Hypothesis Spinal Shock and `Brain Death': Somatic Pathophysiological
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Suplento1 Volumen 71 En
S1 Volumen 71 Mayo 2015 Revista Española de Vol. 71 Supl. 1 • Mayo 2015 Vol. Clínica e Investigación Órgano de expresión de la Sociedad Española de SEINAP Investigación en Nutrición y Alimentación en Pediatría Sumario XXX CONGRESO DE LA SOCIEDAD espaÑOLA DE CUIDADOS INTENSIVOS PEDIÁTRICOS Toledo, 7-9 de mayo de 2015 MESA REDONDA: ¿HACIA DÓNDE VAMOS EN LA MESA REDONDA: EL PACIENTE AGUDO MONITORIZACIÓN? CRONIFICADO EN UCIP 1 Monitorización mediante pulsioximetría: ¿sólo saturación 47 Nutrición en el paciente crítico de larga estancia en UCIP. de oxígeno? P. García Soler Z. Martínez de Compañón Martínez de Marigorta 3 Avances en la monitorización de la sedoanalgesia. S. Mencía 53 Traqueostomía, ¿cuándo realizarla? M.A. García Teresa Bartolomé y Grupo de Sedoanalgesia de la SECIP 60 Los cuidados de enfermería, ¿un reto? J.M. García Piñero 8 Avances en neuromonitorización. B. Cabeza Martín CHARLA-COLOQUIO SESIÓN DE PUESTA AL DÍA: ¿ES BENEFICIOSA LA 64 La formación en la preparación de las UCIPs FLUIDOTERAPIA PARA MI PACIENTE? españolas frente al riesgo de epidemias infecciosas. 13 Sobrecarga de líquidos y morbimortalidad asociada. J.C. de Carlos Vicente M.T. Alonso 68 Lecciones aprendidas durante la crisis del Ébola: 20 Estrategias de fluidoterapia racional en Cuidados experiencia del intensivista de adultos. J.C. Figueira Intensivos Pediátricos. P. de la Oliva Senovilla Iglesias 72 El niño con enfermedad por virus Ébola: un nuevo reto MESA REDONDA: INDICADORES DE CALIDAD para el intensivista pediátrico. E. Álvarez Rojas DE LA SECIP 23 Evolución de la cultura de seguridad en UCIP. MESA REDONDA: UCIP ABIERTAS 24 HORAS, La comunicación efectiva. -

Brain Death and the Cervical Spinal Cord: a Confounding Factor for the Clinical Examination
Spinal Cord (2010) 48, 2–9 & 2010 International Spinal Cord Society All rights reserved 1362-4393/10 $32.00 www.nature.com/sc REVIEW Brain death and the cervical spinal cord: a confounding factor for the clinical examination AR Joffe, N Anton and J Blackwood Department of Pediatrics, Stollery Children’s Hospital, University of Alberta, Edmonton, Alberta, Canada Study design: This study is a systematic review. Objectives: Brain death (BD) is a clinical diagnosis, made by documenting absent brainstem functions, including unresponsive coma and apnea. Cervical spinal cord dysfunction would confound clinical diagnosis of BD. Our objective was to determine whether cervical spinal cord dysfunction is common in BD. Methods: A case of BD showing cervical cord compression on magnetic resonance imaging prompted a literature review from 1965 to 2008 for any reports of cervical spinal cord injury associated with brain herniation or BD. Results: A total of 12 cases of brain herniation in meningitis occurred shortly after a lumbar puncture with acute respiratory arrest and quadriplegia. In total, nine cases of acute brain herniation from various non-meningitis causes resulted in acute quadriplegia. The cases suggest that direct compression of the cervical spinal cord, or the anterior spinal arteries during cerebellar tonsillar herniation cause ischemic injury to the cord. No case series of brain herniation specifically mentioned spinal cord injury, but many survivors had severe disability including spastic limbs. Only two pathological series of BD examined the spinal cord; 56–100% of cases had upper cervical spinal cord damage, suggesting infarction from direct compression of the cord or its arterial blood supply. -

