S2 Table. List of Syntax for 96 Diseases
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

82858686.Pdf
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Frontiers - Publisher Connector MINI REVIEW published: 23 March 2017 doi: 10.3389/fimmu.2017.00336 Adaptive Immunity Is the Key to the Understanding of Autoimmune and Paraneoplastic inflammatory Central Nervous System Disorders Robert Weissert* Department of Neurology, Neuroimmunology, University of Regensburg, Regensburg, Germany There are common aspects and mechanisms between different types of autoimmune diseases such as multiple sclerosis (MS), neuromyelitis optica spectrum disorders (NMOSDs), and autoimmune encephalitis (AE) as well as paraneoplastic inflammatory disorders of the central nervous system. To our present knowledge, depending on the disease, T and B cells as well as antibodies contribute to various aspects of the pathogenesis. Possibly the events leading to the breaking of tolerance between the different diseases are of great similarity and so far, only partially understood. Beside Edited by: endogenous factors (genetics, genomics, epigenetics, malignancy) also exogenous fac- Björn Tackenberg, tors (vitamin D, sun light exposure, smoking, gut microbiome, viral infections) contribute Philipps University of Marburg, Germany to susceptibility in such diseases. What differs between these disorders are the target Reviewed by: molecules of the immune attack. For T cells, these target molecules are presented on Anne Kathrin Mausberg, major histocompatibility complex (MHC) molecules as MHC-bound ligands. B cells have Essen University Hospital, Germany Pavan Bhargava, an important role by amplifying the immune response of T cells by capturing antigen with Johns Hopkins School of Medicine, their surface immunoglobulin and presenting it to T cells. Antibodies secreted by plasma USA cells that have differentiated from B cells are highly structure specific and can have *Correspondence: important effector functions leading to functional impairment or/and lesion evolvement. -

A Radiologic Score to Distinguish Autoimmune Hypophysitis from Nonsecreting Pituitary ORIGINAL RESEARCH Adenoma Preoperatively
A Radiologic Score to Distinguish Autoimmune Hypophysitis from Nonsecreting Pituitary ORIGINAL RESEARCH Adenoma Preoperatively A. Gutenberg BACKGROUND AND PURPOSE: Autoimmune hypophysitis (AH) mimics the more common nonsecret- J. Larsen ing pituitary adenomas and can be diagnosed with certainty only histologically. Approximately 40% of patients with AH are still misdiagnosed as having pituitary macroadenoma and undergo unnecessary I. Lupi surgery. MR imaging is currently the best noninvasive diagnostic tool to differentiate AH from V. Rohde nonsecreting adenomas, though no single radiologic sign is diagnostically accurate. The purpose of this P. Caturegli study was to develop a scoring system that summarizes numerous MR imaging signs to increase the probability of diagnosing AH before surgery. MATERIALS AND METHODS: This was a case-control study of 402 patients, which compared the presurgical pituitary MR imaging features of patients with nonsecreting pituitary adenoma and controls with AH. MR images were compared on the basis of 16 morphologic features besides sex, age, and relation to pregnancy. RESULTS: Only 2 of the 19 proposed features tested lacked prognostic value. When the other 17 predictors were analyzed jointly in a multiple logistic regression model, 8 (relation to pregnancy, pituitary mass volume and symmetry, signal intensity and signal intensity homogeneity after gadolin- ium administration, posterior pituitary bright spot presence, stalk size, and mucosal swelling) remained significant predictors of a correct classification. The diagnostic score had a global performance of 0.9917 and correctly classified 97% of the patients, with a sensitivity of 92%, a specificity of 99%, a positive predictive value of 97%, and a negative predictive value of 97% for the diagnosis of AH. -

Interstitial Granuloma Annulare Triggered by Lyme Disease
Volume 27 Number 5| May 2021 Dermatology Online Journal || Case Presentation 27(5):11 Interstitial granuloma annulare triggered by Lyme disease Jordan Hyde1 MD, Jose A Plaza1,2 MD, Jessica Kaffenberger1 MD Affiliations: 1Division of Dermatology, The Ohio State University Wexner Medical Center, Columbus, Ohio, USA, 2Department of Pathology, The Ohio State University Wexner Medical Center, Columbus, Ohio, USA Corresponding Author: Jessica Kaffenberger MD, Division of Dermatology, The Ohio State University Medical Wexner Medical Center, Suite 240, 540 Officenter Place, Columbus, OH 43230, Tel: 614-293-1707, Email: [email protected] been associated with a variety of systemic diseases Abstract including diabetes mellitus, malignancy, thyroid Granuloma annulare is a non-infectious disease, dyslipidemia, and infection [3,4]. granulomatous skin condition with multiple different associations. We present a case of a man in his 60s There are multiple histological variants of GA, with a three-week history of progressive targetoid including interstitial GA. The histopathology of plaques on his arms, legs, and trunk. Skin biopsy classic GA demonstrates a focal degeneration of demonstrated interstitial granuloma annulare. collagen surrounded by an inflammatory infiltrate Additional testing revealed IgM antibodies to Borrelia composed of lymphocytes and histiocytes. In a less burgdorferi on western blot suggesting interstitial common variant, interstitial GA, scattered histiocytes granuloma annulare was precipitated by the recent are seen -

