Bone Quality + Bone Density = Bone Strength
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

An Update on Dual-Energy X-Ray Absorptiometry Glen M
An Update on Dual-Energy X-Ray Absorptiometry Glen M. Blake, PhD, and Ignac Fogelman, MD Dual-energy x-ray absorptiometry (DXA) scans to measure bone mineral density at the spine and hip have an important role in the evaluation of individuals at risk of osteoporosis, and in helping clinicians advise patients about the appropriate use of antifracture treat- ment. Compared with alternative bone densitometry techniques, hip and spine DXA exam- inations have several advantages that include a consensus that bone mineral density results should be interpreted using the World Health Organization T score definition of osteoporosis, a proven ability to predict fracture risk, proven effectiveness at targeting antifracture therapies, and the ability to monitor response to treatment. This review dis- cusses the evidence for these and other clinical aspects of DXA scanning. Particular attention is directed at the new World Health Organization Fracture Risk Assessment Tool (FRAX) algorithm, which uses clinical risk factors in addition to a hip DXA scan to predict a patient’s 10-year probability of suffering an osteoporotic fracture. We also discuss the recently published clinical guidelines that incorporate the FRAX fracture risk assessment in decisions about patient treatment. Semin Nucl Med 40:62-73 © 2010 Elsevier Inc. All rights reserved. steoporosis is widely recognized as an important public porosis before fractures occur and the development of effec- Ohealth problem because of the significant morbidity, tive treatments. Measurements of bone mineral -

Helping Physicians Succeed with ICD-10-CM January 24, 2014
Helping Physicians Succeed with ICD-10-CM January 24, 2014 Paul Belton, Vice President Corporate Compliance Agenda • Executive Summary • Clinical Roots of ICD-10 • Why physicians should care • How ICD-10 will benefit physicians • Taking control of ICD-10 • Personal Learning Experiences and Goals • ICD-10 Resources 2 Last Call for ICD-9-CM October 1, 2013 could be a day sentimental HIM Veterans raise a glass to a longtime friend – or perhaps foe. For October 1 signifies the end of an era; it is the effective date of the final ICD-9-CM update before ICD-10-CM/PCS codes kick in on October 1, 2014. TOP MOVIES THE AVERAGE INCLUDED: COST OF A SUPERMAN THE NEW HOUSE MOVIE, THE DEER WAS $58,000 HUNTER, THE MUPPET MOVIE, ROCKY II “For those of us who have THE AVERAGE INCOME WAS MARGARET THATCHER WS been maintaining ICD-9-CM $17,500 ELECTED PRIM MINISTER IN since the code set’s THE UK implementation in 1979, this THE BOARD GAM TRIVIIAL THE SONY PURSUIT WAS LAUNCHED WALKMAN final ICD-9-CM code update is DEBUTED, VISICALC BECAME In 1979: RETAILING a historic occasion.” ICD-9-CM THE FIRST FOR $200 has one more year’s worth of SPREADSHEET PROGRAM POPULAR SONGS last calls, with coders using INCLUDED: “MY AVERAGE SHARONA” BY THE MONTHLY this latest and last code set KNACK; “HOT STUFF” AND A GALLON RENT WAS “BAD GIRLS BY GLORIA OF GAS $280 update until next October. A GAYNOR; PINK FLOYD WAS 86 RELEASED “THE WALL” CENTS reflective toast to ICD-9-CM. -
PE2812 Breaking Arm Bones a Second Time
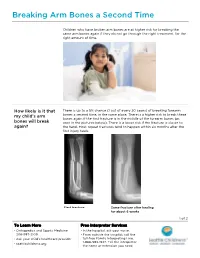
Breaking Arm Bones a Second Time Children who have broken arm bones are at higher risk for breaking the same arm bones again if they do not go through the right treatment, for the right amount of time. How likely is it that There is up to a 5% chance (1 out of every 20 cases) of breaking forearm my child’s arm bones a second time, in the same place. There is a higher risk to break these bones again if the first fracture is in the middle of the forearm bones (as bones will break seen in the pictures below). There is a lower risk if the fracture is closer to again? the hand. Most repeat fractures tend to happen within six months after the first injury heals. First fracture Same fracture after healing for about 6 weeks 1 of 2 To Learn More Free Interpreter Services • Orthopedics and Sports Medicine • In the hospital, ask your nurse. 206-987-2109 • From outside the hospital, call the • Ask your child’s healthcare provider toll-free Family Interpreting Line, 1-866-583-1527. Tell the interpreter • seattlechildrens.org the name or extension you need. Breaking Arm Bones a Second Time How can I help my Wearing a cast for at least six weeks lowers the risk of breaking the same child lower the risk arm bones again. After wearing a cast, we recommend your child wear a brace for 4 weeks in order to protect the injured area and start improving of having a wrist movement. While your child wears a brace, we recommend they do repeated bone not participate in contact sports (e.g., soccer, football or dodge ball). -

