Study and Analysis on Verrucous Skin Lesions Over the Lowerlimbs
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

3628-3641-Pruritus in Selected Dermatoses
Eur opean Rev iew for Med ical and Pharmacol ogical Sci ences 2016; 20: 3628-3641 Pruritus in selected dermatoses K. OLEK-HRAB 1, M. HRAB 2, J. SZYFTER-HARRIS 1, Z. ADAMSKI 1 1Department of Dermatology, University of Medical Sciences, Poznan, Poland 2Department of Urology, University of Medical Sciences, Poznan, Poland Abstract. – Pruritus is a natural defence mech - logical self-defence mechanism similar to other anism of the body and creates the scratch reflex skin sensations, such as touch, pain, vibration, as a defensive reaction to potentially dangerous cold or heat, enabling the protection of the skin environmental factors. Together with pain, pruritus from external factors. Pruritus is a frequent is a type of superficial sensory experience. Pruri - symptom associated with dermatoses and various tus is a symptom often experienced both in 1 healthy subjects and in those who have symptoms systemic diseases . Acute pruritus often develops of a disease. In dermatology, pruritus is a frequent simultaneously with urticarial symptoms or as an symptom associated with a number of dermatoses acute undesirable reaction to drugs. The treat - and is sometimes an auxiliary factor in the diag - ment of this form of pruritus is much easier. nostic process. Apart from histamine, the most The chronic pruritus that often develops in pa - popular pruritus mediators include tryptase, en - tients with cholestasis, kidney diseases or skin dothelins, substance P, bradykinin, prostaglandins diseases (e.g. atopic dermatitis) is often more dif - and acetylcholine. The group of atopic diseases is 2,3 characterized by the presence of very persistent ficult to treat . Persistent rubbing, scratching or pruritus. -
Red, Weeping and Oozing P.51 6
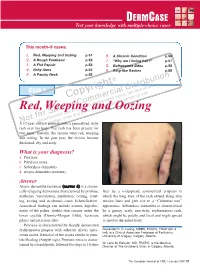
DERM CASE Test your knowledge with multiple-choice cases This month–9 cases: 1. Red, Weeping and Oozing p.51 6. A Chronic Condition p.56 2. A Rough Forehead p.52 7. “Why am I losing hair?” p.57 3. A Flat Papule p.53 8. Bothersome Bites p.58 4. Itchy Arms p.54 9. Ring-like Rashes p.59 5. A Patchy Neck p.55 on © buti t ri , h ist oad rig D wnl Case 1 y al n do p ci ca use o er sers nal C m d u rso m rise r pe o utho y fo C d. A cop or bite ngle Red, Weleepirnohig a sind Oozing a se p rint r S ed u nd p o oris w a t f uth , vie o Una lay AN12-year-old boy dpriesspents with a generalized, itchy rash over his body. The rash has been present for two years. Initially, the lesions were red, weeping and oozing. In the past year, the lesions became thickened, dry and scaly. What is your diagnosis? a. Psoriasis b. Pityriasis rosea c. Seborrheic dermatitis d. Atopic dermatitis (eczema) Answer Atopic dermatitis (eczema) (answer d) is a chroni - cally relapsing dermatosis characterized by pruritus, later by a widespread, symmetrical eruption in erythema, vesiculation, papulation, oozing, crust - which the long axes of the rash extend along skin ing, scaling and, in chronic cases, lichenification. tension lines and give rise to a “Christmas tree” Associated findings can include xerosis, hyperlin - appearance. Seborrheic dermatitis is characterized earity of the palms, double skin creases under the by a greasy, scaly, non-itchy, erythematous rash, lower eyelids (Dennie-Morgan folds), keratosis which might be patchy and focal and might spread pilaris and pityriasis alba. -

