Tarsometatarsal Joint Sprain
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Tarsometatarsal Joint Injury/Arthritis John P
Tarsometatarsal joint injury/arthritis John P. Negrine FRACS Foot and ankle surgeon Dr John Negrine Adult Foot and Ankle surgeon Lisfranc injury • Named after a Napoleonic surgeon who didn’t actually describe the injury – he described am amputation through the joints Dr John Negrine Adult Foot and Ankle surgeon Jacques Lisfranc de St. Martin • 1790 – 1847 • “A surgeon and gynaecologist” • Trained as an assistant to Guillaume Dupuytren • “Pioneered operations including removal of the rectum, lithotomy in women as well as amputation of the cervix” Dr John Negrine Adult Foot and Ankle surgeon What do we call the “Lisfranc joints?” • The tarsometatarsal joints • Anatomy well known to you • The second metatarsal base is recessed and the strong ligament is on the plantar surface connecting the medial cuneiform to the base of the second metatarsal…the “Lisfranc ligament” Dr John Negrine Adult Foot and Ankle surgeon Lisfranc anatomy Dr John Negrine Adult Foot and Ankle surgeon Common injury • Commonly missed • Commonly underestimated • Long time to recovery • Don’t always do well! Dr John Negrine Adult Foot and Ankle surgeon Common ‐ ?Really? • No not really! • 0.2% of fractures • 1:70,000 people in a hospital catchment area • 20% are missed Dr John Negrine Adult Foot and Ankle surgeon Mechanism of injury • 43% Motor vehicle accidents • 24% from falls, jumps or twisting injury • 13% due to crush injury Dr John Negrine Adult Foot and Ankle surgeon Important to differentiate High velocity vs low velocity Dr John Negrine Adult Foot and Ankle surgeon -

Efficacy of Ultrasound Imaging in the Evaluation of the Lisfranc Joint Complex
Efficacy of Ultrasound Imaging in the Evaluation of the Lisfranc Joint Complex THESIS Presented in Partial Fulfillment of the Requirements for the Degree Master of Science in the Graduate School of The Ohio State University By Meridith Kay DeLuca, B.S. Graduate Program in Anatomy The Ohio State University 2018 Master's Examination Committee: Laura C. Boucher, PhD, ATC (Advisor) Christopher Pierson, MD, PhD Bryant Walrod, MD Copyright by Meridith Kay DeLuca 2018 Abstract Lisfranc injuries account for 1 in 55,000 injuries yearly and are associated with poor outcomes and high complication rates. Located between the medial cuneiform and second metatarsal, the dorsal Lisfranc ligament is easily visualized with ultrasonography. Ultrasound can provide quick, cost effective diagnosis of pathology, but is not standardized in practice. The purpose of this study was to compare measurement accuracy of the dorsal Lisfranc ligament between ultrasound and gross dissection with an additional anatomic study of the complex, including the dorsal, interosseous, and plantar Lisfranc ligaments. Ultrasound images of 22 embalmed cadaveric feet (11 male, 7 female, 80.3 years ± 14.03) were obtained using a Sonosite M-Turbo ultrasound machine. The dorsal Lisfranc ligament was imaged and measured using a 6-13MHz linear array. Images were measured a second time using ImageJ software. Specimens were then dissected to evaluate the dorsal, interosseous, and plantar Lisfranc ligaments. Dorsal ligament measurements were compared between methodologies, and morphology of the joint complex was also recorded. Differences in measurement of the dorsal Lisfranc ligament between ultrasound imaging (8.39 mm ± 1.26) and gross dissection (10.80 mm ± 1.85) were significant (p < 0.001). -
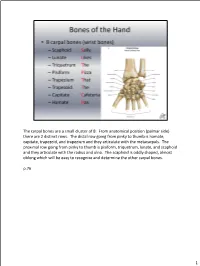
The Carpal Bones Are a Small Cluster of 8. from Anatomical Position (Palmar Side) There Are 2 Distinct Rows
The carpal bones are a small cluster of 8. From anatomical position (palmar side) there are 2 distinct rows. The distal row going from pinky to thumb is hamate, capitate, trapezoid, and trapezium and they articulate with the metacarpals. The proximal row going from pinky to thumb is pisiform, triquetrum, lunate, and scaphoid and they articulate with the radius and ulna. The scaphoid is oddly shaped, almost oblong which will be easy to recognize and determine the other carpal bones. p.76 1 Radiocarpal ligaments (palmar and dorsal)--Connects radius to carpal bones Intercarpal ligaments (palmar and dorsal)--Connects carpal bones to each other Collateral ligaments (ulnar