Study Guide Medical Terminology by Thea Liza Batan About the Author
Study Guide Medical Terminology By Thea Liza Batan About the Author Thea Liza Batan earned a Master of Science in Nursing Administration in 2007 from Xavier University in Cincinnati, Ohio. She has worked as a staff nurse, nurse instructor, and level department head. She currently works as a simulation coordinator and a free- lance writer specializing in nursing and healthcare. All terms mentioned in this text that are known to be trademarks or service marks have been appropriately capitalized. Use of a term in this text shouldn’t be regarded as affecting the validity of any trademark or service mark. Copyright © 2017 by Penn Foster, Inc. All rights reserved. No part of the material protected by this copyright may be reproduced or utilized in any form or by any means, electronic or mechanical, including photocopying, recording, or by any information storage and retrieval system, without permission in writing from the copyright owner. Requests for permission to make copies of any part of the work should be mailed to Copyright Permissions, Penn Foster, 925 Oak Street, Scranton, Pennsylvania 18515. Printed in the United States of America CONTENTS INSTRUCTIONS 1 READING ASSIGNMENTS 3 LESSON 1: THE FUNDAMENTALS OF MEDICAL TERMINOLOGY 5 LESSON 2: DIAGNOSIS, INTERVENTION, AND HUMAN BODY TERMS 28 LESSON 3: MUSCULOSKELETAL, CIRCULATORY, AND RESPIRATORY SYSTEM TERMS 44 LESSON 4: DIGESTIVE, URINARY, AND REPRODUCTIVE SYSTEM TERMS 69 LESSON 5: INTEGUMENTARY, NERVOUS, AND ENDOCRINE S YSTEM TERMS 96 SELF-CHECK ANSWERS 134 © PENN FOSTER, INC. 2017 MEDICAL TERMINOLOGY PAGE III Contents INSTRUCTIONS INTRODUCTION Welcome to your course on medical terminology. You’re taking this course because you’re most likely interested in pursuing a health and science career, which entails proficiencyincommunicatingwithhealthcareprofessionalssuchasphysicians,nurses, or dentists. -

National Health and Nutrition Examination Survey Flyer (12/02)
Osteoporosis Introduction Figure 1. Prevalence of low femur bone density: Osteoporosis is a skeletal disorder in which bones United States 1988–94 weaken and risk of fracture is increased. While any fracture is a serious occurrence, hip fractures are of greatest public health concern because the consequences are often devastating. For example, those who experience hip fractures have an increased risk of death during the first 12 months after the fracture. Among those who survive, many experience loss of mobility and may have to enter long-term care facilities. Finally, hip fractures cost more to repair than any other type of osteoporotic fracture. Defining osteoporosis Bone strength is determined by the amount of bone mass or bone mineral density (BMD) and its quality and microarchitecture. The latter two qualities are not easy to measure, but methods to accurately assess BMD, such as dual-energy x-ray absorptiometry (DXA), are available. In prevalence of low total femur BMD among older U.S. adults 1994, an expert panel convened by the World Health were calculated using the WHO definitions. For this Organization (WHO) developed diagnostic criteria for analysis, BMD values of white women 50 years of age and osteoporosis and reduced bone density in white women. older were compared with those of 20–29-year-old non- These definitions are based on a comparison of the Hispanic white women. There is no consensus at this time individual’s BMD value with those of a young adult concerning the definition of low bone density in groups reference group. Two levels of reduced BMD were defined: other than white women; however, it is clear that osteopenia, which is a mild reduction in BMD, and osteoporosis is not solely a disease of white women. -

