Curriculum Outline General Surgery
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Educational Paper Ciliopathies
Eur J Pediatr (2012) 171:1285–1300 DOI 10.1007/s00431-011-1553-z REVIEW Educational paper Ciliopathies Carsten Bergmann Received: 11 June 2011 /Accepted: 3 August 2011 /Published online: 7 September 2011 # The Author(s) 2011. This article is published with open access at Springerlink.com Abstract Cilia are antenna-like organelles found on the (NPHP) . Ivemark syndrome . Meckel syndrome (MKS) . surface of most cells. They transduce molecular signals Joubert syndrome (JBTS) . Bardet–Biedl syndrome (BBS) . and facilitate interactions between cells and their Alstrom syndrome . Short-rib polydactyly syndromes . environment. Ciliary dysfunction has been shown to Jeune syndrome (ATD) . Ellis-van Crefeld syndrome (EVC) . underlie a broad range of overlapping, clinically and Sensenbrenner syndrome . Primary ciliary dyskinesia genetically heterogeneous phenotypes, collectively (Kartagener syndrome) . von Hippel-Lindau (VHL) . termed ciliopathies. Literally, all organs can be affected. Tuberous sclerosis (TSC) . Oligogenic inheritance . Modifier. Frequent cilia-related manifestations are (poly)cystic Mutational load kidney disease, retinal degeneration, situs inversus, cardiac defects, polydactyly, other skeletal abnormalities, and defects of the central and peripheral nervous Introduction system, occurring either isolated or as part of syn- dromes. Characterization of ciliopathies and the decisive Defective cellular organelles such as mitochondria, perox- role of primary cilia in signal transduction and cell isomes, and lysosomes are well-known -

1311 Diploma in Medical Record Science Second
[LD 0212] AUGUST 2013 Sub. Code: 1311 DIPLOMA IN MEDICAL RECORD SCIENCE SECOND YEAR PAPER II – INTERNATIONAL CLASSIFICATION OF DISEASES (ICD-10) & SURGICAL PROCEDURES (ICM-9CM) Q.P. Code : 841311 Time : Three Hours Maximum : 100 marks Answer ALL questions I Write appropriate codes using ICD -10 (30 x 1 = 30) 1. Therapeutic introduction of hand tendon. 2. Excision of major partial thickness of eyelid excision. 3. Interphalangeal arthrodesis of Toe. 4. Division of percutaneous spinal cord nerve tracts. 5. Transfusion of allograft bone aetriosus. 6. Rastelli operation of truncus arteriosus. 7. Pyoloric sphincter dilatation. 8. Stapling of radius epiphyseal plate. 9. Suture of hands fascia. 10. Suture of hand fascia. 11. Repair of anterior wall (abdomen) hernia. 12. Foreign body removal without incision in t o the brain. 13. Repair of Tetrology of fallot. 14. Frontal Sinusectomy. 15. Urethral sling suspension. 16. Bone shaft transfer. 17. Coil of aneuryum repair. 18. Sling suspension. 19. Radio isotope scanning, pituitary gland. 20. Spinal shunt removal. 21. Acute lung edema. Due to external agent. 22. Proximal end tibial closed fracture was riding a two wheeler-slip & fell down. 23. Thrombosed internal hemorrhoids. 24. Secondary hypertension due to renal disorder. 25. Old myocardial infarction. 26. Fall from high place, injured elbow. 27. Chronic venous (peripheral) insufficiency. 28. Acute myeloid leukemia. 29. Post-operative intestine obstruction. 30. Abnormal pregnancy. II Writes appropriate codes using ICS-9CM (20 x 2 = 40) 1. Pregnant women suffering from acute salphingo oophoritis. 2. Accidental intake of ferrous salt. 3. Sprain of lumbar spine as stuck by another person. 4. -

Research Day 2021 Program
Western Michigan University ScholarWorks at WMU Research Day WMU Homer Stryker M.D. School of Medicine 2021 Research Day 2021 Program Western Michigan University Homer Stryker M.D. School of Medicine Follow this and additional works at: https://scholarworks.wmich.edu/medicine_research_day Part of the Life Sciences Commons, and the Medicine and Health Sciences Commons WMU ScholarWorks Citation Homer Stryker M.D. School of Medicine, Western Michigan University, "Research Day 2021 Program" (2021). Research Day. 298. https://scholarworks.wmich.edu/medicine_research_day/298 This Abstract is brought to you for free and open access by the WMU Homer Stryker M.D. School of Medicine at ScholarWorks at WMU. It has been accepted for inclusion in Research Day by an authorized administrator of ScholarWorks at WMU. For more information, please contact [email protected]. th 38 Annual Kalamazoo Community Medical and Health Sciences Virtual Research Day Wednesday, April 21, 2021 8:00 a.m. – 12:00 p.m. TABLE OF CONTENTS INTRODUCTION ........................................................................................................... 4 KEYNOTE SPEAKER.................................................................................................... 6 SCHEDULE ..................................................................................................................... 7 ORAL PRESENTATIONS ............................................................................................. 8 ORAL ABSTRACTS .................................................................................................... -

