An Exploratory Randomized, Controlled Study on the Efficacy and Safety Of
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Coinfection and Other Clinical Characteristics of COVID-19 In
Coinfection and Other Clinical Characteristics of COVID-19 in Children Qin Wu, MD,a,p Yuhan Xing, MD,b,p Lei Shi, MB,a,p Wenjie Li, MS,a Yang Gao, MS,a Silin Pan, PhD, MD,a Ying Wang, MS,c Wendi Wang, MS,a Quansheng Xing, PhD, MDa BACKGROUND AND OBJECTIVES: Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is abstract a newly identified pathogen that mainly spreads by droplets. Most published studies have been focused on adult patients with coronavirus disease 2019 (COVID-19), but data concerning pediatric patients are limited. In this study, we aimed to determine epidemiological characteristics and clinical features of pediatric patients with COVID-19. METHODS: We reviewed and analyzed data on pediatric patients with laboratory-confirmed COVID-19, including basic information, epidemiological history, clinical manifestations, laboratory and radiologic findings, treatment, outcome, and follow-up results. RESULTS: A total of 74 pediatric patients with COVID-19 were included in this study. Of the 68 case patients whose epidemiological data were complete, 65 (65 of 68; 95.59%) were household contacts of adults. Cough (32.43%) and fever (27.03%) were the predominant symptoms of 44 (59.46%) symptomatic patients at onset of the illness. Abnormalities in leukocyte count were found in 23 (31.08%) children, and 10 (13.51%) children presented with abnormal lymphocyte count. Of the 34 (45.95%) patients who had nucleic acid testing results for common respiratory pathogens, 19 (51.35%) showed coinfection with other pathogens other than SARS-CoV-2. Ten (13.51%) children had real-time reverse transcription polymerase chain reaction analysis for fecal specimens, and 8 of them showed prolonged existence of SARS-CoV-2 RNA. -

CONNECTION the Official Newsletter of Zhejiang University Issue 16 Feb.2020
CONNECTION The Official Newsletter of Zhejiang University Issue 16 Feb.2020 COVID-19 Special Issue Stand Strong Message from Editor-in-Chief CONNECTION Welcome to the special COVID-19 issue of Issue 16 CONNECTION, which highlights the efforts and contributions of ZJU community in face of the epidemic. As a group, they are heroes in harm's way, givers and doers who respond swiftly to the need of our city, our country and the world. When you read their stories, you'll recognize the strength and solidarity that define all ZJUers. ZJU community has demonstrated its courage and resilience in the battle against the novel coronavirus. At this time, let us all come together to protect ourselves and our loved ones, keep all those who are at the front lines in our prayers and pass on our gratitude to those who have joined and contributed to the fight against the virus. Together, we will weather this crisis. LI Min, Editor-in-Chief Director, Office of Global Engagement Editorial office : Global Communications Office of Global Engagement, Zhejiang University 866 Yuhangtang Road, Hangzhou, P.R. China 310058 Phone: +86 571 88981259 Fax: +86 571 87951315 Email: [email protected] Edited by : CHEN Weiying, AI Ni Designed by : HUANG Zhaoyi Material from Connection may be reproduced accompanied with appropriate acknowledgement. CONTENTS Faculty One of the heroes in harm’s way: LI Lanjuan 03 ZJU medics answered the call from Wuhan 04 Insights from ZJU experts 05 Alumni Fund for Prevention and Control of Viral Infectious Diseases set up 10 Alumni community mobilized in the battle against COVID-19 11 Education Classes start online during the epidemic 15 What ZJUers feel about online learning 15 Efforts to address concerns, avoid misinformation 17 International World standing with us 18 International students lending a hand against the epidemic 20 What our fans say 21 FacultyFaculty ZJU community has taken on the responsibility to join the concertedZJU community efforts has takenagainst on thethe responsibility spreadto join the of concerted the virus. -

1. Sars-Cov Nucleocapsid Protein Epitopes and Uses Thereof