2017 Oregon Dental Conference® Course Handout
2017 Oregon Dental Conference® Course Handout Nasser Said-Al-Naief, DDS, MS Course 8125: “The Mouth as The Body’s Mirror: Oral, Maxillofacial, and Head and Neck Manifestations of Systemic Disease” Thursday, April 6 2 pm - 3:30 pm 2/28/2017 The Mouth as The Body’s Mirror Oral Maxillofacial and Head and Neck Manifestation of Ulcerative Conditions of Allergic & Immunological Systemic Disease the Oro-Maxillofacial Diseases Region Nasser Said-Al-Naief, DDS, MS Professor & Chair, Oral Pathology and Radiology Director, OMFP Laboratory Oral manifestations of Office 503-494-8904// Direct: 503-494-0041 systemic diseases Oral Manifestations of Fax: 503-494-8905 Dermatological Diseases Cell: 1-205-215-5699 Common Oral [email protected] Conditions [email protected] OHSU School of Dentistry OHSU School of Medicine 2730 SW Moody Ave, CLSB 5N008 Portland, Oregon 97201 Recurrent aphthous stomatitis (RAS) Recurrent aphthous stomatitis (RAS) • Aphthous" comes from the Greek word "aphtha”- • Recurrence of one or more painful oral ulcers, in periods of days months. = ulcer • Usually begins in childhood or adolescence, • The most common oral mucosal disease in North • May decrease in frequency and severity by age America. (30+). • Affect 5% to 66% of the North American • Ulcers are confined to the lining (non-keratinized) population. mucosa: • * 60% of those affected are members of the • Buccal/labial mucosa, lateral/ventral tongue/floor of professional class. the mouth, soft palate/oropharyngeal mucosa • Etiopathogenesis: 1 2/28/2017 Etiology of RAU Recurrent Aphthous Stomatitis (RAS): Types: Minor; small size, shallow, regular, preceeded by prodrome, heal in 7-10 days Bacteria ( S. -