and radial)--Ulnar collateral ligament and radial collateral ligament connect the forearm to the wrist and help support the sides of the wrist as well There are radiocarpal ligaments and intercarpal ligaments on both the dorsal and palmar sides of the hand. p.78 2 So for the middle phalanges there are only #2-5 since the thumb does not have a middle phalange. The proximal phalange and middle phalange articulation is called the proximal interphalangeal joint and the middle phalange articulating with the distal phalange is called the distal interphalangeal joint. With the thumb there is only 1 interphalangeal joint since it’s just the proximal and distal phalange. p.77 3 p.77 4 The radiocarpal joint is where the carpals articulate with the radius (condyloid joint). The intercarpal joints are the gliding joints between the carpals. The 1st carpometacarpal joint is the thumb, which is a saddle joint, but the 2nd-5th carpometacarpal joints are gliding. -

Ligamentous Lisfranc Injuries in the Athlete Craig Thomas Haytmanek Jr., MD, and Thomas O
Ligamentous Lisfranc Injuries in the Athlete Craig Thomas Haytmanek Jr., MD, and Thomas O. Clanton, MD Ligamentous injuries to the midfoot during athletic endeavors are becoming more common and more troublesome as they can take significant time before the athlete is able to return to play. Late changes in alignment or posttraumatic arthritis are complications of inadequate treatment. The mechanism of injury is either direct impact to the dorsal midfoot or a twisting injury to the hindfoot with a plantar-flexed, fixed forefoot. Examination reveals ecchymosis and pain in the midfoot. Rarely is there enough instability to allow detection on physical examination. Provocative tests such as external rotation stress of the midfoot or physical activity (single leg hop or walking on tip toes) can recreate symptoms if the patient’spain allows for it. Weight-bearing anteroposterior and lateral radiographic examination of both feet focusing on the midfoot is essential, allowing comparison between the injured and uninjured extremity. Diastasis between the proximal first and second metatarsal is a classic radiographic finding, but proximal extension between the cuneiforms can also be present. A more severe injury shows loss of the longitudinal arch or subluxation of the midfoot that is identified on a lateral radiograph. A tear or an avulsion of Lisfranc ligament along with other midfoot ligaments is the underlying pathology. Advanced imaging modalities including computed tomography and magnetic resonance imaging are useful in these more subtle injuries or when more specific anatomical detail is required. Nondisplaced injuries are typically treated conserva- tively with a period of non–weight bearing followed by a gradual return-to-play protocol. -

Calcaneocuboid and Naviculocuneiform Dislocation: an Unusual Injury of the Midfoot
Hindawi Case Reports in Orthopedics Volume 2020, Article ID 8818823, 8 pages https://doi.org/10.1155/2020/8818823 Case Report Calcaneocuboid and Naviculocuneiform Dislocation: An Unusual Injury of the Midfoot Anne Kummer ,1 Xavier Crevoisier,2 and Antoine Eudier 1 1Hôpital Intercantonal de la Broye (HIB), Payerne, Switzerland 2Lausanne University Hospital (CHUV), Switzerland Correspondence should be addressed to Antoine Eudier; [email protected] Received 26 May 2020; Accepted 20 September 2020; Published 28 September 2020 Academic Editor: Paul E. Di Cesare Copyright © 2020 Anne Kummer et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Introduction. Midfoot dislocations are rare traumatic injuries. The best known patterns involve the Lisfranc and Chopart joints, although some other types have been described. Dislocations that occur at the level of the naviculocuneiform and calcaneocuboid joints simultaneously represent a very rare configuration of dislocation. Case Presentation. A 34-year-old man sustained a crush injury to his left foot causing a complete dislocation through the naviculocuneiform and calcaneocuboid joints. Immediate closed reduction and percutaneous pinning were performed, followed by open reduction and stabilization of both joints two weeks later. Anatomical reduction was obtained, and the clinical outcome remained satisfactory 10 months after surgery. Discussion. Anatomical reduction is essential to obtain favorable outcomes in traumatic midfoot injuries. An unusual pattern of midfoot dislocation can be treated according to the same principles as those for classical Lisfranc or Chopart injuries. 1. Introduction We report a case of unusual dislocation of the midfoot, since the dislocation pattern occurred through the calcaneo- Traumatic injuries and dislocations of the midfoot are com- cuboid and naviculocuneiform joints. -

