7. Headache Attributed to Non-Vascular Intracranial Disorder
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Brain Abscess Review of 89 Cases Over a Period of 30 Years
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.36.5.757 on 1 October 1973. Downloaded from Journal ofNeurology, Neurosurgery, and Psychiatry, 1973, 36, 757-768 Brain abscess Review of 89 cases over a period of 30 years A. J. BELLER, A. SAHAR, AND I. PRAISS From the Department ofNeurosurgery, Hadassah Hebrew University Hospital, Jerusalem, Israel SUMMARY Eighty-nine cases of brain abscess, diagnosed over a period of 30 years, are reviewed. The incidence of this disease did not decline throughout the period. Abscesses of ear and nose origin constituted the largest group (38%). Postoperative abscesses seem to have increased in inci- dence, presumably due to routine postoperative antibiotic treatment. Antibiotics were possibly responsible for the suppression of signs of infection in 4500 of the patients, who presented as suffering from a space-occupying lesion. The most accurate diagnostic tool was angiography, which localized the lesion in 9000 and suggested its nature in 61%. Brain scan may prove as satisfactory. Staphylococcus was cultured in about two-thirds of the cases. Mortality seemed to decrease con- comitantly with the advent of more potent antibiotics. The treatment of choice in terms of both Protected by copyright. mortality and morbidity seemed to be enucleation after previous sterilization. The hazards of radical surgery should be taken into consideration. The multiplicity of factors involved in the or subdural collections of pus were not included management of brain abscess complicates its in this study. evaluation. Surgical therapy in the pre-anti- biotic era carried a mortality of 61% (Webster FINDINGS AND COMMENTS and Gurdjian, 1950). -

Headache Diagnosis and Management 2018 Update in Internal Medicine October 25, 2018
Headache Diagnosis and Management 2018 Update in Internal Medicine October 25, 2018 Laurie Knepper MD Associate Professor of Neurology University of Pittsburgh School of Medicine A 22 year old comes to the office with increasing headache. She had headaches as a child, for which she would have to leave school because she was vomiting. These decreased as she got older and were mainly before the onset of her period. Now, for the past 5 months, the headaches have been occurring 3-4 days/week. She become tired and yawny the day before, and with severe headaches, she has dizziness and difficulty focusing her eyes. The day after she is mentally foggy. The Primary Headache ICHD 3 (2013) • Migraine • 1.1 Migraine without aura 80% • 1.2 Migraine with aura 20-30% • 1.3 Chronic migraine 2.5% • Tension Type Headache • Trigeminal Autonomic Neuralgias • Cluster, Paroxysmal Hemicrania, SUNCT, Hemicrania continua • Other primary Headache disorders • Cough, exercise, sexual ,stabbing, Hypnic, New daily persistent Migraine without aura A. At least 5 attacks B. Lasting 4-72 hours C. At least two of: A. Unilateral B. Pulsating C. Moderate or severe pain intensity D. Aggravated by physical activity D. During headache at least one of: A. Nausea and/or vomiting B. Photophobia , phonophobia E. Symptoms not attributed to another disorder Epidemiology • Lifetime prevalence of headache: 66% Migraine: 18% women, 6% men • 28 million in US with migraines • Highest prevalence is mid life => decreased work • $13 billion cost each year- ER, lost income, etc • 40% of migraine patients would benefit from preventative meds Only 13% receive effective preventative treatment • Studies note most “ sinus headaches” are migraines •2/3 of migraines are managed by primary care! The anatomy of Migraine A 49 year old woman presents to your headache clinic for evaluation of new episodes of right arm numbness and speech difficulty. -

