Transfusion Services Test Name: TYPE and DIRECT COOMBS
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Transfusion Problems in Hemolytic Anemias*
Transfusion Problems in Hemolytic Anemias* ALI A. HOSSAIN! Department of Pathdlogy, Medical College of Virginia, Richmond 23219 All hemolytic anemias feature shortened red cell Extrinsic Mechanisms survival due to premature hemolysis of the cell. For the Those hemolytic anemias which are due to extrinsic purposes of this presentation, we may classify the factors may be classified, further, as non-immune or hemolytic anemias, most broadly, according to the immune. Non-immune mechanisms include a) drugs mechanisms leading to hemolysis. and chemicals (phenylhydrazine, naphthalene, lead, snake venoms); b) physical agents (heat); c) bacteria Intrinsic Mechanisms and parasites (hemolytic streptococci, Clostridium Hemolytic anemias due to intrinsically defective welchii, Bartonella, plasmodia); and d) acquired sen erythrocytes are essentially of three types. First are sitivity to penicillin, methylodopa, Keftin®, or fava those anemias in which the red cells are defective due plant as examples. Some of the agents in this. last to lack of an essential factor, eg, pernicious anemia group serve to lyse the cells, either through duect in relapse. The second type includes those in which action or by formation of antibodies. the red cells have an abnormal shape because of an These hemolytic anemias due to extrinsic factors inherited error in the chemical makeup of the hemo of the non-immune variety present no transfusion globin molecules; eg, sickle cells, elliptocytes, sphero problem for the Blood Bank. However, it ~~st b.e cytes, and the target -

Hemolytic Disease of the Newborn
Intensive Care Nursery House Staff Manual Hemolytic Disease of the Newborn INTRODUCTION and DEFINITION: Hemolytic Disease of the Newborn (HDN), also known as erythroblastosis fetalis, isoimmunization, or blood group incompatibility, occurs when fetal red blood cells (RBCs), which possess an antigen that the mother lacks, cross the placenta into the maternal circulation, where they stimulate antibody production. The antibodies return to the fetal circulation and result in RBC destruction. DIFFERENTIAL DIAGNOSIS of hemolytic anemia in a newborn infant: -Isoimmunization -RBC enzyme disorders (e.g., G6PD, pyruvate kinase deficiency) -Hemoglobin synthesis disorders (e.g., alpha-thalassemias) -RBC membrane abnormalities (e.g., hereditary spherocytosis, elliptocytosis) -Hemangiomas (Kasabach Merritt syndrome) -Acquired conditions, such as sepsis, infections with TORCH or Parvovirus B19 (anemia due to RBC aplasia) and hemolysis secondary to drugs. ISOIMMUNIZATION A. Rh disease (Rh = Rhesus factor) (1) Genetics: Rh positive (+) denotes presence of D antigen. The number of antigenic sites on RBCs varies with genotype. Prevalence of genotype varies with the population. Rh negative (d/d) individuals comprise 15% of Caucasians, 5.5% of African Americans, and <1% of Asians. A sensitized Rh negative mother produces anti-Rh IgG antibodies that cross the placenta. Risk factors for antibody production include 2nd (or later) pregnancies*, maternal toxemia, paternal zygosity (D/D rather than D/d), feto-maternal compatibility in ABO system and antigen load. (2) Clinical presentation of HDN varies from mild jaundice and anemia to hydrops fetalis (with ascites, pleural and pericardial effusions). Because the placenta clears bilirubin, the chief risk to the fetus is anemia. Extramedullary hematopoiesis (due to anemia) results in hepatosplenomegaly. -

