Anatomy of Pelvic Floor Dysfunction
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Reference Sheet 1
MALE SEXUAL SYSTEM 8 7 8 OJ 7 .£l"00\.....• ;:; ::>0\~ <Il '"~IQ)I"->. ~cru::>s ~ 6 5 bladder penis prostate gland 4 scrotum seminal vesicle testicle urethra vas deferens FEMALE SEXUAL SYSTEM 2 1 8 " \ 5 ... - ... j 4 labia \ ""\ bladderFallopian"k. "'"f"";".'''¥'&.tube\'WIT / I cervixt r r' \ \ clitorisurethrauterus 7 \ ~~ ;~f4f~ ~:iJ 3 ovaryvagina / ~ 2 / \ \\"- 9 6 adapted from F.L.A.S.H. Reproductive System Reference Sheet 3: GLOSSARY Anus – The opening in the buttocks from which bowel movements come when a person goes to the bathroom. It is part of the digestive system; it gets rid of body wastes. Buttocks – The medical word for a person’s “bottom” or “rear end.” Cervix – The opening of the uterus into the vagina. Circumcision – An operation to remove the foreskin from the penis. Cowper’s Glands – Glands on either side of the urethra that make a discharge which lines the urethra when a man gets an erection, making it less acid-like to protect the sperm. Clitoris – The part of the female genitals that’s full of nerves and becomes erect. It has a glans and a shaft like the penis, but only its glans is on the out side of the body, and it’s much smaller. Discharge – Liquid. Urine and semen are kinds of discharge, but the word is usually used to describe either the normal wetness of the vagina or the abnormal wetness that may come from an infection in the penis or vagina. Duct – Tube, the fallopian tubes may be called oviducts, because they are the path for an ovum. -

Rectum & Anal Canal
Rectum & Anal canal Dr Brijendra Singh Prof & Head Anatomy AIIMS Rishikesh 27/04/2019 EMBRYOLOGICAL basis – Nerve Supply of GUT •Origin: Foregut (endoderm) •Nerve supply: (Autonomic): Sympathetic Greater Splanchnic T5-T9 + Vagus – Coeliac trunk T12 •Origin: Midgut (endoderm) •Nerve supply: (Autonomic): Sympathetic Lesser Splanchnic T10 T11 + Vagus – Sup Mesenteric artery L1 •Origin: Hindgut (endoderm) •Nerve supply: (Autonomic): Sympathetic Least Splanchnic T12 L1 + Hypogastric S2S3S4 – Inferior Mesenteric Artery L3 •Origin :lower 1/3 of anal canal – ectoderm •Nerve Supply: Somatic (inferior rectal Nerves) Rectum •Straight – quadrupeds •Curved anteriorly – puborectalis levator ani •Part of large intestine – continuation of sigmoid colon , but lacks Mesentery , taeniae coli , sacculations & haustrations & appendices epiploicae. •Starts – S3 anorectal junction – ant to tip of coccyx – apex of prostate •12 cms – 5 inches - transverse slit •Ampulla – lower part Development •Mucosa above Houstons 3rd valve endoderm pre allantoic part of hind gut. •Mucosa below Houstons 3rd valve upto anal valves – endoderm from dorsal part of endodermal cloaca. •Musculature of rectum is derived from splanchnic mesoderm surrounding cloaca. •Proctodeum the surface ectoderm – muco- cutaneous junction. •Anal membrane disappears – and rectum communicates outside through anal canal. Location & peritoneal relations of Rectum S3 1 inch infront of coccyx Rectum • Beginning: continuation of sigmoid colon at S3. • Termination: continues as anal canal, • one inch below -
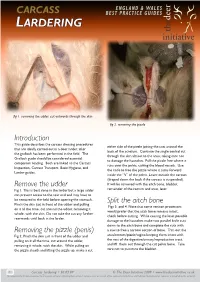
Introduction Remove the Udder Removing the Pizzle (Penis)
fig . removing the udder, cut outwards through the skin fig 2. removing the pizzle Introduction This guide describes the carcass dressing procedures either side of the pizzle joining the cuts around the that are ideally carried out in a deer larder, after back of the scrotum. Continue the single central cut the gralloch has been performed in the field. The through the skin almost to the anus, taking care not Gralloch guide should be considered essential to damage the haunches. Pull the pizzle free where it companion reading. Both are linked to the Carcass runs over the pelvis, cutting the blood vessels. Use Inspection, Carcass Transport, Basic Hygiene, and the knife to free the pizzle where it turns forward Larder guides. inside the “V” of the pelvis. Leave outside the carcass (draped down the back if the carcass is suspended). Remove the udder It will be removed with the aitch bone, bladder, Fig 1. This is best done in the larder but a large udder remainder of the rectum and anus, later. can prevent access to the rear end and may have to be removed in the field before opening the stomach. Split the aitch bone Pinch the skin just in front of the udder and pulling Figs 3. and 4. Note that some venison processors on it all the time, cut around the udder, removing it would prefer that the aitch bone remains intact, whole, with the skin. Do not take the cut any further check before cutting. While causing the least possible rearwards until back in the larder. -