Myalgic Encephalomyelitis/Chronic Fatigue
2019 Science & Discovery Webinar Series ME/CFS in the Era of the Human Microbiome: Persistent Pathogens Drive Chronic Symptoms by Interfering With Host Metabolism, Gene Expression, and Immunity with Amy Proal, Ph.D. November 14, 2019 | 1:00 PM Eastern www.SolveME.org About Our Webinars • Welcome to the 2019 Webinar Series! • The audience is muted; use the question box to send us questions. Dr. Proal will address as many questions as time permits at the end of the webinar • Webinars are recorded and the recording is made available on our YouTube channel http://youtube.com/SolveCFS • The Solve ME/CFS Initiative does not provide medical advice www.SolveCFS.org 2019 Science & Discovery Webinar Series ME/CFS in the Era of the Human Microbiome: Persistent Pathogens Drive Chronic Symptoms by Interfering With Host Metabolism, Gene Expression, and Immunity with Amy Proal, Ph.D. November 14, 2019 | 1:00 PM Eastern www.SolveME.org Myalgic Encephalomyelitis/Chronic Fatigue Syndrome in the Era of the Human Microbiome: Persistent Pathogens Drive Chronic Symptoms by Interfering With Host Metabolism, Gene Expression, and Immunity Amy Proal, Autoimmunity Research Foundation/PolyBio Millions of patients across the globe are suffering with myalgic encephalomyelitis (ME/CFS) Currently there is no one disease-specific biomarker and severely ill patients are often wheelchair dependent, bedridden and unable to perform basic tasks of work or daily living. #millionsmissing Myalgic Encephalomeylitis (ME) = swelling of the brain • Unrelenting fatigue that does -

Spontaneous Spinal Cerebrospinal Fluid Leaks and Intracranial Hypotension
CLINICAL REVIEW CLINICIAN’S CORNER Spontaneous Spinal Cerebrospinal Fluid Leaks and Intracranial Hypotension Wouter I. Schievink, MD Context Spontaneous intracranial hypotension is caused by spontaneous spinal ce- PATIENT PRESENTS WITH A rebrospinal fluid (CSF) leaks and is known for causing orthostatic headaches. It is an new headache that occurs important cause of new headaches in young and middle-aged individuals, but initial shortly after assuming an up- misdiagnosis is common. right position and is re- Objective To summarize existing evidence regarding the epidemiology, pathophysi- Alieved by lying down. Although such a ology, diagnosis, and management of spontaneous spinal CSF leaks and intracranial positional headache pattern is well- hypotension. known following a diagnostic lumbar Evidence Acquisition MEDLINE (1966-2005) and OLDMEDLINE (1950-1965) were puncture, the spontaneous onset of an searched using the terms intracranial hypotension, CSF leak, low pressure headache, orthostatic headache is not well recog- and CSF hypovolemia. Reference lists of these articles and ongoing investigations in nized and the patient may be diag- this area were used as well. nosed with migraine, tension head- Evidence Synthesis Spontaneous intracranial hypotension is caused by single or ache, viral meningitis, or malingering. multiple spinal CSF leaks. The incidence has been estimated at 5 per 100 000 per year, This has been a typical scenario for with a peak around age 40 years. Women are affected more commonly than men. Mechanical factors combine with an underlying connective tissue disorder to cause many patients experiencing spontane- 1 the CSF leaks. An orthostatic headache is the prototypical manifestation but other head- ous intracranial hypotension. -

Pseudomigraine with Pleocytosis
P1: KWW/KKL P2: KWW/HCN QC: KWW/FLX T1: KWW GRBT050-115 Olesen- 2057G GRBT050-Olesen-v6.cls August 17, 2005 1:50 ••Chapter 115 ◗ Pseudomigraine with Pleocytosis Dimos D. Mitsikostas and Julio Pascual Other terms: migraine variants, headache and neurologic dle cerebral artery (9). Alternatively, imaging studies sug- deficits with cerebrospinal fluid lymphocytosis (HaNDL) gest that neurologic deficits of HaDNL might be caused by cortical spreading depression (5,6), as in migraine with aura. Furthermore, overlap of clinical presentations be- INTRODUCTION tween HaNDL and familial hemiplegic migraine triggered a search for mutations in the CACNA1A gene, which were Pseudomigraine is a term first introduced in 1983 to not found (4). Finally, the CSF inflammatory picture of describe attacks of temporary neurologic deficit accom- HaNDL suggests an inflammatory, autoimmune, or postin- panied or followed by migrainous headache and cere- fectious etiology, and supportive data are awaited. brospinal fluid (CSF) pleocytosis of unknown origin and automatic relief (10). Similar clinical presentations were reported previously under different names, such as mi- PRESENTATION AND EVALUATION graine variants (1,13). Diagnostic criteria (Revised International Classification for Headache Disorders [ICHD-II]) of HaNDL are listed EPIDEMIOLOGY in Table 115-1. The clinical characteristics of HaNDL are: (1) more than two discrete episodes of temporal focal Fewer than 100 cases of HaNDL are reported in the liter- neurologic (most often sensory plus aphasic) symptoms ature (2,7), but it may be underdiagnosed as estimates of followed by moderate to severe headache and (2) com- its annual incidence are up to 0.2 cases per 100,000 inhab- plete and spontaneous relief of the condition after a few itants (11). -