www.engineeringvillage.com Citation results: 500 Downloaded: 4/24/2020 1. SARS-COV NUCLEOCAPSID PROTEIN EPITOPES AND USES THEREOF KELVIN, David; PERSAD, Desmond; CAMERON, Cheryl; BRAY, Kurtis, R.; LOFARO, Lori, R.; JOHNSON, Camille; SEKALY, Rafick-Pierre; YOUNES, Souheil-Antoine; CHONG, Pele Assignee: UNIVERSITY HEALTH NETWORK; BECKMAN COULTER, INC.; UNIVERSITE DE MONTREAL; NATIONAL HEALTH RESEARCH INSTITUTES Publication Number: WO2005103259 Publication date: 11/03/2005 Kind: Patent Application Publication Database: WO Patents Compilation and indexing terms, 2020 LexisNexis Univentio B.V. Data Provider: Engineering Village 2. SARS-CoV-specific B-cell epitope and applications thereof Wu, Han-Chung; Liu, I-Ju; Chiu, Chien-Yu Assignee: National Taiwan University Publication Number: US20060062804 Publication date: 03/23/2006 Kind: Utility Patent Application Database: US Patents Compilation and indexing terms, 2020 LexisNexis Univentio B.V. Data Provider: Engineering Village 3. A RECOMBINANT SARS-COV VACCINE COMPRISING ATTENUATED VACCINIA VIRUS CARRIERS QIN, Chuan; WEI, Qiang; GAO, Hong; TU, Xinming; CHEN, Zhiwei; ZHANG, Linqi; HO, David, D. Assignee: INSTITUTE OF LABORATORY ANIMAL SCIENCE OF CHINESE ACADEMY OF MEDICAL SCIENCES; THE AARON DIAMOND AIDS RESEARCH CENTER; QIN, Chuan; WEI, Qiang; GAO, Hong; TU, Xinming; CHEN, Zhiwei; ZHANG, Linqi; HO, David, D. Publication Number: WO2006079290 Publication date: 08/03/2006 Kind: Patent Application Publication Database: WO Patents Compilation and indexing terms, 2020 LexisNexis Univentio B.V. Data -
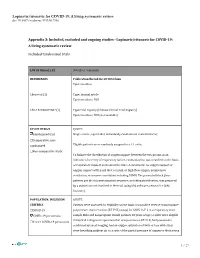
Lopinavir/Ritonavir for COVID-19: a Living Systematic Review Doi: 10.5867/Medwave.2020.06.7966
Lopinavir/ritonavir for COVID-19: A living systematic review doi: 10.5867/medwave.2020.06.7966 Appendix 3: Included, excluded and ongoing studies - Lopinavir/ritonavir for COVID-19: A living systematic review Included randomised trials LOTUS China (1,2) Details or comments REFERENCES Publication thread for LOTUS China Epistemonikos Chen et al (1) Type: Journal article Epistemonikos | DOI ChiCTR2000029387 (2) Type:Trial registry (Chinese Clinical Trial Registry) Epistemonikos | DOI (not available) STUDY DESIGN QUOTE: ☑Randomised trial Single centre , open-label, individually randomized, controlled trial; ☐Comparative, non- randomised Eligible patients were randomly assigned in a 1:1 ratio; ☐Non-comparative study To balance the distribution of oxygen support between the two groups as an indicator of severity of respiratory failure, randomization was stratified on the basis of respiratory support methods at the time of enrollment: no oxygen support or oxygen support with nasal duct or mask, or high-flow oxygen, noninvasive ventilation, or invasive ventilation including ECMO. The permuted block (four patients per block) randomization sequence, including stratification, was prepared by a statistician not involved in the trial, using SAS software, version 9.4 (SAS Institute). POPULATION: INCLUSION QUOTE: CRITERIA Patients were assessed for eligibility on the basis of a positive reverse-transcriptase– ☐COVID-19 polymerase-chain-reaction (RT-PCR) assay) for SARS-CoV-2 in a respiratory tract ☑COVID-19 pneumonia sample Male and nonpregnant female patients 18 years of age or older were eligible if they had a diagnostic specimen that was positive on RT-PCR, had pneumonia ☐Severe COVID-19 pneumonia confirmed by chest imaging, had an oxygen saturation of 94% or less while they were breathing ambient air or a ratio of the partial pressure of oxygen to the fraction 1 / 27 Lopinavir/ritonavir for COVID-19: A living systematic review doi: 10.5867/medwave.2020.06.7966 of inspired oxygen at or below 300 mg Hg. -

A Longitudinal Cohort of Randomly Sampled Weibo Users Yuner Zhu, MA; King-Wa Fu, Phd; Karen A
BRIEF REPORT Limited Early Warnings and Public Attention to Coronavirus Disease 2019 in China, January–February, 2020: A Longitudinal Cohort of Randomly Sampled Weibo Users Yuner Zhu, MA; King-Wa Fu, PhD; Karen A. Grépin, PhD; Hai Liang, PhD; Isaac Chun-Hai Fung, PhD ABSTRACT Objective: Awareness and attentiveness have implications for the acceptance and adoption of disease prevention and control measures. Social media posts provide a record of the public’s attention to an outbreak. To measure the attention of Chinese netizens to coronavirus disease 2019 (COVID-19), a pre-established nationally representative cohort of Weibo users was searched for COVID-19-related key words in their posts. Methods: COVID-19-related posts (N = 1101) were retrieved from a longitudinal cohort of 52 268 randomly sampled Weibo accounts (December 31, 2019–February 