Search Strategies
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Hemangiosarcoma Philip J
Ettinger & Feldman – Textbook of Veterinary Internal Medicine Client Information Sheet Hemangiosarcoma Philip J. Bergman What is hemangiosarcoma? Hemangiosarcoma (HSA; angiosarcoma or malignant hemangioendothelioma) is an extremely aggressive tumor of blood vessel origin. Because blood vessels are present throughout the body, virtually any site in the body can have HSA. HSA occurs most frequently in dogs (approximately 2% of all tumors) and the most common site is the spleen. However, additional common sites include the heart, liver, muscle, lung skin, bones, kidney, brain, abdomen, and oral cavity. In three large canine splenic disease studies encompassing approximately 2000 dogs, a “rule of two thirds” was found suggesting that approximately two thirds of dogs with a splenic mass have a cancer (therefore one third are not malignant) and two thirds of the malignant tumors of the spleen are HSA. HSA is a disease generally of older dogs and cats with an average onset of 9 to 10 years; however, there are reports of extremely young dogs and cats with this disease (5 to 6 months to a few years of age). German shepherd dogs are most commonly diagnosed with HSA; however, other large breed dogs such as golden retrievers and Labrador retrievers may also be overrepresented. In cats, the most common breed is the domestic shorthair. The cause of HSA in dogs and cats is presently unknown. Exposures to toxins such as chemicals, insecticides, and radiation have been reported in humans to be associated with HSA. Ultraviolet light exposure from the sun may be a potential cause of HSA in dogs, as HSAs of the skin are commonly seen in dogs with light hair and poor pigmentation (e.g., Salukis, Whippets, and white Bulldogs). -

Unusual Multiple Cutaneous Retiform Hemangioendothelioma on Forearm
Clinical and Diagnostic Pathology Research Article Unusual multiple cutaneous retiform hemangioendothelioma on forearm and neck misdiagnosed as angiosarcoma with metastasis Bin-cai Pan1, Chun-hua Wang1, Gui-fang Huang1, Xiao-ying Tian2 and Zhi Li3* 1Department of Pathology, Guangdong Tongjiang Hospital, Nanguo East Road, Shunde district, Foshan 528300, China 2School of Chinese Medicine, Hong Kong Baptist University 7, Baptist University Road, Kowloon Tong, Hong Kong, China 3Department of Pathology, The First Affiliated Hospital, Sun Yat-sen university.58, Zhongshan Road II,Guangzhou 510080, China Abstract Retiform hemangioendothelioma (RH) is extremely rare, and often involves the skin and subcutaneous tissues of distal extremities in young adults or children. Since its first description by Calonje in 1994, only a few primary multiple cases have been described in the literature. We present a case of unusual primary multiple RH on forearm and neck occurring in a 56 years old female patient. The patient presented with a slow-growing cutaneous plaque-like lesion on her left forearm, followed by another lesion at the site of neck for several years. In the skin biopsy examination, a diagnosis of angiosarcoma with cutaneous metastasis was made based on multiple lesions at different anatomic sites and vasoformative growth pattern with anastomosing channels under the microscopy. However, postoperative histological diagnosis of the lesion was primary multiple RH by thoroughly microscopical inspection and the presence of thin-walled interconnecting vascular channels arranged in a retiform pattern and absence of lymph node metastasis. Despite wide surgical excision with tumor-free margin, the tumor recurred at the neck 3 months after surgery. -

The Use of High Tumescent Power Assisted Liposuction in the Treatment of Madelung’S Collar
Letter to the Editor The use of high tumescent power assisted liposuction in the treatment of Madelung’s collar Henryk Witmanowski1,2, Łukasz Banasiak1, Grzegorz Kierzynka1, Jarosław Markowicz1, Jerzy Kolasiński1, Katarzyna Błochowiak3, Paweł Szychta1,4 1Department of Plastic, Reconstructive and Aesthetic Surgery, Medical College in Bydgoszcz, Nicolaus Copernicus University in Torun, Poland 2Department of Physiology, Poznan University of Medical Sciences, Poznan, Poland 3Department of the Oral Surgery, Poznan University of Medical Sciences, Poznan, Poland 4Department of Oncological Surgery and Breast Diseases, Polish Mother’s Memorial Hospital-Research Institute, Lodz, Poland Adv Dermatol Allergol 2017; XXXIV (4): 366–371 DOI: https://doi.org/10.5114/ada.2017.69319 Mild symmetrical lipomatosis (plural symmetrical The disease most commonly takes a proximal form lipomatosis, multiple symmetric lipomatosis – MSL), which takes the following areas of the body with the fol- also known as Madelung’s disease or Launois-Bensaude lowing frequency: the genial area 92.3%, cervical region syndrome is a rare disease of unknown etiology, first de- 67.7%, shoulder region 54.8%, abdominal 45.2%, chest scribed by Brodie in 1846, Madelung in 1888, and Launois 41.9%, thigh and pelvic rim 32.3% [11, 12]. The periph- with Bensaude in 1898 [1–3]. eral type mainly locates on both sides at the level of the Madelung’s disease incidence is 1 : 250000 [4]. Mul- hands, feet and knees, this is definitely a rarer form of tiple symmetric lipomatosis occurs mainly in the inhabit- the disease. The mixed form is described very rarely. The ants of the Mediterranean area and Eastern Europe, in specified central type is also engaged primarily around males (male to female ratio is 20 : 1), aged 30–70 years, the lower torso, and intermediate parts of the legs. -

