Abdominal X-Ray Radiological Signs
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Perforated Ulcers Shaleen Sathe, MS4 Christina Lebedis, MD CASE HISTORY
Perforated Ulcers Shaleen Sathe, MS4 Christina LeBedis, MD CASE HISTORY 54-year-old male with known history of hypertension presents with 2 days of acute onset abdominal pain, nausea, vomiting, and diarrhea, with periumbilical tenderness and abdominal distention on exam, without guarding or rebound tenderness. Labs, including CBC, CMP, and lipase, were unremarkable in the emergency department. Radiograph Perforated Duodenal Ulcer Radiograph of the chest in the AP projection shows large amount of free air under diaphragm (blue arrows), suggestive of intraperitoneal hollow viscus perforation. CT Perforated Duodenal Ulcer CT of the abdomen in the axial projection (I+, O-), at the level of the inferior liver edge, shows large amount of intraperitoneal free air (blue arrows) in lung window (b), and submucosal edema in the gastric antrum and duodenal bulb (red arrows), suggestive of a diagnosis of perforated bowel, most likely in the region of the duodenum. US Perforated Gastric Ulcer US of the abdomen shows perihepatic fluid (blue arrow) and free fluid in the right paracolic gutter (not shown), concerning for intraperitoneal pathology. Radiograph Perforated Gastric Ulcer Supine radiograph of the abdomen shows multiple air- filled dilated loops of large bowel, with air lucencies on both sides of the sigmoid colon wall (green arrows), consistent with Rigler sign and perforation. CT Perforated Gastric Ulcer CT of the abdomen in the axial (a) and sagittal (b) projections (I+, O-) shows diffuse wall thickening of the gastric body and antrum (green arrows) with an ulcerating lesion along the posterior wall of the stomach (red arrows), and free air tracking adjacent to the stomach (blue arrow), concerning for gastric ulcer perforation. -
Pediatrics-EOR-Outline.Pdf
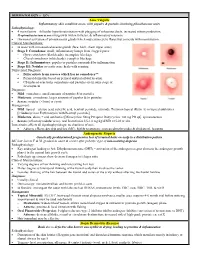
DERMATOLOGY – 15% Acne Vulgaris Inflammatory skin condition assoc. with papules & pustules involving pilosebaceous units Pathophysiology: • 4 main factors – follicular hyperkeratinization with plugging of sebaceous ducts, increased sebum production, Propionibacterium acnes overgrowth within follicles, & inflammatory response • Hormonal activation of pilosebaceous glands which may cause cyclic flares that coincide with menstruation Clinical Manifestations: • In areas with increased sebaceous glands (face, back, chest, upper arms) • Stage I: Comedones: small, inflammatory bumps from clogged pores - Open comedones (blackheads): incomplete blockage - Closed comedones (whiteheads): complete blockage • Stage II: Inflammatory: papules or pustules surrounded by inflammation • Stage III: Nodular or cystic acne: heals with scarring Differential Diagnosis: • Differentiate from rosacea which has no comedones** • Perioral dermatitis based on perioral and periorbital location • CS-induced acne lacks comedones and pustules are in same stage of development Diagnosis: • Mild: comedones, small amounts of papules &/or pustules • Moderate: comedones, larger amounts of papules &/or pustules • Severe: nodular (>5mm) or cystic Management: • Mild: topical – azelaic acid, salicylic acid, benzoyl peroxide, retinoids, Tretinoin topical (Retin A) or topical antibiotics [Clindamycin or Erythromycin with Benzoyl peroxide] • Moderate: above + oral antibiotics [Minocycline 50mg PO qd or Doxycycline 100 mg PO qd], spironolactone • Severe (refractory nodular acne): oral -

Complicated Pseudodiverticulosis of Small Intestine: a Rare Case Report
International Surgery Journal Raj MK et al. Int Surg J. 2019 Sep;6(9):3433-3437 http://www.ijsurgery.com pISSN 2349-3305 | eISSN 2349-2902 DOI: http://dx.doi.org/10.18203/2349-2902.isj20194096 Case Report Complicated pseudodiverticulosis of small intestine: a rare case report Kamal Raj M., V. Venkatachalam*, Manasa A. Institute of General Surgery, Madras Medical College, Chennai, Tamil Nadu, India Received: 08 July 2019 Revised: 16 August 2019 Accepted: 19 August 2019 *Correspondence: Dr. V. Venkatachalam, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Diverticular disease though being a common entity in large bowel is recently noted to occur more proximally as well. In the jejunum, the mucosal outpouchings, called as pseudo-diverticulae, occurs with an incidence of 0.5-1.5%. Diagnosed incidentally as majority of them remain asymptomatic. When they are symptomatic, dyspepsia and bloating, recurrent abdominal cramping, malabsorption and megaloblastic anemia occurs. On occasions it is not uncommon for patients to present with hemorrhage, infections, obstruction or perforation. Perforation, being a rare presentation occurs in less than 6% of the cases. We present a case of a 70 year old male, who presented as acute abdomen, found to have isolated jejunal diverticular perforation intraoperatively. Keywords: Jejunal diverticula, Perforation, Acute abdomen, Pseudo-diverticulae INTRODUCTION for 2 days. He also gave history of dyspepsia and bloating following food consumption. -

