Ankle Sprain Information
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Physio Med Self Help for Achilles Tendinopathy
Physio Med Self Help 0113 229 1300 for Achilles Tendinopathy Achilles tendon injuries are common, often evident in middle aged runners to non-sporting individuals. They are often characterised by pain in the tendon, usually at the beginning and end of exercise, pain and stiffness first thing in the morning or after sitting for long periods. There is much that can be done to both speed up the healing and prevent re-occurrence. Anatomy of the Area The muscles of your calf (the gastrocnemius and soleus) are the muscles which create the force needed to push your foot off the floor when walking, running and jumping, or stand up on your toes. The Achilles tendon is the fibrous band that connects these muscles to your heel. You may recognise the term ‘Achilles Tendonitis’ which was the previous name used for Achilles Tendinopathy. However the name has changed as it is no longer thought to be a totally inflammatory condition, but rather an overuse injury causing pain, some localised inflammation and degeneration of the thick Achilles tendon at the back of the ankle. Potential causes of Achilles Tendinopathy and advice on how to prevent it • Poor footwear or sudden change in training surface e.g. sand makes the calf work harder » Wear suitable shoes for the activity (type, fit and condition of footwear). » Take account of the surface you are exercising on and if soft and unstructured like sand or loose soil reduce the intensity / duration or take a short break or reduce any load you are carrying into smaller loads until you become conditioned to it. -

An Evidence Based Medicine Understanding of Meniscus Injuries and How to Treat Them
An Evidence Based Medicine Understanding of Meniscus Injuries and How to Treat Them Patrick S. Buckley, MD University Orthopaedic Associates June 1, 2019 Disclosures • None www.UOANJ.com Anatomy of the Meniscus • Act as functional extensions of the tibial plateaus to increase depth of tibial articular surface • The meniscotibial attachment contributes to knee stability • Triangular in cross-section Gross Anatomy of the Meniscus • Ultrastructural Anatomy – Primarily Type I collagen (90%) – 70% water – Fiber orientation is circumferential (hoop stressing) Meniscal Vascularity • Relatively avascular • Vascular penetration – 10 - 30% medial – 10 - 25% lateral • Non-vascularized portions gain nutrients from mechanical loading and joint motion Medial Meniscus • Semilunar shape • Thin anterior horn • Broader posterior horn • More stable & less motion than the lateral = tears more often Lateral Meniscus • Almost circular in shape • Intimately associated with the ACL tibial insertion • Posterior horn attachments – Ligament of Humphrey – Ligament of Wrisberg • Lateral meniscus is a more dynamic structure with more motion Main Importance of Menisci • Load transmission • Joint stability Load Bearing / Shock Absorption • MM 50% and 70% LM of load transmitted through mensicus in extension • 85 % at 90° of flexion • Meniscectomy – 50 % decrease in contact area – 20 % less shock absorption www.UOANJ.com Meniscal effect on joint stability • Secondary restraints to anterior tibial translation in normal knees • In an ACL-deficient knee: the posterior horn of the medial meniscus is more important than the lateral meniscus Interaction of ACL and PHMM • Lack of MM in ACLD knees significantly ↑ anterior tibial translation at all knee flexion angles • Think about with high grade pivot! (Levy, JBJS,1982) (Allen, JOR,2000) C9ristiani, AJSM, 2017) Meniscus Function -Now known to be important structure for load distribution and secondary stabilizer to the knee. -