Oral Health & Dental Science
Research Article ISSN 2639-9490 Research Article Oral Health & Dental Science Mastication and Bone Density of Young Women and the Relationship with Tolerance to Exercise -Analysis with thermography and a Bicycle Ergometer- Hidetaka Nakamura1, Kazuyoshi Hashimoto2, Kei Takahashi1,2 and Hideto Matsuda2 1Department of Health and Nutrition, Faculty of Health and *Correspondence: Human Life, Nagoya Bunri University, Japan. Hidetaka Nakamura, 365, Maeda, Inazawa-cho, Inazawa City, Aic- hi, Japan, Tel: +81-587-23-2400; Fax: +81-587-21-2844. 2Department of Fixed Prosthodontics, School of Dentistry, Aichi Gakuin University, Japan. Received: 17 January 2020; Accepted: 05 February 2020 Citation: Hidetaka Nakamura, Kazuyoshi Hashimoto, Kei Takahashi, et al. Mastication and Bone Density of Young Women and the Relationship with Tolerance to Exercise -Analysis with thermography and a Bicycle Ergometer-. Oral Health Dental Sci. 2020; 4(1); 1-8. ABSTRACT Introduction: Chewing well is linked to preventing obesity and lowering the risk of type-2 diabetes and the importance of mastication is recognized. In the field of dentistry, there have been numerous reports on the relationship between bite and tolerance to exercise. However due to the lack of reports relating to mastication and tolerance to exercise we aim to clarify the relationship between mastication and tolerance to exercise and bone density. Method: 23 healthy young females (21.3 ± 0.4 years old) without a history of exercise had their habitual non- masticatory side determined by finding the main occluding area using stopping. The facial skin temperature at rest on the habitual non-masticatory side was measured using thermography and the area was multiplied by that temperature for each 1℃ and totaled. -

GLOSSARY of MEDICAL and ANATOMICAL TERMS
GLOSSARY of MEDICAL and ANATOMICAL TERMS Abbreviations: • A. Arabic • abb. = abbreviation • c. circa = about • F. French • adj. adjective • G. Greek • Ge. German • cf. compare • L. Latin • dim. = diminutive • OF. Old French • ( ) plural form in brackets A-band abb. of anisotropic band G. anisos = unequal + tropos = turning; meaning having not equal properties in every direction; transverse bands in living skeletal muscle which rotate the plane of polarised light, cf. I-band. Abbé, Ernst. 1840-1905. German physicist; mathematical analysis of optics as a basis for constructing better microscopes; devised oil immersion lens; Abbé condenser. absorption L. absorbere = to suck up. acervulus L. = sand, gritty; brain sand (cf. psammoma body). acetylcholine an ester of choline found in many tissue, synapses & neuromuscular junctions, where it is a neural transmitter. acetylcholinesterase enzyme at motor end-plate responsible for rapid destruction of acetylcholine, a neurotransmitter. acidophilic adj. L. acidus = sour + G. philein = to love; affinity for an acidic dye, such as eosin staining cytoplasmic proteins. acinus (-i) L. = a juicy berry, a grape; applied to small, rounded terminal secretory units of compound exocrine glands that have a small lumen (adj. acinar). acrosome G. akron = extremity + soma = body; head of spermatozoon. actin polymer protein filament found in the intracellular cytoskeleton, particularly in the thin (I-) bands of striated muscle. adenohypophysis G. ade = an acorn + hypophyses = an undergrowth; anterior lobe of hypophysis (cf. pituitary). adenoid G. " + -oeides = in form of; in the form of a gland, glandular; the pharyngeal tonsil. adipocyte L. adeps = fat (of an animal) + G. kytos = a container; cells responsible for storage and metabolism of lipids, found in white fat and brown fat. -

