Functional Vagotopy in the Cervical Vagus Nerve of the Domestic Pig: Implications for Vagus Nerve Stimulation
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
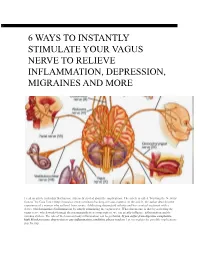
6 Ways to Instantly Stimulate Your Vagus Nerve to Relieve Inflammation, Depression, Migraines and More
O 6 WAYS TO INSTANTLY STIMULATE YOUR VAGUS NERVE TO RELIEVE INFLAMMATION, DEPRESSION, MIGRAINES AND MORE I read an article yesterday that has me extremely excited about the implications. The article is called “Hacking the Nervous System” by Gaia Vince (http://mosaicscience.com/story/hacking-nervous-system). In the article, the author describes the experience of a woman who suffered from severe, debilitating rheumatoid arthritis and her eventual treatment with a device which minimized inflammation by simply stimulating the vagus nerve. What this means, is that by activating the vagus nerve which works through the parasympathetic nervous system, we can greatly influence inflammation and the immune system. The role of the brain on body inflammation can be profound. If you suffer from digestive complaints, high blood pressure, depression or any inflammatory condition, please read on. Let me explain the possible implications step by step. What is the vagus nerve? First of all, the vagus nerve is the longest nerve in the body which originates in the brain as cranial nerve ten, travels down the from go the neck and then passes around the digestive system, liver, spleen, pancreas, heart and lungs. This nerve is a major player in the parasympathetic nervous system, which is the ‘rest and digest’ part (opposite to the sympathetic nervous system which is ‘fight of flight’). Vagal tone The tone of the vagus nerve is key to activating the parasympathetic nervous system. Vagal tone is measured by tracking your heart-rate alongside your breathing rate. Your heart-rate speeds up a little when your breathe in, and slows down a little when you breathe out. -

Questions and Answers About Vagus Nerve Stimulation by Jerry Shih, M.D. 1. WHAT IS VAGUS NERVE STIMULATION? Therapeutic Vagus Ne
Questions and Answers About Vagus Nerve Stimulation By Jerry Shih, M.D. 1. WHAT IS VAGUS NERVE STIMULATION? Therapeutic vagus nerve stimulation (VNS) is chronic, intermittent electrical stimulation of the mid-cervical segment of the left vagus nerve. The stimulation occurs automatically at set intervals, during waking and sleep. The electrical pulses are generated by a pacemaker-like device that is implanted below the clavicle and are delivered by a lead wire that is coiled around the vagus nerve. 2. WHAT IS THE EVIDENCE THAT VAGUS NERVE STIMULATION IS EFFECTIVE IN EPILEPSY? The empirical evidence of antiepileptic efficacy arose sequentially from l) experiments in animal models of epilepsy; 2) anecdotal reports and small case series ofearly human trials, and 3) two prospec-tive, double-blind, controlled studies in large groups of patients with complex partial and secondarily generalized seizures. 3. HOW DOES VAGUS NERVE STIMULATION CONTROL SEIZURES? The mechanisms by which therapeutic VNS reduces seizure activity in humans and in experimental models of epilepsy are unknown. 4. WHEN SHOULD ONE CONSIDER VAGUS NERVE STIMULATION? Medically refractory complex partial and secondarily generalized seizures have been efficaciously treated with adjunctive VNS in the large, randomized studies. Children may benefit considerably from VNS, but large-scale, randomized, controlled studies have not been completed in young children. Thus, any adolescent or adult whose complex partial or secondarily generalized seizures have not been controlled with the appropriate first- and second -line antiepileptic drugs may be a good candidate for VNS. The FDA has specifically approved VNS with the Cyberonics device for adjunctive therapy of refractory partial-onset seizures in persons l2 years of age. -