Ministry of Health of Ukraine Ukrainian Medical Dental Academy
Ministry of Health of Ukraine Ukrainian Medical Dental Academy Methodical instructions for independent work for students during training to practical (seminar) classes and in class Academic discipline Surgical dentistry Module № 5 Lesson topic № 1 Anatomy of the temporomandibular joint (TMJ). Modern methods of diagnosing TMJ diseases. Arthroscopy, its possibilities in the diagnosis and treatment of TMJ diseases. Dislocations of the mandible: etiology, clinic, diagnosis, treatment. Curation of the patient in the clinic of maxillofacial surgery. Writing an academic medical history. Course V Faculty Stomatological Poltava 2020 1. Relevance of the topic. Knowledge of the anatomical structure of the temporomandibular joint (TMJ) and the characteristics of modern diagnostic methods for assessing their pathologies. The etiology, clinical diagnosis and treatment of mandibular dislocations allows you to choose a timely and effective way to treat this pathology, avoid mistakes and complications, allows the dentist to diagnose TMJ and prescribe optimal treatment. Academic history in which the student is able to use knowledge , obtained in the study of basic and applied sciences, obtained demonstrate practical skills. 2. Specific target: 2 .1.Analyze to know statistics, diseases TMJ.; 2.2. Explain the methods of diagnosing diseases TMJ; 2.3. To offer to examine patients with diseases of TMJ; 2.4. Classify diseases TMJ; 2.5. Interpret theoretical and clinical studies of diseases TMJ; 2.6. Draw diagrams, graphs 2.7. Analyze the treatment plan for patients with diseases TMJ; 2.8. Make a plan for the treatment of patients with diseases TMJ; 3. Basic knowledge, skills, abilities necessary for studying the topic (interdisciplinary integration). Names of previous Acquired skills disciplines Anatomy To study the anatomical and topographic structure of the temporomandibular joint. -

ANKLE LIGAMENT STRAIN DURING SUPINATION SPRAIN INJURY – a Alt, W., Lohrer, H., & Gollhofer, A
Vilas-Boas, Machado, Kim, Veloso (eds.) Portuguese Journal of Sport Sciences Biomechanics in Sports 29 11 (Suppl. 2), 2011 REFERENCES: ANKLE LIGAMENT STRAIN DURING SUPINATION SPRAIN INJURY – A Alt, W., Lohrer, H., & Gollhofer, A. (1999). FunctionalProperties of Adhesive Ankle Taping: COMPUTATIONAL BIOMECHANICS STUDY Neuromuscular and Mechanical Effects Before and After Exercise. Foot & Ankle International , 20(4), 238-45. Daniel Tik-Pui Fong1,2, Feng Wei3, Youlian Hong4,5, Tron Krosshaug6, Benesch, S., Putz, W., Rosenbaum, D., & Becker, H.-P. (2000). Reliability of Peroneal Reaction Time Roger C. Haut3 and Kai-Ming Chan1,2 Measurements. Clin Biomech , 15. Cordova, M. L., Bernard, L. W., Au, K. K., Demchak, T. J., Stone, M. B., & Sefton, J. M. (2010). Department of Orthopaedics and Traumatology, Prince of Wales Hospital, Cryotherapy and ankle bracing effects on peroneus longus response during sudden inversion. J 1 Electromyogr Kinesiol , 20, 248-53. Faculty of Medicine, The Chinese University of Hong Kong, Hong Kong, China The Hong Kong Jockey Club Sports Medicine and Health Sciences Centre, Delahunt, E. (2007). Peroneal reflex contribution to the development of functional instability of the 2 ankle joint. Phys Ther Sport , 8, 98-104. Faculty of Medicine, The Chinese University of Hong Kong, Hong Kong, China 3 Docherty, C. L., & Arnold, B. L. (2008). Force sence deficits in functionally unstable ankles. J Orthop Orthopaedic Biomechanics Laboratories, Michigan State University, USA Res , 26(11), 1489-93. Department of Sports Science and Physical Education, Faculty of Education, 4 Eechaute, C., Vaes, P., Duquet, W., & Gheluwe, B. v. (2009). Reliability ans discriminative validity of The Chinese University of Hong Kong, Hong Kong, China sudden ankle inversion measurements in patients with chronic ankle instability. -
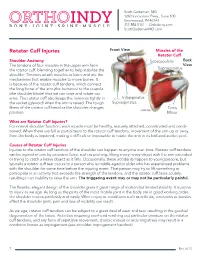
Rotator Cuff Injuries
Scott Gudeman, MD 1260 Innovation Pkwy., Suite 100 Greenwood, IN 46143 317.884.5161 OrthoIndy.com ScottGudemanMD.com Rotator Cuff Injuries Front View Muscles of the Rotator Cuff Shoulder Anatomy Subscapularis Back The tendons of four muscles in the upper arm form View Supraspinatus the rotator cuff, blending together to help stabilize the shoulder. Tendons attach muscles to bone and are the mechanisms that enable muscles to move bones. It is because of the rotator cuff tendons, which connect the long bone of the arm (the humerus) to the scapula (the shoulder blade) that we can raise and rotate our arms. The rotator cuff also keeps the humerus tightly in Infraspinatus the socket (glenoid) when the arm is raised. The tough Supraspinatus fibers of the rotator cuff bend as the shoulder changes Teres position. Minor What are Rotator Cuff Injuries? For normal shoulder function, each muscle must be healthy, securely attached, coordinated and condi- tioned. When there are full or partial tears to the rotator cuff tendons, movement of the arm up or away from the body is impaired, making it difficult or impossible to rotate the arm in its ball-and-socket joint. Causes of Rotator Cuff Injuries Injuries to the rotator cuff tendons of the shoulder can happen to anyone over time. Rotator cuff tendons can be injured or torn by excessive force, such as pitching, lifting a very heavy object with the arm extended or trying to catch a heavy object as it falls. Occasionally, these accidents happen to young people, but typically a rotator cuff tear occurs to a person who is middle-aged or older who has experienced problems with the shoulder for some time before the injuring event. -

