Immunizing Children Against Hepatitis B -- a Training Module
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Introduction of Inactivated Poliovirus Vaccine and Impact on Vaccine- Associated Paralytic Poliomyelitis — Beijing, China, 2014–2016
Morbidity and Mortality Weekly Report Introduction of Inactivated Poliovirus Vaccine and Impact on Vaccine- Associated Paralytic Poliomyelitis — Beijing, China, 2014–2016 Dan Zhao, MD1; Rui Ma, MD1; Tao Zhou, MD1; Fan Yang, MD1; Jin Wu, MD2; Hao Sun3; Fang Liu, MD4; Li Lu, MD1; Xiaomei Li1; Shuyan Zuo, MD5; Wei Yao6; JianYin6 When included in a sequential polio vaccination schedule, the risk for VAPP associated with subsequent OPV doses. inactivated polio vaccine (IPV) reduces the risk for vaccine- Countries that have previously introduced at least 1 IPV dose associated paralytic poliomyelitis (VAPP), a rare adverse event before vaccination with OPV have rapidly eliminated VAPP associated with receipt of oral poliovirus vaccine (OPV). (1). IPV has been available in China’s private sector since During January 2014, the World Health Organization (WHO) 2009. After completion of immunogenicity studies (3–5), recommended introduction of at least 1 IPV dose into routine Beijing introduced IPV into the public sector EPI program in immunization schedules in OPV-using countries (1). The December 2014 as part of a sequential schedule that included Polio Eradication and Endgame Strategic Plan 2013–2018 1 dose of IPV at age 2 months, followed by 3 doses of trivalent recommended completion of IPV introduction in 2015 and OPV at ages 3, 4, and 48 months. After the global synchronized globally synchronized withdrawal of OPV type 2 in 2016 (2). withdrawal of all Sabin type 2 vaccines in April 2016, trivalent Introduction of 1 dose of IPV into Beijing’s Expanded Program OPV was replaced with bivalent OPV, which contains types 1 on Immunization (EPI) on December 5, 2014 represented and 3 oral polio vaccine viruses. -

Valuing the Cost of Improving Chilean Primary Vaccination: a Cost Minimization Analysis of a Hexavalent Vaccine
Olivera et al. BMC Health Services Research (2020) 20:295 https://doi.org/10.1186/s12913-020-05115-7 RESEARCH ARTICLE Open Access Valuing the cost of improving Chilean primary vaccination: a cost minimization analysis of a hexavalent vaccine Ignacio Olivera1, Carlos Grau1, Hugo Dibarboure2, Juan Pablo Torres3, Gustavo Mieres1, Luis Lazarov1, Fabián P. Alvarez4 and Juan Guillermo López Yescas5* Abstract Background: The phased withdrawal of oral polio vaccine (OPV) and the introduction of inactivated poliovirus vaccine (IPV) is central to the polio ‘end-game’ strategy. Methods: We analyzed the cost implications in Chile of a switch from the vaccination scheme consisting of a pentavalent vaccine with whole-cell pertussis component (wP) plus IPV/OPV vaccines to a scheme with a hexavalent vaccine with acellular pertussis component (aP) and IPV (Hexaxim®) from a societal perspective. Cost data were collected from a variety of sources including national estimates and previous vaccine studies. All costs were expressed in 2017 prices (US$ 1.00 = $Ch 666.26). Results: The overall costs associated with the vaccination scheme (4 doses of pentavalent vaccine plus 1 dose IPV and 3 doses OPV) from a societal perspective was estimated to be US$ 12.70 million, of which US$ 8.84 million were associated with the management of adverse events related to wP. In comparison, the cost associated with the 4-dose scheme with a hexavalent vaccine (based upon the PAHO reference price) was US$ 19.76 million. The cost of switching to the hexavalent vaccine would be an additional US$ 6.45 million. Overall, depending on the scenario, the costs of switching to the hexavalent scheme would range from an additional US$ 2.62 million to US$ 6.45 million compared with the current vaccination scheme. -

