CT Signs in the Lungs Girish S
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Pediatrics-EOR-Outline.Pdf
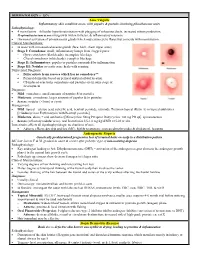
DERMATOLOGY – 15% Acne Vulgaris Inflammatory skin condition assoc. with papules & pustules involving pilosebaceous units Pathophysiology: • 4 main factors – follicular hyperkeratinization with plugging of sebaceous ducts, increased sebum production, Propionibacterium acnes overgrowth within follicles, & inflammatory response • Hormonal activation of pilosebaceous glands which may cause cyclic flares that coincide with menstruation Clinical Manifestations: • In areas with increased sebaceous glands (face, back, chest, upper arms) • Stage I: Comedones: small, inflammatory bumps from clogged pores - Open comedones (blackheads): incomplete blockage - Closed comedones (whiteheads): complete blockage • Stage II: Inflammatory: papules or pustules surrounded by inflammation • Stage III: Nodular or cystic acne: heals with scarring Differential Diagnosis: • Differentiate from rosacea which has no comedones** • Perioral dermatitis based on perioral and periorbital location • CS-induced acne lacks comedones and pustules are in same stage of development Diagnosis: • Mild: comedones, small amounts of papules &/or pustules • Moderate: comedones, larger amounts of papules &/or pustules • Severe: nodular (>5mm) or cystic Management: • Mild: topical – azelaic acid, salicylic acid, benzoyl peroxide, retinoids, Tretinoin topical (Retin A) or topical antibiotics [Clindamycin or Erythromycin with Benzoyl peroxide] • Moderate: above + oral antibiotics [Minocycline 50mg PO qd or Doxycycline 100 mg PO qd], spironolactone • Severe (refractory nodular acne): oral -

CHEST RADIOLOGY: Goals and Objectives
Harlem Hospital Center Department of Radiology Residency Training Program CHEST RADIOLOGY: Goals and Objectives ROTATION 1 (Radiology Years 1): Resident responsibilities: • ED chest CTs • Inpatient and outpatient plain films including the portable intensive care unit radiographs • Consultations with referring clinicians MEDICAL KNOWLEDGE: • Residents must demonstrate knowledge about established and evolving biomedical, clinical, and cognitive sciences and the application of this knowledge to patient care. At the end of the rotation, the resident should be able to: • Identify normal radiographic and CT anatomy of the chest • Identify and describe common variants of normal, including aging changes. • Demonstrate a basic knowledge of radiographic interpretation of atelectasis, pulmonary infection, congestive heart failure, pleural effusion and common neoplastic diseases of the chest • Identify the common radiologic manifestation of thoracic trauma, including widened mediastinum, signs of aortic laceration, pulmonary contusion/laceration, esophageal and diaphragmatic rupture. • Know the expected postoperative appearance in patients s/p thoracic surgery and the expected location of the life support and monitoring devices on chest radiographs of critically ill patients (intensive care radiology); be able to recognize malpositioned devices. • Identify cardiac enlargement and know the radiographic appearance of the dilated right vs. left atria and right vs. left ventricles, and pulmonary vascular congestion • Recognize common life-threatening -

Signs in Chest Imaging
Diagn Interv Radiol 2011; 17:18–29 CHEST IMAGING © Turkish Society of Radiology 2011 PICTORIAL ESSAY Signs in chest imaging Oktay Algın, Gökhan Gökalp, Uğur Topal ABSTRACT adiological practice includes classification of illnesses with similar A radiological sign can sometimes resemble a particular object characteristics through recognizable signs. Knowledge of and abil- or pattern and is often highly suggestive of a group of similar pathologies. Awareness of such similarities can shorten the dif- R ity to recognize these signs can aid the physician in shortening ferential diagnosis list. Many such signs have been described the differential diagnosis list and deciding on the ultimate diagnosis for for X-ray and computed tomography (CT) images. In this ar- ticle, we present the most frequently encountered plain film a patient. In this report, 23 important and frequently seen radiological and CT signs in chest imaging. These signs include for plain signs are presented and described using chest X-rays, computed tomog- films the air bronchogram sign, silhouette sign, deep sulcus raphy (CT) images, illustrations and photographs. sign, Continuous diaphragm sign, air crescent (“meniscus”) sign, Golden S sign, cervicothoracic sign, Luftsichel sign, scim- itar sign, doughnut sign, Hampton hump sign, Westermark Plain films sign, and juxtaphrenic peak sign, and for CT the gloved finger Air bronchogram sign sign, CT halo sign, signet ring sign, comet tail sign, CT an- giogram sign, crazy paving pattern, tree-in-bud sign, feeding Bronchi, which are not normally seen, become visible as a result of vessel sign, split pleura sign, and reversed halo sign. opacification of the lung parenchyma. -