Common Elbow Injuries Symptoms
During the summer months, many people stay active by playing golf or tennis. These sports, however, carry a risk of injury to the tendons – bands of tissue that connect muscles to bones – in the elbow. This month’s AT Corner will explain how these injuries happen, how to treat them if they occur and, most importantly, how to prevent them. Common Elbow Injuries Tendonitis: Inflammation, pain and difficulty using the joint caused by repetitive activities and/or sudden trauma. Tendonosis: A degeneration (breakdown) or tear of tendons which occurs as a result of aging. Symptoms of tendonosis usually last more than a few weeks. Note: Your risk of tendonitis and tendonosis increases with age. They also occur more frequently in those who routinely perform activities that require repetitive movement, as this places greater amounts of stress on the tendons. Tennis elbow: Also referred to as lateral epicondylitis, this condition occurs when there is an injury to the outer elbow tendon. Golfers’ elbow: Also referred to as medial epicondylitis, this condition occurs when there is an injury to the inner elbow tendon. Note: Injuries to these tendons can occur in other sports and activities that use the wrist and forearm muscles. Most times, the dominant arm is the one affected. Symptoms • Pain that spreads from the elbow into the upper arm or down the forearm • Forearm weakness • Pain that can begin suddenly or gradually worsen over time • Difficulty with activities that require arm strength Treatment Over-the-counter medications: NSAIDs, such as ibuprofen (Advil®, Motrin®) and naproxen (Aleve®), or acetaminophen (Tylenol®) can provide pain relief. -

I. BACKGROUND a Cervical Musculoligamentous Injury (Sprain/Strain)
CERVICAL MUSCULOLIGAMENTOUS INJURY (Sprain/Strain) I. BACKGROUND A cervical musculoligamentous injury (sprain/strain) may cause neck pain due to a partial stretching or tearing of the soft tissues (muscles, fascia, ligaments, tendons etc.). Non-specific upper extremity complaints such as stiffness, muscle fatigue, and paresthesias may also be reported. Although injury to the neck can result in fracture or neurologic impairment, by definition, a diagnosis of cervical sprain or strain excludes a fracture. The recovery period following a cervical musculoligamentous injury is of variable duration, but symptoms generally resolve within 6 weeks. II. DIAGNOSTIC CRITERIA A. Pertinent Historical and Physical Findings The onset of neck pain and paraspinal muscle spasm may begin either immediately after the injury occurs or can develop gradually over the next 24-48 hours. This pain is usually aggravated with motion of the neck and/or shoulder and is frequently reduced with rest. The pain usually does not radiate below the shoulder. It can be accompanied by paresthesias or a sense of weakness in the upper extremities related to muscle spasm in the neck. Headaches arising from the cervical region or occiput may accompany neck pain. Physical findings include tenderness to palpation and/or spasm of the paraspinal, trapezius, or anterior cervical (e.g. sternocleidomastoid) muscles, and painful and/or decreased active cervical range of motion. With isolated cervical sprain/strain, the objective neurological examination should be normal. B. Appropriate Diagnostic Tests and Examinations Indications for radiographs of the cervical spine include high velocity trauma, neurologic injury on clinical examination, history of cancer or osteoporosis, age > 65 years, etc. -