(ACIP) General Best Guidance for Immunization
9. Special Situations Updates Major revisions to this section of the best practices guidance include the timing of intramuscular administration and the timing of clotting factor deficiency replacement. Concurrent Administration of Antimicrobial Agents and Vaccines With a few exceptions, use of an antimicrobial agent does not interfere with the effectiveness of vaccination. Antibacterial agents have no effect on inactivated, recombinant subunit, or polysaccharide vaccines or toxoids. They also have no effect on response to live, attenuated vaccines, except BCG vaccines. Antimicrobial or immunosuppressive agents may interfere with the immune response to BCG and should only be used under medical supervision (for additional information, see www.merck.com/product/usa/pi_circulars/b/bcg/bcg_pi.pdf). Antiviral drugs used for treatment or prophylaxis of influenza virus infections have no effect on the response to inactivated influenza vaccine (2). However, live, attenuated influenza vaccine should not be administered until 48 hours after cessation of therapy with antiviral influenza drugs. If feasible, to avoid possible reduction in vaccine effectiveness, antiviral medication should not be administered for 14 days after LAIV administration (2). If influenza antiviral medications are administered within 2 weeks after receipt of LAIV, the LAIV dose should be repeated 48 or more hours after the last dose of zanamavir or oseltamivir. The LAIV dose should be repeated 5 days after peramivir and 17 days after baloxavir. Alternatively, persons receiving antiviral drugs within the period 2 days before to 14 days after vaccination with LAIV may be revaccinated with another approved vaccine formulation (e.g., IIV or recombinant influenza vaccine). Antiviral drugs active against herpesviruses (e.g., acyclovir or valacyclovir) might reduce the efficacy of vaccines containing live, attenuated varicella zoster virus (i.e., Varivax and ProQuad) (3,4). -

Frequently Asked Questions About Measles Immunizations
Immunization Unit Assessment, Compliance, and Evaluation Group Measles FAQs Q: When did the vaccine for measles become available? A: The first measles vaccines were available in 1963, and were replaced with a much better vaccine in 1968. Q: Do people who received MMR in the 1960s need to have their dose repeated? A: Not necessarily. People who have documentation of receiving a live measles vaccine in the 1960s do not need to be revaccinated. People who were vaccinated with a killed or inactivated measles vaccine, or vaccine of unknown type, should be revaccinated with at least 1 dose of MMR. Q: What kind of vaccine is it? A: The vaccines available in the United States that protect against measles are the MMR and MMRV, which protects against measles, mumps, and rubella or measles, mumps, rubella, and varicella (chickenpox). They are both live attenuated, or weakened, vaccines. Q: Which vaccine can I get, the MMR or the MMRV? A: The MMRV is only approved for people aged 12 months – 12 years. The MMR is approved for anyone 6 months of age and older, but it is routinely recommended for use in people 12 months of age and older. Any dose of MMR received before 12 months of age is not considered valid and should be repeated in 4 weeks or at age 12 months, whichever is later. Q: How is the vaccine given? A: The vaccine is administered in the fatty layer of tissue underneath the skin. Q: Is the measles shot just a one-time dose? A: The measles vaccine is very effective. -

The Hepatitis B Vaccine Is the Most Widely Used Vaccine in the World, with Over 1 Billion Doses Given
Hepatitis B Vaccine Protect Yourself and Those You Love What is Hepatitis B? Hepatitis B is the most common serious liver infection in the world. It is caused by the hepatitis B virus (HBV), which attacks liver cells and can lead to liver failure, cirrhosis (scarring), or liver cancer later in life. The virus is transmitted through direct contact with infected blood and bodily fluids, and from an infected woman to her newborn at birth. Is there a safe vaccine for hepatitis B? YES! The good news is that there is a safe and effective vaccine for hepatitis B. The vaccine is a series, typically given as three shots over a six-month period that will provide a lifetime of protection. You cannot get hepatitis B from the vaccine – there is no human blood or live virus in the vaccine. The hepatitis B vaccine is the most widely used vaccine in the world, with over 1 billion doses given. The hepatitis B vaccine is the first "anti-cancer" vaccine because it can help prevent liver cancer! Who should be vaccinated against hepatitis B? The World Health Organization (WHO) and the U.S. Centers for Disease Control and Prevention (CDC) recommend the hepatitis B vaccine for all newborns and children up to 18 years of age, and all high-risk adults. All infants should receive the first dose of the vaccine in the delivery room or in the first 24 hours of life, preferably within 12 hours. (CDC recommends the first dose within 12 hours vs. the WHO recommendation of 24 hours.) The HBV vaccine is recommended to anyone who is at high risk of infection. -

