Bacterial Meningitis and Neurological Complications in Adults
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Myalgic Encephalomyelitis/Chronic Fatigue
2019 Science & Discovery Webinar Series ME/CFS in the Era of the Human Microbiome: Persistent Pathogens Drive Chronic Symptoms by Interfering With Host Metabolism, Gene Expression, and Immunity with Amy Proal, Ph.D. November 14, 2019 | 1:00 PM Eastern www.SolveME.org About Our Webinars • Welcome to the 2019 Webinar Series! • The audience is muted; use the question box to send us questions. Dr. Proal will address as many questions as time permits at the end of the webinar • Webinars are recorded and the recording is made available on our YouTube channel http://youtube.com/SolveCFS • The Solve ME/CFS Initiative does not provide medical advice www.SolveCFS.org 2019 Science & Discovery Webinar Series ME/CFS in the Era of the Human Microbiome: Persistent Pathogens Drive Chronic Symptoms by Interfering With Host Metabolism, Gene Expression, and Immunity with Amy Proal, Ph.D. November 14, 2019 | 1:00 PM Eastern www.SolveME.org Myalgic Encephalomyelitis/Chronic Fatigue Syndrome in the Era of the Human Microbiome: Persistent Pathogens Drive Chronic Symptoms by Interfering With Host Metabolism, Gene Expression, and Immunity Amy Proal, Autoimmunity Research Foundation/PolyBio Millions of patients across the globe are suffering with myalgic encephalomyelitis (ME/CFS) Currently there is no one disease-specific biomarker and severely ill patients are often wheelchair dependent, bedridden and unable to perform basic tasks of work or daily living. #millionsmissing Myalgic Encephalomeylitis (ME) = swelling of the brain • Unrelenting fatigue that does -

SOS – Save Our Shoulders: a Guide for Polio Survivors
1 • Save Our Shoulders: A Guide for Polio Survivors A Guide for Polio Survivors S.O.S. Save Our Shoulders: A Guide for Polio Survivors by Jennifer Kuehl, MPT Roberta Costello, MSN, RN Janet Wechsler, PT Funding for the production of this manual was made possible by: The National Institute for Disability and Rehabilitation Research Grant #H133A000101 and The U.S. Department of the Army Grant #DAMD17-00-1-0533 Investigators: Mary Klein, PhD Mary Ann Keenan, MD Alberto Esquenazi, MD Acknowledgements We gratefully acknowledge the contributions and input provided from all of those who participated in our research. The time and effort of our participants was instrumental in the creation of this manual. Jennifer Kuehl, MPT Moss Rehabilitation Research Institute, Philadelphia Roberta Costello, MSN, RN Moss Rehabilitation Research Institute, Philadelphia Janet Wechsler, PT Moss Rehabilitation Research Institute, Philadelphia Mary Klein, PhD Moss Rehabilitation Research Institute, Philadelphia Mary Ann Keenan, MD University of Pennsylvania, Philadelphia Alberto Esquenazi, MD MossRehab Hospital, Philadelphia Cover and manual design by Ron Kalstein, MEd Albert Einstein Medical Center, Philadelphia Table of Contents 1. Introduction . .5 2. General Information About the Shoulder . .6 3. Facts About Shoulder Problems . .8 4. Treatment Options . .13 5. About Exercise . .16 6. Stretching Exercises . .19 7. Cane Stretches . .22 8. Strengthening Exercises . .25 9. Tips to Avoid Shoulder Problems . .29 10. Conclusion . .31 11. Resources . .31 The information contained within this manual is for reference only and is not a substitute for professional medical advice. Before beginning any exercise program consult your physician. Save Our Shoulders: A Guide for Polio Survivors • 4 Introduction Many polio survivors report new symptoms as they age. -