Frontiers in Dermatology and Venereology - a Series of Theme Issues in Relation to the 100-Year Anniversary of Actadv
ISSN 0001-5555 ActaDV Volume 100 2020 Theme issue ADVANCES IN DERMATOLOGY AND VENEREOLOGY A Non-profit International Journal for Interdisciplinary Skin Research, Clinical and Experimental Dermatology and Sexually Transmitted Diseases Frontiers in Dermatology and Venereology - A series of theme issues in relation to the 100-year anniversary of ActaDV Official Journal of - European Society for Dermatology and Psychiatry Affiliated with - The International Forum for the Study of Itch Immediate Open Access Acta Dermato-Venereologica www.medicaljournals.se/adv ACTA DERMATO-VENEREOLOGICA The journal was founded in 1920 by Professor Johan Almkvist. Since 1969 ownership has been vested in the Society for Publication of Acta Dermato-Venereologica, a non-profit organization. Since 2006 the journal is published online, independently without a commercial publisher. (For further information please see the journal’s website https://www. medicaljournals.se/acta) ActaDV is a journal for clinical and experimental research in the field of dermatology and venereology and publishes high- quality papers in English dealing with new observations on basic dermatological and venereological research, as well as clinical investigations. Each volume also features a number of review articles in special areas, as well as Correspondence to the Editor to stimulate debate. New books are also reviewed. The journal has rapid publication times. Editor-in-Chief: Olle Larkö, MD, PhD, Gothenburg Former Editors: Johan Almkvist 1920–1935 Deputy Editors: Sven Hellerström 1935–1969 -

Dermatological Disorders in Tuvalu Between 2009 and 2012
MOLECULAR MEDICINE REPORTS 12: 3629-3631, 2015 Dermatological disorders in Tuvalu between 2009 and 2012 LI-JUNG LAN1,2, YING-SHUANG LIEN2,3, SHAO-CHUAN WANG2,4, NESE ITUASO-CONWAY5, MING-CHE TSAI2,6, PAO-YING TSENG6, YU-LIN YEH1, CHUN-TZU CHEN7, KO‑HUANG LUE2,8, JING-GUNG CHUNG9,10 and YU-PING HSIAO1,2 1Department of Dermatology, Chung Shan Medical University Hospital, Taichung 40201; 2Institute of Medicine, School of Medicine, Chung Shan Medical University, Taichung 40201; Departments of 3Obstetrics and Gynecology, and 4Urology, Chung Shan Medical University Hospital, Taichung 40201; 5Public Health, Princess Margaret Hospital, Ministry of Health, Funafuti, Tuvalu; 6International Medical Service Center, Chung Shan Medical University Hospital, Taichung 40201; Departments of 7Chief Secretary Group and 8Pediatrics, Chung Shan Medical University Hospital, Taichung 40201; 9Department of Biological Science and Technology, China Medical University, Taichung 40201; 10Department of Biotechnology, Asia University, Taichung 41354, Taiwan, R.O.C. Received July 1, 2014; Accepted September 18, 2014 DOI: 10.3892/mmr.2015.3806 Abstract. There is a distinct lack of knowledge on the land area of Tuvalu is only 25.9 km2, and the highest point does prevalence of skin disorders in Tuvalu. The aim of the current not exceed 4 m above sea level (1). Currently, an estimated study was to assess the prevalence of cutaneous diseases and 11,000 people live in Tuvalu (1). The Taiwan International to evaluate access dermatological care in Tuvalu. Cutaneous Cooperation and Development Fund (Taiwan ICDF) has disorders in the people of Tuvalu between 2009 and 2012 coordinated the medical resources of Taiwanese hospitals in were examined. -

(12) United States Patent (10) Patent No.: US 7,359,748 B1 Drugge (45) Date of Patent: Apr
USOO7359748B1 (12) United States Patent (10) Patent No.: US 7,359,748 B1 Drugge (45) Date of Patent: Apr. 15, 2008 (54) APPARATUS FOR TOTAL IMMERSION 6,339,216 B1* 1/2002 Wake ..................... 250,214. A PHOTOGRAPHY 6,397,091 B2 * 5/2002 Diab et al. .................. 600,323 6,556,858 B1 * 4/2003 Zeman ............. ... 600,473 (76) Inventor: Rhett Drugge, 50 Glenbrook Rd., Suite 6,597,941 B2. T/2003 Fontenot et al. ............ 600/473 1C, Stamford, NH (US) 06902-2914 7,092,014 B1 8/2006 Li et al. .................. 348.218.1 (*) Notice: Subject to any disclaimer, the term of this k cited. by examiner patent is extended or adjusted under 35 Primary Examiner Daniel Robinson U.S.C. 154(b) by 802 days. (74) Attorney, Agent, or Firm—McCarter & English, LLP (21) Appl. No.: 09/625,712 (57) ABSTRACT (22) Filed: Jul. 26, 2000 Total Immersion Photography (TIP) is disclosed, preferably for the use of screening for various medical and cosmetic (51) Int. Cl. conditions. TIP, in a preferred embodiment, comprises an A6 IB 6/00 (2006.01) enclosed structure that may be sized in accordance with an (52) U.S. Cl. ....................................... 600/476; 600/477 entire person, or individual body parts. Disposed therein are (58) Field of Classification Search ................ 600/476, a plurality of imaging means which may gather a variety of 600/162,407, 477, 478,479, 480; A61 B 6/00 information, e.g., chemical, light, temperature, etc. In a See application file for complete search history. preferred embodiment, a computer and plurality of USB (56) References Cited hubs are used to remotely operate and control digital cam eras. -