98796-Anatomy of the Orbit
Anatomy of the orbit Prof. Pia C Sundgren MD, PhD Department of Diagnostic Radiology, Clinical Sciences, Lund University, Sweden Lund University / Faculty of Medicine / Inst. Clinical Sciences / Radiology / ECNR Dubrovnik / Oct 2018 Lund University / Faculty of Medicine / Inst. Clinical Sciences / Radiology / ECNR Dubrovnik / Oct 2018 Lay-out • brief overview of the basic anatomy of the orbit and its structures • the orbit is a complicated structure due to its embryological composition • high number of entities, and diseases due to its composition of ectoderm, surface ectoderm and mesoderm Recommend you to read for more details Lund University / Faculty of Medicine / Inst. Clinical Sciences / Radiology / ECNR Dubrovnik / Oct 2018 Lund University / Faculty of Medicine / Inst. Clinical Sciences / Radiology / ECNR Dubrovnik / Oct 2018 3 x 3 Imaging technique 3 layers: - neuroectoderm (retina, iris, optic nerve) - surface ectoderm (lens) • CT and / or MR - mesoderm (vascular structures, sclera, choroid) •IOM plane 3 spaces: - pre-septal •thin slices extraconal - post-septal • axial and coronal projections intraconal • CT: soft tissue and bone windows 3 motor nerves: - occulomotor (III) • MR: T1 pre and post, T2, STIR, fat suppression, DWI (?) - trochlear (IV) - abducens (VI) Lund University / Faculty of Medicine / Inst. Clinical Sciences / Radiology / ECNR Dubrovnik / Oct 2018 Lund University / Faculty of Medicine / Inst. Clinical Sciences / Radiology / ECNR Dubrovnik / Oct 2018 Superior orbital fissure • cranial nerves (CN) III, IV, and VI • lacrimal nerve • frontal nerve • nasociliary nerve • orbital branch of middle meningeal artery • recurrent branch of lacrimal artery • superior orbital vein • superior ophthalmic vein Lund University / Faculty of Medicine / Inst. Clinical Sciences / Radiology / ECNR Dubrovnik / Oct 2018 Lund University / Faculty of Medicine / Inst. -

Morphology of the Foramen Magnum in Young Eastern European Adults
Folia Morphol. Vol. 71, No. 4, pp. 205–216 Copyright © 2012 Via Medica O R I G I N A L A R T I C L E ISSN 0015–5659 www.fm.viamedica.pl Morphology of the foramen magnum in young Eastern European adults F. Burdan1, 2, J. Szumiło3, J. Walocha4, L. Klepacz5, B. Madej1, W. Dworzański1, R. Klepacz3, A. Dworzańska1, E. Czekajska-Chehab6, A. Drop6 1Department of Human Anatomy, Medical University of Lublin, Lublin, Poland 2St. John’s Cancer Centre, Lublin, Poland 3Department of Clinical Pathomorphology, Medical University of Lublin, Lublin, Poland 4Department of Anatomy, Collegium Medicum, Jagiellonian University, Krakow, Poland 5Department of Psychiatry and Behavioural Sciences, Behavioural Health Centre, New York Medical College, Valhalla NY, USA 6Department of General Radiology and Nuclear Medicine, Medical University of Lublin, Lublin, Poland [Received 21 July 2012; Accepted 7 September 2012] Background: The foramen magnum is an important anatomical opening in the base of the skull through which the posterior cranial fossa communicates with the vertebral canal. It is also related to a number of pathological condi- tions including Chiari malformations, various tumours, and occipital dysplasias. The aim of the study was to evaluate the morphology of the foramen magnum in adult individuals in relation to sex. Material and methods: The morphology of the foramen magnum was evalu- ated using 3D computer tomography images in 313 individuals (142 male, 171 female) aged 20–30 years. Results: The mean values of the foramen length (37.06 ± 3.07 vs. 35.47 ± ± 2.60 mm), breadth (32.98 ± 2.78 vs. 30.95 ± 2.71 mm) and area (877.40 ± ± 131.64 vs. -