Syringomyelia in Cervical Spondylosis: a Rare Sequel H
THIEME Editorial 1 Editorial Syringomyelia in Cervical Spondylosis: A Rare Sequel H. S. Bhatoe1 1 Department of Neurosciences, Max Super Specialty Hospital, Patparganj, New Delhi, India Indian J Neurosurg 2016;5:1–2. Neurological involvement in cervical spondylosis usually the buckled hypertrophic ligament flavum compresses the implies radiculopathy or myelopathy. Cervical spondylotic cord. Ischemia due to compromise of microcirculation and myelopathy is the commonest cause of myelopathy in the venous congestion, leading to focal demyelination.3 geriatric age group,1 and often an accompaniment in adult Syringomyelia is an extremely rare sequel of chronic cervical patients manifesting central cord syndrome and spinal cord cord compression due to spondylotic process, and manifests as injury without radiographic abnormality. Myelopathy is the accelerated myelopathy (►Fig. 1). Pathogenesis of result of three factors that often overlap: mechanical factors, syringomyelia is uncertain. Al-Mefty et al4 postulated dynamic-repeated microtrauma, and ischemia of spinal cord occurrence of myelomalacia due to chronic compression of microcirculation.2 Age-related mechanical changes include the cord, followed by phagocytosis, leading to a formation of hypertrophy of the ligamentum flavum, formation of the cavity that extends further. However, Kimura et al5 osteophytic bars, degenerative disc prolapse, all of them disagreed with this hypothesis, and postulated that following contributing to a narrowing of the spinal canal. Degenerative compression of the cord, there is slosh effect cranially and kyphosis and subluxation often aggravates the existing caudally, leading to an extension of the syrinx. It is thus likely compressiononthespinalcord.Flexion–extension that focal cord cavitation due to compression and ischemia movements of the spinal cord places additional, dynamic occurs due to periventricular fluid egress into the cord, the stretch on the cord that is compressed. -

Fatigue After Stroke
SPECIAL REPORT Fatigue after stroke PJ Tyrrell Fatigue is a common symptom after stroke. It is not invariably related to stroke severity & DG Smithard† and can occur in the absence of depression. It is one of the most troublesome symptoms for †Author for correspondence many patients and yet nothing is known of its causation. There are no specific treatments. William Harvey Hospital, Richard Steven’s Ward, This article assesses the available literature in the context of what is known about fatigue Ashford, Kent, in other disorders. Post-stroke fatigue may be a manifestation of sickness behavior, TN24 0LZ, UK mediated through the central effects of the cytokine interleukin-1, perhaps via effects on Tel.: +44 123 361 6214 Fax: +44 123 361 6662 glutamate neurotransmission. Possible therapeutic strategies are discussed which might be [email protected] a logical basis from which to plan randomized control trials. Following stroke, approximately a third of common and disabling symptom of Parkinson’s patients die, a third recover and a third remain disease [7,8] and of systemic lupus [9]. More than significantly disabled. Even those who recover 90% of patients with poliomyelitis develop a physically may be left with significant emotional delayed syndrome of post-myelitis fatigue [10]. and psychologic dysfunction – including anxi- Fatigue is the most prevalent symptom of ety, readjustment reactions and depression. One patients with cancer who receive radiation, cyto- common but often overlooked symptom is toxic or other therapies [11], and it may persist fatigue. This may occur soon or late after stroke, for years after the cessation of treatment [12]. -