12, 2020). Results: Attention to COVID-19 was limited prior to China openly acknowledging human-to-human transmis- sion on January 20. Following this date, attention quickly increased and has remained high over time. Particularly high levels of social media traffic appeared around when Wuhan was first placed in quarantine (January 23–24, 8–9% of the overall posts), when a scandal associated with the Red Cross Society of China occurred (February 1, 8%), and, following the death of Dr Li Wenliang (February 6–7, 11%), one of the whis- tleblowers who was reprimanded by the Chinese police in early January for discussing this outbreak online. Conclusion: Limited early warnings represent missed opportunities to engage citizens earlier in the out- break. Governments should more proactively communicate early warnings to the public in a transparent manner. -

The Wuhan Coronavirus and Its Impact on China's Foreign Relations
12 2 April 2020 The Wuhan Coronavirus and Its Impact on China’s Foreign Relations – Part One Lindsay Hughes Senior Research Analyst Indo-Pacific Research Programme Key Points China has semi-officially denied that the coronavirus that is currently sweeping across the world originated there. Beijing has also claimed that it is a role model in its handling of the pandemic. Those claims are vigorously disputed by Western countries. The West is also becoming increasingly exasperated with China’s lies, double standards and apparent willingness to steal, blackmail and coerce. The West is now re-evaluating its individual and collective relationships with China. Summary The Covid-19 pandemic, which has swept through many parts of the world, had infected over 330,000 people globally at the time of writing and caused around 15,000 deaths by 23 March. In Australia, the number of confirmed cases has moved past 1,700, with 37 per cent of those being reported between 21 March and 23 March. This graph below shows the infection rate in Australia. In the US, the number of confirmed Covid-19 cases had surpassed 32,000 by 23 March, having grown ten-fold from a week earlier. New Zealand moved to the highest state of alert and closed its schools on 25 March, while India declared a “people’s curfew” on 22 March, leading to virtually empty streets in the capital, New Delhi, and in its financial capital, Mumbai. While most Indians complied with the curfew, many did not, leading the government there to declare that those who violated the curfew would face up to six months imprisonment. -

A Longitudinal Cohort of Randomly Sampled Weibo Users Yuner Zhu, MA; King-Wa Fu, Phd; Karen A
BRIEF REPORT Limited Early Warnings and Public Attention to Coronavirus Disease 2019 in China, January–February, 2020: A Longitudinal Cohort of Randomly Sampled Weibo Users Yuner Zhu, MA; King-Wa Fu, PhD; Karen A. Grépin, PhD; Hai Liang, PhD; Isaac Chun-Hai Fung, PhD ABSTRACT Objective: Awareness and attentiveness have implications for the acceptance and adoption of disease prevention and control measures. Social media posts provide a record of the public’s attention to an outbreak. To measure the attention of Chinese netizens to coronavirus disease 2019 (COVID-19), a pre-established nationally representative cohort of Weibo users was searched for COVID-19-related key words in their posts. Methods: COVID-19-related posts (N = 1101) were retrieved from a longitudinal cohort of 52 268 randomly sampled Weibo accounts (December 31, 2019–February 12, 2020). Results: Attention to COVID-19 was limited prior to China openly acknowledging human-to-human transmis- sion on January 20. Following this date, attention quickly increased and has remained high over time. Particularly high levels of social media traffic appeared around when Wuhan was first placed in quarantine (January 23–24, 8–9% of the overall posts), when a scandal associated with the Red Cross Society of China occurred (February 1, 8%), and, following the death of Dr Li Wenliang (February 6–7, 11%), one of the whis- tleblowers who was reprimanded by the Chinese police in early January for discussing this outbreak online. Conclusion: Limited early warnings represent missed opportunities to engage citizens earlier in the out- break. Governments should more proactively communicate early warnings to the public in a transparent manner. -

(COVID-19):International Expert Opinions and Experience from China