Postpartum Pneumoperitoneum and Peritonitis After Water Birth Brown Et Al
Gastrointestinal Radiology: Postpartum pneumoperitoneum and peritonitis after water birth Brown et al. Postpartum pneumoperitoneum and peritonitis after water birth Vanessa Brown 1, Sascha Dua 1*, Anna Athow 1, Rudi Borgstein 1, Oladapo Fafemi 1 1. Department of General Surgery, North Middlesex University Hospital Trust, London, UK * Correspondence: Miss Sascha Dua, 18 Eton Rise, Eton College Road, London, NW3 2DD, UK ( [email protected] ) Radiology Case. 2009 Apr; 3(4): 1-4 :: DOI: 10.3941/jrcr.v3i4.12 ABSTRACT Pneumoperitoneum (the presence of free gas in the peritoneal cavity) usually indicates gastrointestinal perforation with associated peritoneal contamination. We describe the unusual case of a 28-year-old female, who was 7 days postpartum and presented with features of peritonitis that were www.RadiologyCases.com www.RadiologyCases.com initially missed despite supporting radiological evidence. The causes of pneumoperitoneum are discussed. In the postpartum period the female genital tract provides an alternative route by which gas can enter the abdominal cavity and cause pneumoperitoneum. In the postpartum period it is important to remember that the clinical signs of peritonism, guarding and rebound tenderness may be diminished or subtle due to abdominal wall laxity. CASE REPORT Journalof Radiology Case Reports was performed (Fig. 1) and the patient referred to the CASE REPORT gynaecologist who requested an ultrasound of the abdomen A 28-year-old woman presented to the emergency department and pelvis to rule out retained products of conception (Fig. 2). with a two-day history of generalised abdominal pain. She had The ultrasound showed a bulky uterus with a small amount of given birth to her first child three days previously at home. -

CT Signs in the Lungs Girish S
CT Signs in the Lungs Girish S. Shroff, MD,* Edith M. Marom, MD,† Myrna C.B. Godoy, MD, PhD,* Mylene T. Truong, MD,* and Caroline Chiles, MDz Radiologic signs are often based on items or patterns that are encountered in everyday life. They are especially useful because their observation allows the differential diagnosis to be narrowed, and in some cases, enables a diagnosis to be made. In this review, several clas- sic and newer computed tomography signs in the lungs are discussed. Semin Ultrasound CT MRI 40:265-274 © 2018 Elsevier Inc. All rights reserved. Introduction should be considered when the pipe cleaner sign is seen (Fig. 2). Nodule distribution varies slightly among the con- adiologic signs are often based on items or patterns that ditions—in sarcoidosis, nodules tend to predominate along R are encountered in everyday life. They are especially use- larger bronchovascular bundles and in the subpleural ful because their observation allows the differential diagnosis regions whereas in silicosis and coal worker’s pneumoconi- to be narrowed, and in some cases, enables a diagnosis to be osis, nodules tend to predominate in the centrilobular and made. Furthermore, early recognition of signs associated subpleural regions.2 Smooth or nodular interlobular septal with aggressive infections may be life-saving. In this review, thickening is usually the dominant feature in lymphangitic the following computed tomography (CT) signs in the lungs carcinomatosis. Interlobular septal thickening is typically will be discussed: pipe cleaner, halo, reversed halo, air cres- absent in granulomatous diseases such as sarcoidosis and cent, Monod, Cheerio, straight edge, air bronchogram, tree- silicosis. -