Piercing the Veil: the Limits of Brain Death As a Legal Fiction
University of Michigan Journal of Law Reform Volume 48 2015 Piercing the Veil: The Limits of Brain Death as a Legal Fiction Seema K. Shah Department of Bioethics, National Institutes of Health Follow this and additional works at: https://repository.law.umich.edu/mjlr Part of the Health Law and Policy Commons, and the Medical Jurisprudence Commons Recommended Citation Seema K. Shah, Piercing the Veil: The Limits of Brain Death as a Legal Fiction, 48 U. MICH. J. L. REFORM 301 (2015). Available at: https://repository.law.umich.edu/mjlr/vol48/iss2/1 This Article is brought to you for free and open access by the University of Michigan Journal of Law Reform at University of Michigan Law School Scholarship Repository. It has been accepted for inclusion in University of Michigan Journal of Law Reform by an authorized editor of University of Michigan Law School Scholarship Repository. For more information, please contact [email protected]. PIERCING THE VEIL: THE LIMITS OF BRAIN DEATH AS A LEGAL FICTION Seema K. Shah* Brain death is different from the traditional, biological conception of death. Al- though there is no possibility of a meaningful recovery, considerable scientific evidence shows that neurological and other functions persist in patients accurately diagnosed as brain dead. Elsewhere with others, I have argued that brain death should be understood as an unacknowledged status legal fiction. A legal fiction arises when the law treats something as true, though it is known to be false or not known to be true, for a particular legal purpose (like the fiction that corporations are persons). -

Book of Abstracts
IAPDD 2018 ABSTRACTS A Fate Worse Than Death Todd Karhu ............................................................................................................................................. 3 Ancient Lessons on the Norms of Grief Emilio Comay del Junco ........................................................................................................................ 4 Beyond Morality and the Clinic: Contemplating End-Of-Life Decisions Yael Lavi .................................................................................................................................................. 5 Brainstem Death, Cerebral Death, or Whole-Brain Death? Personal Identity and the Destruction of the Brain Lukas Meier ............................................................................................................................................ 6 Choosing Immortality Tatjana von Solodkoff ............................................................................................................................ 7 Death and Grief Piers Benn ................................................................................................................................................ 8 Death and Possibility Roman Altshuler .................................................................................................................................... 9 Does Death Render Life Absurd? Joshua Thomas .................................................................................................................................... -

Locked-In' Syndrome, the Persistent Vegetative State and Brain Death
Spinal Cord (1998) 36, 741 ± 743 ã 1998 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/98 $12.00 http://www.stockton-press.co.uk/sc Moral Dilemmas Moral dilemmas of tetraplegia; the `locked-in' syndrome, the persistent vegetative state and brain death R Firsching Director and Professor, Klinik fuÈr Neurochirurgie, UniversitaÈtsklinikum, Leipziger Str. 44; 39120 Magdeburg, Germany Keywords: tetraplegia; `locked-in' syndrome; persistent vegetative state; brain death Lesions of the upper part of the spinal cord, the persistent vegetative state (PVS) stand on less safe medulla oblongata or the brain stem have dierent grounds and greater national dierences may be neurological sequelae depending on their exact location discerned: The causes may be variable, ranging from and extent. trauma to hemorrhage, hypoxia and infection. The High tetraplegia with a lesion at the level of the C3 pathomorphology is a matter of debate.5 Findings segment will leave the patient helpless but fully from the most famous PVS patient, KA Quinlan, conscious of his situation, and communication is revealed severe destruction of the thalamus,6 also usually possible. destruction of white matter and extensive destruction The patient who is `locked in' suers from a lesion of the cerebral cortex has been reported. The level of of the pyramidal tract, mostly at the upper pontine ± consciousness in these patients cannot be clari®ed, as cerebral peduncle ± level.1 Communication is reduced they are unresponsive. They are certainly not to vertical eye movements and blinking. comatose, as they open their eyes, and the kind of The persistent vegetative state is a quite hetero- pain perception that these patients have is similarly genous entity, and the underlying lesions are variable. -