Association Between ABO and Duffy Blood Types and Circulating Chemokines and Cytokines
Genes & Immunity (2021) 22:161–171 https://doi.org/10.1038/s41435-021-00137-5 ARTICLE Association between ABO and Duffy blood types and circulating chemokines and cytokines 1 2 3 4 5 6 Sarah C. Van Alsten ● John G. Aversa ● Loredana Santo ● M. Constanza Camargo ● Troy Kemp ● Jia Liu ● 4 7 8 Wen-Yi Huang ● Joshua Sampson ● Charles S. Rabkin Received: 11 February 2021 / Revised: 30 April 2021 / Accepted: 17 May 2021 / Published online: 8 June 2021 This is a U.S. government work and not under copyright protection in the U.S.; foreign copyright protection may apply 2021, corrected publication 2021 Abstract Blood group antigens are inherited traits that may play a role in immune and inflammatory processes. We investigated associations between blood groups and circulating inflammation-related molecules in 3537 non-Hispanic white participants selected from the Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial. Whole-genome scans were used to infer blood types for 12 common antigen systems based on well-characterized single-nucleotide polymorphisms. Serum levels of 96 biomarkers were measured on multiplex fluorescent bead-based panels. We estimated marker associations with blood type using weighted linear or logistic regression models adjusted for age, sex, smoking status, and principal components of p 1234567890();,: 1234567890();,: population substructure. Bonferroni correction was used to control for multiple comparisons, with two-sided values < 0.05 considered statistically significant. Among the 1152 associations tested, 10 were statistically significant. Duffy blood type was associated with levels of CXCL6/GCP2, CXCL5/ENA78, CCL11/EOTAXIN, CXCL1/GRO, CCL2/MCP1, CCL13/ MCP4, and CCL17/TARC, whereas ABO blood type was associated with levels of sVEGFR2, sVEGFR3, and sGP130. -

Blood Product Replacement: Obstetric Hemorrhage
CMQCC OBSTETRIC HEMORRHAGE TOOLKIT Version 2.0 3/24/15 BLOOD PRODUCT REPLACEMENT: OBSTETRIC HEMORRHAGE Richard Lee, MD, Los Angeles County and University of Southern California Medical Center Laurence Shields, MD, Marian Regional Medical Center/Dignity Health Holli Mason, MD, Cedars-Sinai Medical Center Mark Rollins, MD, PhD, University of California, San Francisco Jed Gorlin, MD, Innovative Blood Resources/Memorial Blood Center, St. Paul, Minnesota Maurice Druzin, MD, Lucile Packard Children’s Hospital Stanford University Jennifer McNulty, MD, Long Beach Memorial Medical Center EXECUTIVE SUMMARY • Outcomes are improved with early and aggressive intervention. • Both emergency blood release and massive transfusion protocols should be in place. • In the setting of significant obstetric hemorrhage, resuscitation transfusion should be based on vital signs and blood loss and should not be delayed by waiting for laboratory results. • Calcium replacement will often be necessary with massive transfusion due to the citrate used for anticoagulation in blood products. • During massive transfusion resuscitation, the patient’s arterial blood gas, electrolytes, and core temperature should be monitored to guide clinical management and all transfused fluids should be warmed; direct warming of the patient should be initiated as needed to maintain euthermia and to avoid added coagulopathy. BACKGROUND AND LITERATURE REVIEW After the first several units of packed red blood cells (PRBCs) and in the face of continuing or worsening hemorrhage, aggressive transfusion therapy becomes critical. This report covers the experience with massive transfusion protocols. Lessons from military trauma units as well as civilian experience with motor vehicle accidents and massive obstetric hemorrhage have identified new principles such as earlier use of plasma (FFP/thawed plasma/plasma frozen within 24 hours/liquid plasma) and resuscitation transfusion while laboratory results are pending. -