Tumors and Tumor-Like Lesions of Blood Vessels 16 F.Ramon
16_DeSchepper_Tumors_and 15.09.2005 13:27 Uhr Seite 263 Chapter Tumors and Tumor-like Lesions of Blood Vessels 16 F.Ramon Contents 42]. There are two major classification schemes for vas- cular tumors. That of Enzinger et al. [12] relies on 16.1 Introduction . 263 pathological criteria and includes clinical and radiolog- 16.2 Definition and Classification . 264 ical features when appropriate. On the other hand, the 16.2.1 Benign Vascular Tumors . 264 classification of Mulliken and Glowacki [42] is based on 16.2.1.1 Classification of Mulliken . 264 endothelial growth characteristics and distinguishes 16.2.1.2 Classification of Enzinger . 264 16.2.1.3 WHO Classification . 265 hemangiomas from vascular malformations. The latter 16.2.2 Vascular Tumors of Borderline classification shows good correlation with the clinical or Intermediate Malignancy . 265 picture and imaging findings. 16.2.3 Malignant Vascular Tumors . 265 Hemangiomas are characterized by a phase of prolif- 16.2.4 Glomus Tumor . 266 eration and a stationary period, followed by involution. 16.2.5 Hemangiopericytoma . 266 Vascular malformations are no real tumors and can be 16.3 Incidence and Clinical Behavior . 266 divided into low- or high-flow lesions [65]. 16.3.1 Benign Vascular Tumors . 266 Cutaneous and subcutaneous lesions are usually 16.3.2 Angiomatous Syndromes . 267 easily diagnosed and present no significant diagnostic 16.3.3 Hemangioendothelioma . 267 problems. On the other hand, hemangiomas or vascular 16.3.4 Angiosarcomas . 268 16.3.5 Glomus Tumor . 268 malformations that arise in deep soft tissue must be dif- 16.3.6 Hemangiopericytoma . -

Central Nervous System Tumors General ~1% of Tumors in Adults, but ~25% of Malignancies in Children (Only 2Nd to Leukemia)
Last updated: 3/4/2021 Prepared by Kurt Schaberg Central Nervous System Tumors General ~1% of tumors in adults, but ~25% of malignancies in children (only 2nd to leukemia). Significant increase in incidence in primary brain tumors in elderly. Metastases to the brain far outnumber primary CNS tumors→ multiple cerebral tumors. One can develop a very good DDX by just location, age, and imaging. Differential Diagnosis by clinical information: Location Pediatric/Young Adult Older Adult Cerebral/ Ganglioglioma, DNET, PXA, Glioblastoma Multiforme (GBM) Supratentorial Ependymoma, AT/RT Infiltrating Astrocytoma (grades II-III), CNS Embryonal Neoplasms Oligodendroglioma, Metastases, Lymphoma, Infection Cerebellar/ PA, Medulloblastoma, Ependymoma, Metastases, Hemangioblastoma, Infratentorial/ Choroid plexus papilloma, AT/RT Choroid plexus papilloma, Subependymoma Fourth ventricle Brainstem PA, DMG Astrocytoma, Glioblastoma, DMG, Metastases Spinal cord Ependymoma, PA, DMG, MPE, Drop Ependymoma, Astrocytoma, DMG, MPE (filum), (intramedullary) metastases Paraganglioma (filum), Spinal cord Meningioma, Schwannoma, Schwannoma, Meningioma, (extramedullary) Metastases, Melanocytoma/melanoma Melanocytoma/melanoma, MPNST Spinal cord Bone tumor, Meningioma, Abscess, Herniated disk, Lymphoma, Abscess, (extradural) Vascular malformation, Metastases, Extra-axial/Dural/ Leukemia/lymphoma, Ewing Sarcoma, Meningioma, SFT, Metastases, Lymphoma, Leptomeningeal Rhabdomyosarcoma, Disseminated medulloblastoma, DLGNT, Sellar/infundibular Pituitary adenoma, Pituitary adenoma, -