Degenerative Cervical Myelopathy: Clinical Presentation, Assessment, and Natural History
Journal of Clinical Medicine Review Degenerative Cervical Myelopathy: Clinical Presentation, Assessment, and Natural History Melissa Lannon and Edward Kachur * Division of Neurosurgery, McMaster University, Hamilton, ON L8S 4L8, Canada; [email protected] * Correspondence: [email protected] Abstract: Degenerative cervical myelopathy (DCM) is a leading cause of spinal cord injury and a major contributor to morbidity resulting from narrowing of the spinal canal due to osteoarthritic changes. This narrowing produces chronic spinal cord compression and neurologic disability with a variety of symptoms ranging from mild numbness in the upper extremities to quadriparesis and incontinence. Clinicians from all specialties should be familiar with the early signs and symptoms of this prevalent condition to prevent gradual neurologic compromise through surgical consultation, where appropriate. The purpose of this review is to familiarize medical practitioners with the pathophysiology, common presentations, diagnosis, and management (conservative and surgical) for DCM to develop informed discussions with patients and recognize those in need of early surgical referral to prevent severe neurologic deterioration. Keywords: degenerative cervical myelopathy; cervical spondylotic myelopathy; cervical decompres- sion Citation: Lannon, M.; Kachur, E. Degenerative Cervical Myelopathy: Clinical Presentation, Assessment, 1. Introduction and Natural History. J. Clin. Med. Degenerative cervical myelopathy (DCM) is now the leading cause of spinal cord in- 2021, 10, 3626. https://doi.org/ jury [1,2], resulting in major disability and reduced quality of life. While precise prevalence 10.3390/jcm10163626 is not well described, a 2017 Canadian study estimated a prevalence of 1120 per million [3]. DCM results from narrowing of the spinal canal due to osteoarthritic changes. This Academic Editors: Allan R. -

A Histopathological and Immunohistochemical Study of Acute and Chronic Human Compressive Myelopathy
Cellular Pathology and Apoptosis in Experimental and Human Acute and Chronic Compressive Myelopathy ROWENA ELIZABETH ANNE NEWCOMBE M.B.B.S. B.Med Sci. (Hons.) Discipline of Pathology, School of Medical Sciences University of Adelaide June 2010 A thesis submitted in partial fulfilment of the requirements for the degree of Doctor of Philosophy CHAPTER 1 INTRODUCTION 1 The term “compressive myelopathy” describes a spectrum of spinal cord injury secondary to compressive forces of varying magnitude and duration. The compressive forces may act over a short period of time, continuously, intermittently or in varied combination and depending on their magnitude may produce a spectrum varying from mild to severe injury. In humans, spinal cord compression may be due to various causes including sudden fracture/dislocation and subluxation of the vertebral column, chronic spondylosis, disc herniation and various neoplasms involving the vertebral column and spinal canal. Neoplasms may impinge on the spinal cord and arise from extramedullary or intramedullary sites. Intramedullary expansion producing a type of internal compression can be due to masses created by neoplasms or fluid such as the cystic cavitation seen in syringomyelia. Acute compression involves an immediate compression of the spinal cord from lesions such as direct trauma. Chronic compression may develop over weeks to months or years from conditions such as cervical spondylosis which may involve osteophytosis or hypertrophy of the adjacent ligamentum flavum. Compressive myelopathies include the pathological changes from direct mechanical compression at one or multiple levels and changes in the cord extending multiple segments above and below the site of compression. Evidence over the past decade suggests that apoptotic cell death in neurons and glia, in particular of oligodendrocytes, may play an important role in the pathophysiology and functional outcome of human chronic compressive myelopathy. -