ARPKD): Kidney-Related and Non-Kidney-Related Phenotypes
Pediatr Nephrol (2014) 29:1915–1925 DOI 10.1007/s00467-013-2634-1 EDUCATIONAL REVIEW Clinical manifestations of autosomal recessive polycystic kidney disease (ARPKD): kidney-related and non-kidney-related phenotypes Rainer Büscher & Anja K. Büscher & Stefanie Weber & Julia Mohr & Bianca Hegen & Udo Vester & Peter F. Hoyer Received: 26 April 2013 /Revised: 5 September 2013 /Accepted: 6 September 2013 /Published online: 10 October 2013 # IPNA 2013 Abstract Autosomal recessive polycystic kidney disease disease. In this review we focus on common and uncommon (ARPKD), although less frequent than the dominant form, is kidney-related and non-kidney-related phenotypes. Clinical a common, inherited ciliopathy of childhood that is caused by management of ARPKD patients should include consideration mutations in the PKHD1-gene on chromosome 6. The charac- of potential problems related to these manifestations. teristic dilatation of the renal collecting ducts starts in utero and can present at any stage from infancy to adulthood. Renal Keywords ARPKD . Extrarenal manifestation . Children . insufficiency may already begin in utero and may lead to early Hepatic fibrosis . Portal hypertension . Caroli’ssyndrome abortion or oligohydramnios and lung hypoplasia in the new- born. However, there are also affected children who have no evidence of renal dysfunction in utero and who are born with Introduction normal renal function. Up to 30 % of patients die in the perinatal period, and those surviving the neonatal period reach Autosomal recessive polycystic kidney disease (ARPKD) be- end stage renal disease (ESRD) in infancy, early childhood or longs to the family of cilia-related disorders and is an important adolescence. In contrast, some affected patients have been inherited disease with distinct clinical features and genetics. -

Clinical Practice Guideline for the Management of Anorectal Abscess, Fistula-In-Ano, and Rectovaginal Fistula Jon D
PRACTICE GUIDELINES Clinical Practice Guideline for the Management of Anorectal Abscess, Fistula-in-Ano, and Rectovaginal Fistula Jon D. Vogel, M.D. • Eric K. Johnson, M.D. • Arden M. Morris, M.D. • Ian M. Paquette, M.D. Theodore J. Saclarides, M.D. • Daniel L. Feingold, M.D. • Scott R. Steele, M.D. Prepared on behalf of The Clinical Practice Guidelines Committee of the American Society of Colon and Rectal Surgeons he American Society of Colon and Rectal Sur- and submucosal locations.7–11 Anorectal abscess occurs geons is dedicated to ensuring high-quality pa- more often in males than females, and may occur at any Ttient care by advancing the science, prevention, age, with peak incidence among 20 to 40 year olds.4,8–12 and management of disorders and diseases of the co- In general, the abscess is treated with prompt incision lon, rectum, and anus. The Clinical Practice Guide- and drainage.4,6,10,13 lines Committee is charged with leading international Fistula-in-ano is a tract that connects the perine- efforts in defining quality care for conditions related al skin to the anal canal. In patients with an anorec- to the colon, rectum, and anus by developing clinical tal abscess, 30% to 70% present with a concomitant practice guidelines based on the best available evidence. fistula-in-ano, and, in those who do not, one-third will These guidelines are inclusive, not prescriptive, and are be diagnosed with a fistula in the months to years after intended for the use of all practitioners, health care abscess drainage.2,5,8–10,13–16 Although a perianal abscess workers, and patients who desire information about the is defined by the anatomic space in which it forms, a management of the conditions addressed by the topics fistula-in-ano is classified in terms of its relationship to covered in these guidelines. -