Mid-Back Strain
Comp. by: Kkala Stage: Revises2 Chapter No.: 186 Title Name: Safran Page Number: 0 Date:16/6/11 Time:20:52:23 B978-1-4160-5650-8.00286-7, 00286 Mid-Back Strain DESCRIPTION Chronic inflammation, scarring, and partial muscle– tendon tears may occur. A mid-back strain is an injury to the muscles and tendons Healing or resolution of symptoms may be delayed, of the middle back that attach to the ribs and chest wall particularly if activity is resumed too soon. and to the spine. These muscles stabilize the spine and Prolonged disability may result. allow its motion. The mid back provides a large portion of the back’s overall motion, but it primarily allows for rotation of the back in a twisting motion. GENERAL TREATMENT CONSIDERATIONS COMMON SIGNS AND SYMPTOMS Injury to the back results in pain and inflammation. The Pain in the back that may affect only one side and is pain and inflammation result in muscle spasms in the worse with movement back, which in turn result in more pain. Thus the initial Muscle spasms and often swelling in the back treatment consists of rest, medications, and ice to relieve Loss of strength of the back muscles pain, inflammation, and muscle spasms. As pain and Crepitation (a crackling sound) when the muscles are spasms subside, exercises to improve strength and flexi- touched bility and education in the use of proper back mechanics and sports technique are started. Referral to a physical CAUSES therapist or athletic trainer may be recommended for these and possibly other treatments, such as transcutane- Prolonged overuse of the muscle–tendon units in the ous electronic nerve stimulation (TENS) and ultrasound. -

ACHILLES TENDONITIS in GYMNASTICS by Holly Heitzman, MS, LAT, ATC, PTA
ACHILLES TENDONITIS IN GYMNASTICS By Holly Heitzman, MS, LAT, ATC, PTA endonitis is common in Tendocalcaneal Bursitis- A bursa is a fluid-filled gymnastics with multiple sac designed to limit friction. When a bursa sac becomes irritated and inflamed, it is called bursitis. repetitions of floor routines, Tendocalcaneal bursa is located under the fibrous beam routines and sprinting Achilles tendon and behind the heel bone (calcaneus). toward the vault. The calf Achilles tendon rupture – In severe cases, a force Tmuscles and the Achilles tendons are may even rupture the tendon. The rupture may be constantly being worked and stressed. preceded by periods of chronic tendonitis. Multiple The Achilles tendon provides power episodes of tendonitis may weaken the tendon and its fiber structure. Many athletes report that a rupture when pushing off the foot. A strain can feels like someone kicked them in the leg. They no cause injury to the calf muscles or the longer have the ability to walk or push off. Surgery Achilles tendon. This can happen during is the common course of treatment for an Achilles rupture. a strong contraction of the muscle, as when sprinting toward the vault or when Sever’s disease – At the site at which the Achilles doing a tumbling pass, the foot may be tendon attaches to the heel, it becomes inflamed and the bone starts to deteriorate. Sever’s disease forced upward upon transition of landing may be associated with a growth spurt. As the bones to jumping. The strain may affect different get longer, the tendon becomes tighter; therefore, portions of the tendon. -