Cutaneous Angiosarcoma: Report of Three Different and Typical Cases Admitted in a Unique Dermatology Clinic*
CASE REPORT 235 s Cutaneous angiosarcoma: report of three different and typical cases admitted in a unique dermatology clinic* Aline Neves Freitas Cabral1 Rafael Henrique Rocha1 Ana Cristina Vervloet do Amaral1 Karina Bittencourt Medeiros2 Paulo Sérgio Emerich Nogueira1 Lucia Martins Diniz3 DOI: http://dx.doi.org/10.1590/abd1806-4841.20175326 Abstract: Angiosarcoma is a rare and aggressive tumor with high rates of metastasis and relapse. It shows a particular predi- lection for the skin and superficial soft tissues. We report three distinct and typical cases of angiosarcoma that were diagnosed in a single dermatology clinic over the course of less than a year: i) Angiosarcoma in lower limb affected by chronic lymph- edema, featuring Stewart-Treves syndrome; ii) a case of the most common type of angiosarcoma loated in the scalp and face of elderly man and; iii) a skin Angiosarcoma in previously irradiated breast. All lesions presented characteristic histopathological findings: irregular vascular proliferation that dissects the collagen bundles with atypical endothelial nuclei projection toward the lumen. Keywords: Hemangiosarcoma; Lymphangiosarcoma; Lymphedema; Non-Filarial Lymphedema; Sarcoma INTRODUCTION Angiosarcoma (AS) is a rare and aggressive neoplasm, that fibers, formed by endothelium with atypical nuclei, prominent to- originates from endothelial cells of lymphatic and blood vessels. It ac- ward the lumen; The tumoral lesion exhibited cohesive epithelioid counts for 5% of malignant skin tumors and less than 1% of all sarco- masses of atypical, large, rounded cells with acidophilic cytoplasm mas. It is notable for having a predilection for the skin and superficial and frequent mitotic figures. (Figure 2). Immunohistochemical anal- soft tissues. -
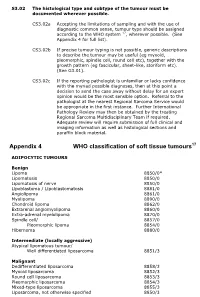

Appendix 4 WHO Classification of Soft Tissue Tumours17
S3.02 The histological type and subtype of the tumour must be documented wherever possible. CS3.02a Accepting the limitations of sampling and with the use of diagnostic common sense, tumour type should be assigned according to the WHO system 17, wherever possible. (See Appendix 4 for full list). CS3.02b If precise tumour typing is not possible, generic descriptions to describe the tumour may be useful (eg myxoid, pleomorphic, spindle cell, round cell etc), together with the growth pattern (eg fascicular, sheet-like, storiform etc). (See G3.01). CS3.02c If the reporting pathologist is unfamiliar or lacks confidence with the myriad possible diagnoses, then at this point a decision to send the case away without delay for an expert opinion would be the most sensible option. Referral to the pathologist at the nearest Regional Sarcoma Service would be appropriate in the first instance. Further International Pathology Review may then be obtained by the treating Regional Sarcoma Multidisciplinary Team if required. Adequate review will require submission of full clinical and imaging information as well as histological sections and paraffin block material. Appendix 4 WHO classification of soft tissue tumours17 ADIPOCYTIC TUMOURS Benign Lipoma 8850/0* Lipomatosis 8850/0 Lipomatosis of nerve 8850/0 Lipoblastoma / Lipoblastomatosis 8881/0 Angiolipoma 8861/0 Myolipoma 8890/0 Chondroid lipoma 8862/0 Extrarenal angiomyolipoma 8860/0 Extra-adrenal myelolipoma 8870/0 Spindle cell/ 8857/0 Pleomorphic lipoma 8854/0 Hibernoma 8880/0 Intermediate (locally -