Imaging Findings of Paragonimus Westermani
+ MODEL HOSTED BY Available online at www.sciencedirect.com ScienceDirect Radiology of Infectious Diseases xx (2016) 1e8 www.elsevier.com/locate/jrid Research article Imaging findings of Paragonimus westermani Shambhu Kumar Sah a, Silin Du a, Yi Liu a, Ping Yin a, Oormila Ganganah b, Manu Chiniah c, Pranesh Kumar Yadav d, You You Guo a, Yongmei Li a,* a Department of Radiology, The First Affiliated Hospital of Chongqing Medical University, No. 1 Youyi Road, Yuzhong District, Chongqing 400016, China b Department of Respiratory Medicine, The First Affiliated Hospital of Chongqing Medical University, No. 1 Youyi Road, Yuzhong District, Chongqing 400016, China c Department of General Surgery, The First Affiliated Hospital of Chongqing Medical University, No. 1 Youyi Road, Yuzhong District, Chongqing 400016, China d Department of Orthopedics, The Second Affiliated Hospital of Chongqing Medical University, Yuzhong District, Chongqing 400016, China Received 21 January 2016; revised 22 January 2016; accepted 22 January 2016 Available online ▪▪▪ Abstract Purpose: To analyze the imaging findings of pulmonary and extra-pulmonary paragonimiasis. Methods: The imaging findings of serologically and clinically confirmed 22 cases of Paragonimus westermani infection identified over a five- year period (2010e2015) were retrospectively analyzed. Chest CT (n ¼ 22), brain CT (n ¼ 2) & MRI (n ¼ 1), abdomen CT (n ¼ 3) scans were available. Results: Chest CT scan was abnormal in 20 patients and the CT findings were as follows: nodule (n ¼ 18), ground glass opacity (GGO) (n ¼ 12), worm cyst (n ¼ 10), migration track (n ¼ 7), fibrosis (n ¼ 5), pleural effusion (n ¼ 15), pleural thickening (n ¼ 10), pleural calcification (n ¼ 1). Hilar or mediastinal lymphadenopathy was noted in three patients. -

Abdominal X-Ray Radiological Signs
Abdominal X-ray Radiological Signs Suzanne O’Hagan Lightbulb moment a moment of sudden inspiration, revelation, or recognition Approach to AXR • Bowel gas pattern • Extraluminal air • Soft tissue masses • Calcifications Normal AXR Liver Gas in stomach Splenic flexure 11th rib T12 Psoas margin Left kidney Hepatic flexure Transverse colon Iliac crest Gas in sigmoid Sacrum Gas in caecum SI joint Bladder Femoral head Gas pattern What is normal? • Stomach – Almost always air in stomach • Small bowel – Usually small amount of air in 2 or 3 loops • Large bowel – Almost always air in rectum and sigmoid – Varying amount of gas in rest of large bowel Normal fluid levels • Stomach – Always (upright, decub) • Small bowel – Two or three levels acceptable (upright, decub) • Large bowel – None normally (functions to remove fluid) Large vs small bowel • Large bowel – Peripheral (except RUQ occupied by liver) – Haustral markings don’t extend from wall to wall • Small bowel – Central – Valvulae conniventes extend across lumen and are spaced closer together Radiographic principles Series of films for acute abdomen • Obstruction series/ Acute abdominal series/ Complete abdominal series – Supine (almost always) – Upright or left decubitus (almost always) – Prone or lateral rectum (variable) – Chest, upright or supine (variable) Acute abdominal series What to look for VIEW LOOK FOR SUPINE ABDOMEN Bowel gas pattern Calcifications Masses PRONE ABDOMEN Gas in rectosigmoid Gas in ascending and descending colon UPRIGHT ABDOMEN Free air, air-fluid levels UPRIGHT -