A Patient with Plaque Type Morphea Mimicking Systemic Lupus Erythematosus
CASE REPORT A Patient With Plaque Type Morphea Mimicking Systemic Lupus Erythematosus Wardhana1, EA Datau2 1 Department of Internal Medicine, Siloam International Hospitals. Karawaci, Indonesia. 2 Department of Internal Medicine, Prof. Dr. RD Kandou General Hospital & Sitti Maryam Islamic Hospital, Manado, North Sulawesi, Indonesia. Correspondence mail: Siloam Hospitals Group’s CEO Office, Siloam Hospital Lippo Village. 5th floor. Jl. Siloam No.6, Karawaci, Indonesia. email: [email protected] ABSTRAK Morfea merupakan penyakit jaringan penyambung yang jarang dengan gambaran utama berupa penebalan dermis tanpa disertai keterlibatan organ dalam. Penyakit ini juga dikenal sebagai bagian dari skleroderma terlokalisir. Berdasarkan gambaran klinis dan kedalaman jaringan yang terlibat, morfea dikelompokkan ke dalam beberapa bentuk dan sekitar dua pertiga orang dewasa dengan morfea mempunyai tipe plak. Produksi kolagen yang berlebihan oleh fibroblast merupakan penyebab kelainan pada morfea dan mekanisme terjadinya aktivitas fibroblast yang berlebihan ini masih belum diketahui, meskipun beberapa mekanisme pernah diajukan. Morfe tipe plak biasanya bersifat ringan dan dapat sembuh dengan sendirinya. Morfea tipe plak yang penampilan klinisnya menyerupai lupus eritematosus sistemik, misalnya meliputi alopesia dan ulkus mukosa di mulut, jarang dijumpai. Sebuah kasus morfea tipe plak pada wanita berusia 20 tahun dibahas. Pasien ini diobati dengan imunosupresan dan antioksidan local maupun sistemik. Kondisi paisen membaik tanpa disertai efek samping yang berarti. Kata kunci: morfea, tipe plak. ABSTRACT Morphea is an uncommon connective tissue disease with the most prominent feature being thickening or fibrosis of the dermal without internal organ involvement. It is also known as a part of localized scleroderma. Based on clinical presentation and depth of tissue involvement, morphea is classified into several forms, and about two thirds of adults with morphea have plaque type. -
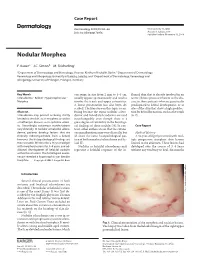
Nodular Morphea
Case Report Dermatology 2009;218:63–66 Received: July 13, 2008 DOI: 10.1159/000173976 Accepted: July 23, 2008 Published online: November 13, 2008 Nodular Morphea a b c F. Kauer J.C. Simon M. Sticherling a b Department of Dermatology and Venerology, Vivantes Klinikum Neukölln, Berlin , Department of Dermatology, c Venerology and Allergology, University of Leipzig, Leipzig , and Department of Dermatology, Venerology and Allergology, University of Erlangen, Erlangen , Germany Key Words can range in size from 2 mm to 4–5 cm, flamed skin that is already involved in an -Scleroderma ؒ Keloid ؒ Hypertrophic scar ؒ usually appear spontaneously and tend to active fibrotic process inherent to the dis Morphea involve the trunk and upper extremities. ease in those patients who are genetically A linear presentation has also been de- predisposed to keloid development, or at scribed. The literature on this topic is con- sites of the skin that show a high predilec- Abstract fusing because the terms ‘nodular sclero- tion for keloid formation, such as the trunk Scleroderma may present as being strictly derma’ and ‘keloidal scleroderma’ are used [6, 7] . limited to the skin, as in morphea, or within interchangeably even though there is a a multiorgan disease, as in systemic sclero- great degree of variability in the histologi- sis. Accordingly, cutaneous manifestations cal findings of these nodules [4] . In con- C a s e R e p o r t vary clinically. In nodular or keloidal sclero- trast, other authors stress that the cutane- derma, patients develop lesions that are ous manifestations may vary clinically, but Medical History clinically indistinguishable from a keloid; all share the same histopathological pat- A 16-year-old girl presented with mul- however, the histopathological findings are tern of both morphea/scleroderma and ke- tiple progressive morpheic skin lesions more variable. -

Rituximab Monotherapy and Rituximab-Containing
J Clin Exp Hematop Vol. 55, No. 2, Nov. 2015 Case Study Rituximab Monotherapy and Rituximab-Containing Chemotherapy Were Effective for Paraneoplastic Pemphigus Accompanying Follicular Lymphoma, but not for Subsequent Bronchiolitis Obliterans Taichi Hirano,1) Yusuke Higuchi,1) Hiromichi Yuki,1) Shinya Hirata,1) Kisato Nosaka,1) Norito Ishii,2) Takashi Hashimoto,2) Hiroaki Mitsuya,1) and Yutaka Okuno1) A 60-year-old male patient suffered from mild exertional dyspnea, wheezing, and systemic blisters. He was diagnosed with paraneoplastic pemphigus (PNP) with follicular lymphoma in the pancreas head and pelvic cavity. He was first treated with eight cycles of rituximab; his blisters and erosions gradually improved and highly elevated levels of auto-antibodies related to PNP gradually decreased to normal levels. However, obstructive and restrictive respiratory failure still progressed. Computed tomography of the inspiratory and expiratory phases revealed obstructive pulmonary disorder, leading to a diagnosis of bronchiolitis obliterans (BO). The patient underwent plasma exchange and was repeatedly treated with rituximab monotherapy and rituximab-containing chemotherapies, but died 7 months after the diagnosis of BO. Early introduction of rituximab- containing regimens may be necessary to prevent the development of BO accompanying PNP. However, when a diagnosis of PNP-related BO is made, lung transplantation may also be considered for patients in whom rituximab-containing regimens are effective for PNP. 〔J Clin Exp Hematop 55(2) : 83-88, 2015〕 Keywords: follicular lymphoma, paraneoplastic pemphigus, bronchiolitis obliterans, rituximab Without control of the malignant neoplasms, resolution of the INTRODUCTION skin blisters is difficult and requires high doses of cortico- Paraneoplastic pemphigus (PNP) is a systemic autoim- steroids and immunosuppressive drugs. -