Targeted Exome Sequencing Provided Comprehensive Genetic Diagnosis of Congenital Anomalies of the Kidney and Urinary Tract
Journal of Clinical Medicine Article Targeted Exome Sequencing Provided Comprehensive Genetic Diagnosis of Congenital Anomalies of the Kidney and Urinary Tract 1,2, 3,4, 3 1,5 Yo Han Ahn y, Chung Lee y, Nayoung K. D. Kim , Eujin Park , Hee Gyung Kang 1,2,6,* , Il-Soo Ha 1,2,6, Woong-Yang Park 3,4,7 and Hae Il Cheong 1,2,6 1 Department of Pediatrics, Seoul National University College of Medicine, Seoul 03080, Korea; [email protected] (Y.H.A.); [email protected] (E.P.); [email protected] (I.-S.H.); [email protected] (H.I.C.) 2 Department of Pediatrics, Seoul National University Children’s Hospital, Seoul 03080, Korea 3 Samsung Genome Institute, Samsung Medical Center, Seoul 06351, Korea; [email protected] (C.L.); [email protected] (N.K.D.K.); [email protected] (W.-Y.P.) 4 Department of Health Sciences and Technology, Samsung Advanced Institute for Health Sciences and Technology, Sungkyunkwan University, Seoul 06351, Korea 5 Department of Pediatrics, Kangnam Sacred Heart Hospital, Hallym University College of Medicine, Seoul 07441, Korea 6 Kidney Research Institute, Medical Research Center, Seoul National University College of Medicine, Seoul 03080, Korea 7 Department of Molecular Cell Biology, Sungkyunkwan University School of Medicine, Suwon 16419, Korea * Correspondence: [email protected] These authors equally contributed to this article. y Received: 31 January 2020; Accepted: 8 March 2020; Published: 10 March 2020 Abstract: Congenital anomalies of the kidney and urinary tract (CAKUT) are the most common cause of chronic kidney disease in children. -

Article Case Report Congenital Hepatic Fibrosis
Article Case report Congenital hepatic fibrosis: case report and review of literature Brahim El Hasbaoui, Zainab Rifai, Salahiddine Saghir, Anas Ayad, Najat Lamalmi, Rachid Abilkassem, Aomar Agadr Corresponding author: Zainab Rifai, Department of Pediatrics, Children’s Hospital, Faculty of Medicine and Pharmacy, University Mohammed V, Rabat, Morocco. [email protected] Received: 19 Jan 2021 - Accepted: 03 Feb 2021 - Published: 18 Feb 2021 Keywords: Fibrosis, hyper-transaminasemia, cholestasis, ciliopathy, case report Copyright: Brahim El Hasbaoui et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Cite this article: Brahim El Hasbaoui et al. Congenital hepatic fibrosis: case report and review of literature. Pan African Medical Journal. 2021;38(188). 10.11604/pamj.2021.38.188.27941 Available online at: https://www.panafrican-med-journal.com//content/article/38/188/full Congenital hepatic fibrosis: case report and review &Corresponding author of literature Zainab Rifai, Department of Pediatrics, Children’s Hospital, Faculty of Medicine and Pharmacy, Brahim El Hasbaoui1, Zainab Rifai2,&, Salahiddine University Mohammed V, Rabat, Morocco Saghir1, Anas Ayad1, Najat Lamalmi3, Rachid 1 1 Abilkassem , Aomar Agadr 1Department of Pediatrics, Military Teaching Hospital Mohammed V, Faculty of Medicine and Pharmacy, University Mohammed V, Rabat, Morocco, 2Department of Pediatrics, Children’s Hospital, Faculty of Medicine and Pharmacy, University Mohammed V, Rabat, Morocco, 3Department of Histopathologic, Avicenne Hospital, Faculty of Medicine and Pharmacy, University Mohammed V, Rabat, Morocco Article characterized histologically by defective Abstract remodeling of the ductal plate (DPM). -

Management of Choledochal Cysts
REVIEW CURRENT OPINION Management of choledochal cysts Sean M. Ronnekleiv-Kelly, Kevin C. Soares, Aslam Ejaz, and Timothy M. Pawlik Purpose of review Historically, surgical treatment of choledochal cyst consisted of cyst enterostomy. However, incomplete cyst excision can result in recurrent symptoms and malignant transformation within the cyst remnant. 09/20/2020 on BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3pxNPODIEKBpIl4WIJuUC3wZcoMyoyOwWjpQO3AzJmNqjsWy7MP1HEA== by https://journals.lww.com/co-gastroenterology from Downloaded Downloaded Accordingly, management of choledochal cyst now includes complete cyst excision whenever possible. We provide a review detailing the up to date management of choledochal cysts. We describe choledochal from cyst-type specific surgical approaches, the impact of minimally invasive surgery in choledochal cyst https://journals.lww.com/co-gastroenterology therapy, and long-term sequelae of choledochal cyst management. Recent findings Treatment of choledochal cyst aims to avoid the numerous hepatic, pancreatic, or biliary complications that may occur. More recently, minimally invasive approaches are being used for the treatment of choledochal cyst with acceptable morbidity and mortality. Moreover, long-term follow up of choledochal cyst patients after resection has demonstrated that although the risk of biliary malignancy is significantly decreased after choledochal cyst resection, these patients may remain at a slightly increased risk of biliary malignancy by BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3pxNPODIEKBpIl4WIJuUC3wZcoMyoyOwWjpQO3AzJmNqjsWy7MP1HEA== -