Pitfalls in the Diagnosis of Brain Death
Neurocritical Care Society Neurocrit Care DOI 10.1007/s12028-009-9231-y REVIEW ARTICLE Pitfalls in the Diagnosis of Brain Death Katharina M. Busl Æ David M. Greer Ó Humana Press Inc. 2009 Abstract Since the establishment of the concept of death, i.e., brain death. The criteria included unrespon- declaring death by brain criteria, a large extent of variability siveness, absence of movement or breathing, and absence in the determination of brain death has been reported. There of brainstem reflexes. In addition, an isoelectric EEG was are no standardized practical guidelines, and major differ- recommended, and hypothermia and drug intoxication ences exist in the requirements for the declaration of were to be excluded [2]. brain death throughout the USA and internationally. The In 1981, the President’s Commission for the Study of American Academy of Neurology published evidence- Ethical Problems in Medicine and Behavioral Research based practice parameters for the determination of brain issued a landmark report on ‘‘Defining Death’’ and rede- death in adults in 1995, requiring the irreversible absence of fined the criteria for the diagnosis of brain death in adults, clinical brain function with the cardinal features of coma, encompassing the complete cessation of all functions of the absent brainstem reflexes, and apnea, as well as the exclu- entire brain (i.e., ‘‘whole brain concept’’), and its irre- sion of reversible confounders. Ancillary tests are versibility [3]. The Uniform Determination of Death Act, recommended in cases of uncertainty of the clinical diag- which was subsequently adopted as federal legislation by nosis. Every step in the determination of brain death bears most states in the USA, is based on these recommenda- potential pitfalls which can lead to errors in the diagnosis of tions. -

Pediatric Shock
REVIEW Pediatric shock Usha Sethuraman† & Pediatric shock accounts for significant mortality and morbidity worldwide, but remains Nirmala Bhaya incompletely understood in many ways, even today. Despite varied etiologies, the end result †Author for correspondence of pediatric shock is a state of energy failure and inadequate supply to meet the metabolic Children’s Hospital of Michigan, Division of demands of the body. Although the mortality rate of septic shock is decreasing, the severity Emergency Medicine, is on the rise. Changing epidemiology due to effective eradication programs has brought in Carman and Ann Adams new microorganisms. In the past, adult criteria had been used for the diagnosis and Department of Pediatrics, 3901 Beaubien Boulevard, management of septic shock in pediatrics. These have been modified in recent times to suit Detroit, MI 48201, USA the pediatric and neonatal population. In this article we review the pathophysiology, Tel.: +1 313 745 5260 epidemiology and recent guidelines in the management of pediatric shock. Fax: +1 313 993 7166 [email protected] Shock is an acute syndrome in which the circu- to generate ATP. It is postulated that in the face of latory system is unable to provide adequate oxy- prolonged systemic inflammatory insult, overpro- gen and nutrients to meet the metabolic duction of cytokines, nitric oxide and other medi- demands of vital organs [1]. Due to the inade- ators, and in the face of hypoxia and tissue quate ATP production to support function, the hypoperfusion, the body responds by turning off cell reverts to anaerobic metabolism, causing the most energy-consuming biophysiological acute energy failure [2]. -
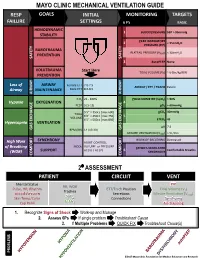
Mechanical Ventilation Guide
MAYO CLINIC MECHANICAL VENTILATION GUIDE RESP GOALS INITIAL MONITORING TARGETS FAILURE SETTINGS 6 P’s BASIC HEMODYNAMIC 1 BLOOD PRESSURE SBP > 90mmHg STABILITY PEAK INSPIRATORY 2 < 35cmH O PRESSURE (PIP) 2 BAROTRAUMA PLATEAU PRESSURE (P ) < 30cmH O PREVENTION PLAT 2 SAFETY SAFETY 3 AutoPEEP None VOLUTRAUMA Start Here TIDAL VOLUME (V ) ~ 6-8cc/kg IBW PREVENTION T Loss of AIRWAY Female ETT 7.0-7.5 AIRWAY / ETT / TRACH Patent Airway MAINTENANCE Male ETT 8.0-8.5 AIRWAY AIRWAY FiO2 21 - 100% PULSE OXIMETRY (SpO2) > 90% Hypoxia OXYGENATION 4 PEEP 5 [5-15] pO2 > 60mmHg 5’5” = 350cc [max 600] pCO2 40mmHg TIDAL 6’0” = 450cc [max 750] 5 VOLUME 6’5” = 500cc [max 850] ETCO2 45 Hypercapnia VENTILATION pH 7.4 GAS GAS EXCHANGE BPM (RR) 14 [10-30] GAS EXCHANGE MINUTE VENTILATION (VMIN) > 5L/min SYNCHRONY WORK OF BREATHING Decreased High Work ASSIST CONTROL MODE VOLUME or PRESSURE of Breathing PATIENT-VENTILATOR AC (V) / AC (P) 6 Comfortable Breaths (WOB) SUPPORT SYNCHRONY COMFORT COMFORT 2⁰ ASSESSMENT PATIENT CIRCUIT VENT Mental Status PIP RR, WOB Pulse, HR, Rhythm ETT/Trach Position Tidal Volume (V ) Trachea T Blood Pressure Secretions Minute Ventilation (V ) SpO MIN Skin Temp/Color 2 Connections Synchrony ETCO Cap Refill 2 Air-Trapping 1. Recognize Signs of Shock Work-up and Manage 2. Assess 6Ps If single problem Troubleshoot Cause 3. If Multiple Problems QUICK FIX Troubleshoot Cause(s) PROBLEMS ©2017 Mayo Clinic Foundation for Medical Education and Research CAUSES QUICK FIX MANAGEMENT Bleeding Hemostasis, Transfuse, Treat cause, Temperature control HYPOVOLEMIA Dehydration Fluid Resuscitation (End points = hypoxia, ↑StO2, ↓PVI) 3rd Spacing Treat cause, Beware of hypoxia (3rd spacing in lungs) Pneumothorax Needle D, Chest tube Abdominal Compartment Syndrome FLUID Treat Cause, Paralyze, Surgery (Open Abdomen) OBSTRUCTED BLOOD RETURN Air-Trapping (AutoPEEP) (if not hypoxic) Pop off vent & SEE SEPARATE CHART PEEP Reduce PEEP Cardiac Tamponade Pericardiocentesis, Drain. -