Paraneoplastic Pemphigus: an Unusual Neoplasm Association
erimenta xp l D E e r & m l a a t c o i l n o i Journal of Clinical & Experimental Toosi et al. J Clin Exp Dermatol Res 2011, 2:4 l g y C f R DOI: 10.4172/2155-9554.1000124 o e l ISSN: 2155-9554 s a e n a r r u c o h J Dermatology Research Case Report Open Access Paraneoplastic Pemphigus: An Unusual Neoplasm Association Parviz Toosi1, Zahra Asadi Kani2, Mehdi Qeisari2 and Nastaran Namazi3* 1Professor of dermatology, Skin research center, Shohad-e-Tajrish hospital, Shahid Beheshti university of medical science, Tehran, Iran 2Dermatopathologist, Skin research center, Shohad-e-Tajrish hospital, Shahid Beheshti university of medical science, Tehran, Iran 3Resident of dermatology, Skin research center, Shohad-e-Tajrish hospital, Shahid Beheshti university of medical science, Tehran, Iran Abstract The occurrence of paraneoplastic pemphigus (PNP) in childhood has been reported infrequently. Association with benign mesentry tumors has not been reported in these patients before. Here, we report an unusual case of PNP in a child that was concomitant with benign mesentry fibroma and responded to medical treatment only after surgical excision of tumor. Keywords: Paraneoplastic pemphigus; Neoplasm association; Here we report an unusual case of childhood paraneoplastic Benign tumor; Mesentry fibroma pemphigus in association with benign mesocolon fibroma that responded to tumor excision dramatically. Introduction Case Report PNP, described by Anhalt et al. in 1990, is an IgG-mediated disease, characterized clinically by polymorphous eruption with prominent A 12 year old girl was referred to our dermatology clinic because mucosal and acral involvement in the presence of a known or occult of painful mucosal erosions from one month ago, made her unable neoplasm. -

Autoimmune Adrenal Insufficiency in Celiac Disease
International Journal of Celiac Disease, 2016, Vol. 4, No. 3, xx Available online at http://pubs.sciepub.com/ijcd/4/3/5 ©Science and Education Publishing DOI:10.12691/ijcd-4-3-5 Autoimmune Adrenal Insufficiency in Celiac Disease Hugh J Freeman* Department of Medicine (Gastroenterology), UBC Hospital, Vancouver, BC, Canada *Corresponding author: [email protected] Abstract Celiac disease is an immune-mediated intestinal disorder that may be associated with other immune- mediated extra-intestinal disorders, including immune-mediated endocrine diseases, such as autoimmune thyroiditis, most often with hypothyroidism. Other monoglandular autoimmune endocrine disorders may also occur, including autoimmune adrenal insufficiency (Addison’s disease). In celiac disease, clinical features of adrenal failure may be limited, difficult to differentiate from symptoms that might be attributed to celiac disease, or even life-threatening. In others with celiac disease, a polyglandular autoimmune syndrome has also been reported. Recent screening studies from multiple countries, particularly in Europe, have indicated that patients with autoimmune adrenal failure or Addison’s disease should be carefully screened for occult or silent celiac disease. Up to 10% of Addisonian patients may be serologically positive and histopathological features of untreated celiac disease may be detected, even with clinically occult intestinal disease. Celiac disease patients with a monoglandular autoimmune disorder should also be followed carefully for the later appearance of other autoimmune endocrine disorders as these may not all appear at the time of diagnosis of celiac disease, but sporadically during the life-long clinical course of celiac disease. Keywords: Addison’s Disease, Autoimmune Adrenal Insufficiency, Celiac Disease, Hypothyroidism, Polyglandular Endocrine Failure Cite This Article: Hugh J Freeman, “Autoimmune Adrenal Insufficiency in Celiac Disease.” International Journal of Celiac Disease, vol. -