Signs in Chest Imaging
Diagn Interv Radiol 2011; 17:18–29 CHEST IMAGING © Turkish Society of Radiology 2011 PICTORIAL ESSAY Signs in chest imaging Oktay Algın, Gökhan Gökalp, Uğur Topal ABSTRACT adiological practice includes classification of illnesses with similar A radiological sign can sometimes resemble a particular object characteristics through recognizable signs. Knowledge of and abil- or pattern and is often highly suggestive of a group of similar pathologies. Awareness of such similarities can shorten the dif- R ity to recognize these signs can aid the physician in shortening ferential diagnosis list. Many such signs have been described the differential diagnosis list and deciding on the ultimate diagnosis for for X-ray and computed tomography (CT) images. In this ar- ticle, we present the most frequently encountered plain film a patient. In this report, 23 important and frequently seen radiological and CT signs in chest imaging. These signs include for plain signs are presented and described using chest X-rays, computed tomog- films the air bronchogram sign, silhouette sign, deep sulcus raphy (CT) images, illustrations and photographs. sign, Continuous diaphragm sign, air crescent (“meniscus”) sign, Golden S sign, cervicothoracic sign, Luftsichel sign, scim- itar sign, doughnut sign, Hampton hump sign, Westermark Plain films sign, and juxtaphrenic peak sign, and for CT the gloved finger Air bronchogram sign sign, CT halo sign, signet ring sign, comet tail sign, CT an- giogram sign, crazy paving pattern, tree-in-bud sign, feeding Bronchi, which are not normally seen, become visible as a result of vessel sign, split pleura sign, and reversed halo sign. opacification of the lung parenchyma. -

Acute Abdomen
Acute abdomen CASE 1: 46Y♀VOMITING 新光吳火獅紀念醫院 VS 許瓅文 103.09.09 46Y♀vomiting • Chief complaint •Past Hx – Abdominal pain, vomiting and no appetite for 2 – Ectopic pregnancy s/p OP 20yrs ago days – Pregnancy: denied • Present illness •PE – Intermittent abdominal pain – Abdomen: – Abdominal distention(+) diffuse tender(+) – Vomitus: yellowish/ greenish fluid no rebound pain – No flatus bowel sound: hypoactive – Similar episode before percussion: tympanic Impression?/ Order KUB (EIA: negative) • CBD/DC/Plt Hx • Standing abdomen • Panel Ⅰ/ T-bil/ Lipase Site of tender • PT/aPTT OP? •KUB (待EIA) Anticoagulant use? • Urine EIA •NPO • D5S run 60mL/hr Adhesion ileus Order Clinical feature •2nd KUB: ileus improved •2nd KUB: fixed bowel loop • Flatus(+), abdominal • Fever(+) • Promeran 1amp iv q6h & st Severe distension pain and distension vomiting • Persisted abd.pain • On NG with decompression improved • Rebound pain(+) • D5S run 120mL/hr Try water and soft diet Fluid resuscitation • NG decompression: 量多, • 排GI床/ 待轉EC Dry mouth/ UOP No discomfort greenish AKI? Prerenal azotemia? • f/u KUB 8hrs later MBD =>what’s next? Order Ileus • Abdominal CT with/without contrast • Abd OP Hx + ileus ≒ adhesion ileus =>empiric • B/C xⅡ Tx Bowel obstruction: • Be ware of mechanical bowel obstruction!!! • Cefmetazole 1g iv q8h & st bezoar => OP => CT indication/ OP indicated • Be ware of medication ↓ bowel motility for Abd OP Hx Pt Terminal ileitis 78y♂ Abdominal pain • Chief complaint – Abdominal pain since 6 hrs ago • Present illness – 看護:一陣一陣喊肚子痛 – Vomiting once, food content CASE 2: 78Y♂ ABDOMINAL PAIN – Diarrhea for 2 times, watery, brownish/ yellowish – No fever •Past Hx – Old CVA with bed-ridden/ DM/ HTN/ CAD Hx Impression?/ Order – Abd OP Hx: nil •NPO • PE: • D5S run 60mL/hr – Chest: clear BS, IRHB • CBD/DC/Plt – Abdomen: soft, no tender point •F/S DKA? no rebound pain • VBG G6 檢查項目避免重複開立 – Ext: warm, no pitting edema • Cr, AST, lipase, T-bil •KUB •ECG Previous ECG: Af OPD drug: warfarin 3mg qd • PT/aPTT Lab data/ Image Impression?/ Order • WBC: 22000/ seg. -
![Pdf Talk [Compatibility Mode]](https://docslib.b-cdn.net/cover/4561/pdf-talk-compatibility-mode-1964561.webp)
Pdf Talk [Compatibility Mode]
13/11/55 IMAGING MODALITIES Improve reading skill of abdominal imaging • PLAIN FILM • ULTRASONOGRAPHY • BARIUM EXAMINATION ผศ นพ สิทธิพงศ ศรีสัจจากุล BODY IMAGING • CT Department of Radiology, SirirajHospital, • MRI MahidolUniversity • PET @ King ChulalongkornMemorial Hospital, 25 november12 PLAIN FILM • ACUTE ABDOMINAL SERIES -CXR upright PLAIN FILM -Plain abdomen supine and upright Density in Plain Film Plain Abdomen: Upright View 3 Liver 4 2 3 1 1 = air Properitoneal 2 = fat fat line 4 Abdominal 3 = soft tissue wall 5 4 = bone Small bowel loops 5 = metallic 1 PDF created with pdfFactory Pro trial version www.pdffactory.com 13/11/55 Plain Abdomen: Supine View Plain Abdomen vs Plain KUB Transverse Stomach colon Descending colon Supine Plain KUB PLAIN ABDOMEN How to read plain abdomen 1 Abdominal wall and properitonealfat line 2 Distance between bowel wall and abdominal Peripheral to central approach or vice versa wall 3 Gas distribution in GI tract ( stomach, small bowel and large bowel) 4 Soft tissue density in abdomen such as solid organs, fluid-filled bowel loops PLAIN ABDOMEN 5 Bony structures 6 Detection of abnormalities -Abnormal gas -free air , bowel dilatation, pneumatosis -Abnormal mass -intraperitoneumor retroperitoneum -Organomegaly -Abnormal calcification -Foreign bodies 2 PDF created with pdfFactory Pro trial version www.pdffactory.com 13/11/55 ABNORMAL PLAIN FILM CXR upright moderate to marked pneumoperitoneum Plain abdomen upright triangular sign • ICU admission • Sick patient • No upright film liver diaphragm ascites -