Diagnosis and treatment for Novel Coronavirus Pneumonia (COVID-19): International Expert Opinions and Experience from China Translated by Jafron Biomedical Co.,Ltd. 1 CONTENTS 1. Diagnosis and Treatment Scheme for Novel Coronavirus Pneumonia, 7th Edition………………………………………………………….…..3 2. Expert consensus: Application of Artificial Liver Blood Purification System in the Treatment of Severe and Critical Pneumonia Caused by Novel Coronavirus……………………..…………...…..…………….17 3. Expert consensus: Diagnosis and treatment of acute kidney injury associated with novel coronavirus infection…...…….……………….21 4. Expert consensus:The use of blood purification for severe and critical novel coronavirus pneumonia………………………………………...31 5. Coronavirus epidemic: preparing for extracorporeal organ support in intensive care………….……..………………………………………..42 2 Diagnosis and Treatment Scheme for Novel Coronavirus Pneumonia, 7th Edition Mar 3, 2020 National Health Commission of the People's Republic of China Original Document: http://www.nhc.gov.cn/yzygj/s7653p/202003/46c9294a7dfe4cef80dc7f5912eb1989.shtml _____________________________________________________________________ Since December 2019, Wuhan City, Hubei Province (China) has found several novel coronavirus pneumonia patients, with the spread of the epidemic, other parts of China and abroad have also found such cases. As an acute respiratory infectious disease, the disease has been included in the Class B infectious disease stipulated in the Law of the People's Republic of China on the Prevention and Control of Infectious Diseases, and to be managed as the Class A infectious disease. Through a series of preventive control and medical treatment measures, the rising trend of the epidemic situation in China has been curbed to a certain extent, and the epidemic situation in most provinces has been alleviated, but the number of cases abroad is on the rise. -

February 2020 ` 50 News from China China-India Review
Vol. XXXII | No.2 | February 2020 ` 50 NEWS FROM CHINA CHINA-INDIA REVIEW PEOPle’s WAR CHINA SHALL OVERCOME PEOPLE POWER MARCHING TOGETHER H.E. SUN WEIDONG From Ambassador’s Desk China’s Ambassador to India China Unites to Win People’s War nation’s strength is tested in difficult of the Political Bureau and decided to set up times. The Chinese leadership and the Central Leading Group on Responding to Apeople have united and joined hands to COVID-19 Outbreak. It has never happened defeat the deadly COVID-19 (novel coronavirus before in Chinese history to have this highest- pneumonia) epidemic. The Chinese government level meeting on the first day of the Spring has taken the most comprehensive, rigorous Festival. It demonstrated that for President Xi and thorough prevention and control measures. curbing the epidemic is foremost priority and We have been working literally 24x7 to win this he is ready to leave no stone unturned in this “People’s War,” as President Xi has said. mission. The results of these cumulative efforts show In this battle against the epidemic, we are a new dawn breaking through darkness. The reassured by growing international support recovery rate of COVID-19 patients in Hubei and solidarity with China. In this context, I will Province surged from 7.14% on Feb. 12 to 53.81% like to thank Prime Minister Narendra Modi on March 2. There is a sharp drop in the fatality for writing a letter to President Xi, expressing rate, with 3,728 patients in severe and critical India’s solidarity with China. -

China's Local Governments Are Combating COVID-19 With
Front. Med. 2020, 14(2): 220–224 https://doi.org/10.1007/s11684-020-0755-z COMMENTARY China’s local governments are combating COVID-19 with unprecedented responses ---- from a Wenzhou governance perspective Fanghua Gong1,2, Yong Xiong2, Jian Xiao1,2, Li Lin1,2, Xiaodong Liu3, Dezhong Wang2, Xiaokun Li (✉)1,2 1School of Pharmaceutical Sciences, Wenzhou Medical University, Wenzhou 325035, China; 2Biomedicine Collaborative Innovation Center, Wenzhou 325035, China; 3School of Public Health and Management, Wenzhou Medical University, Wenzhou 325035, China © Higher Education Press and Springer-Verlag GmbH Germany, part of Springer Nature 2020 Abstract The COVID-19 caused by a novel strain of coronavirus has been spreading rapidly since its occurrence in December 2019. It is highly communicable through human-to-human transmission. China has been making