Perforated Sigmoid Diverticulitis in a Lumbar Hernia After
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Diverticular Abscess Presenting As a Strangulated Inguinal Hernia: Case Report and Review of the Literature
Ulster Med J 2007; 76 (2) 107-108 Presidential Address 107 Case Report Diverticular Abscess Presenting as a Strangulated Inguinal Hernia: Case Report and review of the literature. S Imran H Andrabi, Ashish Pitale*, Ahmed AS El-Hakeem Accepted 22 December 2006 ABSTRACT noted nausea, anorexia and increasing abdominal pain. She had no previous history of any surgery or trauma and was on Potentially life threatening diseases can mimic a groin hernia. warfarin for atrial fibrillation. We present an unusual case of diverticulitis with perforation and a resulting abscess presenting as a strangulated inguinal hernia. The features demonstrated were not due to strangulation of the contents of the hernia but rather pus tracking into the hernia sac from the peritoneal cavity. The patient underwent sigmoid resection and drainage of retroperitoneal and pericolonic abscesses. Radiological and laboratory studies augment in reaching a diagnosis. The differential diagnosis of inguinal swellings is discussed. Key Words: Diverticulitis, diverticular perforation, diverticular abscess, inguinal hernia INTRODUCTION The association of complicated inguinal hernia and diverticulitis is rare1. Diverticulitis can present as left iliac fossa pain, rectal bleeding, fistulas, perforation, bowel obstruction and abscesses. Our patient presented with a diverticular perforation resulting in an abscess tracking into the inguinal canal and clinically masquerading as a Fig 2. CT scan showing inflammatory changes with strangulated inguinal hernia. The management warranted an stranding of the subcutaneous fat in the left groin and a exploratory laparotomy and drainage of pus. large bowel diverticulum CASE REPORT On admission, she had a tachycardia (pulse 102 beats/min) and a temperature of 37.5OC. -

Repair of a Grynfeltt-Lesshaft Hernia with the PROCEED
Glatz et al. Surgical Case Reports (2018) 4:50 https://doi.org/10.1186/s40792-018-0456-x CASE REPORT Open Access Repair of a Grynfeltt-Lesshaft hernia with the PROCEED™ VENTRAL PATCH: a case report Torben Glatz* , Hannes Neeff, Philipp Holzner, Stefan Fichtner-Feigl and Oliver Thomusch Abstract Background: Primary hernias in the triangle of Grynfeltt are very rare and therefore pose a difficulty in diagnosis and treatment. Due to the lack of systematic studies, the surgical approach must be chosen individually for each patient. Here, we describe an easy and safe surgical approach. Case presentation: We report the case of a 53-year-old male patient with a history of mental disability and pronounced scoliosis, who presented with a Grynfeltt-Lesshaft hernia with protrusion of the ascending colon and the right ureter. The hernia was repaired via a dorsal, extraperitoneal approach. The hernia gap with a diameter of approximately 1 cm was closed with insertion of a 6.4 × 6.4 cm PROCEED™ VENTRAL PATCH (Ethicon, Norderstedt, Germany). The operating time was 33 min and the patient was discharged the next day and showed no signs of recurrence at 1-year follow up. Conclusion: The technique described here is favorable because it requires very little dissection of the surrounding tissue and no trans-/intraabdominal dissection. The technique was chosen in this particular case to guarantee a fast postoperative recovery and prompt hospital discharge. Keywords: Grynfeltt-Lesshaft hernia, Lumbar hernia, PROCEED™ VENTRAL PATCH Background incarceration and a right lumbar protrusion with the Lumbar hernias are a very rare cause of abdominal com- clinical appearance of a soft tissue mass. -
Abdominal Wall Anterior 98-108 Posterior 109-11 Abductor Digiti