CT Halo Sign: the Spectrum of Pulmonary Diseases
The British Journal of Radiology, 78 (2005), 862–865 E 2005 The British Institute of Radiology DOI: 10.1259/bjr/77712845 Pictorial review CT halo sign: the spectrum of pulmonary diseases Y R LEE, MD, Y W CHOI, MD, K J LEE, MD, S C JEON, MD, C K PARK, MD and J-N HEO, MD Department of Diagnostic Radiology, College of Medicine, Hanyang University, 17 Haengdang-dong, Sungdong-gu, Seoul 133-792, Korea Abstract. The CT halo sign indicates ground glass attenuation surrounding a pulmonary nodule on CT. Although it was initially proposed as an early, specific finding of invasive pulmonary aspergillosis, it can be caused by many other pathological conditions such as infection, neoplastic and inflammatory diseases. The halo of ground glass attenuation pathologically represents pulmonary haemorrhage, tumour infiltration, or non- haemorrhagic inflammatory processes. Although non-specific, this sign is important because the clinical setting and associated radiological features may give a clue to the differential diagnosis. In this review, we demonstrate the spectrum of pulmonary diseases showing the ‘‘CT halo sign’’ on thin-section CT and discuss their radiological and clinical features. The CT halo sign, also known as the halo sign, indicates 1–3 cm nodules (the CT halo sign). Later, the nodules can ground glass attenuation surrounding a pulmonary nodule enlarge and eventually may demonstrate cavitation with an on thin-section CT. This appearance was first described in air crescent sign, a finding that occurs during granulocyte immunocompromised patients with invasive pulmonary recovery. The frequency of the halo sign in patients with aspergillosis [1]. Besides infectious conditions such as invasive pulmonary aspergillosis is relatively high in the aspergillosis, many neoplastic and inflammatory processes early stages of the disease, but becomes progressively less may also cause the halo sign (Table 1) [1–7]. -

All the Faces of Aspergillosis
All the faces of Aspergillosis. T. González de la Huebra Labrador1, D. García Casado2, A. 1 Garrote Pascual1, P.A. Chaparro García , A. Herrero Hernández1; 1Salamanca (España), 2Segovia (España). ECR 2014 Learning objectives To describe the different forms of pulmonary aspergillosis and its radiologic findings at chest radiography, conventional computed tomography (CT) and high-resolution CT (HRCT). Background Aspergillosis is a mycotic disease caused by Aspergillus organisms and is frequently seen in immunocompromised patients. Aspergillus fumigatus is by far the most common pathogen in humans. There is a wide spectrum of pulmonary aspergillosis, ranging from simple colonization to life-threatening invasive form, depending on the immunologic status of the host, individual susceptibility, or preexisting lung disease. Pulmonary aspergillosis is traditionally subdivided into three categories: mycetoma, invasive aspergillosis, and allergic bronchopulmonary aspergillosis (ABPA). However, we should know that these entities may overlap in an individual patient. Findings and procedure details ASPERGILLOMA or MYCETOMA: The aspergilloma, mycetoma, or fungus ball is a conglomeration of fungal hyphae of Aspergillus that typically colonize preexisting chronic cavities in the lung which are often due to sarcoidosis or previous tuberculosis Fig. 1. However, cavities from other causes, including bronchiectasis, pulmonary neoplasms, emphysema Fig. 2 or cystic congenital lesions, may also be colonized. Patients may remain asymptomatic, but hemoptysis is the most common clinical manifestation. Mycetomas are seen as a rounded mass of soft-tissue density within a lung cavity, found most often in the upper lobes Fig. 1 Fig. 2 or in the superior segments of the lower lobes. CT usually shows a characteristic spongelike appearance (a mass with irregular airspaces) Fig. -