Current Neurosurgical Management of Glossopharyngeal Neuralgia and Technical Nuances for Microvascular Decompression Surgery
Neurosurg Focus 34 (3):E8, 2013 ©AANS, 2013 Current neurosurgical management of glossopharyngeal neuralgia and technical nuances for microvascular decompression surgery ROBERTO REY-DIOS, M.D.,1 AND AARON A. COHEN-GADOL, M.D., M.SC.2 1Department of Neurosurgery, University of Mississippi Medical Center, Jackson, Mississippi; 2Goodman Campbell Brain and Spine, Indiana University Department of Neurological Surgery, Indianapolis, Indiana Glossopharyngeal neuralgia (GPN) is an uncommon facial pain syndrome often misdiagnosed as trigeminal neuralgia. The rarity of this condition and its overlap with other cranial nerve hyperactivity syndromes often leads to a significant delay in diagnosis. The surgical procedures with the highest rates of pain relief for GPN are rhizotomy and microvascular decompression (MVD) of cranial nerves IX and X. Neurovascular conflict at the level of the root exit zone of these cranial nerves is believed to be the cause of this pain syndrome in most cases. Vagus nerve rhizotomy is usually reserved for cases in which vascular conflict is not evident. A review of the literature reveals that although the addition of cranial nerve X rhizotomy may improve the chances of long-term pain control, this maneuver also increases the risk of permanent dysphagia and vocal cord paralysis. The risks of this procedure have to be carefully weighed against its benefits. Based on the authors’ experience, careful patient selection with a thorough exploratory operation most often leads to identification of the site of vascular conflict, obviating the need for cranial nerve X rhizotomy. (http://thejns.org/doi/abs/10.3171/2012.12.FOCUS12391) KEY WORDS • glossopharyngeal neuralgia • microvascular decompression • vagus nerve • rhizotomy • cranial nerve LOSSOPHARYNGEAL neuralgia, or vagoglossopharyn impairment can be found in the distribution of the above geal neuralgia, is a cranial nerve hyperactivity nerves due to structural lesions.20 This classification does pain syndrome leading to severe, transient, sharp not take into consideration associated syncopal events. -

Glossopharyngeal and Vagal Neuralgia
BRITISH 26 August 1967 MEDICAL JOURNAL 529 Br Med J: first published as 10.1136/bmj.3.5564.529 on 26 August 1967. Downloaded from Glossopharyngeal and Vagal Neuralgia JAGDISH C. CHAWLA,* F.R.C.S.; MURRAY A. FALCONERt M.CH. F.R.C.S. Brit. med. J., 1967, 3, 529-531 Tic douloureux involving the glossopharyngeal nerve is rare (1945) did record two cases in which, after intracranial section and when it does occur probably often involves the vagus nerve of the glossopharyngeal nerve alone, pain persisted, but it as well. Many cases are undoubtedly not recognized, and yet disappeared after a second operation in which the upper vagal the condition responds favourably and permanently to intra- rootlets were cut, an experience which Bohm and Strang (1962) cranial section of the glossopharyngeal nerve and upper fila- also shared. Wilson and McAlpine (1946) reported a single ments of the vagus nerve. We therefore propose to review the case in which the glossopharyngeal nerve had been dissected in literature, discuss our own experiences, and try to clarify the its tonsillar bed and avulsed with relief. Our experience, how- clinical syndromes that this condition presents and the surgical ever, suggests that recurrence can arise after this procedure, approach that is required. and has led us to recommend intracranial section of the glosso- pharyngeal nerve plus section of the upper two vagal rootlets. Review of the Literature Present Series The condition of glossopharyngeal neuralgia was first described by Weisenburg (1910), who recognized it in a patient This study is based on a review of 10 patients admitted to with a tumour of the cerebellopontine angle. -