Index Cambridge University Press 978-0-521-72809-6 - Atlas of Musculoskeletal Ultrasound Anatomy: Second Edition Dr Mike Bradley and Dr Paul O’Donnell Index More information Index abdominal wall brachialis 42 echogenicity xi anterior 98–108 – – brachioradialis 49 elbow 49 64 posterior 109 11 anterior 53–8 calcaneo-fibular – abductor digiti minimi 70, 87 ligament 193 lateral 49 52 abductor pollicis brevis 87 medial 60 calf 178–86 posterior 62–4 abductor pollicis longus 79 antero-lateral compartment – extensor carpi radialis brevis acromioclavicular joint 26–7 179 80 lateral compartment 181–2 49, 79 adductor brevis 134 posterior compartment extensor carpi radialis longus – adductor canal 151 183 6 49, 79 adductor longus 134 capsule echogenicity xi extensor carpi ulnaris 79 – adductor magnus 134, 137 carpal tunnel 70 3 extensor digiti minimi 79 air echogenicity xi cartilage echogenicity extensor digitorum 79 costal cartilage xi – extensor digitorum longus 178 anatomical snuffbox 76 7 fibrocartilage xi anisotropy ix hyaline cartilage xi extensor hallucis longus 178, 205, 218–19 ankle 187–205 chest wall 13–21 anterior 202–5 anterior 13 extensor indicis 79 – lateral 193–6 costal cartilages 13 16 extensor pollicis brevis 79 medial 197–201 lateral 17 posterior 187–92 posterior 18–21 extensor pollicis longus 79 ribs 13–16 annular ligament 52 extensor retinaculum 202 collateral ligament anterior cruciate ligament fascia echogenicity xi lateral 167 (ACL) 153–7 fat echogenicity xi medial 165 antero-lateral pelvis 127–30 ulnar (UCL) 61 femoral neck -

MANAGEMENT of ACUTE ABDOMINAL PAIN Patrick Mcgonagill, MD, FACS 4/7/21 DISCLOSURES
MANAGEMENT OF ACUTE ABDOMINAL PAIN Patrick McGonagill, MD, FACS 4/7/21 DISCLOSURES • I have no pertinent conflicts of interest to disclose OBJECTIVES • Define the pathophysiology of abdominal pain • Identify specific patterns of abdominal pain on history and physical examination that suggest common surgical problems • Explore indications for imaging and escalation of care ACKNOWLEDGEMENTS (1) HISTORICAL VIGNETTE (2) • “The general rule can be laid down that the majority of severe abdominal pains that ensue in patients who have been previously fairly well, and that last as long as six hours, are caused by conditions of surgical import.” ~Cope’s Early Diagnosis of the Acute Abdomen, 21st ed. BASIC PRINCIPLES OF THE DIAGNOSIS AND SURGICAL MANAGEMENT OF ABDOMINAL PAIN • Listen to your (and the patient’s) gut. A well honed “Spidey Sense” will get you far. • Management of intraabdominal surgical problems are time sensitive • Narcotics will not mask peritonitis • Urgent need for surgery often will depend on vitals and hemodynamics • If in doubt, reach out to your friendly neighborhood surgeon. Septic Pain Sepsis Death Shock PATHOPHYSIOLOGY OF ABDOMINAL PAIN VISCERAL PAIN • Severe distension or strong contraction of intraabdominal structure • Poorly localized • Typically occurs in the midline of the abdomen • Seems to follow an embryological pattern • Foregut – epigastrium • Midgut – periumbilical • Hindgut – suprapubic/pelvic/lower back PARIETAL/SOMATIC PAIN • Caused by direct stimulation/irritation of parietal peritoneum • Leads to localized -

Lumps and Bumps of the Abdominal Wall and Lumbar Region—Part 1: Hernias, What the Radiologist Should Know
Published online: 2019-06-18 THIEME 12 Review Article Lumps and Bumps of the Abdominal Wall and Lumbar Region—Part 1: Hernias, What the Radiologist Should Know Sangoh Lee1 Sarah R. Hudson1 Catalin V. Ivan1 Tahir Hussain1 Ratan Verma1 Arumugam Rajesh1 James A. Stephenson1 1Gastrointestinal Imaging Group, Department of Radiology, Address for correspondence James A. Stephenson, MD, FRCR, University Hospitals of Leicester NHS Trust, Leicester General Gastrointestinal Imaging Group, Department of Radiology, Hospital, Leicester, United Kingdom University Hospitals of Leicester NHS Trust, Leicester General Hospital, Leicester LE5 4PW, United Kingdom (e-mail: [email protected]). J Gastrointestinal Abdominal Radiol ISGAR 2018;1:12–18 Abstract Abdominal hernias represent common conditions and occur when a structure of the abdominal cavity protrudes through a defect in the abdominal wall. Recently, there has Keywords been an increase in demand from the clinical teams to confirm the clinical suspicion ► abdominal wall of an abdominal wall hernia, and to assess preoperatively large or complex hernias ► hernias through imaging. This pictorial review aims to present the different appearances of ► lumbar region abdominal wall and lumbar region hernias on imaging. however, many surgeons now prefer to have confirmatory Introduction imaging prior to invasive corrective surgery. Moreover, Abdominal hernias occur when part of or an organ of a body imaging can be particularly useful in assessing large abdom- 1 cavity protrudes through a defect in the wall of that cavity. inal wall defects with involvement of different abdominal It is a common condition with lifetime risk of developing a anatomical boundaries/walls (such as large incisional hernias 2 groin hernia estimated at 27% for men and 3% for women. -