(ACIP) General Best Guidance for Immunization
8. Altered Immunocompetence Updates This section incorporates general content from the Infectious Diseases Society of America policy statement, 2013 IDSA Clinical Practice Guideline for Vaccination of the Immunocompromised Host (1), to which CDC provided input in November 2011. The evidence supporting this guidance is based on expert opinion and arrived at by consensus. General Principles Altered immunocompetence, a term often used synonymously with immunosuppression, immunodeficiency, and immunocompromise, can be classified as primary or secondary. Primary immunodeficiencies generally are inherited and include conditions defined by an inherent absence or quantitative deficiency of cellular, humoral, or both components that provide immunity. Examples include congenital immunodeficiency diseases such as X- linked agammaglobulinemia, SCID, and chronic granulomatous disease. Secondary immunodeficiency is acquired and is defined by loss or qualitative deficiency in cellular or humoral immune components that occurs as a result of a disease process or its therapy. Examples of secondary immunodeficiency include HIV infection, hematopoietic malignancies, treatment with radiation, and treatment with immunosuppressive drugs. The degree to which immunosuppressive drugs cause clinically significant immunodeficiency generally is dose related and varies by drug. Primary and secondary immunodeficiencies might include a combination of deficits in both cellular and humoral immunity. Certain conditions like asplenia and chronic renal disease also can cause altered immunocompetence. Determination of altered immunocompetence is important to the vaccine provider because incidence or severity of some vaccine-preventable diseases is higher in persons with altered immunocompetence; therefore, certain vaccines (e.g., inactivated influenza vaccine, pneumococcal vaccines) are recommended specifically for persons with these diseases (2,3). Administration of live vaccines might need to be deferred until immune function has improved. -

Measles: Chapter 7.1 Chapter 7: Measles Paul A
VPD Surveillance Manual 7 Measles: Chapter 7.1 Chapter 7: Measles Paul A. Gastanaduy, MD, MPH; Susan B. Redd; Nakia S. Clemmons, MPH; Adria D. Lee, MSPH; Carole J. Hickman, PhD; Paul A. Rota, PhD; Manisha Patel, MD, MS I. Disease Description Measles is an acute viral illness caused by a virus in the family paramyxovirus, genus Morbillivirus. Measles is characterized by a prodrome of fever (as high as 105°F) and malaise, cough, coryza, and conjunctivitis, followed by a maculopapular rash.1 The rash spreads from head to trunk to lower extremities. Measles is usually a mild or moderately severe illness. However, measles can result in complications such as pneumonia, encephalitis, and death. Approximately one case of encephalitis2 and two to three deaths may occur for every 1,000 reported measles cases.3 One rare long-term sequelae of measles virus infection is subacute sclerosing panencephalitis (SSPE), a fatal disease of the central nervous system that generally develops 7–10 years after infection. Among persons who contracted measles during the resurgence in the United States (U.S.) in 1989–1991, the risk of SSPE was estimated to be 7–11 cases/100,000 cases of measles.4 The risk of developing SSPE may be higher when measles occurs prior to the second year of life.4 The average incubation period for measles is 11–12 days,5 and the average interval between exposure and rash onset is 14 days, with a range of 7–21 days.1, 6 Persons with measles are usually considered infectious from four days before until four days after onset of rash with the rash onset being considered as day zero. -