Practical Approaches to Dysphagia Caused by Esophageal Motor Disorders Amindra S
Practical Approaches to Dysphagia Caused by Esophageal Motor Disorders Amindra S. Arora, MB BChir and Jeffrey L. Conklin, MD Address nonspecific esophageal motor disorders (NSMD), diffuse Division of Gastroenterology and Hepatology, Mayo Clinic, esophageal spasm (DES), nutcracker esophagus (NE), 200 First Street SW, Rochester, MN 55905, USA. hypertensive lower esophageal sphincter (hypertensive E-mail: [email protected] LES), and achalasia [1••,3,4••,5•,6]. Out of all of these Current Gastroenterology Reports 2001, 3:191–199 conditions, only achalasia can be recognized by endoscopy Current Science Inc. ISSN 1522-8037 Copyright © 2001 by Current Science Inc. or radiology. In addition, only achalasia has been shown to have an underlying distinct pathologic basis. Recent data suggest that disorders of esophageal motor Dysphagia is a common symptom with which patients function (including LES incompetence) affect nearly present. This review focuses primarily on the esophageal 20% of people aged 60 years or over [7••]. However, the motor disorders that result in dysphagia. Following a brief most clearly defined motility disorder to date is achalasia. description of the normal swallowing mechanisms and the Several studies reinforce the fact that achalasia is a rare messengers involved, more specific motor abnormalities condition [8•,9]. However, no population-based studies are discussed. The importance of achalasia, as the only exist concerning the prevalence of most esophageal motor pathophysiologically defined esophageal motor disorder, disorders, and most estimates are derived from people with is discussed in some detail, including recent developments symptoms of chest pain and dysphagia. A recent review of in pathogenesis and treatment options. Other esophageal the epidemiologic studies of achalasia suggests that the spastic disorders are described, with relevant manometric worldwide incidence of this condition is between 0.03 and tracings included. -

Chapter 18 CRANIAL NERVE INJURIES
Cranial Nerve Injuries Chapter 18 CRANIAL NERVE INJURIES † ‡ SCOTT B. ROOFE, MD, FACS*; CAROLINE M. KOLB, MD ; AND JARED SEIBERT, MD INTRODUCTION CRANIAL NERVE V CRANIAL NERVE VII Evaluation Imaging Electrodiagnostic Testing Eye Care Nerve Exploration Nerve Repair Interposition Grafting Intratemporal Injuries Facial Nerve Decompression LOWER CRANIAL NERVES, IX THROUGH XII CRANIAL NERVE IX CRANIAL NERVE X CRANIAL NERVE XI CRANIAL NERVE XII SUMMARY CASE PRESENTATIONS Case Study 18-1 Case Study 18-2 *Colonel, Medical Corps, US Army; Program Director, Otolaryngology Residency, Tripler Army Medical Center, 1 Jarrett White Road, Honolulu, Hawaii 96859-5000; Assistant Professor of Surgery, Uniformed Services University of the Health Sciences †Major, Medical Corps, US Army; Staff Otolaryngologist, Fort Belvoir Community Hospital, 9300 Dewitt Loop, Fort Belvoir, Virginia 20112 ‡Captain, Medical Corps, US Army; Otolaryngology Resident, Tripler Army Medical Center, 1 Jarrett White Road, Honolulu, Hawaii 96859-5000 213 Otolaryngology/Head and Neck Combat Casualty Care INTRODUCTION Injuries to the head and neck rank as some of the cal to maximizing the outcomes for these patients. most common injuries suffered in the current combat The otolaryngologist clearly has a vital role in the environment. These injuries often lead to extensive management of nearly all cranial nerve injuries. bony and soft tissue disruption, which places the cra- However, in the combat environment, this specialty nial nerves at increased risk for damage. Functional generally focuses on deficits arising from cranial deficits of any of these nerves can be devastating to nerves VII and VIII as well as the lower cranial nerves, both appearance and function. Due to the complex IX through XII. -

Rebuilding Body–Brain Interaction from the Vagal Network in Spinal Cord Injuries
brain sciences Perspective Rebuilding Body–Brain Interaction from the Vagal Network in Spinal Cord Injuries Maria Luisa De Martino 1,2,† , Mina De Bartolo 1,†, Erik Leemhuis 1,2 and Mariella Pazzaglia 1,2,* 1 Department of Psychology, Sapienza University of Rome, Via dei Marsi 78, 00185 Rome, Italy; [email protected] (M.L.D.M.); [email protected] (M.D.B.); [email protected] (E.L.) 2 Body and Action Lab, IRCCS Fondazione Santa Lucia, Via Ardeatina 306, 00179 Rome, Italy * Correspondence: [email protected]; Tel.: +39-6-49917633 † These authors contributed equally to this work. Abstract: Spinal cord injuries (SCIs) exert devastating effects on body awareness, leading to the disruption of the transmission of sensory and motor inputs. Researchers have attempted to improve perceived body awareness post-SCI by intervening at the multisensory level, with the integration of somatic sensory and motor signals. However, the contributions of interoceptive-visceral inputs, particularly the potential interaction of motor and interoceptive signals, remain largely unaddressed. The present perspective aims to shed light on the use of interoceptive signals as a significant resource for patients with SCI to experience a complete sense of body awareness. First, we describe intero- ceptive signals as a significant obstacle preventing such patients from experiencing body awareness. Second, we discuss the multi-level mechanisms associated with the homeostatic stability of the body, which creates a unified, coherent experience of one’s self and one’s body, including real-time updates. Body awareness can be enhanced by targeting the vagus nerve function by, for example, applying Citation: De Martino, M.L.; De transcutaneous vagus nerve stimulation. -

