Automated External Defibrillat
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Incidence of Post Cross Clamp Ventricular Fibrillation in Isolated Coronary Artery Bypass Surgery Using Del Nido Cardioplegia and Conventional Blood Cardioplegia
Jemds.com Original Research Article Incidence of Post Cross Clamp Ventricular Fibrillation in Isolated Coronary Artery Bypass Surgery Using del Nido Cardioplegia and Conventional Blood Cardioplegia Biju Kambil Thyagarajan1, Anandakuttan Sreenivasan2, Ravikrishnan Jayakumar3, Ratish Radhakrishnan4 1, 2, 3, 4 Department of Cardiovascular and Thoracic Surgery, Government T D Medical College, Alappuzha, Kerala, India. ABSTRACT BACKGROUND The cardiac surgical procedures and surgical outcomes witnessed a dramatic Corresponding Author: improvement with the introduction of cardiopulmonary bypass and cardioplegia Dr. Anandakuttan Sreenivasan, techniques. Ventricular fibrillation immediately after removal of aortic cross clamp is Department of Cardiovascular and an energy consuming process leading to myocardial injury in an already energy Thoracic Surgery, Government T D Medical College, Alappuzha, Kerala, India, depleted heart. Electrical cardioversion, which itself causes myocardial injury, is E-mail: [email protected] required to regain normal rhythm. Prevention of ventricular fibrillation is important in preventing myocardial injury. We retrospectively analysed the incidence of post DOI: 10.14260/jemds/2020/797 cross clamp ventricular fibrillation requiring electrical defibrillation in isolated coronary artery bypass surgery using del Nido cardioplegia and conventional blood How to Cite This Article: cardioplegia. Thyagarajan BK, Sreenivasan A, Jayakumar R, et al. Incidence of post cross clamp METHODS ventricular fibrillation in isolated coronary -

Public Access Defibrillation/AED Program Implementation Guide
Public Access Defibrillation/AED Program Implementation Guide There are 4 key elements to establishing a Public Access Defibrillation program. These include: Having designated rescuers trained in CPR and in how to use an automated external defibrillator (AED) Having a physician to provide medical oversight and direction Integrating your program with the local emergency medical services (EMS) system Using and maintaining the AED(s) according to the manufacturers specifications Steps: 1. Gain consensus Within your company or organization begin to identify the key decision makers and arrange a meeting to gain support. The American Heart Association or your local EMS Agency can assist you with presentation materials. 2. Review the law and regulations Review Federal, State and local laws and regulations regarding Public Access Defibrillation program requirements. Consult your local Emergency Medical Services (EMS) Agency The California laws ang regulations that pertain to AEDs are Title 22, and AB 658. 3. Consult your local Emergency Medical Services (EMS) Agency The local EMS Agency can provide you with information regarding training, purchasing AEDs, medical direction and laws and regulations. 4. Identify your response team Identify who would be most likely to respond in an emergency – this will help determine how and where AEDs are mounted or stored. 5. Select equipment and vendor Some considerations in selecting the AED may include: Reputation of the AED manufacturer for the product’s quality and customer service, compatibility with the equipment used in the local EMS system, and ease of operation of the AED. 6. Design Policies and Procedures These may include: Who manages the AED program When the AED should be used, when it should not be used Training required to use the AED Locations of AEDs and other equipment (such as gloves and pocket mask for CPR) Notification process for internal AED responders and external emergency medical services responders Maintenance schedule for equipment Training and refresher training policies 7. -