(DTP-Hep B-Hib) Vaccine Into the EPI Programme
EPIDEMIOLOGICAL UNIT Department of Health Services Ministry of Health Care and Nutrition 231, de Saram Place, Colombo 01000, Sri Lanka Telephone: (+94-11-) 2681548, 2695112, Fax: (+94-11-) 2696583, E-mail: [email protected], [email protected] My No: EPI/81/VII/2007 22nd October 2007 Provincial /Regional Directors of Health Services, Directors of Teaching Hospitals/Specialized Campaigns, M. SS /D.M.OO of Provincial /Base Hospitals, Heads of Decentralized Units and, Medical Officers of Health Introduction of combined pentavalent (DTP-Hep B- Hib) Vaccine into the EPI A decision has been taken to introduce Hib (Haemophilus Influenzae B) vaccine into the EPI programme in Sri Lanka from year 2008. This decision is based on the recommendation by the National Advisory Committee on Communicable Diseases. The Hib vaccine will be in the form of a combined pentavalent (DTP-HepB-Hib) vaccine, which would include DTP and Hep B and therefore would replace both DTP and Hepatitis B in the present schedule. Background The bacterium, Haemophilus influenzae type B (Hib), is an important cause of infections in infants and young children; severe disease in adults due to Hib is uncommon. Where it has been studied carefully, Hib is the leading cause of acute bacterial meningitis in infants and children less than five years old, accounting for one-third to one-half of all cases of bacterial meningitis in this age group. Bacterial meningitis is fatal unless treated immediately with antibiotics. Even with proper treatment 3-25% of affected children may die. Permanent disability with sequelae that include deafness, learning disabilities, and difficulties in movement is not uncommon among those who survive the infection. -

Vaccine Information for PARENTS and CAREGIVERS
NATIONAL INSTITUTE FOR COMMUNICABLE DISEASES Division of the National Health Laboratory Service VACCINE INFOR MATION FOR PARENTS & CAREGIVERS First Edition November 2016 Editors-in-Chief Nkengafac Villyen Motaze (MD, MSc, PhD fellow), Melinda Suchard (MBBCh, FCPath (SA), MMed) Edited by: Cheryl Cohen, (MBBCh, FCPath (SA) Micro, DTM&H, MSc (Epi), Phd) Lee Baker, (Dip Pharm) Lucille Blumberg, (MBBCh, MMed (Micro) ID (SA) FFTM (RCPS, Glasgow) DTM&H DOH DCH) Published by: Ideas Wise and Wonderful (IWW) for National Institute for Communicable Diseases (NICD) First Edition: Copyright © 2016 Contributions by: Clement Adu-Gyamfi (BSc Hons, MSc), Jayendrie Thaver (BSc), Kerrigan McCarthy, (MBBCh, FCPath (SA), DTM&H, MPhil (Theol) Kirsten Redman (BSc Hons), Nishi Prabdial-Sing (PhD), Nonhlanhla Mbenenge (MBBCh, MMED) Philippa Hime (midwife), Vania Duxbury (BSc Hons), Wayne Howard (BSc Hons) Acknowledgments: Amayeza, Vaccine Information Centre (http://www.amayeza-info.co.za/) Centre for Communicable Diseases Fact Sheets (http://www.cdc.gov/vaccines/hcp/vis/) World Health Organization Fact Sheets (http://www.who.int/mediacentre/factsheets/en/) National Department of Health, South Africa (http://www.health.gov.za/) Disclaimer This book is intended as an educational tool only. Information may be subject to change as schedules or formulations are updated. Summarized and simplified information is presented in this booklet. For full prescribing information and contraindications for vaccinations, please consult individual package inserts. There has been -