A Newly Recognized Blood Group in Domestic Shorthair Cats: the Mik Red Cell Antigen
J Vet Intern Med 2007;21:287–292 A Newly Recognized Blood Group in Domestic Shorthair Cats: The Mik Red Cell Antigen Nicole M. Weinstein, Marie-Claude Blais, Kimberly Harris, Donna A. Oakley, Lillian R. Aronson, and Urs Giger Background: Naturally occurring alloantibodies produced against A and B red cell antigens in cats can cause acute hemolytic transfusion reactions. Blood incompatibilities, unrelated to the AB blood group system, have also been suspected after blood transfusions through routine crossmatch testing or as a result of hemolytic transfusion reactions. Hypothesis: Incompatible crossmatch results among AB compatible cats signify the presence of a naturally occurring alloantibody against a newly identified blood antigen in a group of previously never transfused blood donor cats. The associated alloantibody is clinically important based upon a hemolytic transfusion reaction after inadvertent transfusion of red cells expressing this red cell antigen in a feline renal transplant recipient that lacks this red cell antigen. Methods: Blood donor and nonblood donor cats were evaluated for the presence of auto- and alloantibodies using direct antiglobulin and crossmatch tests, respectively, and were blood typed for AB blood group status. Both standard tube and novel gel column techniques were used. Results: Plasma from 3 of 65 cats and 1 feline renal transplant recipient caused incompatible crossmatch test results with AB compatible erythrocytes indicating these cats formed an alloantibody against a red cell antigen they lack, termed Mik. The 3 donors and the renal transplant recipient were crossmatch-compatible with one another. Tube and gel column crossmatch test results were similar. Conclusions and Clinical Importance: The absence of this novel Mik red cell antigen can be associated with naturally occurring anti-Mik alloantibodies and can elicit an acute hemolytic transfusion reaction after an AB-matched blood transfusion. -
Apheresis Donation This Quick Reference Guide Will Help You Identify the Best Donation for Your Unique Blood Type
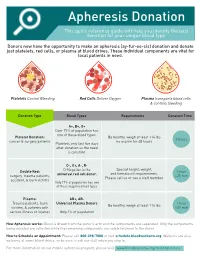
Apheresis Donation This quick reference guide will help you identify the best donation for your unique blood type. Donors now have the opportunity to make an apheresis (ay-fur-ee-sis) donation and donate just platelets, red cells, or plasma at blood drives. These individual components are vital for local patients in need. Platelets Control Bleeding Red Cells Deliver Oxygen Plasma transports blood cells & controls bleeding Donation Type Blood Types Requirements Donation Time A+, B+, O+ Over 75% of population has one of these blood types. Platelet Donation: Be healthy, weigh at least 114 lbs 2 hours cancer & surgery patients no aspirin for 48 hours Platelets only last five days after donation so the need is constant. O-, O+, A-, B- Special height, weight, Double Red: O-Negative is the 1 hour and hematocrit requirements. surgery, trauma patients, universal red cell donor. +25 min Please call us or see a staff member accident, & burn victims Only 17% of population has one of these negative blood types Plasma: AB+, AB- Trauma patients, burn Universal Plasma Donors 1 hour Be healthy, weigh at least 114 lbs victims, & patients with +30 min serious illness or injuries Only 4% of population How Apheresis works: Blood is drawn from the donor’s arm and the components are separated. Only the components being donated are collected while the remaining components are safely returned to the donor How to Schedule an Appointment: Please call 800-398-7888 or visit schedule.bloodworksnw.org. Walk-ins are also welcome at some blood drives, so be sure to ask our staff when you stop in. -

Blood Type and Transplantation & A2 Donor to B Recipient
Page 1 of 2 Blood Type and Transplantation Information for Kidney Transplant Patients Does blood type matter in transplantation? Everyone waiting for a transplant has their blood typed. You will have one of four blood types: O, A, B or AB. Your blood type is determined by the antigens that are present on your blood cells. These antigens are A or B. These antigens will be found both in your blood and on your organs. What antigen does each blood type have? Blood type O Blood type A Blood type B Blood type AB have no have A antigens. have B antigens. have both A O antigens. A B AB and B antigens. How does my body react to antigens? Your body will react to antigens that are different than your own by attacking with antibodies. Antibodies are proteins created by your immune system to attack anything that does not belong. Antibodies are the soldiers in your body’s army protecting you from foreign invasions such as viruses. Unfortunately, the antibodies cannot tell the difference between harmful viruses and beneficial transplanted organs. What blood type will my donor be? Transplants can occur between all blood types. However, when the donor’s blood type is different than yours and there are different antigens being transplanted on your new organ, your antibodies will be triggered and attack the transplanted organ. This is called rejection. Because of this, transplants usually happen between a donor and a recipient of the same blood type. This is called an identical transplant. Can I get an organ from a donor that has a different blood type than mine? Yes! If you do not have antibodies in your body against the antigens that come from the donor, your immune system should not attack the transplanted organ. -