Clinical Characteristics and Incidence of Perianal Diseases in Patients with Ulcerative Colitis
Annals of Original Article Coloproctology Ann Coloproctol 2018;34(3):138-143 pISSN 2287-9714 eISSN 2287-9722 https://doi.org/10.3393/ac.2017.06.08 www.coloproctol.org Clinical Characteristics and Incidence of Perianal Diseases in Patients With Ulcerative Colitis Yong Sung Choi1, Do Sun Kim2, Doo Han Lee2, Jae Bum Lee2, Eun Jung Lee2, Seong Dae Lee2, Kee Ho Song2, Hyung Joong Jung2 Departments of 1Gastroenterology and 2Surgery, Daehang Hospital, Seoul, Korea Purpose: While perianal disease (PAD) is a characteristic of patients with Crohn disease, it has been overlooked in pa- tients with ulcerative colitis (UC). Thus, our study aimed to analyze the incidence and the clinical features of PAD in pa- tients with UC. Methods: We reviewed the data on 944 patients with an initial diagnosis of UC from October 2003 to October 2015. PAD was categorized as hemorrhoids, anal fissures, abscesses, and fistulae after anoscopic examination by experienced proctol- ogists. Data on patients’ demographics, incidence and types of PAD, medications, surgical therapies, and clinical course were analyzed. Results: The median follow-up period was 58 months (range, 12–142 months). Of the 944 UC patients, the cumulative in- cidence rates of PAD were 8.1% and 16.0% at 5 and 10 years, respectively. The incidence rates of bleeding hemorrhoids, anal fissures, abscesses, and fistulae at 10 years were 6.7%, 5.3%, 2.6%, and 3.4%, respectively. The cumulative incidence rates of perianal sepsis (abscess or fistula) were 2.2% and 4.5% at 5 and 10 years, respectively. In the multivariate analyses, male sex (risk ratio [RR], 4.6; 95% confidence interval [CI], 1.7–12.5) and extensive disease (RR, 4.2; 95% CI, 1.6–10.9) were significantly associated with the development of perianal sepsis. -