Pentavalent and Hexavalent Vaccines
Pentavalent and Hexavalent Vaccines Cold Chain Equipment Database ID 3_7 Year 2004 The freeze indicator is used to warn of freezing and is packed with vaccines that are sensitive to freezing temperatures: DTP, TT, DT, Td (freezing point of -6.5°C), hepatitis B (-0.5°C), liquid Hib and their combinations (DTP-HepB, and DTP-HepB+Hib vaccines) and JE. Every refrigerator storing vaccines should have a freeze indicator (Freeze Watch™). It is strongly recommended that one freeze indicator be placed in each cold box during vaccine transport and distribution. This is critical in places subject to low temperatures. Immunization in practice: a practical resource guide for Health workers – 2004 update_____Module 3: The cold chain WHO/IVB/04.06 Page 13 Vaccine Handling Database ID 81_1 Year 2006 The recommended conditions for storing vaccines used in immunization programmes are shown in Appendix 81_1. This diagram also indicates the maximum times and temperatures in each case. At the higher levels of the cold chain, i.e., at national (primary), and regional or province level, OPV must be kept frozen between - 15oC and -25oC. Freeze-dried vaccines (i.e., BCG, measles, MMR and yellow fever) may also be kept frozen at -15oC to -25oC if cold chain space permits, but this is neither essential nor recommended. At other levels of the cold chain (intermediate vaccine stores and health facilities), these vaccines should be stored between +2oC and +8oC. All other vaccines should be stored at between +2oC and +8oC at all levels of the cold chain. Liquid formulations of vaccines containing diphtheria, pertussis, tetanus, hepatitis B, Haemophilus influenzae type b, IPV and their combinations should not be frozen. -
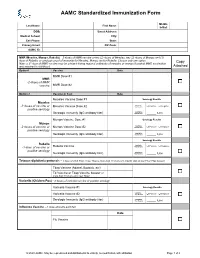
AAMC Standardized Immunization Form
AAMC Standardized Immunization Form Middle Last Name: First Name: Initial: DOB: Street Address: Medical School: City: Cell Phone: State: Primary Email: ZIP Code: AAMC ID: MMR (Measles, Mumps, Rubella) – 2 doses of MMR vaccine or two (2) doses of Measles, two (2) doses of Mumps and (1) dose of Rubella; or serologic proof of immunity for Measles, Mumps and/or Rubella. Choose only one option. Copy Note: a 3rd dose of MMR vaccine may be advised during regional outbreaks of measles or mumps if original MMR vaccination was received in childhood. Attached Option1 Vaccine Date MMR Dose #1 MMR -2 doses of MMR vaccine MMR Dose #2 Option 2 Vaccine or Test Date Measles Vaccine Dose #1 Serology Results Measles Qualitative -2 doses of vaccine or Measles Vaccine Dose #2 Titer Results: Positive Negative positive serology Quantitative Serologic Immunity (IgG antibody titer) Titer Results: _____ IU/ml Mumps Vaccine Dose #1 Serology Results Mumps Qualitative -2 doses of vaccine or Mumps Vaccine Dose #2 Titer Results: Positive Negative positive serology Quantitative Serologic Immunity (IgG antibody titer) Titer Results: _____ IU/ml Serology Results Rubella Qualitative Positive Negative -1 dose of vaccine or Rubella Vaccine Titer Results: positive serology Quantitative Serologic Immunity (IgG antibody titer) Titer Results: _____ IU/ml Tetanus-diphtheria-pertussis – 1 dose of adult Tdap; if last Tdap is more than 10 years old, provide date of last Td or Tdap booster Tdap Vaccine (Adacel, Boostrix, etc) Td Vaccine or Tdap Vaccine booster (if more than 10 years since last Tdap) Varicella (Chicken Pox) - 2 doses of varicella vaccine or positive serology Varicella Vaccine #1 Serology Results Qualitative Varicella Vaccine #2 Titer Results: Positive Negative Serologic Immunity (IgG antibody titer) Quantitative Titer Results: _____ IU/ml Influenza Vaccine --1 dose annually each fall Date Flu Vaccine © 2020 AAMC. -

Kids and COVID 19 Vaccination
Kids and COVID 19 Vaccination Q: What COVID vaccine is available for kids right now? A: Pfizer-BioNTech mRNA vaccine was initially approved for individuals to as young as age 16 years old and was recently approved for kids as young as 12 years of age. This is a two shot series, given 3 weeks apart. The dose is the same as that given to adults. Q: When will younger kids be able to get vaccinated? A: Pfizer is currently conducting studies on kids as young as 6 months of age. Moderna is in the process of submitting data on their studies for ages 12-18 yrs and have started the process for studies in younger kids. Many reputable sources suggest that kids as young as 6yrs of age may be eligible for vaccination this fall. Keep checking our website for more information on timeline and details for vaccination in younger kids and infants. Q: How do I get my child vaccinated? A: In North Idaho, there are many locations that offer the Pfizer vaccine. Many local pharmacies have the Pfizer vaccine available (check online or in person to ensure they have Pfizer brand available for those under age 18 yrs). The local Walgreen’s pharmacies are offering Pfizer vaccine and appointments can be scheduled at www.walgreens.com. Other option: www.panhandlehealth.org. This site will allow you to make appointments at the Kootenai county fairgrounds site as well as other sites in adjacent counties. We are not yet offering COVID vaccination at Coeur d’Alene Pediatrics, but hope to be able to do so in the future.