Chest Imaging Using Signs, Symbols, and Naturalistic Images
Chiarenza et al. Insights into Imaging (2019) 10:114 https://doi.org/10.1186/s13244-019-0789-4 Insights into Imaging EDUCATIONAL REVIEW Open Access Chest imaging using signs, symbols, and naturalistic images: a practical guide for radiologists and non-radiologists Alessandra Chiarenza1, Luca Esposto Ultimo1, Daniele Falsaperla1, Mario Travali1, Pietro Valerio Foti1, Sebastiano Emanuele Torrisi2,3, Matteo Schisano2, Letizia Antonella Mauro1, Gianluca Sambataro2,4, Antonio Basile1, Carlo Vancheri2 and Stefano Palmucci1* Abstract Several imaging findings of thoracic diseases have been referred—on chest radiographs or CT scans—to signs, symbols, or naturalistic images. Most of these imaging findings include the air bronchogram sign, the air crescent sign, the arcade-like sign, the atoll sign, the cheerios sign, the crazy paving appearance, the comet-tail sign, the darkus bronchus sign, the doughnut sign, the pattern of eggshell calcifications, the feeding vessel sign, the finger- in-gloove sign, the galaxy sign, the ginkgo leaf sign, the Golden-S sign, the halo sign, the headcheese sign, the honeycombing appearance, the interface sign, the knuckle sign, the monod sign, the mosaic attenuation, the Oreo- cookie sign, the polo-mint sign, the presence of popcorn calcifications, the positive bronchus sign, the railway track appearance, the scimitar sign, the signet ring sign, the snowstorm sign, the sunburst sign, the tree-in-bud distribution, and the tram truck line appearance. These associations are very helpful for radiologists and non-radiologists and increase learning and assimilation of concepts. Therefore, the aim of this pictorial review is to highlight the main thoracic imaging findings that may be associated with signs, symbols, or naturalistic images: an “iconographic” glossary of terms used for thoracic imaging is reproduced— placing side by side radiological features and naturalistic figures, symbols, and schematic drawings. -

An Unusual Disease with an Interesting Sign
Andreas Afthinos1, Emmanouil Antonakis1, Maria Horti2, Eleftherios Markatis1, Konstantinos Pagratis1, Ilias C. Papanikolaou1 [email protected] Case report An unusual disease with an interesting sign Case report Cite as: Afthinos A, Antonakis E, Horti M, et al. An unusual disease with an interesting A 78-year-old male presented at the emergency sign. Breathe 2020; 16: room complaining of dry cough, fever up to 38.5 °C 190302. and malaise for 1 month. He had visited a general practitioner and received amoxicillin 500 mg three times a day for 7 days for a presumed chest infection, without improvement. He had a history of diabetes and arterial blood hypertension, for which he was receiving metformin 1000 mg twice a day and amlodipine 10 mg a day for 7 years. He reported no alcohol abuse and was an ex-smoker of 20 pack-years (quit 30 years ago). He had no recent hospitalisations or any medical interventions. Physical examination revealed a patient who was febrile (37.8 °C) and in a mildly lethargic condition; however, he was fully orientated. Arterial blood pressure was 115/75 mmHg, heart Figure 1 Chest radiography showing pulmonary infil- rate was 85 beats·min−1, respiratory rate was 20 trates with air bronchogram in mid- and lower-lung fields breathes·min−1 and oxygen saturation was 92%. bilaterally. Arterial blood gases showed partial oxygen pressure 67 mmHg, CO2 32 mmHg and pH 7.43. He had diffuse crackles over mid- and lower-lung fields Task 1 bilaterally. Laboratory tests revealed elevated white What is your differential diagnosis? blood cell counts (12 800 cells per μL) of neutrophilic a) Community-acquired pneumonia type (78%), erythrocyte sedimentation rate b) Aspiration pneumonia 85 mm·h−1and C-reactive protein 8 mg·dL−1. -

Crisis Guide Otolaryngology
Crisis Guide Otolaryngology Editors: Jodi D. Zuckerman, M.D. G. Aaron Rogers, M.D. 1 Table of contents Table Table of contents About this Text 4 About the Authors 5 Introduction 6 I: Common ENT Infections Section I: Common ENT Infections 8 Acute Otitis Media & Mastoiditis – Oswaldo Henriquez, M.D. 8-9 Necrotizing Otitis Externa – Ajani Nugent, M.D. 10-11 Complications of Acute Sinusitis – Praveen Duggal, M.D. 12-13 Invasive Fungal Sinusitis – Anita Sethna, M.D. 14-15 Acute Tonsillitis and Peritonsillar Absess – Elina Kari, M.D. 16-17 Epiglottitis & Supraglottitis – Jodi D. Zuckerman, M.D. 18 Retro- & Parapharyngeal Infections – Frederick Durden, M.D. 19 II: Trauma Ludwig’s Angina – Eric Berg, M.D. 21-22 Deep Space Neck Infections – Elina Kari, M.D. 23-24 Section II: Trauma 26 Nasal Septal Hematoma – Avani Ingley, M.D. 26-27 Auricular Hematoma – Adrienne Laury, M.D. 28-29 III: Operative Complications Mandibular Fractures – Eric Berg, M.D. 30-31 Orbital Floor Fractures – Casey Mathison, M.D. 32-33 Frontal Bone Fractures – Lindsey Arviso, M.D. 34-35 Temporal Bone Fractures – Grace Leu, M.D. and Aaron Rogers, M.D. 36-37 Blunt Laryngeal Trauma – Aaron Rogers, M.D. 38-39 Penetrating Neck Injury – Shatul Parikh, M.D. and Jodi D. Zuckerman, M.D. 40-41 IV: Miscellany IV: Crisis guide: Otolaryngology Table of contents 2 Table of contents Table I: Common ENT Infections Section III: Operative Complications 42 Post-Tonsillectomy Hemorrhage – Clyde Mathison, M.D. 42-43 Carotid Blowout – Ajani Nugent, M.D. 38 44-45 Tracheostomy Bleeding – Iman Naseri, M.D. -