Venous and Lymphatic Vessels. ANATOM.UA PART 1
Lection: Venous and lymphatic vessels. ANATOM.UA PART 1 https://fipat.library.dal.ca/ta2/ Ch. 1 Anatomia generalis PART 2 – SYSTEMATA MUSCULOSKELETALIA Ch. 2 Ossa Ch. 3 Juncturae Ch. 4 Musculi PART 3 – SYSTEMATA VISCERALIA Ch. 5 Systema digestorium Ch. 6 Systema respiratorium Ch. 7 Cavitas thoracis Ch. 8 Systema urinarium Ch. 9 Systemata genitalia Ch. 10 Cavitas abdominopelvica PART 4 – SYSTEMATA INTEGRANTIA I Ch. 11 Glandulae endocrinae Ch. 12 Systema cardiovasculare Ch. 13 Organa lymphoidea PART 5 – SYSTEMATA INTEGRANTIA II Ch. 14 Systema nervosum Ch. 15 Organa sensuum Ch. 16 Integumentum commune ANATOM.UA ANATOM.UA Cardiovascular system (systema cardiovasculare) consists of the heart and the tubes, that are used for transporting the liquid with special functions – the blood or lymph, that are necessary for supplying the cells with nutritional substances and the oxygen. ANATOM.UA 5 Veins Veins are blood vessels that bring blood back to theheart. All veins carry deoxygenatedblood with the exception of thepulmonary veins and umbilical veins There are two types of veins: Superficial veins: close to the surface of thebody NO corresponding arteries Deep veins: found deeper in the body With corresponding arteries Veins of the systemiccirculation: Superior and inferior vena cava with their tributaries Veins of the portal circulation: Portal vein ANATOM.UA Superior Vena Cava Formed by the union of the right and left Brachiocephalic veins. Brachiocephalic veins are formed by the union of internal jugular and subclavianveins. Drains venous blood from: Head &neck Thoracic wall Upper limbs It Passes downward and enter the rightatrium. Receives azygos vein on the posterior aspect just before it enters theheart. -

Plantar Fascia-Specific Stretching Program for Plantar Fasciitis
Plantar Fascia-Specific Stretching Program For Plantar Fasciitis Plantar Fascia Stretching Exercise 1. Cross your affected leg over your other leg. 2. Using the hand on your affected side, take hold of your affected foot and pull your toes back towards shin. This creates tension/stretch in the arch of the foot/plantar fascia. 3. Check for the appropriate stretch position by gently rubbing the thumb of your unaffected side left to right over the arch of the affected foot. The plantar fascia should feel firm, like a guitar string. 4. Hold the stretch for a count of 10. A set is 10 repetitions. 5. Perform at least 3 sets of stretches per day. You cannot perform the stretch too often. The most important times to stretch are before taking the first step in the morning and before standing after a period of prolonged sitting. Plantar Fascia Stretching Exercise 1 2 3 4 URMC Orthopaedics º 4901 Lac de Ville Boulevard º Building D º Rochester, NY 14618 º 585-275-5321 www.ortho.urmc.edu Over, Please Anti-inflammatory Medicine Anti-inflammatory medicine will help decrease the inflammation in the arch and heel of your foot. These include: Advil®, Motrin®, Ibuprofen, and Aleve®. 1. Use the medication as directed on the package. If you tolerate it well, take it daily for 2 weeks then discontinue for 1 week. If symptoms worsen or return, then resume medicine for 2 weeks, then stop. 2. You should eat when taking these medications, as they can be hard on your stomach. Arch Support 1. -