The Vegetative State: Guidance on Diagnosis and Management
n CLINICAL GUIDANCE The vegetative state: guidance on diagnosis and management A report of a working party of the Royal College of Physicians contrasts with sleep, a state of eye closure and motor Clin Med 1INTRODUCTION quiescence. There are degrees of wakefulness. 2003;3:249–54 Wakefulness is normally associated with conscious awareness, but the VS indicates that wakefulness and Background awareness can be dissociated. This can occur because 1.1 This guidance has been compiled to replace the brain systems controlling wakefulness, in the the recommendations published by the Royal College upper brainstem and thalamus, are largely distinct of Physicians in 1996, 1 in response to requests for from those which mediate awareness. 6 clarification from the Official Solicitor. The guidance applies primarily to adult patients and older children Awareness in whom it is possible to apply the criteria for diagnosis discussed below. 1.6 Awareness refers to the ability to have, and the having of, experience of any kind. We are typically aware of our surroundings and of bodily sensations, Wakefulness without awareness but the contents of awareness can also include our 1.2 Consciousness is an ambiguous term, encom- memories, thoughts, emotions and intentions. passing both wakefulness and awareness. This dis- Although understanding of the brain mechanisms of tinction is crucial to the concept of the vegetative awareness is incomplete, structures in the cerebral state, in which wakefulness recovers after brain hemispheres clearly play a key role. Awareness is not injury without recovery of awareness. 2–5 a single indivisible capacity: brain damage can selectively impair some aspects of awareness, leaving others intact. -

Primary Brainstem Death
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.51.5.646 on 1 May 1988. Downloaded from Journal of Neurology, Neurosurgery, and Psychiatry 1988;51:646-650 Primary brainstem death: a clinico-pathological study J OGATA,* M IMAKITA,t C YUTANI,t S MIYAMOTO4, H KIKUCHII From the Research Institute, *Department ofPathology, tDepartment ofNeurosurgery, INational Cardiovascular Centre, Osaka, Japan SUMMARY A case of primary brainstem death in a man with surgically treated cerebellar hae- morrhage is reported. Necropsy revealed extensive necrosis confined to the brainstem and cere- bellum. The absence of diabetes insipidus and the persistence of electroencephalographic activity were the characteristic clinical features of the case. This differentiates the condition from so-called "whole brain death". Analysis of three further cases with acute vascular lesions of the brainstem or cerebellum, shown at necropsy, revealed that primary brainstem death with prolonged somatic survival can occur in specific circumstances after surgical intervension Brainstem death, as encountered in clinical practice, Case report is nearly always a secondary phenomenon. It is the infratentorial repercussion of supratentorial events A 47 year old hypertensive man was found on lying the floor.Protected by copyright. and has been described as the "physiological core" of In 10 minutes, he became unresponsive. The blood pressure "whole brain death" and as the main determinant of measured in a nearby hospital was 270/140 mmHg. Within its clinical features and cardiac prognosis.' Lesions to an hour, he was intubated because spontaneous respiration the upper and lower brainstem which deprive it of its ceased. The blood pressure fell at one stage to 80/52 mmHg. -