Blood Bank I D
The Osler Institute Blood Bank I D. Joe Chaffin, MD Bonfils Blood Center, Denver, CO The Fun Just Never Ends… A. Blood Bank I • Blood Groups B. Blood Bank II • Blood Donation and Autologous Blood • Pretransfusion Testing C. Blood Bank III • Component Therapy D. Blood Bank IV • Transfusion Complications * Noninfectious (Transfusion Reactions) * Infectious (Transfusion-transmitted Diseases) E. Blood Bank V (not discussed today but available at www.bbguy.org) • Hematopoietic Progenitor Cell Transplantation F. Blood Bank Practical • Management of specific clinical situations • Calculations, Antibody ID and no-pressure sample questions Blood Bank I Blood Groups I. Basic Antigen-Antibody Testing A. Basic Red Cell-Antibody Interactions 1. Agglutination a. Clumping of red cells due to antibody coating b. Main reaction we look for in Blood Banking c. Two stages: 1) Coating of cells (“sensitization”) a) Affected by antibody specificity, electrostatic RBC charge, temperature, amounts of antigen and antibody b) Low Ionic Strength Saline (LISS) decreases repulsive charges between RBCs; tends to enhance cold antibodies and autoantibodies c) Polyethylene glycol (PEG) excludes H2O, tends to enhance warm antibodies and autoantibodies. 2) Formation of bridges a) Lattice structure formed by antibodies and RBCs b) IgG isn’t good at this; one antibody arm must attach to one cell and other arm to the other cell. c) IgM is better because of its pentameric structure. P}Chaffin (12/28/11) Blood Bank I page 1 Pathology Review Course 2. Hemolysis a. Direct lysis of a red cell due to antibody coating b. Uncommon, but equal to agglutination. 1) Requires complement fixation 2) IgM antibodies do this better than IgG. -

Autoimmune Hemolytic Anemia in COVID-19 Patients, the « Transmissible » Direct Coombs Test
J H C R JOURNAL OF HEMATOLOGY 2640-2823 AND CLINICAL RESEARCH Research Article More Information *Address for Correspondence: Alice Brochier, Hematology Department of Laboratory Medicine, Autoimmune hemolytic anemia in Saint-Luc University Hospital, Avenue Hippocrate 10, 1200 Brussels, Belgium, Tel: +322764 6814; COVID-19 patients, the « transmissible » Email: [email protected]; Véronique Deneys, Hematology Department of Laboratory Medicine, Saint-Luc University direct Coombs test Hospital, Avenue Hippocrate 10, 1200 Brussels, Belgium, Email: [email protected] Alice Brochier1*, Julien Cabo1, Claudine Guerrieri1, Leïla Belkhir2, Submitted: March 24, 2021 3 1 Pierre-François Laterre and Véronique Deneys * Approved: April 06, 2021 Published: April 07, 2021 1Hematology Department of Laboratory Medicine, Saint-Luc University Hospital, Brussels, Belgium 2Department of Internal Medicine and Infectious Diseases, Saint-Luc University Hospital, Brussels, How to cite this article: Brochier A, Cabo J, Guerrieri C, Belkhir L, Laterre PF, Deneys V. Belgium Autoimmune hemolytic anemia in COVID-19 3 Department of Intensive Care Medicine, Saint-Luc University Hospital, Brussels, Belgium patients, the « transmissible » direct Coombs test. J Hematol Clin Res. 2021; 5: 004-008. Abstract DOI: 10.29328/journal.jhcr.1001016 Copyright: © 2021 Brochier A, et al. This Background: Like other viruses, the SARS-CoV-2 (severe acute respiratory syndrome is an open access article distributed under coronavirus 2) appears to be responsible for several autoimmune complications. The occurrence the Creative Commons Attribution License, of autoimmune hemolytic anemia has been described in several case reports. This AIHA was also which permits unrestricted use, distribution, noticeable by the important number of blood transfusions required for COVID-19 (coronavirus and reproduction in any medium, provided the disease 2019) patients. -