Migraine: Spectrum of Symptoms and Diagnosis
KEY POINT: MIGRAINE: SPECTRUM A Most patients develop migraine in the first 3 OF SYMPTOMS decades of life, some in the AND DIAGNOSIS fourth and even the fifth decade. William B. Young, Stephen D. Silberstein ABSTRACT The migraine attack can be divided into four phases. Premonitory phenomena occur hours to days before headache onset and consist of psychological, neuro- logical, or general symptoms. The migraine aura is comprised of focal neurological phenomena that precede or accompany an attack. Visual and sensory auras are the most common. The migraine headache is typically unilateral, throbbing, and aggravated by routine physical activity. Cutaneous allodynia develops during un- treated migraine in 60% to 75% of cases. Migraine attacks can be accompanied by other associated symptoms, including nausea and vomiting, gastroparesis, di- arrhea, photophobia, phonophobia, osmophobia, lightheadedness and vertigo, and constitutional, mood, and mental changes. Differential diagnoses include cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoenphalopathy (CADASIL), pseudomigraine with lymphocytic pleocytosis, ophthalmoplegic mi- graine, Tolosa-Hunt syndrome, mitochondrial disorders, encephalitis, ornithine transcarbamylase deficiency, and benign idiopathic thunderclap headache. Migraine is a common episodic head- (Headache Classification Subcommittee, ache disorder with a 1-year prevalence 2004): of approximately 18% in women, 6% inmen,and4%inchildren.Attacks Recurrent attacks of headache, consist of various combinations of widely varied in intensity, fre- headache and neurological, gastrointes- quency, and duration. The attacks tinal, and autonomic symptoms. Most are commonly unilateral in onset; patients develop migraine in the first are usually associated with an- 67 3 decades of life, some in the fourth orexia and sometimes with nausea and even the fifth decade. -

Infections in Deep Brain Stimulator Surgery
Open Access Original Article DOI: 10.7759/cureus.5440 Infections in Deep Brain Stimulator Surgery Jacob E. Bernstein 1 , Samir Kashyap 1 , Kevin Ray 1 , Ajay Ananda 2 1. Neurosurgery, Riverside University Health System Medical Center, Moreno Valley, USA 2. Neurosurgery, Kaiser Permanente, Los Angeles, USA Corresponding author: Jacob E. Bernstein, [email protected] Abstract Introduction: Deep brain stimulation has emerged as an effective treatment for movement disorders such as Parkinson’s disease, dystonia, and essential tremor with estimates of >100,000 deep brain stimulators (DBSs) implanted worldwide since 1980s. Infections rates vary widely in the literature with rates as high as 25%. Traditional management of infection after deep brain stimulation is systemic antibiotic therapy with wound incision and debridement (I&D) and removal of implanted DBS hardware. The aim of this study is to evaluate the infections occurring after DBS placement and implantable generator (IPG) placement in order to better prevent and manage these infections. Materials/Methods: We conducted a retrospective review of 203 patients who underwent implantation of a DBS at a single institution. For initial electrode placement, patients underwent either unilateral or bilateral electrode placement with implantation of the IPG at the same surgery and IPG replacements occurred as necessary. For patients with unilateral electrodes, repeat surgery for placement of contralateral electrode was performed when desired. Preoperative preparation with ethyl alcohol occurred in all patients while use of intra-operative vancomycin powder was surgeon dependent. All patients received 24 hours of postoperative antibiotics. Primary endpoint was surgical wound infection or brain abscess located near the surgically implanted DBS leads. -