Southwest Journal of Pulmonary and Critical Care/2017/Volume 14 104 March 2017 Imaging Case of the Month Courtney M. Tomblinson
March 2017 Imaging Case of the Month Courtney M. Tomblinson, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 69-year-old man presented with long-standing complaints of dyspnea, progressing to dyspnea at rest, associated with some dysphagia to solids. He also noted symptoms consistent with exertional stertor (a respiratory sound characterized by heavy snoring or gasping). His past medical history was remarkable only for hypertension controlled with medication. Laboratory data, include white blood cell count, coagulation profile, and serum chemistries were within normal limits. Oxygen saturation on room air was normal. Frontal chest radiography (Figure 1) was performed. Figure 1: Frontal chest radiography. Which of the following statements regarding the chest radiograph is most accurate? 1. Frontal chest radiography shows a cavitary lung mass 2. Frontal chest radiography shows an abnormal mediastinal contour 3. Frontal chest radiography shows multiple small nodules 4. Frontal chest radiography shows peribronchial and mediastinal lymphadenopathy 5. Frontal chest radiography shows pleural effusion Southwest Journal of Pulmonary and Critical Care/2017/Volume 14 104 Correct! 2. Frontal chest radiography shows an abnormal mediastinal contour The frontal chest radiograph shows an abnormal contour along the left superior mediastinum- there is a convex leftward “bulge” cranial to the left heart border and left hilum (Figure 2). Figure 2. Frontal chest radiography shows an abnormal contour (arrows) along the left superior mediastinum. There are no pulmonary nodules, nor is there evidence of dependent pleural liquid. The hilar and peribronchial regions appear normal and no mediastinal lymph node enlargement is present. -

The Halo Sign
J Bras Pneumol. 2016;42(6):435-439 http://dx.doi.org/10.1590/S1806-37562016000000029 ORIGINAL ARTICLE The halo sign: HRCT findings in 85 patients Giordano Rafael Tronco Alves1, Edson Marchiori1, Klaus Irion2, Carlos Schuler Nin3, Guilherme Watte3, Alessandro Comarú Pasqualotto3, Luiz Carlos Severo3, Bruno Hochhegger1,3 1. Programa de Pós-Graduação em ABSTRACT Medicina (Radiologia), Universidade Federal do Rio de Janeiro, Rio de Objective: The halo sign consists of an area of ground-glass opacity surrounding Janeiro (RJ) Brasil. pulmonary lesions on chest CT scans. We compared immunocompetent and 2. Radiology Department, Liverpool Heart immunosuppressed patients in terms of halo sign features and sought to identify those and Chest Hospital, Liverpool, United of greatest diagnostic value. Methods: This was a retrospective study of CT scans Kingdom. performed at any of seven centers between January of 2011 and May of 2015. Patients 3. Universidade Federal de Ciências da Saúde de Porto Alegre, Porto Alegre were classified according to their immune status. Two thoracic radiologists reviewed the (RS) Brasil. scans in order to determine the number of lesions, as well as their distribution, size, and contour, together with halo thickness and any other associated findings.Results: Of the Submitted: 28 February 2016. 85 patients evaluated, 53 were immunocompetent and 32 were immunosuppressed. Of Accepted: 21 July 2016. the 53 immunocompetent patients, 34 (64%) were diagnosed with primary neoplasm. Of Study carried out at the Irmandade da the 32 immunosuppressed patients, 25 (78%) were diagnosed with aspergillosis. Multiple Santa Casa de Misericórdia de Porto and randomly distributed lesions were more common in the immunosuppressed patients Alegre, Porto Alegre (RS) Brasil.