Germline and Mosaic Mutations Causing Pituitary Tumours: Genetic and Molecular Aspects
240 2 Journal of S Pepe et al. Germline and mosaic 240:2 R21–R45 Endocrinology mutations in pituitary tumours REVIEW Germline and mosaic mutations causing pituitary tumours: genetic and molecular aspects Sara Pepe1,2, Márta Korbonits1 and Donato Iacovazzo1 1Centre for Endocrinology, William Harvey Research Institute, Barts and the London School of Medicine, Queen Mary University of London, London, UK 2Department of Medical Biotechnologies, University of Siena, Siena, Italy Correspondence should be addressed to M Korbonits: [email protected] Abstract While 95% of pituitary adenomas arise sporadically without a known inheritable Key Words predisposing mutation, in about 5% of the cases they can arise in a familial setting, either f genetics isolated (familial isolated pituitary adenoma or FIPA) or as part of a syndrome. FIPA is f pituitary caused, in 15–30% of all kindreds, by inactivating mutations in the AIP gene, encoding f pituitary adenoma a co-chaperone with a vast array of interacting partners and causing most commonly f mutation growth hormone excess. While the mechanisms linking AIP with pituitary tumorigenesis have not been fully understood, they are likely to involve several pathways, including the cAMP-dependent protein kinase A pathway via defective G inhibitory protein signalling or altered interaction with phosphodiesterases. The cAMP pathway is also affected by other conditions predisposing to pituitary tumours, including X-linked acrogigantism caused by duplications of the GPR101 gene, encoding an orphan G stimulatory protein- coupled receptor. Activating mosaic mutations in the GNAS gene, coding for the Gα stimulatory protein, cause McCune–Albright syndrome, while inactivating mutations in the regulatory type 1α subunit of protein kinase A represent the most frequent genetic cause of Carney complex, a syndromic condition with multi-organ manifestations also involving the pituitary gland. -

Pineal Region Tumors: Computed Tomographic-Pathologic Spectrum
415 Pineal Region Tumors: Computed Tomographic-Pathologic Spectrum Nancy N. Futrell' While several computed tomographic (CT) studies of posterior third ventricular Anne G. Osborn' neoplasms have included descriptions of pineal tumors, few reports have concentrated Bruce D. Cheson 2 on these uncommon lesions. Some authors have asserted that the CT appearance of many pineal tumors is virtually pathognomonic. A series of nine biopsy-proved pineal gland and eight other presumed tumors is presented that illustrates their remarkable heterogeneity in both histopathologic and CT appearance. These tumors included germinomas, teratocarcinomas, hamartomas, and other varieties. They had variable margination, attenuation, calcification, and suprasellar extension. Germinomas have the best response to radiation therapy. Biopsy of pineal region tumors is now feasible and is recommended for treatment planning. Tumors of the pineal region account for less th an 2% of all intracrani al neoplasms [1]. While several reports of computed tomography (CT) of third ventricular neoplasms have in cluded an occasi onal pineal tumor [2 , 3], few have focused on the radiographic spectrum of th ese uncommon lesions [4]. Some authors have asserted that the CT appearance of many pineal tumors is virtuall y pathognomonic [5]. We studied a series of nine biopsy-proven pineal gland tumors that demonstrated remarkable heterogeneity in both histopath ologic and CT appearance. Materials and Methods A total of 17 pineal gland tumors were detected in 15,000 consecutive CT scans. Four patients were female and 13 were male. Mean age for the fe males was 27 years; for the males, 15 years. Initial symptoms ranged from headache, nausea, and vomiting, to Parinaud syndrome, vi sual field defects, diabetes insipidus, and hypopituitari sm (table 1). -