Ana Tomical Triangles J
43 ANA TOMICAL TRIANGLES J. LESLIE PACE, M.D. Department of Anatomy, Royal University of Malta Anatomical description is given of certain areas in the human hody which have :.l triangular sha!)e and which are of anatomical or surgical importance. There are at lea;,t 30 describe,d ,anatomical triangles, many of which receive eponymous names. Some are of nUlrked importance and well known e.g. Scarpa's femoral triangle, Hesselbach's inguinal triangle, H!ld Petit '5 lumbar triangle; others arc of relative1y minor importance and n.ot so well-known e.g. Elau's, Friteau's and Assezat's triangles. Anatomical trianlfles are described in various regions .of the body e.g. Macewen's ana Trautmann's in the head regiml, Beclaud's and PirDgoff's in the neck region, He'lSelbach '5, Henke '5, Petit's amI Grynfeltt's in the ,abdominal wall region and Searpa's Hnd Weber's in the lower limb Tf~gion. Their size varies, some being large e.g. Scarpa's triangle, others being very small e.g. Macewen's triangle. The bDundaries of these triangular areas may cDnsist of muscle borders e.g. the triangle .of Lannier and the variDUS tria,ngles of the neck; of n111sc1e borders and· bony cn1"fac(1,~ e.g. P(~lit'.~l tri,f)ng]c, t]1(' tria11['1]" ,C)f M'll"('ille J;lIlfl t1H~ tl"i[J11~le of Auscultation; of muscle borders and blood ves,ds e.g. Uesselbach's; of imaginary line, clrawn hetween fixed bony points e.g. -
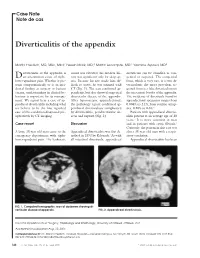
Diverticulitis of the Appendix
Case Note Note de cas Diverticulitis of the appendix Martin Friedlich, MD, MSc, MEd;* Neesh Malik, MD;† Martin Lecompte, MD;† Yasmine Ayroud, MD‡ iverticulitis of the appendix is count was elevated; his medical his- diverticula can be classified as con- Dan uncommon cause of right- tory was significant only for sleep ap- genital or acquired. The congenital lower-quadrant pain. Whether it pre- nea. Because his size made him dif- form, which is very rare, is a true di- sents symptomatically or is an inci- ficult to assess, he was scanned with verticulum; the more prevalent ac- dental finding at surgery or barium CT (Fig. 1). The scan confirmed ap- quired form is a false diverticulum on enema, understanding its clinical be- pendicitis, but also showed suspected the mesenteric border of the appendix. haviour is important for its manage- diverticular disease of the appendix. The incidence of diverticula found in ment. We report here a case of ap- After laparoscopic appendectomy, appendectomy specimens ranges from pendiceal diverticulitis including what the pathology report confirmed ap- 0.004% to 2.1%; from routine autop- we believe to be the first reported pendiceal diverticulosis complicated sies, 0.20% to 0.6%.2 case of this condition diagnosed pre- by diverticulitis, peridiverticular ab- Patients with appendiceal divertic- operatively by CT imaging. scess and rupture (Fig. 2). ulitis present at an average age of 38 years.3 It is more common in men Case report Discussion and in patients with cystic fibrosis.2 Curiously, the patient in this case was A large 38-year-old man came to the Appendiceal diverticulitis was first de- also a 38-year-old man with a respir- emergency department with right- scribed in 1893 by Kelynack.1 As with atory condition. -
Colonic Gallstone Obstruction