Delaying Defibrillation to Give Basic Cardiopulmonary Resuscitation to Patients with Out-Of-Hospital Ventricular Fibrillation a Randomized Trial
ORIGINAL CONTRIBUTION Delaying Defibrillation to Give Basic Cardiopulmonary Resuscitation to Patients With Out-of-Hospital Ventricular Fibrillation A Randomized Trial Lars Wik, MD, PhD Context Defibrillation as soon as possible is standard treatment for patients with ven- Trond Boye Hansen tricular fibrillation. A nonrandomized study indicates that after a few minutes of ven- Frode Fylling tricular fibrillation, delaying defibrillation to give cardiopulmonary resuscitation (CPR) first might improve the outcome. Thorbjørn Steen, MD Objective To determine the effects of CPR before defibrillation on outcome in pa- Per Vaagenes, MD, PhD tients with ventricular fibrillation and with response times either up to or longer than Bjørn H. Auestad, PhD 5 minutes. Design, Setting, and Patients Randomized trial of 200 patients with out-of- Petter Andreas Steen, MD, PhD hospital ventricular fibrillation in Oslo, Norway, between June 1998 and May 2001. ARLY DEFIBRILLATION IS CRITICAL Patients received either standard care with immediate defibrillation (n=96) or CPR first for survival from ventricular fi- with 3 minutes of basic CPR by ambulance personnel prior to defibrillation (n=104). If initial defibrillation was unsuccessful, the standard group received 1 minute of CPR brillation. The survival rate de- before additional defibrillation attempts compared with 3 minutes in the CPR first group. creases by 3% to 4% or 6% to E10% per minute depending on whether Main Outcome Measure Primary end point was survival to hospital discharge. Sec- ondary end points were hospital admission with return of spontaneous circulation (ROSC), basic cardiopulmonary resuscitation 1,2 1-year survival, and neurological outcome. A prespecified analysis examined sub- (CPR) is performed. -

The Refractory VF Arrest Patient: a Review of the Current Treatment
1/24/2018 The Refractory VF Arrest Patient: A Review of the Current Treatment Options Marc Conterato, MD, FACEP Office of the Medical Director North Memorial Health Ambulance Service DISCLOSURE STATEMENT • Board Member, MN Resuscitation Consortium - Images of any commercial devices or medications are for illustration purposes only. The inclusion of such images in this presentation does not imply endorsement of any specific device or company. 2 Objectives • Delineate Refractory Ventricular Fibrillation (RVF) • Recurrent VF versus Refractory VF • What is “Electrical Storm” • Current Pre-hospital treatments • Additional hospital treatments • Dual/Double Sequential Defibrillation • ECMO/ECLS-A New Hope? 3 1 1/24/2018 A Standard Scenario • 55 YOF collapses at stop light, and her car rolls into the car in front of her. Airbags do not deploy, and bystanders find her slumped over the steering wheel and pulseless. • First responder/bystanders start CPR, and deliver three AED shocks prior to EMS arrival. • On EMS arrival, a fourth shock is delivered, an IO and alternative airway placed. Automated CPR started. • Epinephrine 2 mg (total) and Amiodarone 300 mg given, and the patient remains in VF. • Patient downtime is now ~25 minutes, and repeat evaluation reveals persistent VF. 4 What are your options • Continue CPR for a total of 30 minutes with recurrent defibrillations, additional epinephrine, bicarbonate and Amiodarone? • “Load and Go” to the local hospital with CPR enroute and continuing the resuscitation? • “Load and Go” to the local CCL (Cardiac Cath Lab) hospital with CPR enroute and continuing the resuscitation, with possible PCI with ongoing CPR? • Call HEMS unit for transfer to CCL hospital, but can they continue effective CPR in the helicopter? • “Load and Go” to a ECMO/ECLS center with CPR enroute and continuing the resuscitation, on the basis they can accept the patient and continue resuscitation? 5 Defining the problem: What is recurrent versus refractory VF (RVF)? • Recurrent VF is a rhythm that terminates with cardioversion, but then recurs rapidly. -
Flecainide Considerations For
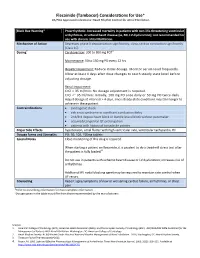
Flecainide (Tambocor) Considerations for Use* US/FDA Approved Indications: Heart Rhythm Control for Atrial Fibrillation Black Box Warning* Proarrhythmic. Increased mortality in patients with non-life-threatening ventricular arrhythmias, structural heart disease (ie, MI, LV dysfunction); not recommended for use with chronic atrial fibrillation. Mechanism of Action Depresses phase 0 depolarization significantly, slows cardiac conduction significantly (Class 1C). Dosing† Cardioversion: 200 to 300 mg PO‡1 Maintenance: 50 to 150 mg PO every 12 hrs Hepatic Impairment: Reduce initial dosage. Monitor serum level frequently. Allow at least 4 days after dose changes to reach steady state level before adjusting dosage. Renal Impairment: CrCl > 35 ml/min: No dosage adjustment is required. CrCl <= 35 ml/min: Initially, 100 mg PO once daily or 50 mg PO twice daily. Adjust dosage at intervals > 4 days, since steady-state conditions may take longer to achieve in these patient Contraindications cardiogenic shock sick sinus syndrome or significant conduction delay 2nd/3rd degree heart block or bundle brand block without pacemaker acquired/congenital QT prolongation patients with history of torsade de pointes Major Side Effects hypotension, atrial flutter with high ventricular rate, ventricular tachycardia, HF Dosage forms and Strengths PO: 50, 100, 150mg tablets Special Notes Close monitoring of this drug is required. When starting a patient on flecainide, it is prudent to do a treadmill stress test after the patient is fully loaded.4 Do not use in patients with ischemic heart disease or LV dysfunction; increases risk of arrhythmias. Additional AV nodal blocking agent may be required to maintain rate control when AF recurs. -