Case Report Follicular Lymphoma with Paraneoplastic Pemphigus As the First Symptom: a Case Report and Review of the Literature
Int J Clin Exp Pathol 2020;13(7):1915-1923 www.ijcep.com /ISSN:1936-2625/IJCEP0112784 Case Report Follicular lymphoma with paraneoplastic pemphigus as the first symptom: a case report and review of the literature Shishou Wu1,2, Dong Gao3, Yuanfeng Zhang4, Ping Yang2, Yunjun Wang1,2, Ning Wang2, Jianfeng Xu5, Guohua Yu1,2 1Department of Clinical Medicine, Binzhou Medical University, Yantai, China; Departments of 2Pathology, 3Dermo- tology, 4Hematology, 5Respiratory Medicine, Affiliated Yantai Yuhuangding Hospital, Qingdao University, Yantai, China Received April 18, 2020; Accepted June 3, 2020; Epub July 1, 2020; Published July 15, 2020 Abstract: Paraneoplastic pemphigus (PNP) is an autoimmune bullous dermatosis associated with tumors, first de- scribed by Anhalt et al. in 1990. Reports of paraneoplastic pemphigus complicated by follicular lymphoma (FL) are rare in the medical literature. Here, we retrospectively analyze a case of PNP accompanied by FL. The patient was a 54-year-old woman who suffered from PNP associated with FL at the beginning. She had received a pathological diagnosis and was treated with R-CHOP and other drugs. Her mucosal lesions and cutaneous lesions improved, and the FL was in remission. Eleven months later, she died of BO after receiving the diagnosis of PNP. We also review most of the studies and reports about PNP accompanied by FL. We list the clinicopathologic features, therapeutic schedule, and prognosis in order to improve hematologists’ understanding and treatment of the diseases. Keywords: Follicular lymphoma, paraneoplastic pemphigus, bronchiolitis obliterans Introduction Bronchiolitis obliterans (BO) is a life-threaten- ing form of irreversible, obstructive lung dis- PNP is a rare paraneoplastic, systemic autoim- ease. -

Novel Autoantigens in Autoimmune Hypophysitis
Clinical Endocrinology (2008) 69, 269 –278 doi: 10.1111/j.1365-2265.2008.03180.x ORIGINAL ARTICLE NovelBlackwell Publishing Ltd autoantigens in autoimmune hypophysitis Isabella Lupi*, Karl W. Broman†, Shey-Cherng Tzou*, Angelika Gutenberg*‡, Enio Martino§ and Patrizio Caturegli*¶ *Department of Pathology, The Johns Hopkins University, School of Medicine, Baltimore, MD, USA, †Department of Biostatistics and Medical Informatics, University of Wisconsin, Madison, WI, USA, ‡Department of Neurosurgery, Georg-August University, Göttingen, Germany, §Department of Endocrinology and Metabolism, University of Pisa, Pisa, Italy and ¶Feinstone Department of Molecular Microbiology and Immunology, The Johns Hopkins Bloomberg School of Public Health, Baltimore, MD, USA although the performance was still inadequate to make immuno- Summary blotting a clinically useful test. Conclusion The study reports two novel proteins that could act Background Pituitary autoantibodies are found in autoimmune as autoantigens in autoimmune hypophysitis. Further studies are hypophysitis and other conditions. They are a marker of pituitary needed to validate their pathogenic role and diagnostic utility. autoimmunity but currently have limited clinical value. The methods used for their detection lack adequate sensitivity and (Received 8 November 2007; returned for revision 5 December 2007; specificity, mainly because the pathogenic pituitary autoantigen(s) finally revised 20 December 2007; accepted 20 December 2007) are not known and therefore antigen-based immunoassays have -

Hypophysitis
3 179 M N Joshi and others Hypophysitis 179:3 R151–R163 Review MECHANISMS IN ENDOCRINOLOGY Hypophysitis: diagnosis and treatment Mamta N Joshi1, Benjamin C Whitelaw2,3 and Paul V Carroll1,3 Correspondence 1Department of Endocrinology, Guy’s & St. Thomas’ NHS Foundation Trust, London, UK, 2Department of should be addressed Endocrinology, Kings College Hospital NHS Foundation Trust, London, UK, and 3Faculty of Life Sciences & Medicine, to P V Carroll King’s College Hospital London, London, UK Email [email protected] Abstract Hypophysitis is a rare condition characterised by inflammation of the pituitary gland, usually resulting in hypopituitarism and pituitary enlargement. Pituitary inflammation can occur as a primary hypophysitis (most commonly lymphocytic, granulomatous or xanthomatous disease) or as secondary hypophysitis (as a result of systemic diseases, immunotherapy or alternative sella-based pathologies). Hypophysitis can be classified using anatomical, histopathological and aetiological criteria. Non-invasive diagnosis of hypophysitis remains elusive, and the use of currently available serum anti-pituitary antibodies are limited by low sensitivity and specificity. Newer serum markers such as anti-rabphilin 3A are yet to show consistent diagnostic value and are not yet commercially available. Traditionally considered a very rare condition, the recent recognition of IgG4-related disease and hypophysitis as a consequence of use of immune modulatory therapy has resulted in increased understanding of the pathophysiology of hypophysitis. Modern imaging techniques, histological classification and immune profiling are improving the accuracy of the diagnosis of the patient with hypophysitis. The objective of this review is to bring readers up-to- date with current understanding of conditions presenting as hypophysitis, focussing on recent advances and areas for future development.