Ankle Sprains & Strains and Fractures
Sprains, strains and fractures pe o c S t Common causes of simple ankle injuries usually involve sports, biomechanical instability or trauma. Strains o A strain is usually attributable to overuse and repetitive damage to the muscle or tendon and are common in athletes and elderly patients — groups at high risk for wear and tear injuries. A patient suffering from a mild strain will complain of the ankle feeling sore and weak, and inflammation of the joint may be apparent. For a o severe strain, the patient will complain of significant pain and difficulty walking on the injured foot. This may indicate a full or partial tear of the muscle or tendon. Sprains F A sprain is a partial dislocation of the ankle joint with tearing of the ankle ligaments. Most sprains affect the ligaments on the lateral side of the ankle caused by sudden inversion of the ankle below the tibia, causing the lateral ligaments to stretch or tear. Sprains can occur in the opposite direction, with aversion injuries affecting the deltoid ligament, although this is less common and is usually minor. Severity of injury is graded based on the number of ligaments involved and the degree of damage. Grade 1 sprains: the patient will still be able to walk with minor discomfort and there will be no tearing of the ligaments. Grade 2 sprains: there will be partial tearing of the ligaments, the patient will find it painful to put weight on the affected foot, and the ankle will be inflamed with bruising. Grade 3 sprains: the patient may have heard an audible pop at the time of injury, indicating that ligaments will be completely torn. -

Acute and Chronic Whiplash Disorders – a Review
J Rehabil Med 2004; 36: 193–210 REVIEW ARTICLE ACUTE AND CHRONIC WHIPLASH DISORDERS – A REVIEW Ylva Sterner1 and Bjo¨rn Gerdle2,3 From the 1Department of Anaesthesia, Pain Clinic, Karolinska Institutet, Danderyd Hospital, 2Department of Rehabilitation Medicine, Faculty of Health Sciences, Linko¨ping and 3Pain and Rehabilitation Centre, University Hospital, Linko¨ping, Sweden Objective: This review examines acute and chronic whiplash- guidelines concerning WAD are sparse due to lack of random- associated disorders to facilitate assessment, treatment and ized, controlled and prospective studies. Assessment, investi- rehabilitation for further research and evidence-based gation and treatment strategies for WAD should be based on practises. science and experience-based practise, remembering that Design: A review of the literature. statistical results generally are on a group level and cannot be Results and conclusion: Whiplash-associated disorders correlated directly to individuals. account for a large proportion of the overall impairment During the First World War, it became clear that the violence and disability caused by traffic injuries. Rarely can a definite inflicted on the cervical spine of pilots during emergency ejec- injury be determined in the acute (or chronic) phase. Crash- tion was great enough to cause a blackout for several seconds related factors have been identified, and several trauma and accidents occurred that were due to a whiplash effect. This mechanisms possibly causing different injuries have been understanding resulted in the development of a headrest and a described. Most whiplash trauma will not cause injury, and shoulder harness to protect pilots. Although a great deal of the majority of patients (92–95%) will return to work. -

Sprains, Strains, Tendonitis, Bursitis
Physical and Sports Therapy Sprains, Strains, Tendonitis, Bursitis Over a lifetime, the average person will encounter a number of common ailments, such as sprains, strains, tendonitis, and bursitis. These issues cause local pain, such as elbow pain with Tennis Elbow or Golfer’s Elbow, limited function such as walking restrictions due to Achilles Tendonitis or Plantar Fasciitis, or difficulty sleeping such as is experienced with Hip Bursitis. In most cases, such conditions are easily controlled and eradicated with appropriate care. Unfortunately, left untreated, these relatively simple conditions sometimes become severe and greatly impact function. Some common musculoskeletal issues include: Sprain: The overstretching of a ligament beyond the allowed length of the ligament, causing pain, swelling, and limited movement. Strain: Trauma caused to soft tissue, such as muscle, due to overstretching Tendonitis: Inflammation of a tendon, commonly due to overuse and commonly present at the elbow, shoulder, or knee Bursitis: Inflammation of a bursa, a fluid-filled sack in place to protect joints. They often become inflamed and irritated, commonly occurring at the shoulder and hip. What can physical therapy do for Sprains/Strains/Tendonitis/Bursitis? Physical Therapists are the experts in the medical field at the treatment of musculoskeletal conditions. Often times, only a single visit is necessary to instruct in proper home care of the condition. Treatments for Sprains/Strains/Tendonitis/Bursitis: Exercise: Used to strengthen, stretch, and stabilize. The primary tool used against musculoskeletal injuries. Manual Therapy: Hands-on therapy is valuable for treating local musculoskeletal issues, particularly cross-friction massage. Modalities: Several additional tools are helpful such as heat, cold, electrical stimulation, ultrasound, iontophoresis and the like.