Lisfranc Injury: Imaging Findings for This Important but Often-Missed Diagnosis
Lisfranc Injury: Imaging Findings for this Important but Often-Missed Diagnosis Rajan T. Gupta, MD,a Rakhee P. Wadhwa, MD,b Thomas J. Learch, MD, b and Steven M. Herwick, MDa The Lisfranc injury is a popular topic in the radiology, emergency medicine literature. Much of the litera- orthopedic surgery, and emergency medicine literature, ture has focused on the injury’s frequency and primarily due to the subtleties of the radiographic find- potential long-term complications. The purpose of ings and potentially dire consequences of missed diag- noses. The purpose of this article is to help readers this article is to describe the mechanism of injury, understand the anatomy of the tarsometatarsal joint, identify key radiographic findings, and illustrate identify a systematic approach for the evaluation of the how computed tomography (CT) and magnetic res- joint, and demonstrate how a multimodality approach onance (MR) can be used as diagnostic aids in can be used in both straightforward and more complex complex cases. cases. Specifically, the utility of lateral and weight- The Lisfranc joint bears the name of a field bearing radiographs as well as computed tomography and magnetic resonance will be addressed. The dorso- surgeon in Napoleon’s army, Jacques Lisfranc, who plantar radiograph is often the first radiological exami- described a technique for amputation of the forefoot 1 nation performed, after initial history and physical ex- through the tarsometatarsal joint. Multiple authors, amination. An understanding of the anatomy of the including Cassebaum,2 have noted that fractures or normal Lisfranc joint and subtle findings in the abnormal dislocations at the tarsometatarsal joint were never joint is essential in making an accurate diagnosis. -

Applied Anatomy of the Lower Leg, Ankle and Foot
Applied anatomy of the lower leg, ankle and foot CHAPTER CONTENTS • Varus–valgus: these movements occur at the subtalar Definitions . e287 joint. In valgus, the calcaneus is rotated outwards on the talus; in varus, the calcaneus is rotated inwards on the The .leg . e287 talus. Anterolateral compartment . e287 • Abduction–adduction: these take place at the midtarsal Lateral compartment . e288 joints. Abduction moves the forefoot laterally and Posterior compartment . e288 adduction moves the forefoot medially on the midfoot. The .ankle .and .foot . e289 • Pronation–supination are also movements at the midtarsal joints. In pronation, the forefoot is rotated big toe The posterior segment . e289 downwards and little toe upwards. In supination, the The middle segment . e291 reverse happens: the big toe rotates upwards and the little The anterior segment . e293 toe downwards. Sometimes the terms internal rotation Muscles .and .tendons . e294 and external rotation are used to indicate supination or pronation. Plantiflexors . e294 • Inversion–eversion: these are combinations of three Dorsiflexors . e295 movements. In inversion, the varus movement at the Invertors (adduction–supination) . e295 subtalar joint is combined with an adduction and Evertors (abduction–pronation) . e295 supination movement at the midtarsal joint. During Intrinsic muscles . e296 eversion, a valgus movement at the subtalar joint is combined with an abduction and pronation movement at The .plantar .fascia . e297 the midtarsal joint. The .heel .pad . e298 The leg The bones (tibia and fibula) together with the interosseous Definitions membrane and fasciae divide the leg into three separate com- partments: anterolateral, lateral and posterior. They contain The functional terminology in the foot is very misleading, the so-called extrinsic foot muscles. -
Post-Traumatic Arthritis of the Tarsometatarsal Joint Complex: a Case Report