Pelvic Anatomyanatomy
PelvicPelvic AnatomyAnatomy RobertRobert E.E. Gutman,Gutman, MDMD ObjectivesObjectives UnderstandUnderstand pelvicpelvic anatomyanatomy Organs and structures of the female pelvis Vascular Supply Neurologic supply Pelvic and retroperitoneal contents and spaces Bony structures Connective tissue (fascia, ligaments) Pelvic floor and abdominal musculature DescribeDescribe functionalfunctional anatomyanatomy andand relevantrelevant pathophysiologypathophysiology Pelvic support Urinary continence Fecal continence AbdominalAbdominal WallWall RectusRectus FasciaFascia LayersLayers WhatWhat areare thethe layerslayers ofof thethe rectusrectus fasciafascia AboveAbove thethe arcuatearcuate line?line? BelowBelow thethe arcuatearcuate line?line? MedianMedial umbilicalumbilical fold Lateralligaments umbilical & folds folds BonyBony AnatomyAnatomy andand LigamentsLigaments BonyBony PelvisPelvis TheThe bonybony pelvispelvis isis comprisedcomprised ofof 22 innominateinnominate bones,bones, thethe sacrum,sacrum, andand thethe coccyx.coccyx. WhatWhat 33 piecespieces fusefuse toto makemake thethe InnominateInnominate bone?bone? PubisPubis IschiumIschium IliumIlium ClinicalClinical PelvimetryPelvimetry WhichWhich measurementsmeasurements thatthat cancan bebe mademade onon exam?exam? InletInlet DiagonalDiagonal ConjugateConjugate MidplaneMidplane InterspinousInterspinous diameterdiameter OutletOutlet TransverseTransverse diameterdiameter ((intertuberousintertuberous)) andand APAP diameterdiameter ((symphysissymphysis toto coccyx)coccyx) -

The Cyclist's Vulva
The Cyclist’s Vulva Dr. Chimsom T. Oleka, MD FACOG Board Certified OBGYN Fellowship Trained Pediatric and Adolescent Gynecologist National Medical Network –USOPC Houston, TX DEPARTMENT NAME DISCLOSURES None [email protected] DEPARTMENT NAME PRONOUNS The use of “female” and “woman” in this talk, as well as in the highlighted studies refer to cis gender females with vulvas DEPARTMENT NAME GOALS To highlight an issue To discuss why this issue matters To inspire future research and exploration To normalize the conversation DEPARTMENT NAME The consensus is that when you first start cycling on your good‐as‐new, unbruised foof, it is going to hurt. After a “breaking‐in” period, the pain‐to‐numbness ratio becomes favourable. As long as you protect against infection, wear padded shorts with a generous layer of chamois cream, no underwear and make regular offerings to the ingrown hair goddess, things are manageable. This is wrong. Hannah Dines British T2 trike rider who competed at the 2016 Summer Paralympics DEPARTMENT NAME MY INTRODUCTION TO CYCLING Childhood Adolescence Adult Life DEPARTMENT NAME THE CYCLIST’S VULVA The Issue Vulva Anatomy Vulva Trauma Prevention DEPARTMENT NAME CYCLING HAS POSITIVE BENEFITS Popular Means of Exercise Has gained popularity among Ideal nonimpact women in the past aerobic exercise decade Increases Lowers all cause cardiorespiratory mortality risks fitness DEPARTMENT NAME Hermans TJN, Wijn RPWF, Winkens B, et al. Urogenital and Sexual complaints in female club cyclists‐a cross‐sectional study. J Sex Med 2016 CYCLING ALSO PREDISPOSES TO VULVAR TRAUMA • Significant decreases in pudendal nerve sensory function in women cyclists • Similar to men, women cyclists suffer from compression injuries that compromise normal function of the main neurovascular bundle of the vulva • Buller et al. -
Female Perineum Doctors Notes Notes/Extra Explanation Please View Our Editing File Before Studying This Lecture to Check for Any Changes
Color Code Important Female Perineum Doctors Notes Notes/Extra explanation Please view our Editing File before studying this lecture to check for any changes. Objectives At the end of the lecture, the student should be able to describe the: ✓ Boundaries of the perineum. ✓ Division of perineum into two triangles. ✓ Boundaries & Contents of anal & urogenital triangles. ✓ Lower part of Anal canal. ✓ Boundaries & contents of Ischiorectal fossa. ✓ Innervation, Blood supply and lymphatic drainage of perineum. Lecture Outline ‰ Introduction: • The trunk is divided into 4 main cavities: thoracic, abdominal, pelvic, and perineal. (see image 1) • The pelvis has an inlet and an outlet. (see image 2) The lowest part of the pelvic outlet is the perineum. • The perineum is separated from the pelvic cavity superiorly by the pelvic floor. • The pelvic floor or pelvic diaphragm is composed of muscle fibers of the levator ani, the coccygeus muscle, and associated connective tissue. (see image 3) We will talk about them more in the next lecture. Image (1) Image (2) Image (3) Note: this image is seen from ABOVE Perineum (In this lecture the boundaries and relations are important) o Perineum is the region of the body below the pelvic diaphragm (The outlet of the pelvis) o It is a diamond shaped area between the thighs. Boundaries: (these are the external or surface boundaries) Anteriorly Laterally Posteriorly Medial surfaces of Intergluteal folds Mons pubis the thighs or cleft Contents: 1. Lower ends of urethra, vagina & anal canal 2. External genitalia 3. Perineal body & Anococcygeal body Extra (we will now talk about these in the next slides) Perineum Extra explanation: The perineal body is an irregular Perineal body fibromuscular mass. -