Discharge Advice After Atrial Fibrillation Ablation
Oxford University Hospitals NHS Trust Oxford Heart Centre Discharge advice after Atrial Fibrillation ablation Information for patients page 2 This booklet contains important advice about discharge after your Atrial Fibrillation (AF) ablation. It contains information about what to do when you get home. Contents 1. Discharge summary 4 Follow-up 4 Transport 4 2. What to do when you get home 5 Puncture site care 5 Bleeding 6 Sedation/General Anaesthetic 6 After the catheter ablation 6 Recurrence of AF symptoms - what to do 6 Driving 7 Return to work 8 3. Medication 8 4. How to contact us 9 5. Further information 10 6. Message for doctor reviewing this patient 10 page 3 1. Discharge summary Your Consultant at the John Radcliffe Hospital is: ………………………….…............................................................…….. Follow-up You will be sent an appointment for follow-up in the Arrhythmia clinic. (This appointment will be sent in the post. If you do not receive a date for an appointment within 8 weeks, please call the John Radcliffe Hospital and ask to speak to the secretary of your Consultant. Follow-up appointments are currently planned approximately 3 to 4 months after your procedure.) Transport to your outpatient appointments If you have difficulty getting to your outpatient appointments your GP surgery may have the phone numbers of voluntary transport schemes which operate at subsidised rates. A directory of these services is available at www.oxonrcc.org.uk for residents of the Oxfordshire area. page 4 2. What to do when you get home When you are discharged home, you should have a quiet few days resting to recover from your procedure. -

Resuscitation and Defibrillation
AARC GUIDELINE: RESUSCITATION AND DEFIBRILLATION AARC Clinical Practice Guideline Resuscitation and Defibrillation in the Health Care Setting— 2004 Revision & Update RAD 1.0 PROCEDURE: signs, level of consciousness, and blood gas val- Recognition of signs suggesting the possibility ues—included in those conditions are or the presence of cardiopulmonary arrest, initia- 4.1 Airway obstruction—partial or complete tion of resuscitation, and therapeutic use of de- 4.2 Acute myocardial infarction with cardio- fibrillation in adults. dynamic instability 4.3 Life-threatening dysrhythmias RAD 2.0 DESCRIPTION/DEFINITION: 4.4 Hypovolemic shock Resuscitation in the health care setting for the 4.5 Severe infections purpose of this guideline encompasses all care 4.6 Spinal cord or head injury necessary to deal with sudden and often life- 4.7 Drug overdose threatening events affecting the cardiopul- 4.8 Pulmonary edema monary system, and involves the identification, 4.9 Anaphylaxis assessment, and treatment of patients in danger 4.10 Pulmonary embolus of or in frank arrest, including the high-risk de- 4.11 Smoke inhalation livery patient. This includes (1) alerting the re- 4.12 Defibrillation is indicated when cardiac suscitation team and the managing physician; (2) arrest results in or is due to ventricular fibril- using adjunctive equipment and special tech- lation.1-5 niques for establishing, maintaining, and moni- 4.13 Pulseless ventricular tachycardia toring effective ventilation and circulation; (3) monitoring the electrocardiograph and recogniz- -