Advances in Clinical Medical Research and Healthcare Delivery Volume 1 Issue 1 Inaugural Issue Article 4 2021 Colonic Gallstone Obstruction Abdoulaziz Toure M.D Arnot Ogden Medical Center, [email protected] Mitchell Witkowski LECOM, [email protected] Vithal Vernenkar D.O Newark Wayne Community Hospital, [email protected] Brian Watkins MD, MS, FACS Newark Wayne Community Hospital, [email protected] Prasad V. Penmetsa M.D Rochester General Hospital, [email protected] Follow this and additional works at: https://scholar.rochesterregional.org/advances Part of the Health and Medical Administration Commons, Medical Education Commons, and the Medical Specialties Commons Recommended Citation Toure A, Witkowski M, Vernenkar V, Watkins B, Penmetsa PV. Colonic Gallstone Obstruction. Advances in Clinical Medical Research and Healthcare Delivery. 2021; 1(1). doi: 10.53785/2769-2779.1005. This Article is brought to you for free and open access by RocScholar. It has been accepted for inclusion in Advances in Clinical Medical Research and Healthcare Delivery by an authorized editor of RocScholar. ISSN: 2769-2779 Colonic Gallstone Obstruction Abstract This report discusses a case of a 79-year-old Caucasian female who presented with large bowel obstruction. A significant TC findings of cholecystocolic fistula and an impacted gallstone at the junction of the descending and sigmoid colon. We present a case of colonic gallstone obstruction that was treated with endoscopic lithotripsy. This interventional approach is effective in stable elderly patients with high surgical risk and in patients with significant comorbidities. Keywords gallstone complication, Cholecystocolic fistula, colonic gallstones, large bowel gallstones, gallstone ileus This article is available in Advances in Clinical Medical Research and Healthcare Delivery: https://scholar.rochesterregional.org/advances/vol1/iss1/4 Toure et al.: Colonic Gallstone Obstruction Background Gallstone ileus is a rare complication of cholelithiasis. -

Anterior Abdominal Wall
Abdominal wall Borders of the Abdomen • Abdomen is the region of the trunk that lies between the diaphragm above and the inlet of the pelvis below • Borders Superior: Costal cartilages 7-12. Xiphoid process: • Inferior: Pubic bone and iliac crest: Level of L4. • Umbilicus: Level of IV disc L3-L4 Abdominal Quadrants Formed by two intersecting lines: Vertical & Horizontal Intersect at umbilicus. Quadrants: Upper left. Upper right. Lower left. Lower right Abdominal Regions Divided into 9 regions by two pairs of planes: 1- Vertical Planes: -Left and right lateral planes - Midclavicular planes -passes through the midpoint between the ant.sup.iliac spine and symphysis pupis 2- Horizontal Planes: -Subcostal plane - at level of L3 vertebra -Joins the lower end of costal cartilage on each side -Intertubercular plane: -- At the level of L5 vertebra - Through tubercles of iliac crests. Abdominal wall divided into:- Anterior abdominal wall Posterior abdominal wall What are the Layers of Anterior Skin Abdominal Wall Superficial Fascia - Above the umbilicus one layer - Below the umbilicus two layers . Camper's fascia - fatty superficial layer. Scarp's fascia - deep membranous layer. Deep fascia : . Thin layer of C.T covering the muscle may absent Muscular layer . External oblique muscle . Internal oblique muscle . Transverse abdominal muscle . Rectus abdominis Transversalis fascia Extraperitoneal fascia Parietal Peritoneum Superficial Fascia . Camper's fascia - fatty layer= dartos muscle in male . Scarpa's fascia - membranous layer. Attachment of scarpa’s fascia= membranous fascia INF: Fascia lata Sides: Pubic arch Post: Perineal body - Membranous layer in scrotum referred to as colle’s fascia - Rupture of penile urethra lead to extravasations of urine into(scrotum, perineum, penis &abdomen) Muscles . -

Gross Anatomy Mcqs Database Contents 1
Gross Anatomy MCQs Database Contents 1. The abdomino-pelvic boundary is level with: 8. The superficial boundary between abdomen and a. the ischiadic spine & pelvic diaphragm thorax does NOT include: b. the arcuate lines of coxal bones & promontorium a. xiphoid process c. the pubic symphysis & iliac crests b. inferior margin of costal cartilages 7-10 d. the iliac crests & promontorium c. inferior margin of ribs 10-12 e. none of the above d. tip of spinous process T12 e. tendinous center of diaphragm 2. The inferior limit of the abdominal walls includes: a. the anterior inferior iliac spines 9. Insertions of external oblique muscle: b. the posterior inferior iliac spines a. iliac crest, external lip c. the inguinal ligament b. pubis d. the arcuate ligament c. inguinal ligament e. all the above d. rectus sheath e. all of the above 3. The thoraco-abdominal boundary is: a. the diaphragma muscle 10. The actions of the rectus abdominis muscle: b. the subcostal line a. increase of abdominal pressure c. the T12 horizontal plane b. decrease of thoracic volume d. the inferior costal rim c. hardening of the anterior abdominal wall e. the subchondral line d. flexion of the trunk e. all of the above 4. Organ that passes through the pelvic inlet occasionally: 11. The common action of the abdominal wall muscles: a. sigmoid colon a. lateral bending of the trunk b. ureters b. increase of abdominal pressure c. common iliac vessels c. flexion of the trunk d. hypogastric nerves d. rotation of the trunk e. uterus e. all the above 5. -

