transdermal Gels medication may become a clinical failure The most difficult of patients rather quickly. -

85624 SP JAPAN 2018-19 Allergeaze Order Form
2021 / 2022 Allergen Order Form ご購入方法 注)ご注文書は全てローマ字でご入力/ご記入ください。注文書内の* 印の欄は入力必須項目です。 1. 注文者情報(Contact Person)、送付先(Shipping)、請求書宛先(Billing)、お支払い方法(Payment) をご入力ください。 2. 各アレルゲンを個別でご購入する場合は、ご注文の数を各アレルゲン横のボックス(qty) にご入力下さい。アレルゲンをシリーズや 種類・グループごとにまとめてご購入の場合は、ご注文の数を項目別一番上のグレーのボックス(qty) にご入力ください。 3. Eメール又はFAXでご注文:注文書PDFファイルを入力/記入後、添付書類としてEメールで送信の場合は [email protected] まで。FAXの場合は046-200-5626まで。 SERIES: シリーズ別..........選定されたリサーチグループによる推薦アレルゲン種。 GROUPINGS: グループ別..........国際的なリサーチグループや専門文献のレビューの推薦に基き、環境などによる接触の原因別によってあ らかじめセレクトされ た 濃 度 のアレル ゲン 種 CATEGORIES: カテゴリー別......商品タイプ別アレルゲン種(濃度の違う同一のアレルゲンが含まれている場合もあり)。 CONTACT PERSON *Required fields *First Name Last Name *Phone Fax *Email *Physician’s Name License # SHIPPING *Required fields BILLING *Required fields *Company Name *Company Name *Address *Address *City *City *State *Postal/ZIP *State *Postal/ZIP *Country *Country Use this address for my Billing Information METHOD OF PAYMENT *Required fields 銀行振り込み --- 振込先:三菱東京UFJ大和支店(普)0388950 カ)スマートプラクティスジャパン カナダ( 30日以内に振込みをお願い致 します) Payment terms are Net 30 Days PRICING: 送料 1..................¥3,980/allergen <¥115,000 .................. ¥4,700 12~ .............¥3,860/allergen ¥115,001~¥225,000 ....¥5,200 720 28th Street NE, Suite #210 25~ .............¥3,740/allergen ¥225,001~¥335,000 ....¥7,000 Calgary, AB T2A6R3 (税別) ¥335,001~¥675,000 ..¥14,000 PHONE: 866.903.2671 FAX: 866.903.2672 | ¥675,001~ .................¥21,000 EMAIL: [email protected] 1 ALLERGEN ORDER FORM: SERIES SKU test substance %, vehicle qty SKU test substance %, vehicle qty