High Yield Points
Team Motivation FMGE/MCI Coaching Academy Radiology (FMGE Essentia - 3) HIGH YIELD POINTS RESPIRATORY SYSTEM – SIGNS SIGN / SPECIFIC FEATURE SEEN IN Meniscus / Moon/ Air crescent / Double arch sign Hydatid cyst of lung Cumbo sign Water lilly / Camalotte sign Serpent sign / Rising sun sign Empty cyst sign Popcorn calcification Hamartoma Mediastinal nodes of histoplasmosis Westermark sign Pulmonary thrombo-embolism Hapton’s hump Palla sign Fleishner lines Felson’s sign Sail sign Thymic enlargement Mulvay Wave sign Notch sign Comet tail sign Rounded atelectasis Golden S sign RUL collapse secondary to a central mass Luftsichel sign LUL collapse Broncholobar sign LLL collapse Ring around artery sign Pneumo-mediastinum Continuous diaphragm sign Tubular artery sign Double bronchial wall sign V sign of Naclerio Spinnaker sail sign Deep sulcus sign Pneumothorax Visceral pleural line Thumb sign Epiglottitis Steeple sign Croup Air crescent sign Aspergilloma Monod sign Bulging fissure sign Klebsiella pneumonia Batwing sign Pulmonary edema on CXR Collar sign Diaphragmatic rupture Dependant viscera sign Feeding vessel sign Pulmonary septic emboli Finger in glove sign ABPA Halo sign Aspergillosis Head cheese sign Subacute hypersensitivity pneumonitis Juxtaphrenic peak sign RUL atelectasis Reversed halo sign Cryptogenic organized pneumonia Saber sheath trachea COPD Sandstorm lungs Alveolar microlithiasis Signet ring sign Bronchiectasis Superior triangle sign RLL atelectasis Split pleura sign Empyema Tree in bud sign on HRCT Endobronchial spread in TB -

Perforated Duodenal Diverticulum with Subtle Pneumoretroperitoneum on Abdominal X-Ray
Hindawi Case Reports in Emergency Medicine Volume 2017, Article ID 7089573, 4 pages https://doi.org/10.1155/2017/7089573 Case Report Perforated Duodenal Diverticulum with Subtle Pneumoretroperitoneum on Abdominal X-Ray Yuzeng Shen and Mark Kwok Fai Leong Department of Emergency Medicine, Singapore General Hospital, Singapore Correspondence should be addressed to Yuzeng Shen; [email protected] Received 18 May 2017; Revised 25 August 2017; Accepted 17 September 2017; Published 19 October 2017 Academic Editor: Kalpesh Jani Copyright © 2017 Yuzeng Shen and Mark Kwok Fai Leong. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Abdominal pain is one of the most common presenting complaints at the Emergency Department (ED). Given the myriad of possible differential diagnoses for abdominal pain, it becomes more important to diagnose conditions requiring emergent surgical intervention early. We present a case of an elderly male patient with abdominal pain secondary to perforated hollow viscus, subtle evidence of pneumoretroperitoneum on the initial supine abdominal X-ray, and review the signs of pneumoperitoneum and pneumoretroperitoneum on plain abdominal X-rays. 1. Introduction constipation, and vomiting episode may have been associated with consumption of tramadol tablets. There were no prior Perforated hollow viscus may result in pneumoperitoneum episodes of similar symptoms and no identified relieving or pneumoretroperitoneum, depending on the location of factors. He did not have any other associated symptoms perforation along the gastrointestinal tract [1, 2], and may such as fever, change in bowel habits, or history suggesting lead to significant mortality and morbidity. -