Buddhism and Death: the Brain-Centered Criteria
Journal of Buddhist Ethics ISSN 1076-9005 http://jbe.gold.ac.uk/ Buddhism and Death: The Brain-Centered Criteria John-Anderson L. Meyer University of Hawai‘i Email: [email protected] Copyright Notice: Digital copies of this work may be made and distributed provided no change is made and no alteration is made to the content. Reproduction in any other format, with the exception of a single copy for private study, requires the written permission of the author. All enquiries to: [email protected] Buddhism and Death: The Brain-Centered Criteria John-Anderson L. Meyer Abstract This essay explores the two main definitions of human death that have gained popularity in the western medical con- text in recent years, and attempts to determine which of these criteria — “whole-brain” or “cerebral” — is best in accord with a Buddhist understanding of death. In the end, the position is taken that there is textual and linguistic evidence in place for both the “cerebral” and “whole-brain” definitions of death. Be- cause the textual sources underdetermine the definitive Buddhist conception of death, it is left to careful reasoning by way of logic, intuition, and inference to determine which definition of death is best representative of Buddhism. Buddhism, generally considered, is a belief system that holds as its ultimate aim the elimination of suffering through the cessation of the endless cycle of death and rebirth. The attainment of nirvana, defined by some as “the absolute extinction of the life-affirming will manifested as . convul- sively clinging to existence; and therewith also the ultimate and absolute deliverance from all future rebirth, old age, disease and death,”1 is the goal of Buddhism and the outcome of the definitive elimination of all suffering. -

Polytrauma Shock • Trauma Related Costs in the U.S
POLYTRAUMA SHOCK • TRAUMA RELATED COSTS IN THE U.S. 400 BILLION $ • 3.8 MILLION DEATHS PER YEAR • THE LEADING CAUSE OF DEATH IN PERSONS AGED 1 TO 45 IN THE MOST DEVELOPED COUNTRIES • TRIMODAL DEATH DISTRIBUTION 1. SECONDS, MINS FOLLOWING INJURY DUE TO BRAIN, C. SPINE, LARGE VESSEL INJ. 2. 1-2 HOURS FOLLOWING INJURY DUE TO EPIDURAL HAEMATOMAS, BLEEDINGS GOLDEN HOUR 3. SEVERAL DAYS FOLLOWING INJURY DUE TO M.O.F., SEPSIS TRIMODAL DEATH DISTRIBUTION 50% 40% 30% 20% 10% 0% HOURS 0 1 2 3 4 WEEKS 1 2 3 4 TRIMODAL BIMODAL? THE SECOND GROUP IS DECREASING DUE TO PROPER TREATMENT GOLDEN HOUR NOT ONLY SALVAGEABILITY BUT MANY LATE PROBLEMS (SIRS, MOF) ARE THE CONSEQUENCES OF THE PRIMARY HYPOXIA AND MEDIATOR RELEASE SILVER DAY BRONZE WEEK PLATINA 10 MIN DEFINITION OF POLYTRAUMA A. INJURY TO ONE OR MORE BODY REGIONS OR ORGANS OF WHICH ONE, OR THEIR COMBINATIONS IS LIFE THREATENING B. INJURY TO MORE BODY REGIONS FOLLOWING WHICH, DURING TREATMENT, WE HAVE TO MAKE COMPROMISES C. INJURY TO HOLLOW ORGANS + INJURY TO EXTREMITIES D. INJURY DEFINED BY A SCORING SYSTEM TRAUMA SCORE NUMBER OF BREATHS PER MIN 0-4 INTENSITY OF BREATHING 0-1 SYSTOLIC BLOOD PRESSURE 0-4 CAPILLARY REFILL 0-2 GLASGOW COMA SCALE 0-5 POSSIBILITY FOR SURVIVAL 16+ <2 99% 0% GLASGOW COMA SCALE EYE OPENING SPONTANEOUS 4 TO SPEECH 3 TO PAIN 2 NONE 1 BEST MOTOR RESPONSE OBEYS COMMANDS 6 LOCALIZES PAIN 5 NORMAL FLEXION 4 ABNORMAL FLEXION 3 EXTENSION 2 NONE 1 VERBAL RESPONSE ORIENTED 5 CONFUSED CONVERS. 4 WORDS 3 SOUNDS 2 NOTHING 1 ABBREVIATED INJURY SCALE (ISS) 1 MILD 2 MEDIUM 3 SEVERE 4 VERY