How to Stimulate Your Vagus Nerve for Better Mental Health Adapted from - January 21, 2017 Jordan Fallis
How to Stimulate Your Vagus Nerve for Better Mental Health Adapted from - January 21, 2017 Jordan Fallis “By developing an understanding of the workings of your vagus nerve, you may find it possible to work with your nervous system rather than feel trapped when it works against you.” — Dr. Arielle Schwartz, Clinical Psychologist Stimulating my vagus nerve has played a key role in the management of my mental health over the years. What exactly is the vagus nerve? The vagus nerve is the longest nerve in your body. It connects your brain to many important organs throughout the body, including the gut (intestines, stomach), heart and lungs. In fact, the word "vagus" means “wanderer” in Latin, which accurately represents how the nerve wanders all over the body and reaches various organs. The vagus nerve is also a key part of your parasympathetic “rest and digest” nervous system. It influences your breathing, digestive function and heart rate, all of which can have a huge impact on your mental health. But what you really need to pay special attention to is the "tone" of your vagus nerve. Vagal tone is an internal biological process that represents the activity of the vagus nerve. Increasing your vagal tone activates the parasympathetic nervous system, and having higher vagal tone means that your body can relax faster after stress. In 2010, researchers discovered a positive feedback loop between high vagal tone, positive emotions, and good physical health. In other words, the more you increase your vagal tone, the more your physical and mental health will improve, and vice versa (5). -

Cranial Nerves
Cranial Nerves Cranial nerve evaluation is an important part of a neurologic exam. There are some differences in the assessment of cranial nerves with different species, but the general principles are the same. You should know the names and basic functions of the 12 pairs of cranial nerves. This PowerPage reviews the cranial nerves and basic brain anatomy which may be seen on the VTNE. The 12 Cranial Nerves: CN I – Olfactory Nerve • Mediates the sense of smell, observed when the pet sniffs around its environment CN II – Optic Nerve Carries visual signals from retina to occipital lobe of brain, observed as the pet tracks an object with its eyes. It also causes pupil constriction. The Menace response is the waving of the hand at the dog’s eye to see if it blinks (this nerve provides the vision; the blink is due to cranial nerve VII) CN III – Oculomotor Nerve • Provides motor to most of the extraocular muscles (dorsal, ventral, and medial rectus) and for pupil constriction o Observing pupillary constriction in PLR CN IV – Trochlear Nerve • Provides motor function to the dorsal oblique extraocular muscle and rolls globe medially © 2018 VetTechPrep.com • All rights reserved. 1 Cranial Nerves CN V – Trigeminal Nerve – Maxillary, Mandibular, and Ophthalmic Branches • Provides motor to muscles of mastication (chewing muscles) and sensory to eyelids, cornea, tongue, nasal mucosa and mouth. CN VI- Abducens Nerve • Provides motor function to the lateral rectus extraocular muscle and retractor bulbi • Examined by touching the globe and observing for retraction (also tests V for sensory) Responsible for physiologic nystagmus when turning head (also involves III, IV, and VIII) CN VII – Facial Nerve • Provides motor to muscles of facial expression (eyelids, ears, lips) and sensory to medial pinna (ear flap). -