Open Access Case Report DOI: 10.7759/cureus.923 Post-traumatic Arthritis of the Tarsometatarsal Joint Complex: A Case Report Chirag Kapoor 1 , Amit Patel 1 , Maulik Jhaveri 1 , Paresh Golwala 1 1. Orthopaedics, Sumandeep Vidyapeeth, Vadodara, Gujarat Corresponding author: Chirag Kapoor, [email protected] Abstract Tarsometatarsal (TMT) arthritis is characterized by instability and pain in the foot. The commonest cause is post-traumatic arthritis. A Lisfranc injury involves the articulation between the medial cuneiform and the base of the second metatarsal, which is considered a keystone to midfoot integrity. Neglected or undertreated injury to the Lisfranc joint complex leads to secondary arthritis and significant disability. We present a case of a young male patient with a two-year-old neglected Lisfranc joint injury and secondary osteoarthritis of the first, second, and fourth TMT joints, which we treated surgically with arthrodesis using screws, with a good functional outcome on final follow-up. Categories: Medical Physics, Pain Management, Orthopedics Keywords: osteoarthritis, arthrodesis, tarsometatarsal joint Introduction Tarsometatarsal (TMT) arthritis is characterized by midfoot instability, pain, and severe functional impairment. The most common cause is post-traumatic arthritis, followed by primary osteoarthritis and other inflammatory processes. Injury to the TMT joint complex occurs in one in 55,000 persons per year, which accounts for 0.2% of all fractures, and up to 20% of the cases are undiagnosed and left untreated [1]. The most common area of involvement is from Lisfranc injuries, resulting in degeneration of the first, second, and fourth TMT joints [2]. The Lisfranc joint injury pattern is notorious for developing secondary arthritis if left untreated or treated with incongruity. -
Midfoot Arthritis
A Review Paper Midfoot Arthritis Siraj A. Sayeed, MD, Fazel A. Khan, MD, Norman S. Turner III, MD, and Harold B. Kitaoka, MD vicular ligaments; in some cases, a true synovial joint is Abstract present rather than this syndesmosis.1 Foot and ankle complaints are commonly encountered The joints between the cuneiforms and the first to third in orthopedic practice. Midfoot arthritis has the poten- metatarsal and between the cuboid and the fourth and tial to cause a significant amount of pain and disabil- fifth metatarsals collectively comprise the Lisfranc joint. ity. A variety of conditions can cause or lead to midfoot At this location, both the proximal and distal bones com- arthritis. Treatment consists of either conservative man- prising the joint are arranged in the coronal plane in the agement or surgical arthrodesis of the painful joints. In this article, we review the midfoot (its basic anatomy form of an arch. Formation of this arch is mediated both and biomechanics) and midfoot arthritis (its clinical pre- by bony anatomy and by soft-tissue reinforcement. All sentation and etiology, radiographic evaluation, and treat- the cuneiforms are wedge-shaped, with their narrow por- ment options). tions being plantar, thus allowing for the arch configura- tion. The corresponding arch configuration of the meta- idfoot arthritis, a specific complaint in adults, tarsal bases is depicted in Figure 1. As shown, the second has the potential to cause a significant amount metatarsal base assumes the position of keystone. This of pain and disability. Yet, the literature specifi- geometry gives the midfoot inherent stability. In addition cally on midfoot arthritis is scant. -
Management of Tarsometatarsal Joint Injuries
Review Article Management of Tarsometatarsal Joint Injuries Abstract Brian M. Weatherford, MD Joint disruptions to the tarsometatarsal (TMT) joint complex, also John G. Anderson, MD known as the Lisfranc joint, represent a broad spectrum of pathology from subtle athletic sprains to severe crush injuries. Although injuries Donald R. Bohay, MD, FACS to the TMT joint complex are uncommon, when missed, they may lead to pain and dysfunction secondary to posttraumatic arthritis and arch collapse. An understanding of the appropriate anatomy, mechanism, physical examination, and imaging techniques is necessary to diagnose and treat injuries of the TMT joints. Nonsurgical management is indicated in select patients who maintain reduction of the TMT joints under physiologic stress. Successful surgical management of these injuries is predicated on anatomic reduction and stable fixation. Open reduction and internal fixation