African Meningitis Belt
WHO/EMC/BAC/98.3 Control of epidemic meningococcal disease. WHO practical guidelines. 2nd edition World Health Organization Emerging and other Communicable Diseases, Surveillance and Control This document has been downloaded from the WHO/EMC Web site. The original cover pages and lists of participants are not included. See http://www.who.int/emc for more information. © World Health Organization This document is not a formal publication of the World Health Organization (WHO), and all rights are reserved by the Organization. The document may, however, be freely reviewed, abstracted, reproduced and translated, in part or in whole, but not for sale nor for use in conjunction with commercial purposes. The views expressed in documents by named authors are solely the responsibility of those authors. The mention of specific companies or specific manufacturers' products does no imply that they are endorsed or recommended by the World Health Organization in preference to others of a similar nature that are not mentioned. CONTENTS CONTENTS ................................................................................... i PREFACE ..................................................................................... vii INTRODUCTION ......................................................................... 1 1. MAGNITUDE OF THE PROBLEM ........................................................3 1.1 REVIEW OF EPIDEMICS SINCE THE 1970S .......................................................................................... 3 Geographical distribution -

Parkinsonian Symptoms in Normal Pressure Hydrocephalus: a Population-Based Study
http://www.diva-portal.org This is the published version of a paper published in Journal of Neurology. Citation for the original published paper (version of record): Molde, K., Söderström, L., Laurell, K. (2017) Parkinsonian symptoms in normal pressure hydrocephalus: a population-based study. Journal of Neurology, 264(10): 2141-2148 https://doi.org/10.1007/s00415-017-8598-5 Access to the published version may require subscription. N.B. When citing this work, cite the original published paper. Permanent link to this version: http://urn.kb.se/resolve?urn=urn:nbn:se:umu:diva-142915 J Neurol (2017) 264:2141–2148 DOI 10.1007/s00415-017-8598-5 ORIGINAL COMMUNICATION Parkinsonian symptoms in normal pressure hydrocephalus: a population‑based study Karin Molde1 · Lars Söderström1 · Katarina Laurell1 Received: 3 June 2017 / Revised: 17 August 2017 / Accepted: 18 August 2017 / Published online: 6 September 2017 © The Author(s) 2017. This article is an open access publication Abstract It may be challenging to diferentiate normal liberal use of neuroradiological imaging when investigating pressure hydrocephalus (NPH) from neurodegenerative a patient with parkinsonian features. disorders such as Parkinson’s disease. In this population- based study, we wanted to describe the frequency of par- Keywords Normal pressure hydrocephalus · kinsonian symptoms among individuals with and without Hydrocephalus · Parkinsonism · Parkinson’s disease · NPH, and whether the motor examination part of the Unifed UPDRS Parkinson’s Disease Rating Scale (UPDRS-m) score difers between these groups. Furthermore, we wanted to fnd out whether there was a relationship between UPDRS-m score, Introduction NPH symptoms, and radiological signs of NPH. -

DIAGNOSTICS and THERAPY of INCREASED INTRACRANIAL PRESSURE in ISCHEMIC STROKE
DIAGNOSTICS and THERAPY of INCREASED INTRACRANIAL PRESSURE in ISCHEMIC STROKE Erich Schmutzhard INNSBRUCK, AUSTRIA e - mail: erich.schmutzhard@i - med.ac.at Neuro - ICU Innsbruck Conflict of interest : Speaker‘s honoraria from ZOLL Medical and Honoraria for manuscripts from Pfizer Neuro - ICU Innsbruck OUTLINE Introduction Definition: ICP, CPP, PbtiO2, metabolic monitoring, lactate , pyruvate , brain temperature etc Epidemiology of ischemic stroke and ICP elevation in ischemic stroke ACM infarction and the role of collaterals and/ or lack of collaterals for ICP etc Hydrocephalus in posterioir fossa ( mainly cerebellar ) infarction Diagnosis of ICP etc Monitoring of ICP etc Therapeutic management : decompressive craniectomy – meta - analysis of DESTINY HAMLET und co deepening of analgosedation , ventilation , hyperventilation , osmotherapy , CPP - oriented th , MAP management , hypothermia , prophylactic normothermia , external ventricular drainage Neuro - ICU Innsbruck Introduction - Malignant cerebral edema following ischemic stroke is life threatening. - The pathophysiology of brain edema involves failure of the sodium - potassium adenosine triphosphatase pump and disruption of the blood - brain barrier, leading to cytotoxic edema and cellular death. - The Monro - Kellie doctrine clearlc states that - since the brain is encased in a finite space - increased intracranial pressure (ICP) due to cerebral edema can result in herniation through the foramen magnum and openings formed by the falx and tentorium. - Moreover, elevated ICP can cause secondary brain ischemia through decreased cerebral perfusion and blood flow, brain tissue hypoxia, and metabolic crisis. - Direct cerebrovascular compression caused by brain tissue shifting can lead to secondary infarction, especially in the territories of the anterior and posterior cerebral artery. - Tissue shifts can also stretch and tear cerebral vessels, causing intracranial hemorrhage such as Duret’s hemorrhage of the brainstem. -