Menlo Therapeutics Inc. June 2019
Menlo Therapeutics Inc. June 2019 Developing Serlopitant, a Once-Daily Oral NK1 Receptor Antagonist for Pruritus Safe Harbor Statements Special Note Regarding Forward-Looking Statements This presentation contains forward-looking statements, including statements about our plans to develop and commercialize our product candidates, our planned clinical trials for serlopitant, the timing of the availability of data from our clinical trials, the timing of our planned regulatory filings, the timing of and our ability to obtain and maintain regulatory approvals for serlopitant and the clinical utility of serlopitant, alone and as compared to other treatment options, the duration of patent protection, and other statements regarding strategy, future operations and plans, as well as assumptions underlying such statements. These statements involve substantial known and unknown risks, uncertainties and other factors, some of which are outside of our control, that may cause our actual results, levels of activity, performance or achievements to be materially different from the information expressed or implied by these forward- looking statements, including risks related to the clinical drug development process, the regulatory approval process, our reliance on third parties, and our ability to defend our intellectual property. We may not actually achieve the plans, intentions or expectations disclosed in our forward-looking statements, and you should not place undue reliance on our forward-looking statements. Actual results or events could differ materially from the plans, intentions and expectations disclosed in the forward-looking statements we make. Additional information that could lead to material changes in our performance is contained in our filings with the U.S. Securities and Exchange Commission. -

Buffalo Medical Group, P.C. Robert E
Buffalo Medical Group, P.C. Robert E. Kalb, M.D. Phone: (716) 630-1102 Fax: (716) 633-6507 Department of Dermatology 325 Essjay Road Williamsville, New York 14221 2 FOOT- 1 HAND SYNDROME 2 foot - 1 hand syndrome is a superficial infection of the skin caused by the common athlete's foot fungus. It is quite common for people to have a minor amount of an athlete's foot condition. This would appear as slight scaling and/or itching between the toes. In addition, patients may have thickened toenails as part of the athlete's foot condition. Again the problem on the feet is very common and often patients are not even aware of it. In some patients, however, the athlete's foot fungus can spread to another area of the body. For some strange and unknown reason, it seems to affect only one hand. That is why the condition is called 2 foot - 1 hand syndrome. It is not clear why the problem develops in only one hand or why the right or left is involved in some patients. Fortunately there is very effective treatment to control this minor skin problem. If the problem with the superficial fungus infection is confined to the skin, then a short course of treatment with an oral antibiotic is all that is required. This antibiotic is very safe and normally clears the skin up fairly rapidly. It is often used with a topical cream to speed the healing process. If, however, the fingernails of the affected hand are also involved then a more prolonged course of the antibiotic will be necessary. -