Advanced Retroperitoneal Anatomy Andneuro-Anatomy of Thepelvis
APRIL 21-23 • 2016 • ST. LOUIS, MISSOURI, USA Advanced Retroperitoneal Anatomy and Neuro-Anatomy of the Pelvis Hands-on Cadaver Workshop with Focus on Complication Prevention in Minimally Invasive Surgery in Endometriosis, Urogynecology and Oncology WITH ICAPS FACULTY Nucelio Lemos, MD, PhD (Course Chair) Adrian Balica, MD (Course Co-Chair) Eugen Campian, MD, PhD Vadim Morozov, MD Jonathon Solnik, MD, FACOG, FACS An offering through: Practical Anatomy & Surgical Education Department of Surgery, Saint Louis University School of Medicine http://pa.slu.edu COURSE DESCRIPTION • Demonstrate the topographic anatomy of the pelvic sidewall, CREDIT DESIGNATION: This theoretical and cadaveric course is designed for both including vasculature and their relation to the ureter, autonomic Saint Louis University designates this live activity for a maximum intermediate and advanced laparoscopic gynecologic surgeons and somatic nerves and intraperitoneal structures; of 20.5 AMA PRA Category 1 Credit(s) ™. and urogynecologists who want to practice and improve their • Discuss steps of safe laparoscopic dissection of the pelvic ureter; laparoscopic skills and knowledge of retroperitoneal anatomy. • Distinguish and apply steps of safe and effective pelvic nerve Physicians should only claim credit commensurate with the The course will be composed of 3 full days of combined dissection and learn the landmarks for nerve-sparing surgery. extent of their participation in the activity. theoretical lectures on Surgical Anatomy and Pelvic Neuroanatomy with hands on practice of laparoscopic and ACCREDITATION: REGISTRATION / TUITION FEES transvaginal dissection. Saint Louis University School of Medicine is accredited by the Accreditation Council for Continuing Medical Education (ACCME) Early Bird (up to Dec. 31st) ...........US ....$2,295 COURSE OBJECTIVES to provide continuing medical education for physicians. -

Clinical Anatomy of the Anterior Abdominal Wall in Its Relation To
ClinicalClinical AnatomyAnatomy ofof thethe AnteriorAnterior AbdominalAbdominal WallWall inin itsits RelationRelation toto HerniaHernia Handout download: http://www.oucom.ohiou.edu/dbms-witmer/gs-rpac.htm 24 April 2007 LawrenceLawrence M.M. Witmer,Witmer, PhDPhD Professor of Anatomy Department of Biomedical Sciences College of Osteopathic Medicine Ohio University Athens, Ohio 45701 [email protected] AnatomicalAnatomical OverviewOverview External Internal Transversus Rectus oblique oblique abdominis abdominis fleshyfleshy rectusrectus portionportion sheathsheath aponeuroticaponeurotic inguinalinguinal tendinoustendinous portionportion ligamentligament intersectionsintersections • Three flat abdominals: attach to trunk skeleton, inguinal lig., linea alba, etc.; fleshy laterally and aponeurotic medially, forming rectus sheath medially • Two vertical abdominals: rectus abdominis and pyramidalis (not shown) Moore & Dalley 2006 AnatomicalAnatomical OverviewOverview intramuscular exchange of intermuscular exchange of contralateral external oblique fibers contralateral external & internal oblique right external oblique left internal oblique • continuity of external oblique • continuity of fibers across midline fibers across midline • “digastric” muscle with central • blending of superficial & deep tendon fibers on opposite side • torsion of trunk Moore & Dalley 2006 AnatomicalAnatomical OverviewOverview transv. abd. linea alba rectus sheath rectus abdominis int. obl. ext. obl. semilunar line peritoneum transversalis fascia aponeuroses of abdominal -