The Skull O Neurocranium, Form and Function O Dermatocranium, Form
Lesson 15 ◊ Lesson Outline: ♦ The Skull o Neurocranium, Form and Function o Dermatocranium, Form and Function o Splanchnocranium, Form and Function • Evolution and Design of Jaws • Fate of the Splanchnocranium ♦ Trends ◊ Objectives: At the end of this lesson, you should be able to: ♦ Describe the structure and function of the neurocranium ♦ Describe the structure and function of the dermatocranium ♦ Describe the origin of the splanchnocranium and discuss the various structures that have evolved from it. ♦ Describe the structure and function of the various structures that have been derived from the splanchnocranium ♦ Discuss various types of jaw suspension and the significance of the differences in each type ◊ References: ♦ Chapter: 9: 162-198 ◊ Reading for Next Lesson: ♦ Chapter: 9: 162-198 The Skull: From an anatomical perspective, the skull is composed of three parts based on the origins of the various components that make up the final product. These are the: Neurocranium (Chondocranium) Dermatocranium Splanchnocranium Each part is distinguished by its ontogenetic and phylogenetic origins although all three work together to produce the skull. The first two are considered part of the Cranial Skeleton. The latter is considered as a separate Visceral Skeleton in our textbook. Many other morphologists include the visceral skeleton as part of the cranial skeleton. This is a complex group of elements that are derived from the ancestral skeleton of the branchial arches and that ultimately gives rise to the jaws and the skeleton of the gill -
Osteoma of Occipital Bone
© 2003 Indian Journal of Surgery www.indianjsurg.comCase Report Effective treatment is crucial for avoiding recurrent Low-grade chondrosarcoma in an extremity can be incidence and depends on excising all tissues with treated with limited surgery. carcinoma. As the tumour is radio-resistant, complete removal is the only treatment of choice. A wide excision REFERENCES for low-grade chondrosarcoma is generally advised. Following open biopsy, local excision or, if required, 1. Bovee JVMG, van der Heul RO, Taminiau AHM, Hogendoorn PCW, reconstruction is advised.5 Chondrosarcoma of the phalanx: A locally aggressive lesion with minimal metastatic potential. Cancer 1999;86:1724-32. 2. Evans HL, Ayala AG, Romsdahl MM, Prognostic factors in chond- In our case, we think that the removal of the tumoral rosarcoma of bone. Cancer 1977;40:818-31. tissue from the normal tissue margin is the treatment 3. Dahlin DC, Beabout JW, Dedifferentiation of low-grade chondro- sarcomas. Cancer 1971;28:461-6. of choice. Our case is a young case that had Grade 1 4. Damron TA, Rock MG, Unni KK, Subcutaneous involvement after chondrosarcoma in his fourth and fifth finger and fifth a metacarpal chondrosarcoma: Case report and review of litera- metatarsal diaphysis. The difference of our case from ture. Clin Orthop 1995;316:189-94. 5. Ogose A, Unni KK, Swee RG, May GK, Rowland CM, Sim FH. the ones reported in literature is that he was young Chondrosarcoma of small bones of the hands and feet. Cancer (18-year-old) and had a lesion involving two different 1997;80:50-9. compartments synchronously as localization. -

Bone Loss & Bone Formation
EFF E CTS OF CATAPL E X ® D, CALCIFOOD ®, & OSTROPHIN PMG ® ON MARK E RS OF BON E LOSS AND BON E FORMATION David M. Barnes, Ph.D. | Research and Development, Standard Process Inc. 800-848-5061 | www.standardprocess.com EFF E CTS OF CATAPL E X ® D, CALCIFOOD ®, AND OSTROPHIN PMG ® ON MARK E RS OF BON E LOSS AND BON E FORMATION Bone mass decreases with age and failure to maintain bone mass may lead to painful bone conditions like Table 1. Osteoporosis Risk Factors osteoporosis and bone fractures. Thirty-four million Americans are currently at risk for osteoporosis, a • Age. Your risk of osteoporosis disease that researchers agree is largely preventable with increases as you age. healthy nutrition and lifestyle (Hampton, 2004). • Gender. Females are at greater risk It is well-established that intake of both calcium of developing osteoporosis. and vitamin D are effective in supporting • Family and personal history bone health (Boonen et al., 2006). of fractures as an adult. The aim of this study was to measure the effects of • Race. Women who are Caucasian or Asian three Standard Process whole food supplements– are more likely to develop osteoporosis. Cataplex® D, Calcifood®, and Ostrophin PMG®–on changes in bone metabolism of elderly subjects • Bone structure and body weight. Small- with osteopenia (decreased bone density). boned and thin women are at greater risk. Background • Menopause. Postmenopausal women have an The risk of osteoporosis increases with age and it is likely increased risk of developing osteoporosis. that in a population expecting increased longevity, reported • Lifestyle. Smoking and excessive alcohol intake cases of osteoporosis will rise.