Perianal Abscess in a 2-Year-Old Presenting with a Febrile Seizure and Swelling of the Perineum Gregory M
Oxford Medical Case Reports, 2019;01, 26–28 doi: 10.1093/omcr/omy116 Case Report CASE REPORT Perianal abscess in a 2-year-old presenting with a febrile seizure and swelling of the perineum Gregory M. Taylor, DO* and Andrew H. Erlich, DO Emergency Medicine Physician, Beaumont Hospital, Teaching Hospital of Michigan State University, Department of Emergency Medicine, Farmington Hills, MI, USA *Correspondence address. Beaumont Hospital, Teaching Hospital of Michigan State University, Farmington Hills, MI, USA. E-mail: Gregory.Taylor@ Beaumont.org Abstract An anorectal abscess, specifically a perianal abscess, is a relatively uncommon infection in children. It is a purulent fluid collection under the soft tissue outside the anus. Some of these abscesses may spontaneously drain and heal by themselves, while others may result in sepsis and require surgical intervention. The transition to a systemic illness requiring hospital admission is considered rare. We present the case of a 2-year-old male presenting with a febrile seizure and found to be systemically ill secondary to a perianal abscess. To our knowledge, this is the first case reported in the literature of a febrile seizure secondary to a perianal abscess. INTRODUCTION Vitals on arrival to the ED were as follows: 103.1°F, blood pressure of 96/78 mmHg, respiratory rate 27 breaths/min, heart A perianal abscess occurs most often in male children <1 year rate 126 beats/min, weight 12.8 kg and 100% oxygen saturation of age; however, they can occur at any age and in either sex [1]. on room air. As soon as he was brought back to the treatment In one study, an incidence was reported of up to 4.3% [1]. -
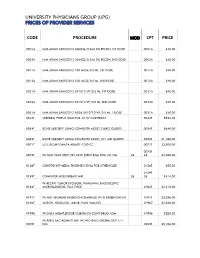
Code Procedure Cpt Price University Physicians Group
UNIVERSITY PHYSICIANS GROUP (UPG) PRICES OF PROVIDER SERVICES CODE PROCEDURE MOD CPT PRICE 0001A IMM ADMN SARSCOV2 30MCG/0.3ML DIL RECON 1ST DOSE 0001A $40.00 0002A IMM ADMN SARSCOV2 30MCG/0.3ML DIL RECON 2ND DOSE 0002A $40.00 0011A IMM ADMN SARSCOV2 100 MCG/0.5 ML 1ST DOSE 0011A $40.00 0012A IMM ADMN SARSCOV2 100 MCG/0.5 ML 2ND DOSE 0012A $40.00 0021A IMM ADMN SARSCOV2 5X1010 VP/0.5 ML 1ST DOSE 0021A $40.00 0022A IMM ADMN SARSCOV2 5X1010 VP/0.5 ML 2ND DOSE 0022A $40.00 0031A IMM ADMN SARSCOV2 AD26 5X10^10 VP/0.5 ML 1 DOSE 0031A $40.00 0042T CEREBRAL PERFUS ANALYSIS, CT W/CONTRAST 0042T $954.00 0054T BONE SURGERY USING COMPUTER ASSIST, FLURO GUIDED 0054T $640.00 0055T BONE SURGERY USING COMPUTER ASSIST, CT/ MRI GUIDED 0055T $1,188.00 0071T U/S LEIOMYOMATA ABLATE <200 CC 0071T $2,500.00 0075T 0075T PR TCAT PLMT XTRC VRT CRTD STENT RS&I PRQ 1ST VSL 26 26 $2,208.00 0126T CAROTID INT-MEDIA THICKNESS EVAL FOR ATHERSCLER 0126T $55.00 0159T 0159T COMPUTER AIDED BREAST MRI 26 26 $314.00 PR RECTAL TUMOR EXCISION, TRANSANAL ENDOSCOPIC 0184T MICROSURGICAL, FULL THICK 0184T $2,315.00 0191T PR ANT SEGMENT INSERTION DRAINAGE W/O RESERVOIR INT 0191T $2,396.00 01967 ANESTH, NEURAXIAL LABOR, PLAN VAG DEL 01967 $2,500.00 01996 PR DAILY MGMT,EPIDUR/SUBARACH CONT DRUG ADM 01996 $285.00 PR PERQ SAC AGMNTJ UNI W/WO BALO/MCHNL DEV 1/> 0200T NDL 0200T $5,106.00 PR PERQ SAC AGMNTJ BI W/WO BALO/MCHNL DEV 2/> 0201T NDLS 0201T $9,446.00 PR INJECT PLATELET RICH PLASMA W/IMG 0232T HARVEST/PREPARATOIN 0232T $1,509.00 0234T PR TRANSLUMINAL PERIPHERAL ATHERECTOMY, RENAL -

Anal Fissure
Anal Fissure What is an anal fissure? An anal fissure is a small tear in the skin of the anus. The anus is the opening of the rectum where bowel movements (BMs) leave the body. Anal fissures are a fairly common problem. What is the cause? A tear may happen when you have: • Hard, dry bowel movements • Constipation • Hemorrhoids • Anal surgery • Inflammation of the rectum caused by intestinal problems such as Crohn's disease What are the symptoms? Symptoms may include: • Pain during or after bowel movements • Cramping of the muscle at the opening of the anus caused by irritation of the tear during a bowel movement • Bright red blood when you have a bowel movement (you may see the blood on the BM, in the toilet water, or on toilet tissue you have used) How is it diagnosed? Your healthcare provider will ask about your symptoms and examine you. You may have a procedure called an anoscopy to confirm the diagnosis. For this procedure your provider uses a small tool with a light called an anoscope to examine the anus and lower part of the rectum. Your healthcare provider may recommend other tests or procedures, such as a sigmoidoscopy or colonoscopy, to learn more about the cause of the fissure or the bleeding. How is it treated? Most fissures will heal with the following at-home treatments: • Your healthcare provider may recommend a stool softener, such as Haley's M-O, psyllium, Metamucil or Citrucel, or mineral oil. • It may help to drink lots of water and add more fiber to your diet.