Hydrocephalus Patient Information Guide Experience Life Without Boundaries
Hydrocephalus Patient Information Guide Experience Life Without Boundaries Aesculap Neurosurgery 2 Table of Contents Foreword Page 4 About Us Page 5 What Is Hydrocephalus Page 6 Types Of Hydrocephalus Page 7 What You Should Know Page 8 Diagnosis Page 9 Treatment/Goal/Surgical Procedure Page 10 Complications Page 10 Prognosis/Helpful Sites Page 11 The Aesculap Shunts Page 12 Medical Definitions Page 13 3 Foreword The intention of this booklet is to provide information to patients, family members, caregivers and friends on the subject of hydrocephalus. The information provided is a general overview of the diagnosis and treatment of hydrocephalus and other conditions associated with hydrocephalus. About us History Aesculap AG (Germany) was founded in 1867 by Gottfried Jetter, a master craftsman trained in surgical instrument and cutlery techniques. Jetter’s original workshop, located in Tuttlingen, Germany, is the same location where Aesculap world headquarters resides today. The employee count has increased over the years (3,000+ employees), and the number of instrument patterns has grown from a select few to over 17,000; however, the German standard for quality and pattern consistency remains the same. Prior to 1977, many of the instruments sold in America by competing companies were sourced from Aesculap in Tuttlingen. In response to the United States customer demand for Aesculap quality surgical instruments, Aesculap, Inc. (U.S.) was established in 1977. Headquartered in Center Valley, Pennsylvania, with over one hundred direct nationwide sales representatives, Aesculap, Inc. currently supports the marketing, sales and distribution of Aesculap surgical instrumentation in the U.S. In order to support the company’s continued growth and provide the service and quality which customers have come to expect, Aesculap relocated the corporate offices from San Francisco to Center Valley, Pennsylvania. -
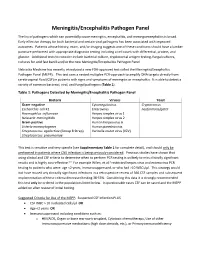
Meningitis/Encephalitis Pathogen Panel
Meningitis/Encephalitis Pathogen Panel The list of pathogens which can potentially cause meningitis, encephalitis, and meningoencephalitis is broad. Early effective therapy for both bacterial and certain viral pathogens has been associated with improved outcomes. Patients whose history, exam, and/or imaging suggests one of these conditions should have a lumber puncture performed with appropriate diagnostic testing including a cell count with differential, protein, and glucose. Additional tests to consider include bacterial culture, cryptococcal antigen testing, fungal cultures, cultures for acid fast bacilli and/or the new Meningitis/Encephalitis Pathogen Panel. Nebraska Medicine has recently introduced a new FDA-approved test called the Meningitis/Encephalitis Pathogen Panel (MEPP). This test uses a nested multiplex PCR-approach to amplify DNA targets directly from cerebrospinal fluid (CSF) in patients with signs and symptoms of meningitis or encephalitis. It is able to detect a variety of common bacterial, viral, and fungal pathogens (Table 1). Table 1: Pathogens Detected by Meningitis/Encephalitis Pathogen Panel Bacteria Viruses Yeast Gram-negative Cytomegalovirus Cryptococcus Escherichia coli K1 Enterovirus neoformans/gattii Haemophilus influenzae Herpes simplex virus 1 Neisseria meningitidis Herpes simplex virus 2 Gram-positive Human herpesvirus 6 Listeria monocytogenes Human parechovirus Streptococcus agalactiae (Group B Strep) Varicella zoster virus (VZV) Streptococcus pneumoniae This test is sensitive and very specific (see Supplementary Table 1 for complete detail), and should only be performed in patients where CNS infection is being seriously considered. Previous studies have shown that using clinical and CSF criteria to determine when to perform PCR testing is unlikely to miss clinically significant results and is highly cost-effective.1-3 For example Wilen, et al.3 restricted herpes virus and enterovirus PCR testing to patients who were: age <2 years, immunosuppressed, or who had >10 WBCs/µl.