Prurigo Nodularis and Lichen Simplex Chronicus
Dermatologic Therapy, Vol. 21, 2008, 42–46 Copyright © Blackwell Publishing, Inc., 2008 Printed in the United States · All rights reserved DERMATOLOGIC THERAPY ISSN 1396-0296 Blackwell Publishing Inc Prurigo nodularis and lichen simplex chronicus TORELLO LOTTI, GIONATA BUGGIANI & FRANCESCA PRIGNANO Department of Dermatological Sciences, University of Florence, Florence, Italy ABSTRACT: Emotional tensions in predisposed subjects may play a key role in inducing a pruritic sensation, leading to a scratching that, becoming a self-perpetuating pathomechanism, may represent the main feature of two distinct cutaneous clinical entities: prurigo nodularis and lichen simplex chronicus. Psychogenic factors play a relevant role in both conditions, and they are often associated with depression and dissociative experiences. Hence, the importance of the evaluation of these patients from the point of view of psychodermatology, which may analyze the relationship between skin disease and psychological factors. Patients with real or perceived imperfections in particular areas of the body (face, scalp, hands, and genital area) are more prone to psychologic distress, whereas cutaneous diseases may lead to experience a heightened level of distress. As psychosomatic factors have been estimated to be present in at least one-third of dermatologic patients, effective management of skin conditions involves consideration of the associated emotional factors. KEYWORDS: lichen simplex chronicus, management, prurigo nodularis, psychodermatology Introduction scars when spontaneously regress (FIG. 2). Itch is intense, and severe crises can be triggered by According to a psychosomatic perspective usually emotional stress. agreed upon in the scientific community, emo- Lichen simplex chronicus (LSC) is a skin disorder tional tensions in predisposed subjects may play characterized by lichenification of the skin as a a key role in inducing itch, thus provoking result of primary excessive scratching (FIG. -

Nodular Prurigo: an Overview of Diagnosis and Management
CLINICAL REVIEW Nodular prurigo: An overview of diagnosis and management Sheila Ryan ABSTRACT Nodular prurigo is a chronic inflammatory skin disease characterised by severe pruritus, nodules, papules, excoriations and ulceration. It is a can be a very distressing disorder for the sufferer. The condition is linked with a variety of disorders including atopic eczema, chronic renal failure, hyperthyroidism, iron deficiency anaemia, obstructive biliary disease, gastric malignancy, lymphoma, leukaemia, hepatitis B and C, HIV and depression. Nodular prurigo affects all ages and commonly occurs between the ages of 20 to 60 years. There are a range of treatments available for nodular prurigo, but their use is based on anecdotal rather than empirical evidence. The range of treatments will be discussed here. The nurse has an important role in guiding and supporting patients with this difficult, often frustrating condition. Citation: Ryan S. Nodular prurigo: An overview of diagnosis and management. Dermatological Nursing 2017. 16(4): 18-21 Introduction of disorders including atopic eczema, Nodular prurigo is a chronic chronic renal failure, hyperthyroidism, iron infl ammatory skin disease characterised defi ciency anaemia, obstructive biliary by severe pruritus, nodules, papules, disease, gastric malignancy, lymphoma, excoriations and ulceration.1 Dr James leukaemia, hepatitis B and C and HIV.1,4 Hyde fi rst described the condition in If nodular prurigo is solely as a result of 1909, which reported pruritic nodules scratching it is remarkable that it does on the lower extremities in middle-aged not evolve in more patients with chronic women.2 The condition is also known pruritic conditions.3 as prurigo nodularis, Hyde’s disease, prurigo simplex chronicus, lichen obtusus Nodular prurigo is also linked corneus and nodular neurodermatitis with psychiatric disorders including circumscripta.1 depression and anxiety.3 The relationship here is also unclear. -

Scabies Presenting As Cutaneous Nodules Or Malar
Volume 24 Number 9| September 2018| Dermatology Online Journal || Case Report 24(9): 8 Scabies presenting as cutaneous nodules or malar erythema: reports of patients with scabies surrepticius masquerading as prurigo nodularis or systemic lupus erythematosus Tyler Werbel1 MS, Brian R Hinds2 MD, Philip R Cohen2 MD Affiliations: 1School of Medicine, University of California San Diego, La Jolla, California, USA, 2Department of Dermatology, University of California San Diego, La Jolla, California, USA Corresponding Authors: Tyler Werbel, MS, 7438 High Avenue, La Jolla, CA 92037, Tel: 352-226-0683, Email: [email protected]; Philip R. Cohen, MD, 10991 Twinleaf Court, San Diego, CA 92131, Email: [email protected] Introduction Abstract Sarcoptes scabiei var. hominis is a mite that causes Scabies surrepticius is a unifying term that represents infestations in humans with over 300 million cases non-classical presentations of scabies mite infestation. A patient with scabies surrepticius is per year [1]. The classical presentation is described: a man with scabies masquerading as characterized by generalized pruritus and lesions prurigo nodularis. The 91-year-old man had such as burrows usually found in the finger space metastatic prostate cancer and presented with webs [2]. However, infestations with scabies can diffuse pruritic nodules. Prurigo nodularis was present with unusual morphologies lacking typical suspected; however, the biopsy revealed scabies lesions or clinical clues to the underlying parasite. In mites in the stratum corneum. He was successfully this setting, the infestation has been referred to as treated with topical permethrin 5% cream and oral scabies surrepticius (Box 1), [3, 4]. A man whose ivermectin. In addition, the features of a woman with scabies mimicking systemic lupus erythematosus are scabies mimicked prurigo nodularis is described, and summarized. -