Gallstone Ileus Treated by Incidental Meckel's Diverticulectomy
Open Access Case Report DOI: 10.7759/cureus.14078 Gallstone Ileus Treated by Incidental Meckel’s Diverticulectomy Zachary A. Koenig 1 , Jason Turner 2 1. School of Medicine, West Virginia University, Morgantown, USA 2. Department of Surgery, West Virginia University, Martinsburg, USA Corresponding author: Zachary A. Koenig, [email protected] Abstract Gallstone ileus is an uncommon cause of intestinal obstruction in the elderly. It is typically recognized on computed tomography by the presence of pneumobilia and a gallstone in the right iliac fossa. Nonetheless, it is important to consider that gallstone ileus may represent the presentation of another pathology rather than an entity on its own. Here, we report successful retrieval of a gallstone that was causing ileus. Intraoperatively, the gallstone was noted lodged in the terminal ileum distal to an incidentally noted Meckel’s diverticulum. The gallstone was milked proximally into the Meckel’s diverticulum and the base was transected. This case illustrates a rare, but unique, surgical technique utilizing a small bowel diverticulum as a vector for stone removal. Categories: Gastroenterology, General Surgery Keywords: gallstone ileus, meckel's diverticulum, diverticulectomy Introduction Meckel’s diverticulum is a true diverticulum that arises from the antimesenteric surface of the middle-to- distal ileum due to incomplete obliteration of the vitelline duct during the seventh week of gestation. It is the most common malformation of the gastrointestinal tract [1]. The anomaly is known for its “rule of twos,” being present in 2% of the population, presenting before the age of two, being twice as common in men compared to women, and being located two feet from the ileocecal valve [2]. -

Laparoscopic Repair of Lumbar Hernia: Case Report and Review of the Literature Case Report121 of Videoendoscopic Surgery
VBrazilianol. 6, Nº 3 Journal Laparoscopic Repair of Lumbar Hernia: Case Report and Review of the Literature Case Report121 of Videoendoscopic Surgery Laparoscopic Repair of Lumbar Hernia: Case Report and Review of the Literature Hérnia Lombar - Correção Videolaparoscópica: Relato de caso e Revisão da Literatura BRUNO HAFEMANN MOSER1; SILVANO SADOWSKI2; JÚLIO CEZAR UILI COELHO3 Hospital Nossa Senhora das Graças, Curitiba. Curitiba, Paraná, Brazil. 1. Digestive Tract Surgeon, Hospital Nossa Senhora das Graças; 2. Digestive Tract Surgeon, Hospital Nossa Senhora das Graças; 3. Chief of the Digestive Tract and Liver Transplant Surgical Service, Hospital Nossa Senhora das Graças and of the University Hospital of the Federal University of Paraná (UFPR). ABSTRACT Lumbar hernias are rare, the symptoms are vague and nonspecific, and usually a CT scan of the abdomen is required for diagnosis. All these factors conspire so that few surgeons have experience in correcting this type of hernia. This is suggested by the few cases reported in the literature, and is especially true for laparoscopic repair. This report describes one patient with a Petit hernia; our objective is to demonstrate the laparoscopic repair as an effective and feasible technique. Key words: Lumbar hernia. Laparoscopic surgery. Petit hernia. Braz. J. Video-Sur, 2013, v. 6, n. 3: 121-123 Accepted after revision: june, 25, 2013. CASE REPORT his 57 year old female patient presented Tcomplaining of pain and bulging in the left lumbar region of five months duration, which worsened with physical activities. She denied a prior history of medical illness or use of medications. Her only surgical history was a cesarean delivery and reduction mammoplasty.