remains the standard treatment, although primary arthrodesis has emerged as a viable option for certain types of TMT joint injuries. he tarsometatarsal (TMT), or these injuries often result in painful TLisfranc, joint complex is com- posttraumatic arthritis and arch posed of the TMT, intertarsal, and collapse. Early diagnosis and main- proximal intermetatarsal joints.1 The tenance of anatomic reduction of the unique osseous anatomy of the TMT joints are necessary to maxi- midfoot along with the stout liga- mize patient function. JAAOS Plus Webinar mentous support allows effective Nevertheless, appropriate initial Join Dr. Weatherford, Dr. Anderson, force transfer from the hindfoot to treatment of TMT injuries is contro- and Dr. Bohay for the interactive the forefoot during ambulation. versial. A variety of techniques have JAAOS Plus Webinar discussing “Management of Tarsometatarsal Joint Injuries to the TMT joint complex are been described for the management Injuries,” on Tuesday, July 11, 2017, at rare, accounting for only 0.2% of all of TMT injuries, but rates of post- 8 pm Eastern Time. -

Anatomy of the Foot and Ankle Multimedia Health Education
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Gastrointestinal Surgery Advanced Laparoscopic Surgery Hernia Surgery Surgical Oncology Endoscopy Anatomy Of The Foot And Ankle Multimedia Health Education Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about management of the Foot and Ankle must be made in conjunction with your Physician or a licensed healthcare provider. Mufa T. Ghadiali, M.D., F.A.C.S Diplomate of American Board of Surgery 6405 North Federal Hwy., Suite 402 Fort Lauderdale, FL 33308 Tel.: 954-771-8888 Fax: 954- 491-9485 www.ghadialisurgery.com Anatomy Of The Foot And Ankle Multimedia Health Education MULTIMEDIA HEALTH EDUCATION MANUAL TABLE OF CONTENTS SECTION CONTENT 1 . ANATOMY a. Ankle & Foot Anatomy b. Soft Tissue Anatomy 2 . BIOMECHANICS www.ghadialisurgery.com Anatomy Of The Foot And Ankle Multimedia Health Education Unit 1: Anatomy Introduction The foot and ankle in the human body work together to provide balance, stability, movement, and Propulsion. This complex anatomy consists of: 26 bones 33 joints Muscles Tendons Ligaments Blood vessels, nerves, and soft tissue In order to understand conditions that affect the foot and ankle, it is important to understand the normal anatomy of the foot and ankle. Ankle The ankle consists of three bones attached by muscles, tendons, and ligaments that connect the foot to the leg. In the lower leg are two bones called the tibia (shin bone) and the fibula. -
Biomechanical Model of the Human Foot: Kinematics and Kinetics During the Stance Phase of Walking
See discussions, stats, and author profiles for this publication at: http://www.researchgate.net/publication/14791400 Biomechanical model of the human foot: Kinematics and kinetics during the stance phase of walking ARTICLE in JOURNAL OF BIOMECHANICS · OCTOBER 1993 Impact Factor: 2.75 · DOI: 10.1016/S0021-9290(05)80008-9 · Source: PubMed CITATIONS READS 103 402 2 AUTHORS, INCLUDING: Stephen H Scott Queen's University 137 PUBLICATIONS 4,403 CITATIONS SEE PROFILE All in-text references underlined in blue are linked to publications on ResearchGate, Available from: Stephen H Scott letting you access and read them immediately. Retrieved on: 29 October 2015 J. Biomechanics Vol. 26, No. 9, pp. 1091 1104, 1993. 0021-9290/93 $6.00+.00 Printed in Great Britain 9 1993 Pergamon Press Ltd BIOMECHANICAL MODEL OF THE HUMAN FOOT: KINEMATICS AND KINETICS DURING THE STANCE PHASE OF WALKING STEPHEN H. SCOTT*? and DAVID A. WINTER~w *Department of Systems Design Engineering; and ~Department of Kinesiology, University of Waterloo, Waterloo, Ontario N2L 3G1, Canada Abstract--A model of the human foot is proposed in which the foot is represented as eight rigid segments and eight monocentric, single-degree-of-freedom joints. The soft tissue under tile foot is divided into seven independent sites of contact, or loading, and each of these is modelled as a nonlinear spring and a nonlinear damper in-parallel. The model was used to estimate the kinematics and kinetics'of the foot during the stance phase of walking. The force sustained at each loading site was calculated from walking trials in which only portions of the foot landed on a small force platform.