Non-Hodgkin's Gastrointestinal Lymphoma Presenting As Acute
Cirujano CLINICAL CASE General July-September 2019 Vol. 41, no. 3 / p. 208-216 Non-Hodgkin’s gastrointestinal lymphoma presenting as acute abdomen Linfoma no Hodgkin gastrointestinal presentándose como abdomen agudo CLINICAL CASES Arcenio Luis Vargas-Ávila,* Alan Hernández-Rosas,** José Roldán-Tinoco,*** Levi Alan Guzmán-Peña,*** Julián Vargas-Flores,**** Julio Adán Campos-Badillo,*** CASOS CLÍNICOS Rubén Mena-Maldonado***** Keywords: Lymphoma, small ABSTRACT RESUMEN intestine, hemorrhage, acute abdomen. Non-Hodgkin lymphoma is an uncommon cancer, but El linfoma no Hodgkin es una neoplasia poco común, when it is a primary lymphoma, the gastrointestinal tract pero cuando se trata de un linfoma primario, el tracto Palabras clave: is the most commonly involved and one of the most gastrointestinal es el sitio más comúnmente implicado y Linfoma, intestino common extra-nodal sites. Multiple risk factors have una de las presentaciones extranodales más frecuentes. delgado, hemorragia, been associated. However, its etiology is still unknown. Se han asociado múltiples factores de riesgo; sin embar- abdomen agudo. Nowadays there exist histochemical markers to distinguish go, aún se desconoce su etiología. Actualmente existen different cell types, criteria, and scales to differentiate marcadores histoquímicos que permiten diferenciar los between primary and secondary intestinal lymphomas. distintos tipos celulares así como los criterios y escalas The definitive diagnosis is obtained with a histopathologic para distinguir entre linfomas intestinales primarios y and immunohistochemical study of the extracted surgical secundarios. El diagnóstico definitivo se logra con el piece. Some studies such as endoscopy, CAT scan or estudio histopatológico e inmunohistoquímico de la pieza capsule endoscopy and double balloon enteroscopy have extraída quirúrgica o endoscópicamente. -
Kaplan USMLE Step 2 CK Surgery Lecture Notes2018
USMLE ® • UP-TO-DATE ® STEP 2 CK STEP Updated annually by Kaplan’s all-star faculty STEP2 CK • INTEGRATED Lecture Notes 2018 Notes Lecture Packed with bridges between specialties and basic science Lecture Notes 2018 • TRUSTED Used by thousands of students each year to ace the exam USMLE Surgery Surgery Tell us what you think! Visit kaptest.com/booksfeedback and let us know about your book experience. ISBN: 978-1-5062-2822-8 kaplanmedical.com 9 7 8 1 5 0 6 2 2 8 2 2 8 USMLE® is a joint program of The Federation of State Medical Boards of the United States, Inc. and the National Board of Medical Examiners. USMLE® is a joint program of the Federation of State Medical Boards (FSMB) and the National Board of Medical Examiners (NBME), neither of which sponsors or endorses this product. 978-1-5062-2822-8_USMLE_Step2_CK_Surgery_Course_CVR.indd 1 6/21/17 10:58 AM ® STEP 2 CK Lecture Notes 2018 USMLE Surgery USMLE® is a joint program of The Federation of State Medical Boards of the United States, Inc. and the National Board of Medical Examiners. S2 Surgery.indb 1 6/20/17 9:15 AM USMLE® is a joint program of the Federation of State Medical Boards (FSMB) and the National Board of Medical Examiners (NBME), neither of which sponsors or endorses this product. This publication is designed to provide accurate information in regard to the subject matter covered as of its publication date, with the understanding that knowledge and best practice constantly evolve. The publisher is not engaged in rendering medical, legal, accounting, or other professional service. -

Eyelid Conjunctival Tumors
EYELID &CONJUNCTIVAL TUMORS PHOTOGRAPHIC ATLAS Dr. Olivier Galatoire Dr. Christine Levy-Gabriel Dr. Mathieu Zmuda EYELID & CONJUNCTIVAL TUMORS 4 EYELID & CONJUNCTIVAL TUMORS Dear readers, All rights of translation, adaptation, or reproduction by any means are reserved in all countries. The reproduction or representation, in whole or in part and by any means, of any of the pages published in the present book without the prior written consent of the publisher, is prohibited and illegal and would constitute an infringement. Only reproductions strictly reserved for the private use of the copier and not intended for collective use, and short analyses and quotations justified by the illustrative or scientific nature of the work in which they are incorporated, are authorized (Law of March 11, 1957 art. 40 and 41 and Criminal Code art. 425). EYELID & CONJUNCTIVAL TUMORS EYELID & CONJUNCTIVAL TUMORS 5 6 EYELID & CONJUNCTIVAL TUMORS Foreword Dr. Serge Morax I am honored to introduce this Photographic Atlas of palpebral and conjunctival tumors,which is the culmination of the close collaboration between Drs. Olivier Galatoire and Mathieu Zmuda of the A. de Rothschild Ophthalmological Foundation and Dr. Christine Levy-Gabriel of the Curie Institute. The subject is now of unquestionable importance and evidently of great interest to Ophthalmologists, whether they are orbital- palpebral specialists or not. Indeed, errors or delays in the diagnosis of tumor pathologies are relatively common and the consequences can be serious in the case of malignant tumors, especially carcinomas. Swift diagnosis and anatomopathological confirmation will lead to a treatment, discussed in multidisciplinary team meetings, ranging from surgery to radiotherapy.