MANAGING ATRIAL FIBRILLATION (AF) (MODULE 2) MODULE 2: MANAGING ATRIAL FIBRILLATION Ii CONTENTS
YOUR COMPLETE GUIDE TO ATRIAL FIBRILLATION MANAGING ATRIAL FIBRILLATION (AF) (MODULE 2) MODULE 2: MANAGING ATRIAL FIBRILLATION ii CONTENTS iii Overview of managing AF 28 How are blood thinners used to reduce the risk of stroke in AF? 1 What are the goals of managing AF and atrial flutter? 31 What are the signs of a stroke? 2 Rate Control Strategy: 32 Being realistic when managing AF How is the heart rate controlled? (a) Medicine (b) Procedures 9 Rhythm Control Strategy: How is the heart rhythm controlled? (a) Medicine (b) Procedures 25 Reducing the risk of stroke: How is my stroke risk assessed? HEARTANDSTROKE.CA/AFGUIDE Published: February 2014 © 2014 Canadian Cardiovascular Society and Heart and Stroke Foundation of Canada. All rights reserved. Unauthorized use prohibited. MODULE 2: MANAGING ATRIAL FIBRILLATION iii OVERVIEW OF MANAGING AF AF Diagnosed MODULE 1 Find and Treat Common Causes What is it? Is it harmful? MODULE 2 Manage Arrhythmia Symptoms Assess Stroke Risk (CHADS2) Rate Control Rhythm Control • Medicine • Medicine Blood Thinner, Aspirin, or Nothing • Procedures • Procedures MODULE 3 Living Well with AF What to Expect Understanding Following a from Your AF Common Responses Patient Stories Healthy Lifestyle Management Plan and Finding Support FACT SHEET: OVERVIEW OF MANAGING AF HEARTANDSTROKE.CA/AFGUIDE Published: February 2014 © 2014 Canadian Cardiovascular Society and Heart and Stroke Foundation of Canada. All rights reserved. Unauthorized use prohibited. MODULE 2: MANAGING ATRIAL FIBRILLATION iv WHAT ARE TWO WAYS TO MANAGE AF? While AF is a chronic condition, it can be managed by: • medicine • procedures Medicine is usually tried first to manage symptoms caused by AF. -

The Transthoracic Impedance Cardiogram Is a Potential Haemodynamic Sensor for an Automated External Defibrillator
European Heart Journal (1998) 19, 1879–1888 Article No. hj981199 The transthoracic impedance cardiogram is a potential haemodynamic sensor for an automated external defibrillator P. W. Johnston*, Z. Imam†, G. Dempsey†, J. Anderson† and A. A. J. Adgey *Regional Medical Cardiology Centre, Royal Victoria Hospital, Belfast; †Northern Ireland Bioengineering Centre, Belfast, Northern Ireland Aims The American Heart Association has endorsed the agonal rhythm (20), electromechanical dissociation (22), concept of Public Access Defibrillation. However, there ventricular tachycardia (27) and sinus rhythm (5). These have been reports of inappropriate direct current shocks rhythms were divided into those associated with haemo- from automatic external defibrillators. The specificity of dynamic collapse i.e. no pulse — asystole, ventricular fibril- automatic external defibrillators for shockable rhythms lation, agonal rhythm, electromechanical dissociation and may be improved by the incorporation of a haemodynamic shockable ventricular tachycardia (associated with loss of sensor. consciousness, pulselessness or a systolic blood pressure of <80 mmHg) (Group 1) and those associated with a satis- Methods and Results This study examined the use of four factory cardiac output i.e. non-shockable ventricular tachy- parameters extracted from the impedance cardiogram i.e. cardia (conscious with a pulse) and sinus rhythm (Group 2). Peak dz/dt (the peak of the impedance cardiogram On univariate analysis each of the four impedance cardio- measured from the line dz/dt=0 Ùs"1), Peak-trough (the gram parameters were significantly greater in Group 2 than peak-to-trough measurement of the impedance cardiogram Group 1 (P<0·001). On multivariate analysis the par- Ùs"1), Area 1 (the area under the C wave of the impedance ameters which best differentiated the two groups were Area cardiogram above the line dz/dt=0 mÙ) and Area 2 (the 1 and Peak-trough. -