The Vagus Nerve and Its Home, the Nervous System Viva La Vagus!
Viva La Vagus! by Miriam van Mersbergen Lights, music, excitement: that is what We have ample evidence that voice ceived reality (e.g. sight and hearing).6 Las Vegas has to offer. The bustle of the training provides excellent protection The basic unit in the nervous system Vegas Strip dazzles and amazes. In all the from injury and harm and have begun is called a nerve. Its main function is to drama of that city, however, little atten- to develop sophisticated motor theories communicate.7 Nerves contain three tion is given to the electricity that lights especially for voice production.2 Our basic parts: a cell body called a soma, it up. When one thinks of Las Vegas, they multi-disciplinary perspective of voice dendrites that carry information from may conjure many images, but probably science frequently takes for granted the other structures (other nerves, glands, none will be of the power cords that nerve that supplies the vocal folds with muscles, etc . .) to the soma, and axons, make that city run. power and gives them life. which carry information away from the Similarly, when we wax eloquent or soma to the next structure.8 The relay transcend through singing, we rarely of messages along these nerves can give thought to the power cord mak- The Vagus Nerve and its Home, be simple as a refl ex.9 However, nerve ing all of our efforts possible. Over the the Nervous System communication is often much more past fi fty years we have developed rich The nervous system is the commu- complicated, involving many nerves voice training traditions, sophisticated nication network of our body. -

Vagus Nerve Stimulation
Corporate Medical Policy Vagus Nerve Stimulation File Name: va gus_nerve_stimulation Origination: 6/1998 Last CAP Review: 5/2021 Next CAP Review: 5/2022 Last Review: 5/2021 Description of Procedure or Service Stimulation of the vagus nerve can be performed using a pulsed electrical stimula tor implanted within the carotid artery sheath. This technique has been proposed as a treatment for refractory seizures, depression and other disorders. There are also devices available that are implanted at different areas of the vagus nerve. Vagus nerve stimulation (VNS) wa s initia lly investigated as a treatment alternative in patients with medically refractory partial-onset seizures for whom surgery is not recommended or for whom surgery has failed. Over time, the use of VNS has expanded to generalized seizures, and it has been investigated for a range of other conditions. While the mechanisms for the therapeutic effects of vagal nerve stimulation are not fully understood, the basic premise of VNS in the treatment of various conditions is that vagal visceral afferents have a diffuse central nervous system projection, and activation of these pathways has a widespread effect on neuronal excitability. Electrical stimulus is applied to axons of the vagus nerve, which have their cell bodies in the nodose and junctional ganglia and synapse on the nucleus of the solitary tract in the brainstem. From the solitary tract nucleus, vagal afferent pathways project to multiple areas of the brain. There are also vagal efferent pathways that innervate the heart, vocal cords, and other laryngeal and pharyngeal muscles, and provide parasympathetic innervation to the gastrointestinal tract that may also be stimulated by VNS. -

The 12 Cranial Nerves
The 12 Cranial Nerves Nerve # Name Function 1st Olfactory Relays smell 2nd Optic Transmits visual information 3rd Oculomotor External muscles of the eye 4th Trochlear Also supplies muscles of the eye 5th Trigeminal Chewing and sensation in the face 6th Abducent Controls lateral eye movement 7th Facial Muscles of facial expression, taste buds, sensation in fingers and toes, blinking 8th Auditory Hearing and balance 9th Glossopharyngeal Sensation, taste and swallowing 10th Vagus Organs in chest and abdomen 11th Accessory Supplies two neck muscles, the sternomastoid and trapezius 12th Hypoglossal Muscles of the tongue and neck The 12 Cranial Nerves—Detail Cranial Nerve 1 Sensory nerve – Olfactory Nerve – controls sense of smell Cranial Nerve 2 Sensory nerve- Optic Nerve- controls vision by sending information from retina Cranial Nerve 3 Motor nerve- Oculomotor Nerve-Controls most eye muscles. Works closely with Cranial Nerves 4 & 6. Controls eye movement, pupil dilation, and pupillary constriction. It also controls the muscles that elevate the upper eyelids. Cranial Nerve 4 Motor nerve- Trochlear Nerve- Controls the downward and outward movement of the eye. Works closely with Cranial Nerves 3 & 6. Can cause vertical Diplopia (double vision). Weakness of downward gaze can cause difficulty in descending stairs. Cranial Nerve 5 Motor and sensory nerve-Trigeminal Nerve-Carries sensory information from most of the head, neck, sinuses, and face. Also carries sensory information for ear and tympanic membrane. Provides motor supply to the muscles of masticulation (chewing), and to some of the muscles on the floor of the mouth. Also provides motor supply to tensor tympani (small muscle in the middle ear which tenses to protect the eardrum).