unprecedented efforts in treating the confirmed cases, identifying and isolating their close contacts and suspected cases to control the source of infection and cut the route of transmission. China’s devotion in handling this epidemic has effectively and efficiently curbed communication domestically and across the border. Representative measures adopted by Wenzhou, the worst hit city out of Hubei Province, are examined to elucidate those massive undertakings with the aim of enhancing international understanding and building global rapport in fighting this evolving epidemic situation. Keywords COVID-19; novel coronavirus pneumonia; 2019-nCoV; epidemic management Introduction COVID-19 cases have been reported in China with 4742 cured and 1114 deaths by midnight of February 11, 2020 A novel strain of coronavirus has caused a pneumonia [4] and an additional 441 confirmed cases overseas with 1 outbreak in the central Chinese city of Wuhan since death in the Philippines as of 17:30 on February 12, 2020 December 2019 and has been quickly spreading to other [5]. -
COVID-19 Image Data Collection
COVID-19 Image Data Collection Joseph Paul Cohen 1 2 Paul Morrison 3 Lan Dao 4 Abstract This paper describes the initial COVID-19 open image data collection. It was created by assem- bling medical images from websites and publi- cations and currently contains 123 frontal view X-rays. 1. Motivation In the context of a COVID-19 pandemic, is it crucial to (a) Day 10 (b) Day 13 streamline diagnosis. Data is the first step to developing any diagnostic tool or treatment. While there exist large public datasets of more typical chest X-rays (Wang et al., 2017; Bustos et al., 2019; Irvin et al., 2019; Johnson et al., 2019; Demner-Fushman et al., 2016), there is no collection of COVID-19 chest X-rays or CT scans designed to be used for computational analysis. In this paper, we describe the public database of pneumonia cases with chest X-ray or CT images, specifically COVID- 19 cases as well as MERS, SARS, and ARDS. Data will be (c) Day 17 (d) Day 25 collected from public sources in order not to infringe patient confidentiality. Example images shown in Figure1. Figure 1. Example images from the same patient (#19) extracted Our team believes that this database can dramatically im- from Cheng et al.(2020). This 55 year old female survived a prove identification of COVID-19. Notably, this would COVID-19 infection. provide essential data to train and test a Deep Learning- based system, likely using some form of transfer learning. These tools could be developed to identify COVID-19 char- pneumonia. -
Characterizing the COVID-19 Infodemic on Chinese Social Media: Exploratory Study
JMIR PUBLIC HEALTH AND SURVEILLANCE Zhang et al Original Paper Characterizing the COVID-19 Infodemic on Chinese Social Media: Exploratory Study Shuai Zhang1, PhD; Wenjing Pian2, PhD; Feicheng Ma1, MSc; Zhenni Ni1, BM; Yunmei Liu1, PhD 1School of Information Management, Wuhan University, Wuhan, China 2School of Economics and Management, Fuzhou University, Fuzhou, China Corresponding Author: Feicheng Ma, MSc School of Information Management Wuhan University No 299 Bayi Road, Wuchang District Wuhan, China Phone: 86 13507119710 Email: [email protected] Abstract Background: The COVID-19 infodemic has been disseminating rapidly on social media and posing a significant threat to people's health and governance systems. Objective: This study aimed to investigate and analyze posts related to COVID-19 misinformation on major Chinese social media platforms in order to characterize the COVID-19 infodemic. Methods: We collected posts related to COVID-19 misinformation published on major Chinese social media platforms from January 20 to May 28, 2020, by using PythonToolkit. We used content analysis to identify the quantity and source of prevalent posts and topic modeling to cluster themes related to the COVID-19 infodemic. Furthermore, we explored the quantity, sources, and theme characteristics of the COVID-19 infodemic over time. Results: The daily number of social media posts related to the COVID-19 infodemic was positively correlated with the daily number of newly confirmed (r=0.672, P<.01) and newly suspected (r=0.497, P<.01) COVID-19 cases. The COVID-19 infodemic showed a characteristic of gradual progress, which can be divided into 5 stages: incubation, outbreak, stalemate, control, and recovery.