PUBLIC ACCESS to AUTOMATED EXTERNAL DEFIBRILLATORS (Aeds) FACTS
POSITION STATEMENT PUBLIC ACCESS TO AUTOMATED EXTERNAL DEFIBRILLATORS (AEDs) FACTS • Cardiac refers to the heart. Arrest means stop. Sudden cardiac arrest is the sudden and unexpected loss of heart function. • Signs of cardiac arrest include: no breathing or only gasping, no movement, and no pulse. • Up to 40,000 cardiac arrests occur each year in Canada. That’s one cardiac arrest every 12 minutes. Without rapid and appropriate treatment, most of these cardiac arrests will result in death. Thousands of lives could be saved through public access to automated external defibrillators. • An automated external defibrillator (AED) is a small, portable device used to identify cardiac rhythms and deliver a shock to correct abnormal electrical activity in the heart. As a result of the sophisticated electronics in an AED the operator will only be advised to deliver a shock if the • A landmark study of the City of Chicago airports public heart is in a rhythm which can be corrected by defibrillation. access to AED program showed survival rates as high as If a shockable rhythm is not detected, no shock can be 75%. This success is directly related to highly visible, readily given and the provider will be instructed to perform accessible automated external defibrillators for public use cardiopulmonary resuscitation (CPR) until emergency and an integrated structured emergency response system.7 medical services arrive. • Research shows that AEDs are most effectively used by • When an AED and CPR are immediately available, the trained individuals. However, AEDs are safe and easy to use chance of survival from sudden cardiac arrest is substantially by almost anyone. -

Cardiac Ablation: Types and Outcomes
CARDIAC ABLATION: TYPES AND OUTCOMES CARDIOVERSION AND ABLATION JASSIN M. JOURIA Dr. Jassin M. Jouria is a practicing Emergency Medicine physician, professor of academic medicine, and medical author. He graduated from Ross University School of Medicine and has completed his clinical clerkship training in various teaching hospitals throughout New York, including King’s County Hospital Center and Brookdale Medical Center, among others. Dr. Jouria has passed all USMLE medical board exams, and has served as a test prep tutor and instructor for Kaplan. He has developed several medical courses and curricula for a variety of educational institutions. Dr. Jouria has also served on multiple levels in the academic field including faculty member and Department Chair. Dr. Jouria continues to serve as a Subject Matter Expert for several continuing education organizations covering multiple basic medical sciences. He has also developed several continuing medical education courses covering various topics in clinical medicine. Recently, Dr. Jouria has been contracted by the University of Miami/Jackson Memorial Hospital’s Department of Surgery to develop an e-module training series for trauma patient management. Dr. Jouria is currently authoring an academic textbook on Human Anatomy & Physiology. ABSTRACT Atrial arrhythmias are serious disorders that can cause an irregular and/or rapid heartbeat, which can lead to serious clinical sequelae. Atrial fibrillation is an example of an atrial arrhythmia that can lead to blood clots, stroke, or heart failure. Electrical cardioversion and ablation are two procedures that can minimize these risks and treat atrial arrhythmia. Each of these treatments have risks and neither offers a complete success rate, but they can be very effective in providing greater quality of life, and extending the life expectancy of patients. -

Stress, Protocols, and Tracers
ASNC IMAGING GUIDELINES ASNC imaging guidelines for SPECT nuclear cardiology procedures: Stress, protocols, and tracers a b c Milena J. Henzlova, MD, W. Lane Duvall, MD, Andrew J. Einstein, MD, d e Mark I. Travin, MD, and Hein J. Verberne, MD a Mount Sinai Medical Center, New York, NY b Hartford Hospital, Hartford, CT c New York Presbyterian Hospital, Columbia University Medical Center, New York, NY d Montefiore Medical Center, Albert Einstein College of Medicine, Bronx, NY e Academic Medical Center, Amsterdam, The Netherlands doi:10.1007/s12350-015-0387-x Abbreviations LEHR Low energy high resolution A2A Adenosine 2a LVEF Left ventricular ejection fraction AHA American Heart Association MBq Megabecquerels ALARA As low as reasonably achievable mCi Millicuries AV Atrioventricular MPI Myocardial perfusion imaging BP Blood pressure MRI Magnetic resonance imaging CBF Coronary blood flow mSv Millisievert CAD Coronary artery disease NE Norepinephrine CPET Cardiopulmonary exercise testing NET1 Norepinephrine transporter-1 DSP Deconvolution of septal penetration NPO Nil per os (nothing by mouth) ECG Electrocardiogram NYHA New York Heart Association EF Ejection fraction PET Positron emission tomography ESRD End-stage renal disease ROI Region of interest HF Heart failure SPECT Single-photon emission computed HFrEF Heart failure (with) reduced ejection tomography fraction TAVR Transcatheter aortic valve replacement HMR Heart-to-mediastinum ratio WR Washout rate ICD Implantable cardioversion defibrillator WPW Wolff-Parkinson White IV Intravenous