By Dr.Ahmed Salman Assistant Professorofanatomy &Embryology My Advice to You Is to Focus on the Diagrams That I Drew
The University Of Jordan Faculty Of Medicine REPRODUCTIVE SYSTEM By Dr.Ahmed Salman Assistant ProfessorofAnatomy &embryology My advice to you is to focus on the diagrams that I drew. These diagrams cover the Edited by Dana Hamo doctor’s ENTIRE EXPLANATION AND WHAT HE HAS MENTIONED Quick Recall : Pelvic brim Pelvic diaphragm that separates the true pelvis above and perineum BELOW Perineum It is the diamond-shaped lower end of the trunk Glossary : peri : around, ineo - discharge, evacuate Location : it lies below the pelvic diaphragm, between the upper parts of the thighs. Boundaries : Anteriorly : Inferior margin of symphysis pubis. Posteriorly : Tip of coccyx. Anterolateral : Fused rami of pubis and ischium and ischial tuberosity. Posterolateral : Sacrotuberous ligaments. Dr.Ahmed Salman • Same boundaries as the pelvic Anteriorly: outlet. inferior part of • If we drew a line between the 2 symphysis pubis ischial tuberosities, the diamond shape will be divided into 2 triangles. Anterior and Anterior and Lateral : Lateral : •The ANTERIOR triangle is called ischiopubic ischiopubic urogenital triangle ramus The perineum ramus •The POSTERIOR triangle is called has a diamond anal triangle shape. ischial tuberosity Posterior and Posterior and Lateral : Lateral : Urogenital sacrotuberous sacrotuberous tri. ligament ligament Anal tri. Posteriorly : tip of coccyx UROGENITAL TRI. ANAL TRI. Divisions of the Perineum : By a line joining the anterior parts of the ischial tuberosities, the perineum is divided into two triangles : Anteriorly :Urogenital -

Trans-Obturator Cable Fixation of Open Book Pelvic Injuries
www.nature.com/scientificreports OPEN Trans‑obturator cable fxation of open book pelvic injuries Martin C. Jordan 1*, Veronika Jäckle1, Sebastian Scheidt2, Fabian Gilbert3, Stefanie Hölscher‑Doht1, Süleyman Ergün4, Rainer H. Mefert1 & Timo M. Heintel1 Operative treatment of ruptured pubic symphysis by plating is often accompanied by complications. Trans‑obturator cable fxation might be a more reliable technique; however, have not yet been tested for stabilization of ruptured pubic symphysis. This study compares symphyseal trans‑obturator cable fxation versus plating through biomechanical testing and evaluates safety in a cadaver experiment. APC type II injuries were generated in synthetic pelvic models and subsequently separated into three diferent groups. The anterior pelvic ring was fxed using a four‑hole steel plate in Group A, a stainless steel cable in Group B, and a titan band in Group C. Biomechanical testing was conducted by a single‑ leg‑stance model using a material testing machine under physiological load levels. A cadaver study was carried out to analyze the trans‑obturator surgical approach. Peak‑to‑peak displacement, total displacement, plastic deformation and stifness revealed a tendency for higher stability for trans‑ obturator cable/band fxation but no statistical diference to plating was detected. The cadaver study revealed a safe zone for cable passage with sufcient distance to the obturator canal. Trans‑ obturator cable fxation has the potential to become an alternative for symphyseal fxation with less complications. Disruption of the pubic symphysis is commonly seen in pelvic ring injuries of trauma patients 1,2. Te disrup- tion of the anterior pelvic ring might occur in combination with a posterior pelvic ring impairment of variable severity.