Prurigo Nodularis: George Cohen, MD Department of Dermatology & Cutaneous Picking the Right Treatment Surgery, University of South Florida, Tampa (Dr
Michael Saco, MD; Prurigo nodularis: George Cohen, MD Department of Dermatology & Cutaneous Picking the right treatment Surgery, University of South Florida, Tampa (Dr. Saco); Department of Dermatology, University Most patients with localized nodules should receive of Florida, Gainesville topical treatment first. But disappointing results or (Dr. Cohen) specific findings described here could necessitate [email protected] The authors reported no additional or alternative options. potential conflict of interest relevant to this article. CASE u A 43-year-old woman arrives at your office with persis- Practice tent itching on her arms and legs. for some time, she has used recommendatIonS moisturizing lotions and herbal preparations suggested by her › Start with topical cortico- mother, but they have provided no relief. you note multiple 0.5- steroids under occlusion and to 2-cm firm, excoriated nodules symmetrically distributed on her periodically substitute with elbows and knees bilaterally. She has seasonal allergies and a his- steroid-sparing agents tory of childhood asthma. how would you care for this patient? (calcipotriol ointment or pimecrolimus 1% cream) reating prurigo nodularis (PN) can be a daunting task for localized for even the most experienced clinician. Prurigo nod- prurigo nodularis. B ules are cutaneous lesions often produced by repetitive › Consider adding oral T scratching—hence the nickname “picker’s nodules”—which antihistamines or may occur as sequelae of chronic pruritus or neurotic exco- montelukast to the initial riations. Thus, PN can be classified as a subtype of neuroder- regimen if a pruritic cause is suspected; alternatively, matitis. The nodules can be intensely pruritic, resulting in an 1,2 consider adding these agents itch-scratch cycle that can be difficult to break. -

Hypertrophic Lichen Planus Mimicking Verrucous Lupus Erythematosus
Open Access Case Report DOI: 10.7759/cureus.3555 Hypertrophic Lichen Planus Mimicking Verrucous Lupus Erythematosus Ryan R. Riahi 1 , Philip R. Cohen 2 1. Dermatology, DermSurgery Associates, Sugar Land, USA 2. Dermatologist, San Diego Family Dermatology, San Diego, USA Corresponding author: Ryan R. Riahi, [email protected] Abstract Lichen planus is an inflammatory skin condition that can affect the hair, mucous membranes, nails, and skin. Cutaneous lichen planus typically presents as papules that are planar, polygonal, pruritic, and purple. Subtypes of lichen planus include actinic, annular, atrophic, eruptive, follicular, hypertrophic, inverse, linear, palmoplantar, pemphigoides, pigmentosus, ulcerative, vesiculobullous, and vulvovaginal. The various clinical presentations of lichen planus can mimic other dermatologic conditions. A 63-year-old woman, who presented with pruritic, hyperkeratotic plaques on the lower legs of two years duration, is described; her lesions were morphologically suggestive of verrucous lupus erythematosus. However, an examination also revealed purple papules on the wrists and white, reticulated patches on the bilateral buccal mucosa. Biopsies demonstrated lichenoid dermatitis while laboratory studies for systemic lupus erythematosus were negative. A correlation of the clinical presentation, pathology, and laboratory studies established a diagnosis of hypertrophic lichen planus. The clinical mimickers of hypertrophic lichen planus are reviewed and the therapeutic treatments for this condition discussed. Categories: Dermatology, Internal Medicine, Rheumatology Keywords: cutaneous, erythematosus, hypertrophic, lichen, lichenoid, lupus, mimic, mimicking, planus, verrucous Introduction Lichen planus is a chronic inflammatory and immune-mediated condition of unknown etiology that can affect the hair, mucosa, nails, and skin [1-2]. Classic lichen planus typically involves the flexor extremities and presents as purple, flat-topped papules that are pruritic.