Imaging of Abnormal Air in the Abdomen and Pelvis
Published online: 2019-07-19 THIEME Review Article 87 Imaging of Abnormal Air in the Abdomen and Pelvis Shobhit Sharma1 Jonathan McDougal2 Tarun Pandey1 Kedar Jambhekar1 Roopa Ram1 1Department of Radiology, University of Arkansas for Medical Address for correspondence Roopa Ram, MD, Department of Sciences, Little Rock, Arkansas, United States Radiology, University of Arkansas for Medical Sciences, Slot 556, 2Department of Radiology, University of Kansas Medical Center, 4301, West Markham Street, Little Rock, AR 72205, United States Kansas City, Missouri, United States (e-mail: [email protected]). J Gastrointestinal Abdominal Radiol ISGAR 2019;2:87–97 Abstract The presence of abnormal air collection on an imaging study is quite often the reason as well as the solution to a diagnostic dilemma. The purpose of this review article is to Keywords develop an understanding of anatomical localization and determine etiology of abnor- ► air mal air collections in the abdomen and pelvis. Abnormal air collections are commonly ► pneumomediastinum encountered on imaging studies on a daily basis, and this article will help familiarize ► pneumoperitoneum the interpreting radiologist with the pathophysiology of these collections and help ► pneumothorax solve various diagnostic challenges and avoid potential pitfalls. Introduction by dissecting along the vascular sheaths.1 It can extend into the retroperitoneal space via postesophageal areolar The presence of abnormal air collection on an imaging study tissue or aortic hiatus.2 Retroperitoneal air under tension is quite often the reason as well as the solution to a diagnos- can breach parietal peritoneum and thus can present as tic dilemma. The purpose of this review article is to develop intraperitoneal free air.3 Similarly, intraperitoneal and an understanding of anatomical localization and determine retroperitoneal air can extend into the mediastinum. -

All the Faces of Aspergillosis
All the faces of Aspergillosis. T. González de la Huebra Labrador1, D. García Casado2, A. 1 Garrote Pascual1, P.A. Chaparro García , A. Herrero Hernández1; 1Salamanca (España), 2Segovia (España). ECR 2014 Learning objectives To describe the different forms of pulmonary aspergillosis and its radiologic findings at chest radiography, conventional computed tomography (CT) and high-resolution CT (HRCT). Background Aspergillosis is a mycotic disease caused by Aspergillus organisms and is frequently seen in immunocompromised patients. Aspergillus fumigatus is by far the most common pathogen in humans. There is a wide spectrum of pulmonary aspergillosis, ranging from simple colonization to life-threatening invasive form, depending on the immunologic status of the host, individual susceptibility, or preexisting lung disease. Pulmonary aspergillosis is traditionally subdivided into three categories: mycetoma, invasive aspergillosis, and allergic bronchopulmonary aspergillosis (ABPA). However, we should know that these entities may overlap in an individual patient. Findings and procedure details ASPERGILLOMA or MYCETOMA: The aspergilloma, mycetoma, or fungus ball is a conglomeration of fungal hyphae of Aspergillus that typically colonize preexisting chronic cavities in the lung which are often due to sarcoidosis or previous tuberculosis Fig. 1. However, cavities from other causes, including bronchiectasis, pulmonary neoplasms, emphysema Fig. 2 or cystic congenital lesions, may also be colonized. Patients may remain asymptomatic, but hemoptysis is the most common clinical manifestation. Mycetomas are seen as a rounded mass of soft-tissue density within a lung cavity, found most often in the upper lobes Fig. 1 Fig. 2 or in the superior segments of the lower lobes. CT usually shows a characteristic spongelike appearance (a mass with irregular airspaces) Fig.