African Meningitis Belt
WHO/EMC/BAC/98.3 Control of epidemic meningococcal disease. WHO practical guidelines. 2nd edition World Health Organization Emerging and other Communicable Diseases, Surveillance and Control This document has been downloaded from the WHO/EMC Web site. The original cover pages and lists of participants are not included. See http://www.who.int/emc for more information. © World Health Organization This document is not a formal publication of the World Health Organization (WHO), and all rights are reserved by the Organization. The document may, however, be freely reviewed, abstracted, reproduced and translated, in part or in whole, but not for sale nor for use in conjunction with commercial purposes. The views expressed in documents by named authors are solely the responsibility of those authors. The mention of specific companies or specific manufacturers' products does no imply that they are endorsed or recommended by the World Health Organization in preference to others of a similar nature that are not mentioned. CONTENTS CONTENTS ................................................................................... i PREFACE ..................................................................................... vii INTRODUCTION ......................................................................... 1 1. MAGNITUDE OF THE PROBLEM ........................................................3 1.1 REVIEW OF EPIDEMICS SINCE THE 1970S .......................................................................................... 3 Geographical distribution -
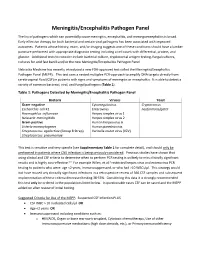
Meningitis/Encephalitis Pathogen Panel
Meningitis/Encephalitis Pathogen Panel The list of pathogens which can potentially cause meningitis, encephalitis, and meningoencephalitis is broad. Early effective therapy for both bacterial and certain viral pathogens has been associated with improved outcomes. Patients whose history, exam, and/or imaging suggests one of these conditions should have a lumber puncture performed with appropriate diagnostic testing including a cell count with differential, protein, and glucose. Additional tests to consider include bacterial culture, cryptococcal antigen testing, fungal cultures, cultures for acid fast bacilli and/or the new Meningitis/Encephalitis Pathogen Panel. Nebraska Medicine has recently introduced a new FDA-approved test called the Meningitis/Encephalitis Pathogen Panel (MEPP). This test uses a nested multiplex PCR-approach to amplify DNA targets directly from cerebrospinal fluid (CSF) in patients with signs and symptoms of meningitis or encephalitis. It is able to detect a variety of common bacterial, viral, and fungal pathogens (Table 1). Table 1: Pathogens Detected by Meningitis/Encephalitis Pathogen Panel Bacteria Viruses Yeast Gram-negative Cytomegalovirus Cryptococcus Escherichia coli K1 Enterovirus neoformans/gattii Haemophilus influenzae Herpes simplex virus 1 Neisseria meningitidis Herpes simplex virus 2 Gram-positive Human herpesvirus 6 Listeria monocytogenes Human parechovirus Streptococcus agalactiae (Group B Strep) Varicella zoster virus (VZV) Streptococcus pneumoniae This test is sensitive and very specific (see Supplementary Table 1 for complete detail), and should only be performed in patients where CNS infection is being seriously considered. Previous studies have shown that using clinical and CSF criteria to determine when to perform PCR testing is unlikely to miss clinically significant results and is highly cost-effective.1-3 For example Wilen, et al.3 restricted herpes virus and enterovirus PCR testing to patients who were: age <2 years, immunosuppressed, or who had >10 WBCs/µl. -
Stroke: Learn the Warning Signs and Protect Yourself Strokes Are the Leading Cause of Major Disability in the U.S
stroke: learn the warning signs and protect yourself Strokes are the leading cause of major disability in the U.S. and the second leading cause of death worldwide. With all the emphasis placed on heart disease reaches us, they’ve already been to the hospital. The and cancer as the two leading causes of death in only thing left by then is active physical therapy.” America, people often forget what ranks as third. The answer is stroke, and it can have debilitating Dr. Ray says that is why he preaches religiously effects even if you survive. to patients about lowering blood pressure and cholesterol, healthy diet and regular exercise, and On average, someone has a stroke in the U.S. every keeping any pre-existing conditions in check through 45 seconds, which equals 700,000 strokes a year. regular checkups. He goes on to say that having a Of these, about 500,000 are first-time strokes. primary care physician is vital. Strokes are so pervasive that they are the leading cause of major disability in the “All adults should speak to their doctors U.S. and the second leading cause of death about diet and controlling their blood worldwide. pressure,” Dr. Ray says. “You want to actively prevent this before it happens.” A stroke occurs when blood flow to parts of the brain is restricted or impaired, There are two basic types of stroke. The first killing off brain cells. Those cells can never is ischemic stroke caused by blood clots or regenerate, which means the damage is other particles in the blood vessels leading permanent. -