The Johns Hopkins Comprehensive Transplant Center Incompatible Kidney Transplant Programs
The Johns Hopkins Comprehensive Transplant Center Incompatible Kidney Transplant Programs The Johns Hopkins Comprehensive Transplant Center’s Incompatible Kidney Transplantation Program allows many patients previously thought to be “incompatible” to receive the gift of life. The program is comprised of several elements: Blood Type Incompatible Kidney Transplant Program Positive Crossmatch and Sensitized Patient Program Paired Kidney Exhange Program Altruistic Donor Program Blood Type Incompatible Kidney Transplant Program More than one-third of willing live donors are turned down because their blood types are not compatible with the person to whom they wish to donate their kidney. Most of us have natural antibodies against organs from people with different blood types. These antibodies can rapidly destroy a transplanted kidney. The Blood Type Incompatible Transplant Program allows patients to receive a kidney from a live donor who has an incompatible blood type (see fig1.). Patients in this program must be willing to undergo all prescribed treatments before and after the transplant to remove harmful antibodies and decrease the risk of rejection. Figure 1: Blood Type Compatibility Chart Donor Recipient How are harmful antibodies removed? Harmful antibodies are removed with a process called plasmapheresis, a procedure similar to dialysis that removes the plasma portion of the blood where antibodies are located. The number of plasmapheresis treatments required by the recipient before surgery varies depending on the amount of harmful antibodies in their blood. After each plasmapheresis the recipient receives an intravenous infusion of immune globulin to replace antibodies needed to fight infections and help prevent harmful antibodies from returning. Once the antibodies against the donor’s blood type decrease to very low levels, the transplantation can take place. -

Direct Antibody Test (DAT) Positive
Direct antibody test (DAT) positive Information for patients, parents and guardians As part of your routine pregnancy screening, you However, only a small number of DAT positive have had a direct antibody test (DAT). We’ve babies will develop these problems. Babies given you this factsheet to explain what a DAT who are not DAT positive can still develop involves and what it means if your baby is DAT anaemia and jaundice. A positive DAT simply positive. If you have any further questions, tells us to look out for any signs of anaemia and please speak to a member of your healthcare jaundice. It does not necessarily mean that your team who will be pleased to advise you. baby will need treatment. What is a direct antibody test (DAT)? If we find out that you have rhesus negative During pregnancy, some of the blood between (Rh-) blood during pregnancy, we may give the mother and baby may mix. This mixing of you an injection called anti-D to stop your blood sometimes produces antibodies (proteins body making antibodies against your baby’s that are part of your body’s natural defences) blood. Occasionally this injection causes the which may become a problem for the baby. DAT result to come out positive. Babies who are DAT positive for this reason do not usually As part of routine antenatal (pregnancy) develop anaemia or jaundice. screening blood tests, your midwife will record your blood type (blood group) and check What is anaemia? whether your blood contains any antibodies Anaemia is a very common condition where the that may affect your baby’s red blood cells. -

Package Insert
Anti-Human Globulin Anti-IgG IH-Card AHG Anti-IgG (Rabbit)(Green)_____________________________________________________________________ English, B186359, Version 07, 2016.07 FOR IN VITRO DIAGNOSTIC USE Gel card for use with the IH-System MEETS FDA POTENCY REQUIREMENTS U.S. LICENSE NUMBER: 1845 Product-Identification: 74020 IH-Card AHG Anti-IgG: VOL 12 cards per box............ REF 813 420 100 VOL 48 cards per box............ REF 813 421 100 VOL 288cards per box........... REF 813 422 100 INTENDED USE The IH-Card AHG Anti-IgG is intended for the detection of antibodies on human red blood cells using the Direct and Indirect Antiglobulin Tests. SUMMARY Moreschi first described the use of Anti-Human Globulin in 1908.1 Coombs rediscovered the test in 1945.2,3 By injecting rabbits with human IgG, they were able to produce a protein (Anti-IgG) that reacted with ˝incomplete˝ antibodies (IgG). Most ˝incomplete˝ antibodies (IgG) fail to agglutinate red blood cells suspended in saline.4 Most clinically significant antibodies in red blood cell serology are of the IgG class and can only be detected by the use of Anti-IgG. The IH-Card AHG Anti-IgG is suitable for the Direct and Indirect Antiglobulin Tests. The Direct Antiglobulin Test allows the detection of in vivo sensitization of human red blood cells with immunoglobulins. The Indirect Antiglobulin Tests allows the detection of in vitro sensitization of human red blood cells with clinically significant antibodies. The Indirect Antiglobulin Test may be used for antibody detection, identification, IAT crossmatching , and D variant testing. An optional autocontrol may help to distinguish autoantibodies and alloantibodies.