Epilepsy After Stroke
Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Epilepsy after stroke In the first few weeks after a stroke some people have a seizure, and a small number go on to develop epilepsy – a tendency to have repeated seizures. These can usually be completely controlled with treatment. This factsheet explains what epilepsy is, the different types of seizures, and how epilepsy is diagnosed and treated. It also includes advice about coping with a seizure, and a glossary. Epilepsy is a tendency to have repeated What causes seizures? seizures – sometimes called ‘fits’ or ‘attacks’. It affects just under one per cent Cells in the brain communicate with one of people in the UK. Stroke is one of many another and with our muscles by passing conditions that can lead to epilepsy. electrical signals along nerve fibres. If you have epilepsy this electrical activity can Around five per cent of people who have a become disordered. A sudden abnormal stroke will have a seizure within the following burst of electrical activity in the brain can few weeks. These are known as acute or lead to a seizure. onset seizures and normally happen within 24 hours of the stroke. You are more likely There are over 40 different types of seizures to have one if you have had a severe stroke, ranging from tingling sensations or ‘going a stroke caused by bleeding in the brain (a blank’ for a few seconds, to shaking and haemorrhagic stroke), or a stroke involving losing consciousness. the part of the brain called the cerebral cortex. If you have an onset seizure, it This can mean that epilepsy is sometimes does not necessarily mean you have or will confused with other conditions, including develop epilepsy. -

Paraneoplastic Neurological and Muscular Syndromes
Paraneoplastic neurological and muscular syndromes Short compendium Version 4.5, April 2016 By Finn E. Somnier, M.D., D.Sc. (Med.), copyright ® Department of Autoimmunology and Biomarkers, Statens Serum Institut, Copenhagen, Denmark 30/01/2016, Copyright, Finn E. Somnier, MD., D.S. (Med.) Table of contents PARANEOPLASTIC NEUROLOGICAL SYNDROMES .................................................... 4 DEFINITION, SPECIAL FEATURES, IMMUNE MECHANISMS ................................................................ 4 SHORT INTRODUCTION TO THE IMMUNE SYSTEM .................................................. 7 DIAGNOSTIC STRATEGY ..................................................................................................... 12 THERAPEUTIC CONSIDERATIONS .................................................................................. 18 SYNDROMES OF THE CENTRAL NERVOUS SYSTEM ................................................ 22 MORVAN’S FIBRILLARY CHOREA ................................................................................................ 22 PARANEOPLASTIC CEREBELLAR DEGENERATION (PCD) ...................................................... 24 Anti-Hu syndrome .................................................................................................................. 25 Anti-Yo syndrome ................................................................................................................... 26 Anti-CV2 / CRMP5 syndrome ............................................................................................ -

Acute Ischemic Stroke in Young Adults with Tuberculous Meningitis Liming Zhang1, Xiaoyu Zhang2, Huaqiang Li1,3, Gang Chen1* and Meijia Zhu2*
Zhang et al. BMC Infectious Diseases (2019) 19:362 https://doi.org/10.1186/s12879-019-4004-5 RESEARCHARTICLE Open Access Acute ischemic stroke in young adults with tuberculous meningitis Liming Zhang1, Xiaoyu Zhang2, Huaqiang Li1,3, Gang Chen1* and Meijia Zhu2* Abstract Background: Ischemic stroke is a common complication in patients with tuberculous meningitis (TBM), which is associated with poor clinical outcome. However, risk factors of stroke in TBM patients were not fully understood, especially in those young adults. Therefore, the aim of our study was to identify risk factors for acute ischemic stroke in young adults with TBM. Methods: TBM patients (18 to 50 years) without cerebral vascular risk factors were prospective recruited between Feb 2014 and Dec 2017. Patients were defined as stroke group and non-stroke group by brain magnetic resonance imaging (MRI). Demographic characteristics, clinical presentations, cerebrospinal fluid (CSF) examination, basal meningeal enhancement, hydrocephalus, tuberculoma and clinical outcome were compared between two groups. Binary logistic regression was performed to determine risk factors for acute ischemic stroke in young TBM patients. Results: Fifty-two patients with TBM were included and 12 (23.1%) patients were in stroke group. Patients in stroke group were older. Clinical presentations were comparable between two groups except headache was more common in TBM patients with stroke. In CSF examination, TBM patients with stroke had higher CSF white blood cell. By MRI, patients in stroke group were more likely to have basal meningeal enhancement but less likely to present tuberculoma. Compared to non-stroke group, patients in stroke group had worse short-term clinical outcome.